Top videos
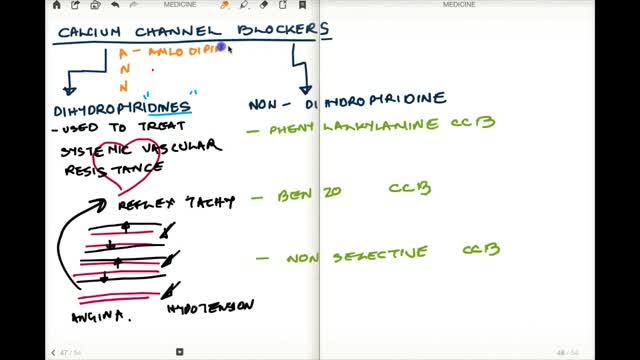
Calcium channel blockers prevent calcium from entering cells of the heart and blood vessel walls, resulting in lower blood pressure. Calcium channel blockers, also called calcium antagonists, relax and widen blood vessels by affecting the muscle cells in the arterial walls. Some calcium channel blockers have the added benefit of slowing your heart rate, which can further reduce blood pressure, relieve chest pain (angina) and control an irregular heartbeat. Examples of calcium channel blockers Some calcium channel blockers are available in short-acting and long-acting forms. Short-acting medications work quickly, but their effects last only a few hours. Long-acting medications are slowly released to provide a longer lasting effect. Several calcium channel blockers are available. Which one is best for you depends on your health and the condition being treated. Examples of calcium channel blockers include: Amlodipine (Norvasc) Diltiazem (Cardizem, Tiazac, others) Felodipine Isradipine Nicardipine Nifedipine (Adalat CC, Afeditab CR, Procardia) Nisoldipine (Sular) Verapamil (Calan, Verelan) In some cases, your doctor might prescribe a calcium channel blocker with other high blood pressure medications or with cholesterol-lowering drugs such as statins.
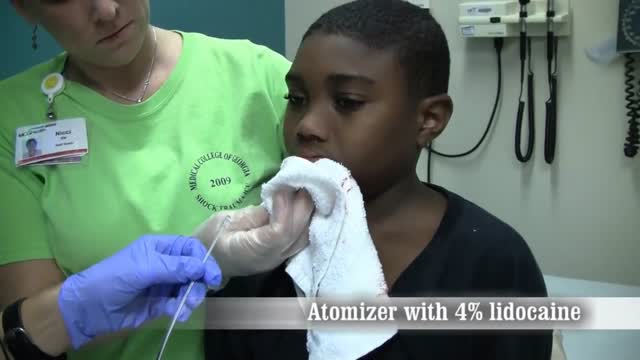
Nosebleeds common. Most often they are a nuisance and not a true medical problem. But they can be both. Nosebleed care Sit upright and lean forward. By remaining upright, you reduce blood pressure in the veins of your nose. This discourages further bleeding. Sitting forward will help you avoid swallowing blood, which can irritate your stomach. Pinch your nose. Use your thumb and index finger to pinch your nostrils shut. Breathe through your mouth. Continue to pinch for five to 10 minutes. Pinching sends pressure to the bleeding point on the nasal septum and often stops the flow of blood. To prevent re-bleeding, don't pick or blow your nose and don't bend down for several hours after the bleeding episode. During this time remember to keep your head higher than the level of your heart. If re-bleeding occurs, blow out forcefully to clear your nose of blood clots and spray both sides of your nose with a decongestant nasal spray containing oxymetazoline (Afrin, Mucinex Moisture Smart, others). Pinch your nose again as described above and call your doctor. When to seek emergency care The bleeding lasts for more than 20 minutes The nosebleed follows an accident, a fall or an injury to your head, including a punch in the face that may have broken your nose
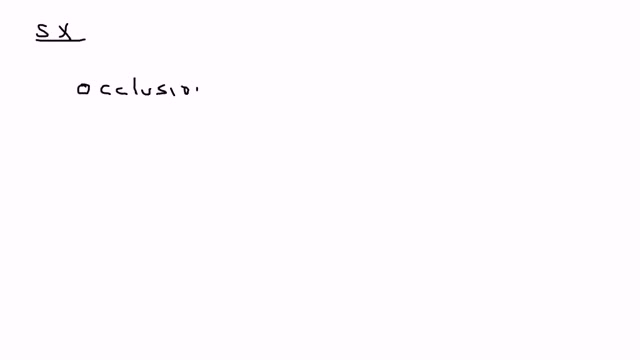
Renal artery stenosis is a narrowing of arteries that carry blood to one or both of the kidneys. Most often seen in older people with atherosclerosis (hardening of the arteries), renal artery stenosis can worsen over time and often leads to hypertension (high blood pressure) and kidney damage.
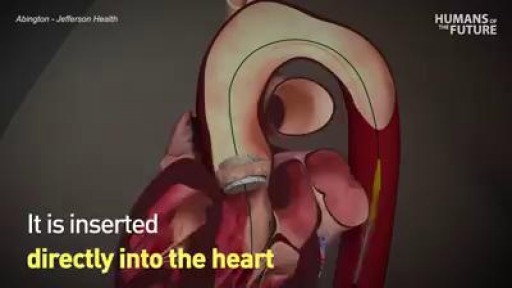
Surgery to replace an aortic valve is done for aortic valve stenosis and aortic valve regurgitation. During this surgery, the damaged valve is removed and replaced with an artificial valve. The valve replacement is typically an open-heart surgery.

