Top videos
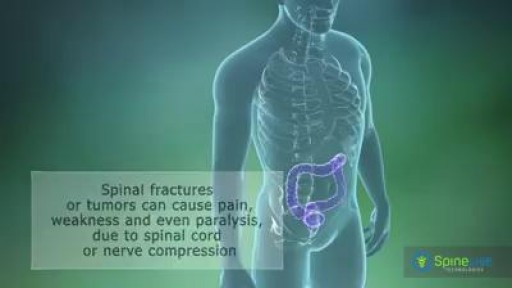
A spinal tumor is a growth that develops within your spinal canal or within the bones of your spine. It may be cancerous or noncancerous. Tumors that affect the bones of the spine (vertebrae) are known as vertebral tumors. Tumors that begin within the spinal cord itself are called spinal cord tumors. There are two main types of tumors that may affect the spinal cord: Intramedullary tumors begin in the cells within the spinal cord itself, such as astrocytomas or ependymomas. Extramedullary tumors develop within the supporting network of cells around the spinal cord. Although they don't begin within the spinal cord itself, these types of tumors may affect spinal cord function by causing spinal cord compression and other problems. Examples of extramedullary tumors that can affect the spinal cord include schwannomas, meningiomas and neurofibromas.

Most intact aortic aneurysms do not produce symptoms. As they enlarge, symptoms such as abdominal pain and back pain may develop. Compression of nerve roots may cause leg pain or numbness. Untreated, aneurysms tend to become progressively larger, although the rate of enlargement is unpredictable for any individual. Rarely, clotted blood which lines most aortic aneurysms can break off and result in an embolus. They may be found on physical examination. Medical imaging is necessary to confirm the diagnosis. Symptoms may include: anxiety or feeling of stress; nausea and vomiting; clammy skin; rapid heart rate. In patients presenting with aneurysm of the arch of the aorta, a common symptom is a hoarse voice as the left recurrent laryngeal nerve (a branch of the vagus nerve) is stretched. This is due to the recurrent laryngeal nerve winding around the arch of the aorta. If an aneurysm occurs in this location, the arch of the aorta will swell, hence stretching the left recurrent laryngeal nerve. The patient therefore has a hoarse voice as the recurrent laryngeal nerve allows function and sensation in the voicebox. Abdominal aortic aneurysms, hereafter referred to as AAAs, are the most common type of aortic aneurysm. One reason for this is that elastin, the principal load-bearing protein present in the wall of the aorta, is reduced in the abdominal aorta as compared to the thoracic aorta (nearer the heart). Another is that the abdominal aorta does not possess vasa vasorum, hindering repair. Most are true aneurysms that involve all three layers (tunica intima, tunica media and tunica adventitia), and are generally asymptomatic before rupture. The most common sign for the aortic aneuysm is the Erythema nodosum also known as leg lesions typically found near the ankle area. The prevalence of AAAs increases with age, with an average age of 65–70 at the time of diagnosis. AAAs have been attributed to atherosclerosis, though other factors are involved in their formation. An AAA may remain asymptomatic indefinitely. There is a large risk of rupture once the size has reached 5 cm, though some AAAs may swell to over 15 cm in diameter before rupturing. Before rupture, an AAA may present as a large, pulsatile mass above the umbilicus. A bruit may be heard from the turbulent flow in a severe atherosclerotic aneurysm or if thrombosis occurs. Unfortunately, however, rupture is usually the first hint of AAA. Once an aneurysm has ruptured, it presents with a classic pain-hypotension-mass triad. The pain is classically reported in the abdomen, back or flank. It is usually acute, severe and constant, and may radiate through the abdomen to the back. The diagnosis of an abdominal aortic aneurysm can be confirmed at the bedside by the use of ultrasound. Rupture could be indicated by the presence of free fluid in potential abdominal spaces, such as Morison's pouch, the splenorenal space (between the spleen and left kidney), subdiaphragmatic spaces (underneath the diaphragm) and peri-vesical spaces. A contrast-enhanced abdominal CT scan is needed for confirmation. Only 10–25% of patients survive rupture due to large pre- and post-operative mortality. Annual mortality from ruptured abdominal aneurysms in the United States alone is about 15,000. Another important complication of AAA is formation of a thrombus in the aneurysm.
When the hematocrit rises to 60 or 70%, which it often does in polycythemia, the blood viscosity can become as great as 10 times that of water, and its flow through blood vessels is greatly retarded because of increased resistance to flow. This will lead to decreased oxygen delivery.
Idiopathic pulmonary fibrosis (IPF) is defined as a specific form of chronic, progressive fibrosing interstitial pneumonia of unknown cause, primarily occurring in older adults, limited to the lungs, and associated with the histopathologic and/or radiologic pattern of usual interstitial pneumonia (UIP).[1] Signs and symptoms The clinical symptoms of idiopathic pulmonary fibrosis are nonspecific and can be shared with many pulmonary and cardiac diseases. Most patients present with a gradual onset (often >6 mo) of exertional dyspnea and/or a nonproductive cough. Approximately 5% of patients have no presenting symptoms when idiopathic pulmonary fibrosis is serendipitously diagnosed.

