Top videos
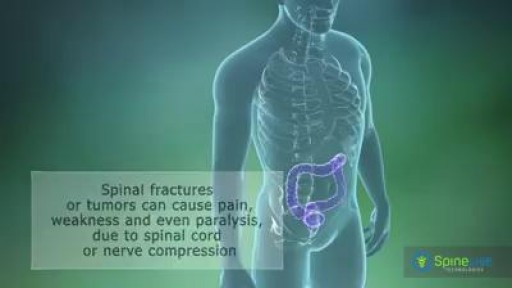
A spinal tumor is a growth that develops within your spinal canal or within the bones of your spine. It may be cancerous or noncancerous. Tumors that affect the bones of the spine (vertebrae) are known as vertebral tumors. Tumors that begin within the spinal cord itself are called spinal cord tumors. There are two main types of tumors that may affect the spinal cord: Intramedullary tumors begin in the cells within the spinal cord itself, such as astrocytomas or ependymomas. Extramedullary tumors develop within the supporting network of cells around the spinal cord. Although they don't begin within the spinal cord itself, these types of tumors may affect spinal cord function by causing spinal cord compression and other problems. Examples of extramedullary tumors that can affect the spinal cord include schwannomas, meningiomas and neurofibromas.
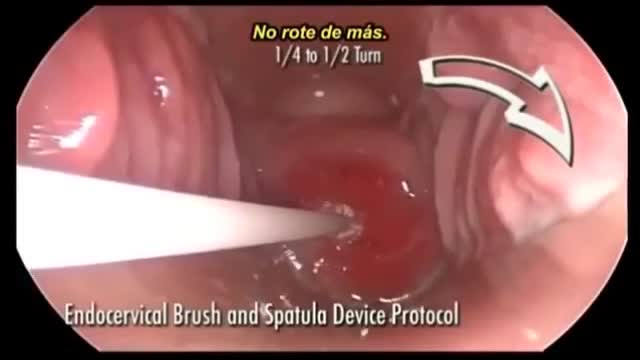
In patients age ;::25, HPV DNA testing is the preferred next step in management if the initial cytology shows ASC-US. In this method, samples are collected for both cytology and reflex HPV DNA. If cytology results are positive, HPV DNA testing is performed. If cytology results are negative, the sample for HPV DNA is discarded. HPV DNA testing along with Pap smear at 3 years is recommended if initial cytology shows ASC-US but HPV DNA testing is negative

Pectus excavatum (hollow chest) deformity is not uncommon (sometimes mild and other times severe in its form). The chest deformity is often the source of self-consciousness for the patients while growing up. Several surgical techniques (Nuss procedure, Ravitch procedure, etc) are available.

In this video a real case of the extremely rare disease "Fibrodysplasia ossificans progressiva" or what is called the "FOP" This disease is commonly misdiagnosed and usually end up by unnecessary surgery which exaggerate the disease. Children born with FOP characteristically have deformed great toes, possibly missing a joint or simply presenting with a notable lump at the minor joint. The first "flare-up" that leads to the formation of FOP bones usually occurs before the age of 10. FOP is a genetic disease. The bone growth progresses from the top downward, just as bones grow in fetuses. A child with FOP will typically develop bones starting at the neck, then on the shoulders, arms, chest area and finally on the feet. However it does not necessarily occur in this order due to injury-caused flare-ups. Often, the tumor-like lumps that characterize the disease appear suddenly. The gene that causes ossification is normally deactivated after a fetus' bones are formed in the womb, but in patients with FOP, the gene keeps working. Aberrant bone formation in patients with FOP occurs when injured connective tissue or muscle cells at the sites of injury or growth incorrectly express an enzyme for bone repair during apoptosis (self-regulated cell death), resulting in lymphocytes containing excess bone morphogenetic protein 4 (BMP4) provided during the immune system response. Since the incorrect enzyme remains unresolved within the immune response, the body continues providing the incorrect BMP4-containing lymphocytes. BMP4 is a product that contributes to the development of the skeleton in the normal embryo.

