Latest videos

Gowers' sign is a medical sign that indicates weakness of the proximal muscles, namely those of the lower limb. The sign describes a patient that has to use his hands and arms to "walk" up his own body from a squatting position due to lack of hip and thigh muscle strength. It is named for William Richard Gowers. Gowers' sign is classically seen in Duchenne muscular dystrophy, but also presents itself in centronuclear myopathy, myotonic dystrophy and various other conditions associated with proximal muscle weakness. For this maneuver, the patient is placed on the floor away from any objects that could otherwise be used to pull oneself to a standing position. It is also used in testing paraplegia.
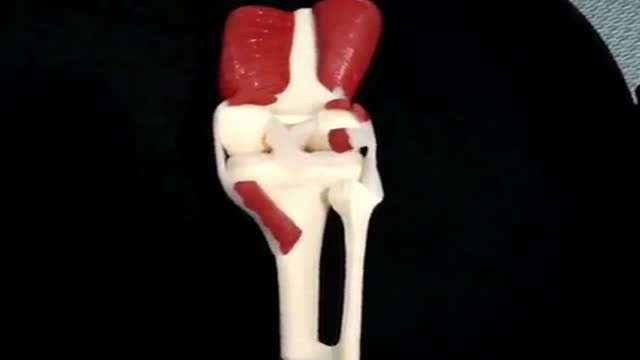
The knee joint is the largest joint in the body, consisting of 4 bones and an extensive network of ligaments and muscles. Injuries to the knee joint are amongst the most common in sporting activities and understanding the anatomy of the joint is fundamental in understanding any subsequent pathology.

A clavicle fracture is a bone fracture in the clavicle, or collarbone. It is often caused by a fall onto an outstretched upper extremity, a fall onto a shoulder, or a direct blow to the clavicle. Many research projects are underway regarding the medical healing process of clavicle fractures.
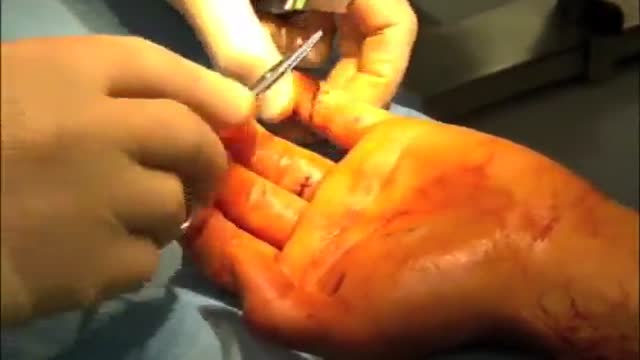
A deep cut on the palm side of your fingers, hand, wrist, or forearm can damage your flexor tendons, which are the tissues that help control movement in your hand. A flexor tendon injury can make it impossible to bend your fingers or thumb.
The term mallet finger has long been used to describe the deformity produced by disruption of the terminal extensor mechanism at the distal interphalangeal (DIP) joint. Mallet finger is the most common closed tendon injury that is seen in athletes; this injury is also common in nonathletes after "innocent" trauma. Mallet finger has also been referred to as drop, hammer, or baseball finger (although baseball accounts for only a small percentage of such injuries).

Minimally Invasive Surgery (MIS) Hip Joint Replacement is an advancement in hip replacement that offers important advantages over standard surgical procedures. Stryker has partnered with surgeons worldwide to develop MIS procedures and surgical instruments that are designed to help your surgeons do their very best to help you recover your lifestyle. These techniques bring together a wide variety of hip implants, new minimally invasive surgical techniques, and new instrumentation. The direct anterior approach is one of the minimally invasive techniques used in hip replacement surgery. Continuing orthopaedic experience suggests that this procedure may offer several advantages over the more traditional surgical approaches to hip replacement.1 Traditional hip replacement techniques involve operating from the side (lateral) or the back (posterior) of the hip, which requires a significant disturbance of the joint and connecting tissues and an incision approximately 8-12 inches long. In comparison, the direct anterior approach requires an incision that is only 3-4 inches in length and located at the front of the hip.1 In this position, the surgeon does not need to detach any of the muscles or tendons.

