Top videos
Overview HIV is a virus that affects the immune system, specifically the CD4 cells. The CD4 cells help protect the body from illness. Unlike other viruses that the immune system can fight off, HIV can’t be eliminated by the immune system. The symptoms of HIV can vary greatly from person to person. No two people with HIV will likely experience the exact same symptoms. However, HIV will generally follow this pattern: acute illness asymptomatic period advanced infection Acute illness Approximately 80 percent of people who contract HIV experience flu-like symptoms within two to four weeks. This flu-like illness is known as acute HIV infection. Acute HIV infection is the primary stage of HIV and lasts until the body has created antibodies against the virus. The most common symptoms of this stage of HIV include: body rash fever sore throat severe headaches Less common symptoms may include: fatigue swollen lymph nodes ulcers in the mouth or on the genitals muscle aches joint pain nausea and vomiting night sweats Symptoms typically last one to two weeks. Anyone who has these symptoms and thinks they may have contracted HIV should consider scheduling an appointment with their healthcare provider to get tested. Symptoms specific to men Symptoms of HIV are generally the same in women and men. One HIV symptom that is unique to men is an ulcer on the penis. HIV may lead to hypogonadism, or poor production of sex hormones, in either sex. However, hypogonadism’s effects on men are easier to observe than its effects on women. Symptoms of low testosterone, one aspect of hypogonadism, can include erectile dysfunction (ED).
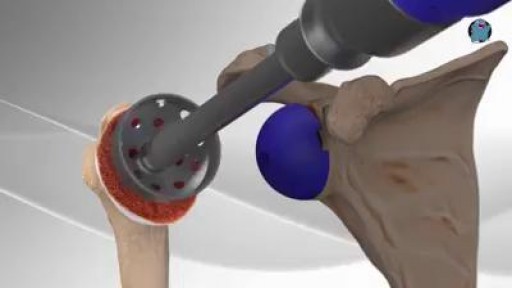
Every year, thousands of conventional total shoulder replacements are successfully done in the United States for patients with shoulder arthritis. This type of surgery, however, is not as beneficial for patients with large rotator cuff tears who have developed a complex type of shoulder arthritis called "cuff tear arthropathy." For these patients, conventional total shoulder replacement may result in pain and limited motion, and reverse total shoulder replacement is a better option.
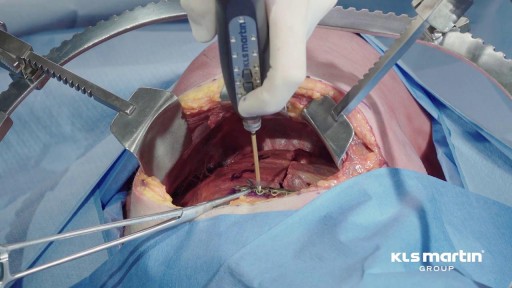
A fractured rib is usually a result of a fall or accident. Prolonged coughing and sports with repetitive movement, such as golf, also can cause a rib fracture. Symptoms include pain when taking a deep breath, pressing on the injured area, or bending or twisting the body. In most cases, fractured ribs usually heal on their own in one or two months. Pain relievers can make it easier to breathe deeply.

You may have heard that some positions, such as your partner on top (missionary position), are better than others for getting pregnant. In fact, there's no evidence to back these theories up. Experts just haven't done the research yet. What experts have done, though, is use scanning to show what's going on inside when you're doing the deed. The research looked at two positions: the missionary position and doggy style. (Doggy style being when you're on all fours, and your partner enters you from behind). Common sense tells us that these positions allow for deep penetration. This means that they're more likely to place sperm right next to your cervix (the opening of your uterus). The scans confirm that the tip of the penis reaches the areas between the cervix and vaginal walls in both of these positions. The missionary position allows the penis to reach the area at the front of the cervix. The rear entry position reaches the area at back of the cervix. It's amazing what some experts spend their time doing, isn't it! Other positions, such as standing up, or woman on top, may be just as good for getting sperm right next to the cervix. We just don't know yet. So, in the meantime, enjoy some variety in your sex life and keep it fun while you're trying for a baby. And talk to others who are hoping to get pregnant by joining our Actively trying group. Do I have to have an orgasm to conceive? Obviously, it's very important for your partner to reach orgasm if you are trying for a baby. There is no evidence, however, that you need to orgasm to conceive. The female orgasm is all about pleasure and satisfaction. It doesn't really help to get the sperm to the egg. Gentle contractions in your uterus can help the sperm along, but these happen without you having an orgasm. So, it's really not vital for you to reach orgasm after your partner, or even to reach orgasm at all, for you to conceive.
