Top videos

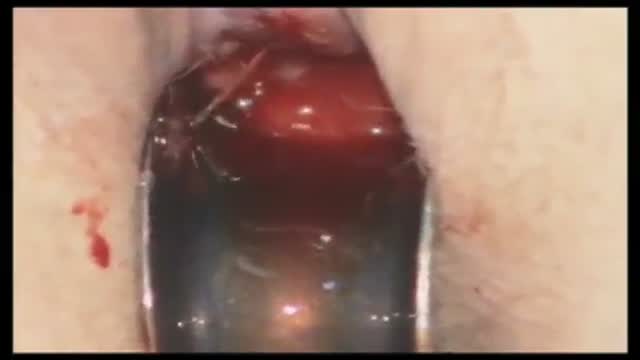
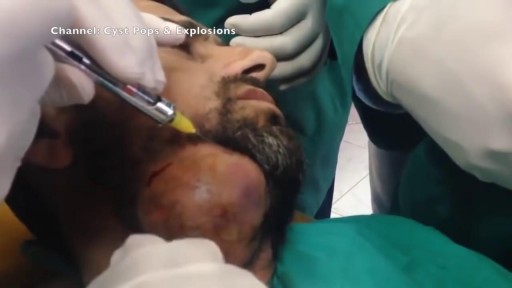
For benign colorectal diseases, totally laparoscopic left-sided colectomy was already reported on some papers. Nowadays, there is increasingly demanded minimally invasive surgerys on malignant bowel diseases including colorectal cancers and so we developed the new techniques in that specimen is del...ivered through the open rectal stump, especially, using Sani Sleeve(TM). In this operation video, you can see that an anvil was fixed to proximal colonic stump with intracorporeal purse-string suture using Endo-stitch(TM). (SETA : Specimen Extraction Through Anus)

Delayed puberty is defined as the absence of any signs suggestive of puberty by 14 years of age. In this case, the patient's pubertal delay appears to be constitutional because of his positive family history, absence of syndromic features or systemic illness, and bone age of 12 years. Puberty correlates more closely with bone age than chronological age. On follow-up, the patient will most likely demonstrate a similar onset of puberty as his father.

Symptoms of liver failure include vomiting, diarrhea and fatigue as well as the symptoms from stage 3. While the progression from cirrhosis to failure can take years, the damage is irreversible and leads to eventual death. The key to treating liver disease is to diagnose the condition as early as possible.

Medications are the most proven, effective way to treat gout symptoms. However, making certain lifestyle changes also may help, such as: Limiting alcoholic beverages and drinks sweetened with fruit sugar (fructose). Instead, drink plenty of nonalcoholic beverages, especially water. Limit intake of foods high in purines, such as red meat, organ meats and seafood. Exercising regularly and losing weight. Keeping your body at a healthy weight reduces your risk of gout.
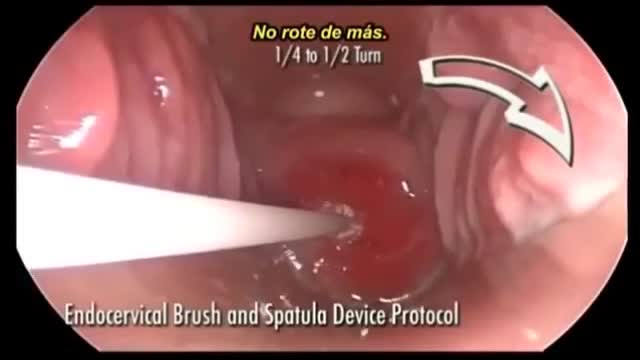
In patients age ;::25, HPV DNA testing is the preferred next step in management if the initial cytology shows ASC-US. In this method, samples are collected for both cytology and reflex HPV DNA. If cytology results are positive, HPV DNA testing is performed. If cytology results are negative, the sample for HPV DNA is discarded. HPV DNA testing along with Pap smear at 3 years is recommended if initial cytology shows ASC-US but HPV DNA testing is negative

This is part 2 Herbal Medicine. Lecture presented to the International Congress of Pediatric Hepatology Sharm 2009. It is one of a series of lectures discussing the Alternative medicine practices with critical appraisal and measure the evidence.

