Top videos

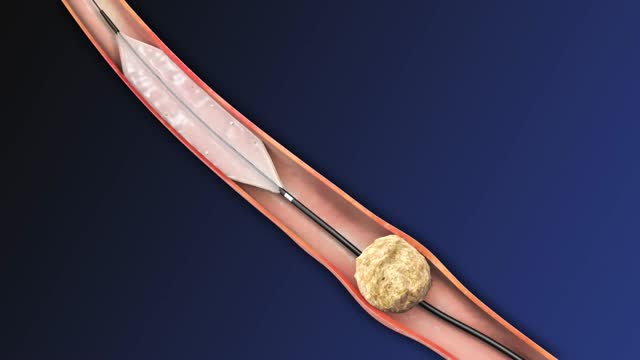
Renal artery stenosis is the narrowing of one or more arteries that carry blood to your kidneys (renal arteries). Narrowing of the arteries prevents normal amounts of oxygen-rich blood from reaching your kidneys. Your kidneys need adequate blood flow to help filter waste products and remove excess fluids. Reduced blood flow may increase blood pressure in your whole body (systemic blood pressure) and injure kidney tissue.

Macrobiopsy of breast lesions is a complicated procedure when performed with vacuum assisted biopsy tools. The Spirotome is a hand-held needle set that doesn't need capital investment, is ready to use and provides tissue samples of high quality in substantial amounts. In this way quantitative molecular biology is possible with one tissue sample. The Coramate is an automated version of this direct and frontal technology.
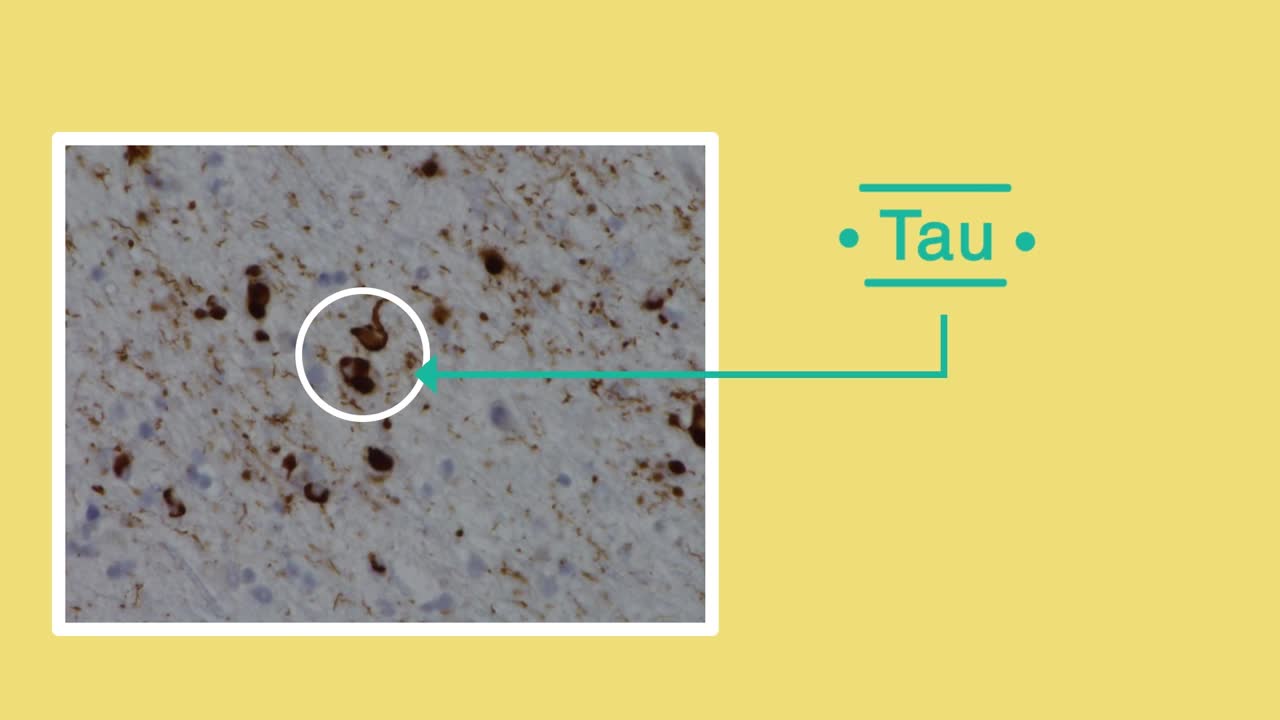
Frontotemporal dementia is the name for a range of conditions in which cells in the frontal and temporal lobes of the brain are damaged. These lobes control behaviour, emotional responses and language. This means that people will experience changes in