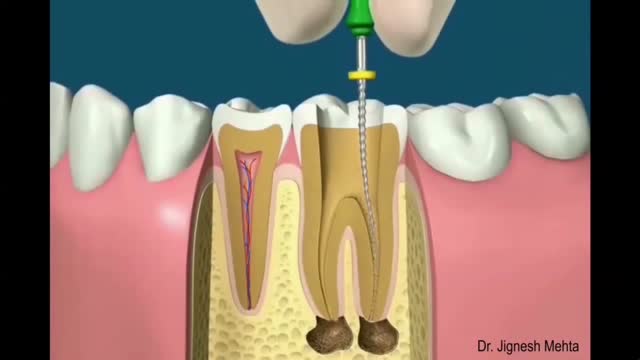
“Endo” is the Greek word for “inside” and “odont” is Greek for “tooth.” Endodontic treatment treats the inside of the tooth. Root canal treatment is one type of endodontic treatment. To understand endodontic treatment, it helps to know something about the anatomy of the tooth. Inside the tooth, under the white enamel and a hard layer called the dentin, is a soft tissue called the pulp. The pulp contains blood vessels, nerves, and connective tissue and creates the surrounding hard tissues of the tooth during development.
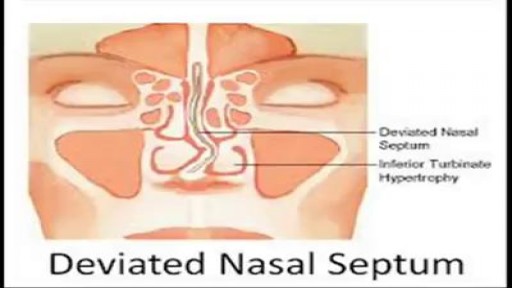
When a deviated septum is severe, it can block one side of your nose and reduce airflow, causing difficulty breathing. The additional exposure of a deviated septum to the drying effect of airflow through the nose may sometimes contribute to crusting or bleeding in certain individuals. Nasal obstruction can occur from a deviated nasal septum, from swelling of the tissues lining the nose, or from both. Treatment of nasal obstruction may include medications to reduce the swelling or nasal dilators that help open the nasal passages. To correct a deviated septum, surgery is necessar
![What does a fistula for dialysis look like? [CHT CERTIFICATION REVIEW] 2022](https://i.ytimg.com/vi/gjB5eKo4eh8/maxresdefault.jpg)
If this is the first time visiting us, make sure to subscribe to our channel here: https://bit.ly/2yXNBYp
What does a fistula for dialysis look like?
A fistula for dialysis is a surgical connection between a vein and an artery.
In this video, I will show you a real fistula and how we should evaluate it before a dialysis connection.
Additional videos:
💉How to properly cannulate a fistula: https://youtu.be/IqoHnzFyhJQ
💉 What is a fistula for dialysis treatment: https://youtu.be/B5EEf-MklFk
💉 The 10-second assessment for fistulas: https://youtu.be/Uqo0LhjZSI8
💉 If you would like to be trained as a dialysis professional focused on offering quality of care to renal patients, visit our program details here: https://utopiahcc.com/hemodialysis-technician/
For nursing and technician schools😷 🩺 🎓, we can offer a special renal failure class to your students. For inquiries please contact us: info@utopiahcc.com
Where to find us:
Facebook: https://www.facebook.com/utopiahealth
Email: info@utopiahcc.com
Website: utopiahcc.com
🤔 Looking for renal and dialysis continuing education for your certification renewal? Check out our CE package where you will get a little over 40 contact hours for a small price and receive your certificates immediately.
Here's the link: https://bit.ly/3dbPvDZ
Want to watch *Free Dialysis Training Videos*?
https://utopiahcc.com/free-dia....lysis-video-training
__________________________________________________________
Additional resources:
What Does a Healthy AV Fistula Look Like? | Azura Vascular ...
www.azuravascularcare.com infodialysisaccess healt...
Jul 17, 2018 — An AV fistula is a surgically-created permanent access located under the skin, making a direct connection between a vein and an artery. An AV fistula is typically created in the non-dominant arm. If the veins in your arm are not large or healthy enough to support a fistula, it may be created in your leg.
Preparing for Dialysis (AV Fistula) Fact Sheets Yale ...
www.yalemedicine.org › conditions › preparing-dialysi...
To undergo dialysis, patients need a surgical procedure to create an access point for the dialysis machine. An AV fistula is the most common access point.
Vascular Access for Hemodialysis - Life Options
lifeoptions.org living-with-kidney-failure vascular-a...
Jump to How a Catheter Looks and Feels — This makes a pattern that looks a bit like a rope ladder. The next best way—for fistulas ONLY—is the “Buttonhole ...
Fistula or Graft Surgery · Needle Fear · How a Fistula or Graft Looks...
Taking Care of Your Fistula - DaVita
www.davita.com dialysis preparing-for-dialysis › ta...
An arteriovenous (AV) fistula is a type of access used for hemodialysis. ... access because it utilizes the patient's own vessels and does not require permanent placement of foreign materials such ... Look for redness or swelling around the fistula area. ... This sound may change from a whooshing noise to a whistle-like sound.
Vascular Access for Hemodialysis - Department of Surgery
surgery.ucsf.edu conditions--procedures vascular-ac...