Immunomodulating effect of autohaemotherapy (a literature review). PMID 3534085 [PubMed indexed for MEDLINE]
J Hyg Epidemiol Microbiol Immunol. 1986;30(3):331-6.
Immunomodulating effect of autohaemotherapy (a literature review).
Klemparskaya NN, Shalnova GA, Ulanova AM, Kuzmina TD, Chuhrov AD.
Abstract
An analysis is presented of experimental and clinical data from different authors on the stimulating effect of autohaemotherapy with regard to the immunological reactivity of humans and animals as well as in vitro experiments with lymphocytes. Erythrolysate has been found to exert a more powerful effect than intact erythrocytes. The stimulating effect of autohaemotherapy on both irradiated and non-irradiated animals manifests itself in an increase in resistance to infection (increased LD50 in experimental infection), enhanced production of antibodies to microbial and tissue antigens and activated functioning of cell-mediated immune defence mechanisms. The favourable influences on radioresistance and the antitumour effect of authohaemotherapy are described. Induced desensitization plays an important part in the mechanism of action of autohaemotherapy. The administration of large doses of erythrocytes or of erythrolysate results in immunosuppression. Autohaemotherapy does not cause side effects and is feasible both on an in-and out-patient basis.
PMID: 3534085
[PubMed - indexed for MEDLINE]
http://www.ncbi.nlm.nih.gov/pubmed/3534085
Autohemotherapy: an immunization with our own blood
http://www.geocities.ws/autohemoterapiabr/
http://autohemoterapia.fortunecity.com/
http://www.geocities.ws/autohemoterapiabr/aht_english.htm
http://autohemoterapia.fortunecity.com/aht_english.htm
-
Auto-hemotherapy PDF files in GOOGLE sites:
https://sites.google.com/site/autohemotherapy/

Sleepiness, tiredness and fatigue are complaints which must be thoroughly analyzed to eliminate blur and ambiguity.
Physiological sleepiness (“sleep pressure”) increases while being awake and additionally underlies the circadian rhythm with a lower threshold to fall asleep during night time.
Excessive daytime sleepiness (EDS) is considered normal only after sleep deprivation. Clinically, EDS manifests by frequents daytime napping and/or reduced alertness with automatic behavior or - in its extreme form - in recurrent attacks of sudden, uncontrollable compulsion to sleep also in inappropriate situations (= “sleep attacks”).
EDS is “objectively” addressed by measuring the mean sleep latency to four to five nap opportunities throughout the day using the multiple sleep latency test (MSLT) or the maintenance of wakefulness test (MWT).
EDS denotes both, a ready entrance into sleep as well as difficulty in staying awake during daytime or accordingly in inappropriate situations. These two partially independent aspects of EDS are separately assessed by the “passive” MSLT and the “active” MWT respectively.
For that reason the MSLT and MWT only weakly correlate with each other when tested over a broad range of patients with EDS. It is important to keep in mind, that these tests are importantly influenced by a great variety of factors such as mood, anxiety, and motivation.
“Vigilance” comprises wakefulness, alertness and attention and therefore is more than just the reciprocal to sleepiness. Cognitive performance tasks such as Steer Clear Reaction Time Test (SCRTT) or driving simulators require the complete integrity of vigilance to achieve normal results. Hypersomnia is usually broadly defined as the combination of abnormally prolonged night-time sleep (regularly >10 h) with EDS during ≥1 months.
On the other hand, the term hypersomnia has also been used in a narrower scene for the isolated abnormality of a prolonged night-time sleep need (>10 h). “Tiredness”, also in colloquial language often used for sleepiness, in a broader sense also describes the feeling of lack of energy, motivation and initiative.
These patients seek rest rather than sleep. They often cannot fall asleep when given the opportunity in spite of feeling tired, and hence, in an MSLT, do not show an abnormally short sleep latency. Furthermore, tiredness (and fatigue) as opposed to sleepiness has a mental (“central”) and physiological (bodily or “peripheral”) component, which the patients can readily distinguish. Patients with insomnia, mild sleep apnea syndrome, or depression rather suffer from mental tiredness than sleepiness during the day.
The simple subjective self-assessment using the Epworth Sleepiness Scale (ESS) quite reliably differentiates between sleepiness and mental tiredness (without sleepiness), which makes it a widely used test. The term “fatigue” is also heterogeneously used.
In physiology the “fatigue” implied a “time on task performance decrement” to describe decreasing muscle force during a sustained physical effort. In clinical medicine one distinguishes physical (“peripheral”) from mental (“central”) fatigue and the term usually denotes a chronic and more abnormal situation than tiredness.
In a broad sense “fatigue” implies a deficiency in coping satisfactorily with mental and physical work load. The chronic fatigue syndrome entails both mental as well as a physical fatigue (so called “leaden paralysis” of limbs). Depressive states are often associated with insomnia and fatigue, but there are also cases with hypersomnia rather than insomnia ( non organic hypersomnia , “atypical depression” or “hypersomnolent depression”)
Sometimes these patients have a tendency to spend much of the day lying in the bed without actually sleeping (so called clinophilia). The basic and clinical aspects of fatigu

