Top videos
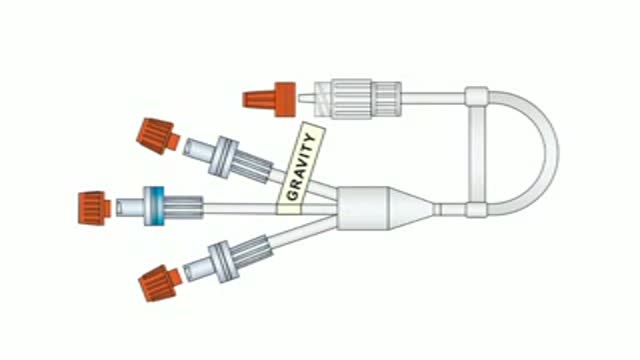
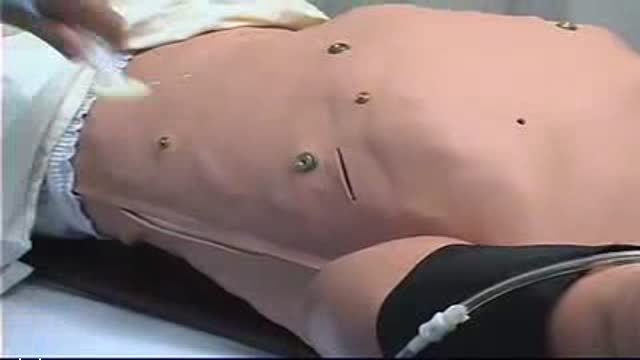
To facilitate the delivery of fluids during labour, obstetric anaesthetists from Coventry designed a triple IV peripheral connector with a central high-flow anti-reflux valve. This connector, now rightly known as the Coventry valve, can be used for all theatre settings and is especially useful in obstetrics, ICU, HDU and orthopaedics. More details on www.mediplus.co.uk
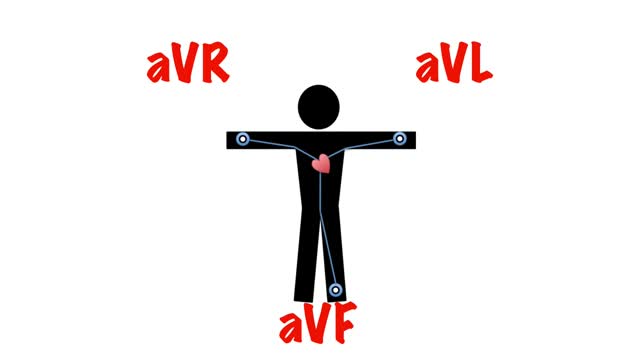
It then spreads down the bundle of his and then purkinje fibres to cause ventricular contraction. So when viewing the heart from the front, the direction of depolarisation is 11 o'clock to 5 o'clock. The general direction of depolarisation is known as the cardiac axis.
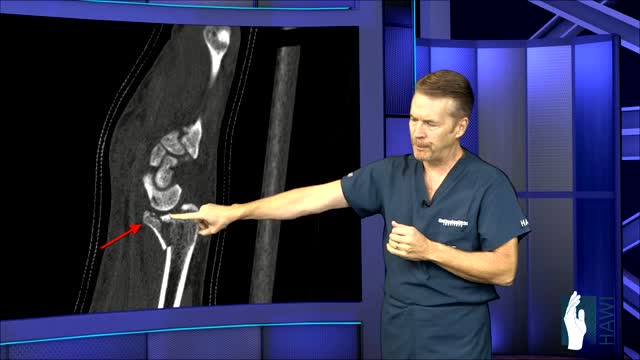
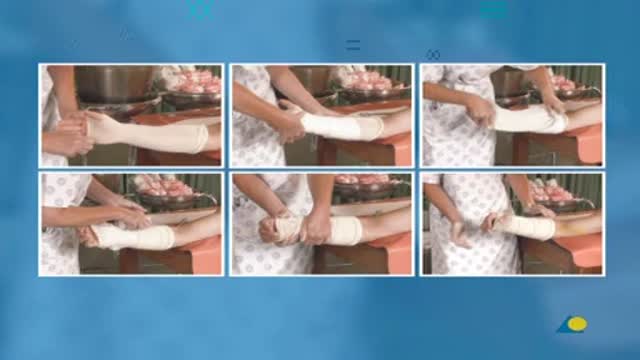
A distal radius fracture almost always occurs about 1 inch from the end of the bone. The break can occur in many different ways, however. One of the most common distal radius fractures is a Colles fracture, in which the broken fragment of the radius tilts upward. This fracture was first described in 1814 by an Irish surgeon and anatomist, Abraham Colles -- hence the name "Colles" fracture.