personality and behaviour, or may struggle with language – for example, in finding the right word. Frontotemporal dementia is a less common form of dementia which is more likely to affect younger people – those under 65.
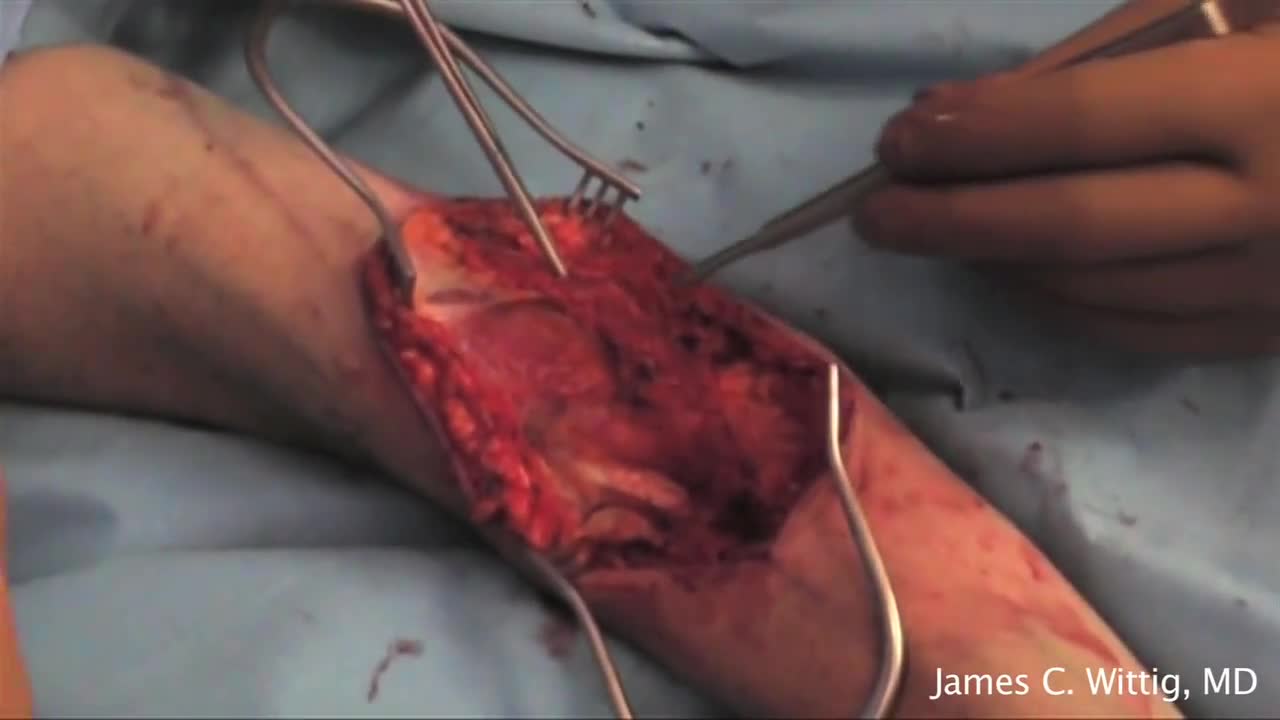
Giant cell tumour is a locally aggressive primary bone tumour, located eccentrically in the metaphysis and epiphysis of a long bone. It commonly affects distal end of Femur, proximal end of Tibia and distal end of Radius. It is occasionally reported in small bones of hand and foot[1], spine[2] and pelvis[3]. Though it occurs in 20 - 35 year old individuals commonly, it can also be seen in children as young as 2 years[4] and also in older individuals
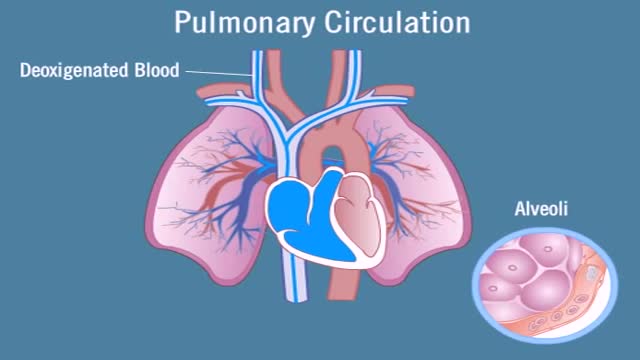
Pulmonary circulation is the portion of the cardiovascular system which carries deoxygenated blood away from the heart, to the lungs, and returns oxygenated (oxygen-rich) blood back to the heart. The function of pulmonary circulation is to exchange carbon dioxide for oxygen in the blood. It is the passage of blood from the heart to the capillaries of the lungs, where the gases are exchanged, and back to the heart to be pumped around the body.