M.Torabi Nami MD, PhDc Department of Neuroscience Institute for Cognitive Science Studies (ICSS), Tehran 15948 Iran Torabi_m@iricss.org Abstract Sleepiness, tiredness and fatigue are complaints which must be thoroughly analyzed to eliminate blur and ambiguity. Physiological sleepiness (“sleep pressure”) increases while being awake and additionally underlies the circadian rhythm with a lower threshold to fall asleep during night time. Excessive daytime sleepiness (EDS) is considered normal only after sleep deprivation. Clinically, EDS manifests by frequents daytime napping and/or reduced alertness with automatic behavior or - in its extreme form - in recurrent attacks of sudden, uncontrollable compulsion to sleep also in inappropriate situations (= “sleep attacks”). EDS is “objectively” addressed by measuring the mean sleep latency to four to five nap opportunities throughout the day using the multiple sleep latency test (MSLT) or the maintenance of wakefulness test (MWT). EDS denotes both, a ready entrance into sleep as well as difficulty in staying awake during daytime or accordingly in inappropriate situations. These two partially independent aspects of EDS are separately assessed by the “passive” MSLT and the “active” MWT respectively. For that reason the MSLT and MWT only weakly correlate with each other when tested over a broad range of patients with EDS. It is important to keep in mind, that these tests are importantly influenced by a great variety of factors such as mood, anxiety, and motivation. “Vigilance” comprises wakefulness, alertness and attention and therefore is more than just the reciprocal to sleepiness. Cognitive performance tasks such as Steer Clear Reaction Time Test (SCRTT) or driving simulators require the complete integrity of vigilance to achieve normal results. Hypersomnia is usually broadly defined as the combination of abnormally prolonged night-time sleep (regularly >10 h) with EDS during ≥1 months. On the other hand, the term hypersomnia has also been used in a narrower scene for the isolated abnormality of a prolonged night-time sleep need (>10 h). “Tiredness”, also in colloquial language often used for sleepiness, in a broader sense also describes the feeling of lack of energy, motivation and initiative. These patients seek rest rather than sleep. They often cannot fall asleep when given the opportunity in spite of feeling tired, and hence, in an MSLT, do not show an abnormally short sleep latency. Furthermore, tiredness (and fatigue) as opposed to sleepiness has a mental (“central”) and physiological (bodily or “peripheral”) component, which the patients can readily distinguish. Patients with insomnia, mild sleep apnea syndrome, or depression rather suffer from mental tiredness than sleepiness during the day. The simple subjective self-assessment using the Epworth Sleepiness Scale (ESS) quite reliably differentiates between sleepiness and mental tiredness (without sleepiness), which makes it a widely used test. The term “fatigue” is also heterogeneously used. In physiology the “fatigue” implied a “time on task performance decrement” to describe decreasing muscle force during a sustained physical effort. In clinical medicine one distinguishes physical (“peripheral”) from mental (“central”) fatigue and the term usually denotes a chronic and more abnormal situation than tiredness. In a broad sense “fatigue” implies a deficiency in coping satisfactorily with mental and physical work load. The chronic fatigue syndrome entails both mental as well as a physical fatigue (so called “leaden paralysis” of limbs). Depressive states are often associated with insomnia and fatigue, but there are also cases with hypersomnia rather than insomnia ( non organic hypersomnia , “atypical depression” or “hypersom