The Epley Maneuver for Vertigo can be very effective at relieving vertigo symptoms, but it’s a procedure that should be performed by a physical therapist or other health care professional. This video is for demonstration purposes only. See Doctor Jo’s blog post about the Epley
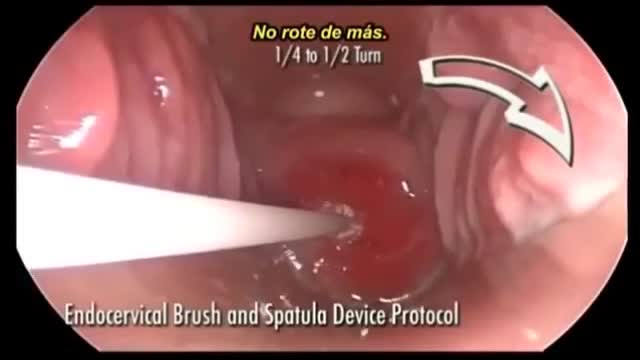
In patients age ;::25, HPV DNA testing is the preferred next step in management if the initial cytology shows ASC-US. In this method, samples are collected for both cytology and reflex HPV DNA. If cytology results are positive, HPV DNA testing is performed. If cytology results are negative, the sample for HPV DNA is discarded. HPV DNA testing along with Pap smear at 3 years is recommended if initial cytology shows ASC-US but HPV DNA testing is negative

Shut the front door: Scientists have finally found the perfect breasts. No, they weren't hiding in the Amazon or roving solo across the Sahara (although we have no doubt there are women in both the Amazon and the Sahara who have magnificent mammaries); it turns out these perfect breasts were hiding in a plastic surgeon's office this whole time! Now, before you get all worked up, the American Society of Plastic Surgeons (ASPS) would like you to know that the super-fake looking plastic breasts of yore are not actually what people think are most attractive now. According to a study published in the Journal of Plastic and Reconstructive Surgery—which involved asking over 1,300 people to look at pictures of naked boobies and rank them by hotness (stop laughing, this is serious research!)—people preferred a more "real" and "normal" look from their silicone, with the ideal breast shape having a 45:55 ratio. People said the best chests have 45 percent of the fullness above the nipple line and 55 percent of the fullness below, in a slightly teardrop shape. Researchers noted this preference remained consistent across gender, racial, and ethnic groups with the 45:55 ratio favored by 87 percent of women in their 30s, 90 percent of men, and 94 percent of plastic surgeons.

Cancer starts when cells in a part of the body begins to grow out of control and can spread to other areas of the body. There are many kinds of cancer. Cells in nearly any part of the body can become cancer. To learn more about how cancers start and spread, see What Is Cancer? Leukemias are cancers that start in cells that would normally develop into different types of blood cells. Here we will talk about acute myeloid leukemia (AML). Acute myeloid leukemia (AML) has many other names, including acute myelocytic leukemia, acute myelogenous leukemia, acute granulocytic leukemia, and acute non-lymphocytic leukemia. “Acute” means that this leukemia can progress quickly if not treated, and would probably be fatal in a few months. “Myeloid” refers to the type of cell this leukemia starts from. Most cases of AML develop from cells that would turn into white blood cells (other than lymphocytes), but some cases of AML develop in other types of blood-forming cells. The different types of AML are listed in “ How is acute myeloid leukemia classified?” AML starts in the bone marrow (the soft inner part of certain bones, where new blood cells are made), but in most cases it quickly moves into the blood. It can sometimes spread to other parts of the body including the lymph nodes, liver, spleen, central nervous system (brain and spinal cord), and testicles. Other types of cancer can start in these organs and then spread to the bone marrow. But these cancers that start elsewhere and then spread to the bone marrow are not leukemias. Normal bone marrow, blood, and lymphoid tissue To understand the different types of leukemia, it helps to know about the blood and lymph systems.

Morning erections have colloquially been termed as “morning wood” while scientifically it is called nocturnal penile tumescence. It is a normal and healthy physiological reaction and response that most men experience in their lives. Morning erections are really the ending of a series of erections that happen to men during the night. Healthy men can, on average, have anywhere between three to five erections in a full night of sleep, each of which lasts from 25-35 minutes.
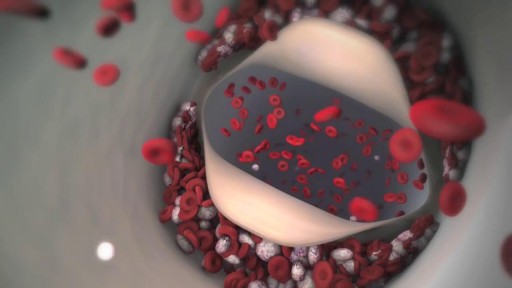
Symptoms of blood clots in specific body locations are as follows: Symptoms of blood clots in legs (deep vein thrombosis (DVT) are pain, redness, and swelling. Symptoms of an arterial blood clot in a limb (leg or arm) include pain, pale color, and coolness to the touch. and the leg is cool and pale.