This video is brought to you by the Stanford Medicine 25 to teach you the common causes of shoulder pain and how to diagnose them by the physical exam.
The Stanford Medicine 25 program for bedside medicine at the Stanford School of Medicine aims to promote the culture of bedside medicine to make current and future clinicians and other healthcare provides better at the art of physical diagnosis and more confident at the bedside of their patients.
Visit us:
Website: http://stanfordmedicine25.stanford.edu/
Blog: http://stanfordmedicine25.stanford.edu/blog.html
Facebook: https://www.facebook.com/StanfordMedicine25
Twitter: https://twitter.com/StanfordMed25
Diagnoses covered in this video:
Rotator Cuff Pathology
Impingement Syndrome
Biceps Tendinopathy
Adhesive Capsulitis (Frozen Shoulder)
Acromioclavicular (AC) Joint Disease
Shoulder Instability
Labral Tears (SLAP Lesions)
A new and safer method of inserting a Foley catheter suprapubically. The technique allows the insertion to be carried out in an Outpatient setting, thus saving time, cost and effort. By using the Seldinger technique, the product reduces the chances of bowel or bladder perforation and resultant morbidity.
The product has been chosen by The NHS National Technology Adoption Centre to help facilitate adoption of the product.
See www.mediplus.co.uk for more information

A 29 years old man lost his left wrist in car turn over in 2014. this video is taken 1 year after replantation. You can see another videos in my site: https://drliaghatclinic.com, https://instagram.com/liaghatclinic, https://t.me/liaghatclinic
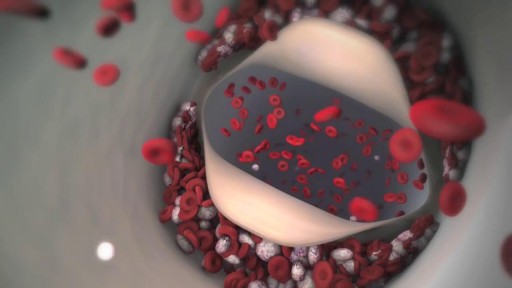
Symptoms of blood clots in specific body locations are as follows: Symptoms of blood clots in legs (deep vein thrombosis (DVT) are pain, redness, and swelling. Symptoms of an arterial blood clot in a limb (leg or arm) include pain, pale color, and coolness to the touch. and the leg is cool and pale.

The most common symptoms of pneumoconiosis are cough and shortness of breath. The risk is generally higher when people have been exposed to mineral dusts in high concentrations and/or for long periods of time. Inadequate or inconsistent use of personal protective equipment (PPE) such as respirators (specially fitted protective masks) is another risk factor since preventing dusts from being inhaled will also prevent pneumoconiosis. Pneumoconiosis does not generally occur from environmental (non-workplace) exposures since dust levels in the environment are much lower.