Urogenital neoplasms spreading to the inguinal lymph nodes are penile carcinoma (the most frequent), urethral and scrotum cancers, tumors of the testis with scrotal violation. Penile carcinoma is an uncommon malignant disease and accounts for as many 0.4-0.6% of male cancers. Most patients are elder...ly. It rarely occurs in men under age 60 and its incidence increases progressively until it reaches a peak in the eighth decade 1. The risk of a lymph node invasion is greater with high grade and high stage tumors 2. Some investigators have reported the inaccuracy of the sentinel node biopsy 3, 4, described by Cabanas 5. Patients with metastatic lymph node penis cancer have a very poor prognosis if penectomy only is performed. Ilioinguinal lymphadenectomy is basically carried out as a treatment modality and not only as a staging act. Patients with lymph node invasion have a 30-40% cure rate. Ilioinguinal lymphadenectomy should be also performed in patients with disseminated neoplasms for the local control of the disease. The 5 years survival rate of patients with clinically negative lymph nodes treated with a modified inguinal lymphadenectomy is 88% versus 38% in patients not initially treated with lymphadenectomy 6. This video-tape clearly shows a therapeutic algorithm, the anatomy of the inguinal lymph nodes, according to Rouviere 7 and Daseler 8, the radical ilioinguinal node dissection with transposition of the sartorius muscle and the modified inguinal lymphadenectomy proposed by Catalona 9. References: 1. Lynch D.F. and Schellhammer P: Tumors of the penis. In Campbell’s Urology Seventh Edition, edited by Walsh P.C., Retik A.B., Darracott Vaughan E. and Wein A.J. W.B. Saunders Company, Vol. 3, chapt. 79, p. 2458, 1998. 2. Pizzocaro G., Piva L., Bandieramonte G., Tana S. Up-to-date management of carcinoma of the penis. Eur. Urol. 32: 5-15, 1997 3. Perinetti E., Crane D.B. and Catalona W.J. Unreliability of sentinel lymph node biopsy for staging penile carcinoma. J. Urol. 124: 734, 1980 4. Fowler J.E. Jr. Sentinel lymph node biopsy for staging penile cancer. Urology 23: 352, 1984 5. Cabanas R.M. An approach for the treatment of penile carcinoma. Cancer 39: 456, 1977 6. Russo P. and Gaudin P. Management strategies for carcinoma of the penis. Contemporary Urology;5:48-66, 2000 7. Rouviere H. Anatomy of the human lymphatic system. Edwards Brothers, p. 218, 1938 8. Daseler E.H., Anson B.J., Reimann A.F. Radical excision of the inguinal and iliac lymph glands: a study based on 450 anatomical dissections and upon supportive clinical observations. Surg. Gynecol. Obstet. 87: 679, 1948 9. Catalona W.J. Modified inguinal lymphadenectomy for carcinoma of the penis with preservation of saphenous veins: technique and preliminary results. J. Urol. 140: 306-310, 1988

This shows a full Abdominoplasty surgery performed by Dr. Art Foley in Olympia Washington. Abdominoplasty is also commonly referred to as a "Tummy Tuck." Tummy tuck is a surgical procedure also known as abdominoplasty to remove excess skin and fat from the middle and lower abdomen and to tighten the muscles of the abdominal wall. The procedure can dramatically reduce the appearance of a protruding abdomen. But bear in mind, it does produce a permanent scar.
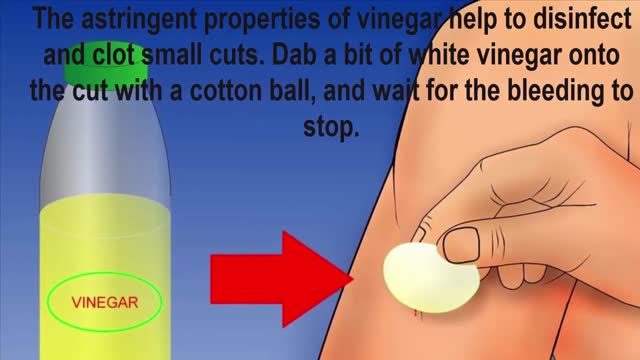
Injuries and certain medical conditions can result in bleeding. This can trigger anxiety and fear, but bleeding has a healing purpose. Still, you need to understand how to treat common bleeding incidents, like cuts and bloody noses, as well as when to seek medical help.

During the examination, the doctor gently puts a lubricated, gloved finger of one hand into the rectum. He or she may use the other hand to press on the lower belly or pelvic area. A digital rectal exam is done for men as part of a complete physical examination to check the prostate gland .

Varicose veins are caused by weakened valves and veins in your legs. Normally, one-way valves in your veins keep blood flowing from your legs up toward your heart. When these valves do not work as they should, blood collects in your legs, and pressure builds up. The veins become weak, large, and twisted.