http://smoking-videos.plus101.com
Quit Smoking Forever Formula Videos - How To Quit Smoking In As Fast As 1 Week Without Agitation, Cravings Or Withdrawal Symptoms.You're about to uncover the 3 elements that will rapidly boost your chances of success to quit smoking and not only that, you'll learn ways to escape cravings and how to avoid a relapse that can happen in the future even to people with the most willpower.
Most babies will move into delivery position a few weeks prior to birth, with the head moving closer to the birth canal. When this fails to happen, the baby’s buttocks and/or feet will be positioned to be delivered first. This is referred to as “breech presentation.” Breech births occur in approximately 1 out of 25 full-term births.
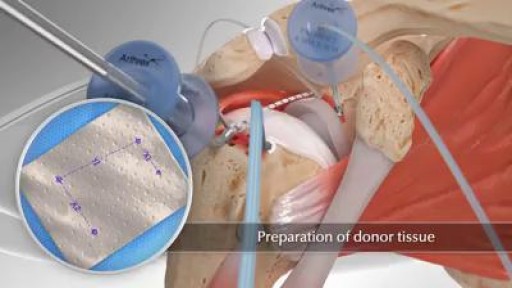
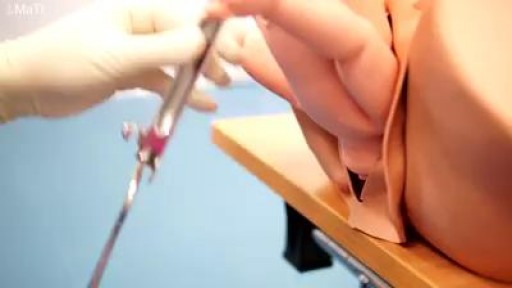
Superior capsule reconstruction (SCR) is a promising alternative treatment for irreparable posterosuperior rotator cuff tears (Figure 1). It utilizes a graft from the superior glenoid to the greater tuberosity to stabilize the humeral head. In a study by Mihata and colleagues of 23 patients who underwent SCR with a fascia lata autograft at a minimum of 2 years follow-up, the American Shoulder and Elbow Surgeons (ASES) score improved significantly from 23.5 preoperatively to 92.9. Postoperative MRI showed 83% of patients had intact reconstructions with no progression of muscle atrophy.
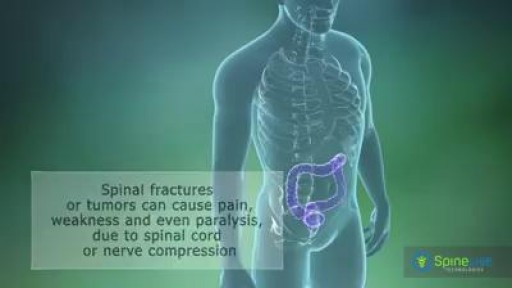
A spinal tumor is a growth that develops within your spinal canal or within the bones of your spine. It may be cancerous or noncancerous. Tumors that affect the bones of the spine (vertebrae) are known as vertebral tumors. Tumors that begin within the spinal cord itself are called spinal cord tumors. There are two main types of tumors that may affect the spinal cord: Intramedullary tumors begin in the cells within the spinal cord itself, such as astrocytomas or ependymomas. Extramedullary tumors develop within the supporting network of cells around the spinal cord. Although they don't begin within the spinal cord itself, these types of tumors may affect spinal cord function by causing spinal cord compression and other problems. Examples of extramedullary tumors that can affect the spinal cord include schwannomas, meningiomas and neurofibromas.
Screening is looking for cancer before a person has any symptoms. This can help find cancer at an early stage when it may be easier to treat. Lung cancer may have spread by the time a person has symptoms. One reason lung cancer is so serious is because it usually is not found until it has spread and is more difficult to treat. Screening may provide new hope for early detection and treatment of lung cancer. Scientists study screening tests to find those with the fewest risks and most benefits. They look at results over time to see if finding the cancer early decreases a person's chance of dying from the disease.

This video clip shows an upper track endoscopy of A 75 year-old female, presented with severe adominal pain since three days. Endoscopy displays a deep ulcer at the lesser curvature of the stomach. This patient has a klatskin´s tumor (bile duct bifurcation).

Bacterial meningitis is very serious and can be deadly. Death can occur in as little as a few hours. While most people with meningitis recover, permanent disabilities such as brain damage, hearing loss, and learning disabilities can result from the infection. There are several types of bacteria that can cause meningitis. Some of the leading causes of bacterial meningitis in the United States include Streptococcus pneumoniae, group B Streptococcus, Neisseria meningitidis, Haemophilus influenzae, and Listeria monocytogenes.
Over one million Americans have the sexually transmitted virus, HIV, which can lead to the deadly disease known as AIDS.
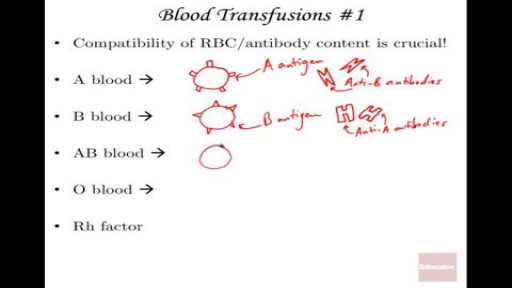
HIV can be transmitted in the sexual fluids, blood or breast milk of an infected person. HIV prevention therefore involves a wide range of activities including prevention of mother-to-child transmission, needle exchanges and harm reduction for injecting drug users, and precautions for health care workers.

Our General Surgery team treats hernia patients on a daily basis. In fact, you could consider them to be hernia experts. We sat down with one of those experts, Dr. Heater Dunlap, to talk about the common signs and symptoms of hernias and to answer the question of when to see a doctor.