Top videos

Craniectomy is neurosurgical procedure that involves removing a portion of the skull in order to relieve pressure on the underlying brain. This procedure is typically done in cases where a patient has experienced a very severe brain injury that involves significant amounts of bleeding around the brain or excessive swelling of the brain.

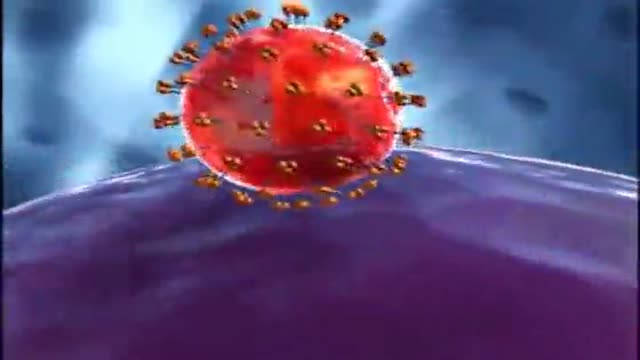
HSV-1 causes "cold sores" on the mouth, and up to 80% of the population has this virus. However, HSV-1 may also be transmitted to the genitals through oral/genital sex and about 40% of genital herpes is caused by HSV-1. Up to 22% of sexually active adults have genital herpes caused by HSV-2.
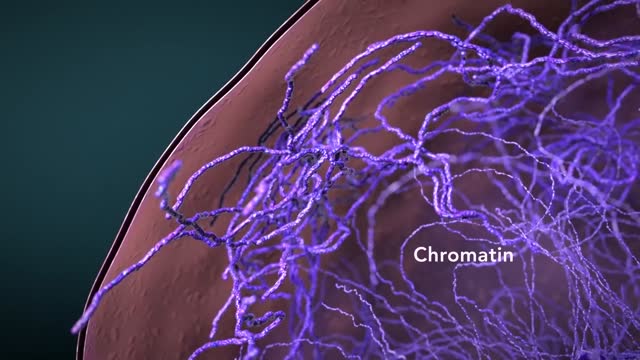
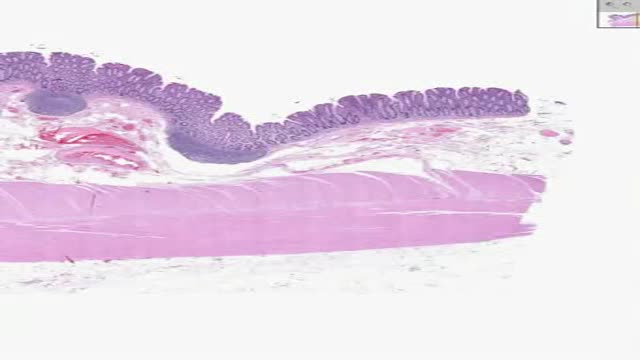
Cytoplasmic organelles are "little organs" that are suspended in the cytoplasm of the cell. Each type of organelle has a definite structure and a specific role in the function of the cell. Examples of cytoplasmic organelles are mitochondrion, ribosomes, endoplasmic reticulum, golgi apparatus, and lysosomes.

The infection is generally transmitted by direct contact with the mucus or sores of someone else with strep. Common symptoms include sore throat, fever, and swollen lymph nodes in the neck. Rarely, complications can involve the heart or kidneys. Treatment is important to reduce complications. Oral antibiotics like penicillin, amoxicillin, cephalexin, or azithromycin are commonly used. Other medicines such as acetaminophen or ibuprofen can help with pain and fever.

Amanda walks Chelsea through how to do the basics of a one leg squat, as she tries not to fall over. Do it at home, at work, or at the gym! No equipment needed! Check us out on Social Media! Facebook: https://www.facebook.com/striveptandperformance/ Instagram: https://www.instagram.com/striveptandperf/ Twitter: https://twitter.com/StrivePTandPerf Blog: http://www.strivept.ca/blog

Dr. Nick demonstrates how to numb a toe for a patient who had a subungual hematoma “collection of blood under the nail”. This patient stubbed his toe and needed to have the nail removed.
#satisfying #reaction #amazing
MAKE SURE TO SUBSCRIBE FOR ALL THE NEW SURGICAL AND EDUCATIONAL VIDEOS COMING!!
👉🏻For more information visit :
https://drnickcampi.com
👉🏻Follow me on TikTok!!
https://vm.tiktok.com/ZMeXLbc5F/I’ll
👉🏻Connect with me!!
https://www.instagram.com/drnickcampitelli
👉🏻Check out this video of how we remove an ingrown toenail!
https://youtu.be/JyZo8aZDYds
👉🏻Dr. Nick Campitelli Performs latest Minimally Invasive Bunion Surgery! Watch this video!
https://youtu.be/eRpABMsCbOU
Dr. Nick Campitelli is a podiatrist who specializes in foot and ankle surgery in the Akron and Cleveland Ohio area. He is the Residency Director of the Western Reserve Hospital / University Hospital Podiatric Medicine and Surgery Residency Program.
*** All content found on the this YouTube video including: text, images, audio, or other formats were created for informational purposes only. The Content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you heard on this video. ***
◦