-Intrapartum antibiotic prophylaxis for mothers colonized with group B Streptococcus can prevent early-onset neonatal disease. Adequate prophylaxis consists of ampicillin, penicillin, or cefazolin for ;::4 hours before delivery. Regardless of intrapartum treatment, all high-risk infants must be observed for ;::49 hours. A complete blood count with differential and blood culture are indicated if the infant is preterm <37 weeks or was exposed to prolonged rupture of membranes.>18 hrs.

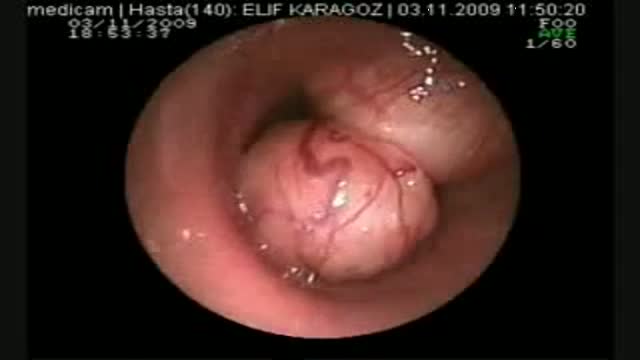
Pancreatic cysts are saclike pockets of fluid on or in your pancreas, a large organ behind the stomach that produces hormones and enzymes that help digest food. Most pancreatic cysts aren't cancerous, and many don't cause symptoms. They're typically found during imaging testing for another problem. Some are actually noncancerous (benign) pockets of fluids lined with scar or inflammatory tissue, not the type of cells found in true cysts (pseudocysts). But some pancreatic cysts can be or can become cancerous. Your doctor might take a sample of the pancreatic cyst fluid to determine if cancer cells are present. Or your doctor might recommend monitoring a cyst over time for changes that indicate cancer.

Erectile dysfunction (ED) is the inability to get or keep an erection firm enough for sexual function. It’s a common sexual problem, affecting as many as 30 million men in the United States. Most cases of ED have a physical cause, such as heart disease, diabetes, and obesity. Lifestyle choices like smoking and drinking excessive amounts of alcohol can also lead to ED. But for some men, psychological issues are the root of the problem.

Robotic-assisted endoscopic thyroid surgery using the daVinci® Surgical System can safely and effectively offer those needing thyroid surgery relief without neck incisions. Dr. Ron Kuppersmith and Dr. Andrew deJong are now performing this procedure at the College Station Medical Center in Texas.

Bartter syndrome has traditionally been classified into three main clinical variants, as follows: Neonatal (or antenatal) Bartter syndrome Classic Bartter syndrome Gitelman syndrome Advances in molecular diagnostics have revealed that Bartter syndrome results from mutations in numerous genes that affect the function of ion channels and transporters that normally mediate transepithelial salt reabsorption in the distal nephron segments. Hundreds of mutations have been identified to date. Such advances may result in the development of new therapies (see the image below). [2] (See Pathophysiology and Etiology.)
A pneumothorax can be caused by a blunt or penetrating chest injury, certain medical procedures, or damage from underlying lung disease. Or it may occur for no obvious reason. Symptoms usually include sudden chest pain and shortness of breath. On some occasions, a collapsed lung can be a life-threatening event.
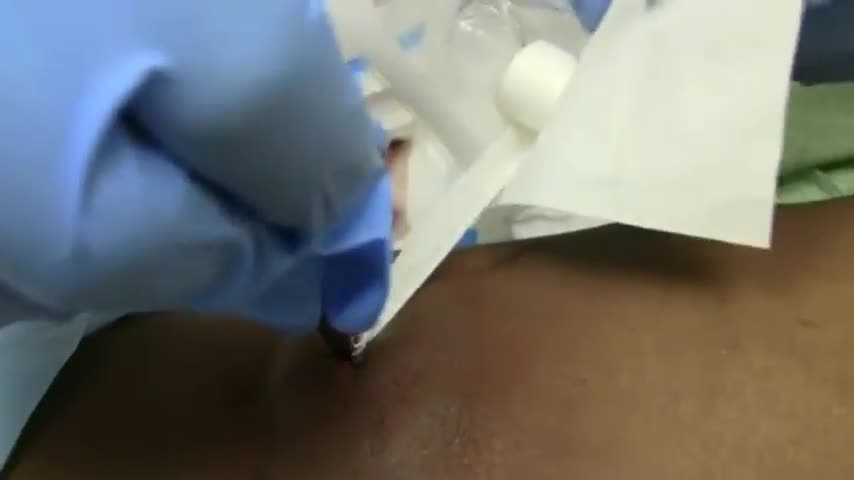
An abscess is an infectious process characterized by a collection of pus surrounded by inflamed tissue. [1, 2] Abscesses can form anywhere in the body, from a superficial skin (subcutaneous) abscess to deep abscesses in muscle, organs, or body cavities. Patients with subcutaneous skin abscesses present clinically as a firm, localized, painful, erythematous swelling that becomes fluctuant (see the image below).