Ellis demonstrates how to administer an intradermal, subcutaneous, and intramuscular injection.
Our Critical Nursing Skills video tutorial series is taught by Ellis Parker MSN, RN-BC, CNE, CHS and intended to help RN and PN nursing students study for your nursing school exams, including the ATI, HESI and NCLEX.
#NCLEX #ClinicalSkills #injections #HESI #Kaplan #ATI #NursingSchool #NursingStudent #Nurse #RN #PN #Education #LVN #LPN #nurseeducator
00:00 What to expect
00:20 Intradermal injections
00:35 Cleaning site
00:54 Explaining bevel up
1:40 Inserting needle
2:00 Injecting medication
2:16 Withdrawing needle
2:29 Subcutaneous Injections
2:39 Selecting site for subcutaneous injections
3:08 Cleaning subcutaneous injections site
3:18 Pinching subcutaneous injections site
3:30 Inserting needle subcutaneous injections
4:13 Injecting medication subcutaneous injections
4:23 Post injection
4:36 Intramuscular injection
4:54 Locating intramuscular injection site
5:18 Cleaning intramuscular injection site
5:38 Inserting needle intramuscular injection
6:28 Anchoring needle intramuscular injection
6:44 Injecting medication intramuscular injection
6:55 Withdrawing needle intramuscular injection
7:05 Disposing of needle
7:43 Cleaning site
8:00 Displacing with Z-track
8:10 Inserting needle
8:23 Releasing tissue
🚨 Reminder: shipping deadlines are looming 👀
🎁 Regular Shipping: Order by Friday, December 15
🚀 Expedited Shipping: Order by Monday, December 18
🔍 Still searching for last-minute gifts? Consider a Level Up RN Gift Card! 💌 It’s not only a thoughtful present but also the perfect way to share treasures like Pharmacology Flashcards OR digital treasures like Flashables Digital Nursing Flashcards & the Level Up RN membership. Give the gift of knowledge this holiday season! 🧠⚡️💖 bit.ly/LevelUpRNGC
🚪 Access our Cram Courses, Quizzes and Videos all in one ad free space with Level Up RN Membership https://bit.ly/LevelUpRNMembership
Want more ways to MASTER Clinical Skills? Check out our flashcards & videos!
👇👇👇👇👇👇👇👇👇👇
👉 https://bit.ly/clinicalnursingskills 👈
☝️👆☝️👆☝️👆☝️👆☝️👆
This is your one-stop-shop for materials to help you LEARN & REVIEW so you can PASS Nursing School.
🤔🤔🤔 DO YOU WANT TO PASS your classes, proctored exams and the NCLEX? 🤔🤔🤔 Our resources are the best you can buy. They are built with a single goal: help you pass with no fluff. Everything you need, and nothing you don’t. Don’t take our word for it, though! Check out our hundreds of ⭐️⭐️⭐️⭐️⭐️ reviews from nurses who passed their exams and the NCLEX with Level Up RN.
🗂️ Our Ultimate Nursing School Survival kit is your number 1 resource to get through nursing school and to pass the NCLEX. Whether you're just starting school or you’re already prepping for the NCLEX, this bundle of flashcards is the best you can buy. It covers all the information you need to know to pass all your exams and it has FREE shipping!
➡️ https://bit.ly/TUNSSK ⬅️
L👀king for EVEN MORE resources to survive Nursing School? Make your Nursing School experience your own! Life’s difficult enough—learning shouldn’t be.
🪅 Games https://nursesquad.com
💻 Digital resources https://bit.ly/NursingStudyCourses
📅 Organizational tools https://bit.ly/OrganizingSchool
✨Want perks? Join our channel!
https://youtube.com/leveluprn/join
🏷 Head to https://leveluprn.com/specials for all our latest deals!🥳️
📧 LOOKING FOR FREE RESOURCES TO HELP WITH YOUR EXAMS? Get exclusive tips, latest video releases and more delivered to your email!
➡️ https://leveluprn.com/signup ⬅️
⚕ 👩 LEVEL UP NURSE SQUAD 👩⚕️
All of the nurses at Level Up RN are here to help! Cathy Parkes started helping her fellow classmates back when she was in nursing school, tutoring so they could pass their exams and graduate. After she got her BSN and started working as an RN at Scripps Encinitas Hospital, she started this YouTube channel to help nursing students around the world. Since then she has built a team of top-notch dedicated nurses and nurse educators who are focused on improving nursing education and supporting career advancement for nurses everywhere. With flashcards, videos, courses, organizational tools and more, we are singularly focused on helping students and nurses Level Up on their exams and nursing careers.

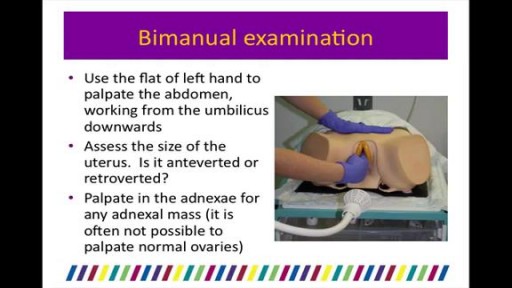
Pelvic organ prolapse occurs when a pelvic organ-such as your bladder-drops (prolapses) from its normal place in your lower belly and pushes against the walls of your vagina. This can happen when the muscles that hold your pelvic organs in place get weak or stretched from childbirth or surgery.