The patient does not need anesthesia for this procedure. ... A vascular surgeon performs AV graft surgery, much like AV fistula surgery, in an outpatient center or ...
Frequently Asked Questions about Dialysis Access Surgery ...
www.bidmc.org transplant-institute frequently-aske...
Dialysis access surgery creates the vascular opening so a needle can be inserted for ... fluid and to correct electrolytes like potassium, sodium, phosphate and calcium, to name a few. ... Where are AV fistulas located and how long do they last?
Fistula and Graft Placement (Eric K. Peden, MD) - YouTube
www.youtube.com watch
Mar 28, 2016 — ... Bootcamp 2015 August 14 - 16, 2015 "Dialysis Access" Fistula and Graft Placement (Eric K. Peden, MD) DICET@Houstonmethodist.org.
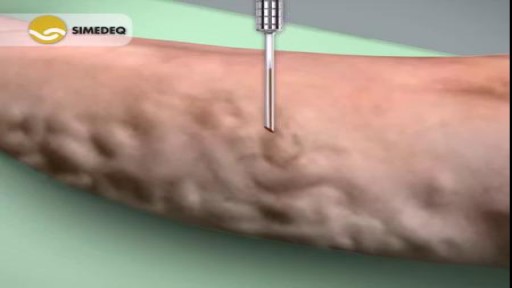
Varicose veins are generally benign. The cause of this condition is not known. For many people, there are no symptoms and varicose veins are simply a cosmetic concern. In some cases, they cause aching pain and discomfort or signal an underlying circulatory problem. Treatment involves compression stockings, exercise, or procedures to close or remove the veins.

Most intact aortic aneurysms do not produce symptoms. As they enlarge, symptoms such as abdominal pain and back pain may develop. Compression of nerve roots may cause leg pain or numbness. Untreated, aneurysms tend to become progressively larger, although the rate of enlargement is unpredictable for any individual. Rarely, clotted blood which lines most aortic aneurysms can break off and result in an embolus. They may be found on physical examination. Medical imaging is necessary to confirm the diagnosis. Symptoms may include: anxiety or feeling of stress; nausea and vomiting; clammy skin; rapid heart rate. In patients presenting with aneurysm of the arch of the aorta, a common symptom is a hoarse voice as the left recurrent laryngeal nerve (a branch of the vagus nerve) is stretched. This is due to the recurrent laryngeal nerve winding around the arch of the aorta. If an aneurysm occurs in this location, the arch of the aorta will swell, hence stretching the left recurrent laryngeal nerve. The patient therefore has a hoarse voice as the recurrent laryngeal nerve allows function and sensation in the voicebox. Abdominal aortic aneurysms, hereafter referred to as AAAs, are the most common type of aortic aneurysm. One reason for this is that elastin, the principal load-bearing protein present in the wall of the aorta, is reduced in the abdominal aorta as compared to the thoracic aorta (nearer the heart). Another is that the abdominal aorta does not possess vasa vasorum, hindering repair. Most are true aneurysms that involve all three layers (tunica intima, tunica media and tunica adventitia), and are generally asymptomatic before rupture. The most common sign for the aortic aneuysm is the Erythema nodosum also known as leg lesions typically found near the ankle area. The prevalence of AAAs increases with age, with an average age of 65–70 at the time of diagnosis. AAAs have been attributed to atherosclerosis, though other factors are involved in their formation. An AAA may remain asymptomatic indefinitely. There is a large risk of rupture once the size has reached 5 cm, though some AAAs may swell to over 15 cm in diameter before rupturing. Before rupture, an AAA may present as a large, pulsatile mass above the umbilicus. A bruit may be heard from the turbulent flow in a severe atherosclerotic aneurysm or if thrombosis occurs. Unfortunately, however, rupture is usually the first hint of AAA. Once an aneurysm has ruptured, it presents with a classic pain-hypotension-mass triad. The pain is classically reported in the abdomen, back or flank. It is usually acute, severe and constant, and may radiate through the abdomen to the back. The diagnosis of an abdominal aortic aneurysm can be confirmed at the bedside by the use of ultrasound. Rupture could be indicated by the presence of free fluid in potential abdominal spaces, such as Morison's pouch, the splenorenal space (between the spleen and left kidney), subdiaphragmatic spaces (underneath the diaphragm) and peri-vesical spaces. A contrast-enhanced abdominal CT scan is needed for confirmation. Only 10–25% of patients survive rupture due to large pre- and post-operative mortality. Annual mortality from ruptured abdominal aneurysms in the United States alone is about 15,000. Another important complication of AAA is formation of a thrombus in the aneurysm.

Mommy Makeover plastic surgery in NYC and is a fairly new phenomena. This video, from 5thavenue surgery; http://www.5thavesurgery.com, goes through a case study of a patient getting plastic surgery in NYC. Check out what a Mommy Makeover can do for your body and what Plastic Surgery can do for you.