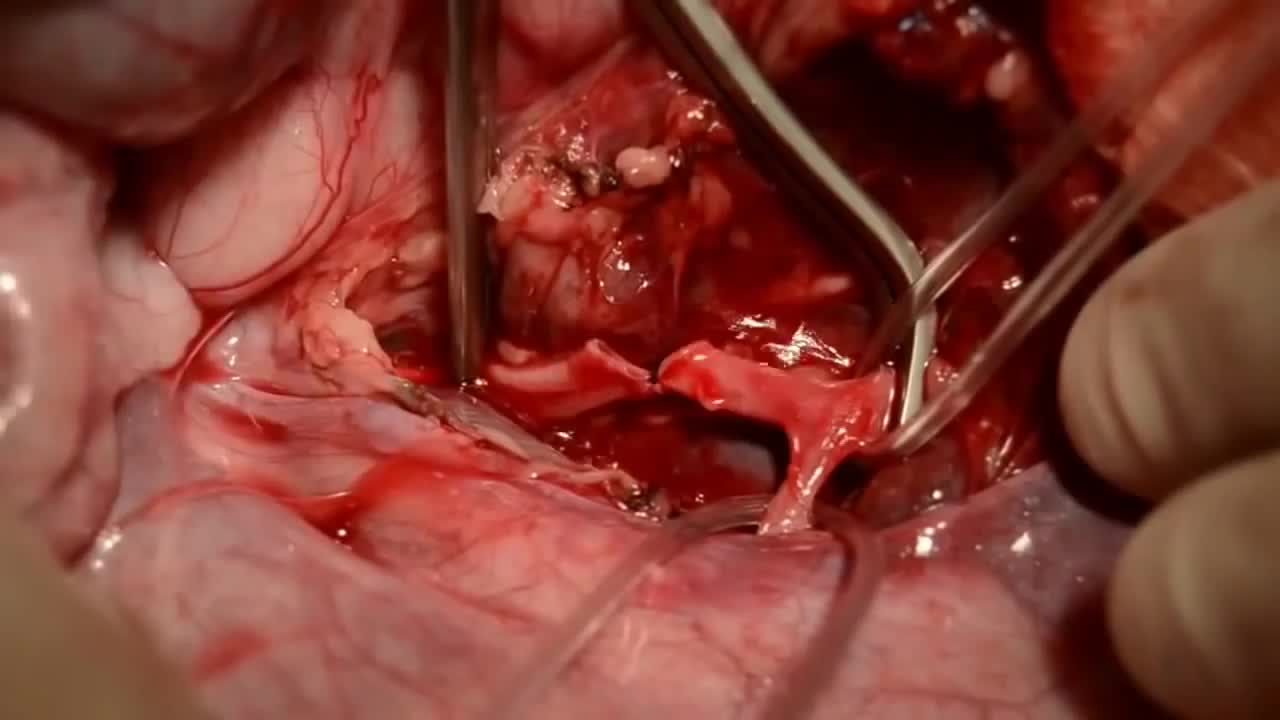
Throughout the body, there are several points at which blood vessels unite. The junctions are termed anastomoses. In the simplest sense, an anastomosis is any connection (made surgically or occurring naturally) between tube-like structures. Naturally occurring arterial anastomoses provide an alternative blood supply to target areas in cases where the primary arterial pathway is obstructed. They are most abundant in regions of the body where the blood supply may can be easily damaged or blocked (such as the joints or intestines). This article focuses on the arterial anastomotic networks of the upper limb.