It’s not tummy tuck procedure.. it’s liposuction only.. don’t get confused with both procedure..
#beforeandafter #kmc #nose #aesthetic #antiaging #beauty #drhabibhairtransplant #peshawar #nose #islamabad #swat #kohat #nowshehra #karakin #mardan
How to start a peripheral IV in the dorsum of the hand: clinical nursing skill technique.
Starting an IV (intravenous catheter) can be an intimidating experience for nurses, especially nursing students and new nurses. However, nurses will perform IV insertions often, so this is an important nursing skill to learn.
Before starting an IV, always follow the protocols of your facility, as well as manufacturer's instructions for any supplies used.
In this video, Nurse Sarah demonstrates how to start a peripheral IV in the dorsum of the hand. Prior to inserting the IV, you'll want to do the following:
-Gather supplies
-Perform hand hygiene
-Prepare supplies (including priming the saline flush, removing air from extension tubing, opening packages, completing labels, and any other steps required by your facility.
-Locate a suitable vein
-Perform hand hygiene
-Don gloves
If the patient has a lot of hair, you might want to use clippers to trim the hairs prior to starting the IV. You may also apply a tourniquet to help veins move near the surface of the skin.
Next, you'll want to clean the site using the cleaner that came in the IV start kit, such as ChloraPrep.
Once the site has dried completely, you can insert the IV. Stabilize the vein with your non-dominant hand, and insert the IV's needle into the vein, watching carefully for blood return (or a blood flash) in the chamber. Advance the IV around 2mm more to ensure the plastic cannula is in the vein, then thread the cannula into the vein and press the needle safety button.
Notes: https://www.registerednursern.....com/how-to-start-an-
IV Video Series: https://www.youtube.com/watch?v=MbG_1-_mnoo&list=PLQrdx7rRsKfXr6kruqEpIovf66sxo0gxh
This video also demonstrates how to flush the IV using the push-pause method, how to secure the IV using the Tegaderm dressing that came with the IV start kit, considerations of the different cap types and the clamp sequence, and more.
For more information, watch the complete tutorial.
#nurse #nursing #iv #startiv #ivtherapy
Website: https://www.registerednursern.com/
More Videos: https://www.youtube.com/watch?v=R2XMro13dD0&list=UUPyMN8DzkFl2__xnTEiGZ1w
Nursing Gear: https://teespring.com/stores/registerednursern
Instagram: https://www.instagram.com/registerednursern_com/
Facebook: https://www.facebook.com/RegisteredNurseRNs
Twitter: https://twitter.com/NursesRN
Popular Playlists:
NCLEX Reviews: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Fluid & Electrolytes: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Nursing Skills: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
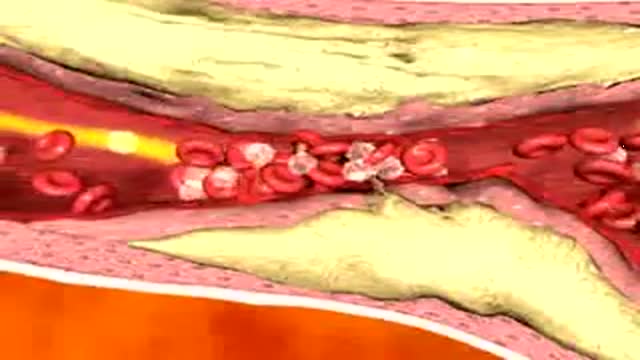
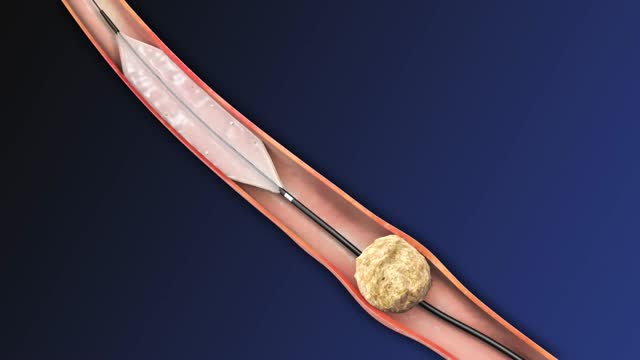
In this animation it depicts an artery with cholesterol plaque (the yellowish area) which is blocking most of the inside of this artery. Then small cells called platelets become clumped together and cause the red blood cells to form a clot. This is what causes a HEART ATTACK.