Childbirth (also called labour, birth, partus or parturition) is the culmination of a human pregnancy or gestation period with birth of one or more newborn infants from a woman’s uterus. The process of normal human childbirth is categorized in three stages of labour: the shortening and dilation of the cervix, descent and birth of the infant, and birth of the placenta. In some cases, childbirth is achieved through caesarean section, the removal of the neonate through a surgical incision in the abdomen, rather than through vaginal birth
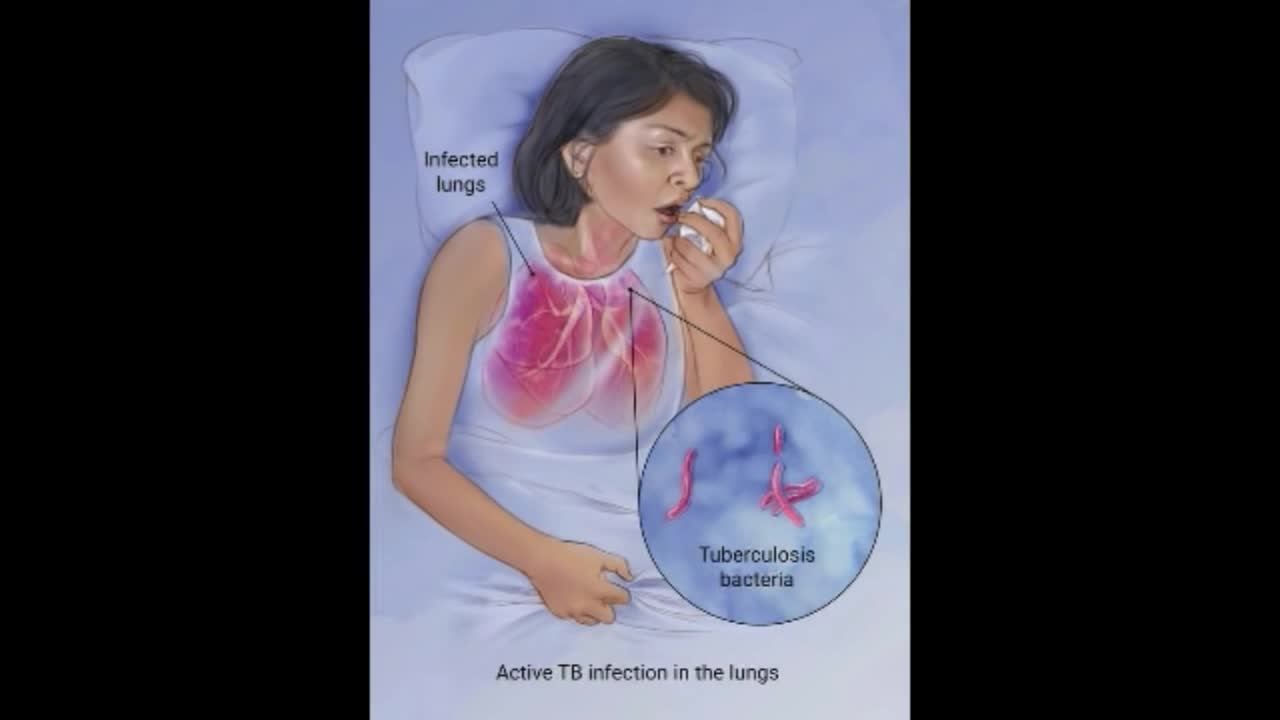
Although your body may harbor the bacteria that cause tuberculosis, your immune system usually can prevent you from becoming sick. For this reason, doctors make a distinction between: Latent TB. In this condition, you have a TB infection, but the bacteria remain in your body in an inactive state and cause no symptoms. Latent TB, also called inactive TB or TB infection, isn't contagious. It can turn into active TB, so treatment is important for the person with latent TB and to help control the spread of TB. An estimated 2 billion people have latent TB. Active TB. This condition makes you sick and can spread to others. It can occur in the first few weeks after infection with the TB bacteria, or it might occur years later. Signs and symptoms of active TB include: Coughing that lasts three or more weeks Coughing up blood Chest pain, or pain with breathing or coughing Unintentional weight loss Fatigue Fever Night sweats
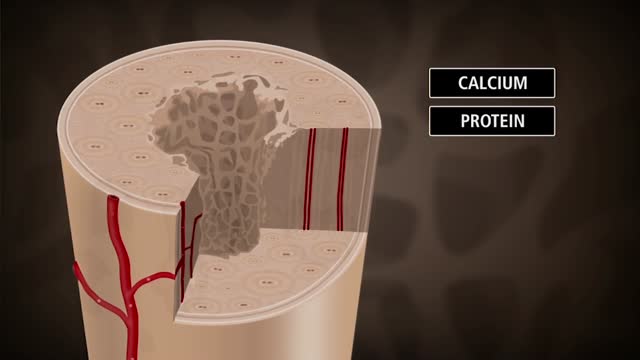
Bone is not a static part of the body — it's constantly being resorbed (broken down) and formed throughout your life. Your entire skeleton is replaced about every decade, according to the NIH. During your childhood and teenage years, bone formation occurs more quickly than bone resorption, resulting in growth. You reach your maximum bone density and strength around age 30, after which bone resorption slowly overtakes bone formation. Osteoporosis develops when there's an abnormal imbalance between bone resorption and formation — that is, resorption occurs too quickly, or formation too slowly.