Top videos
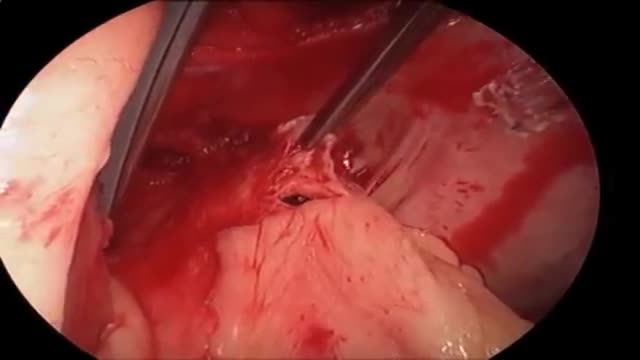
Massive PE causing hemodynamic instability (shock and/or low blood pressure, defined as a systolic blood pressure <90 mmHg or a pressure drop of 40 mmHg for >15 min if not caused by new-onset arrhythmia, hypovolemia or sepsis) is an indication for thrombolysis, the enzymatic destruction of the clot with medication.

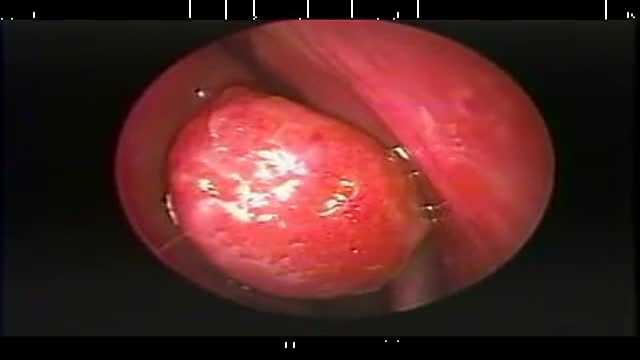
Strep throat is a bacterial infection that can make your throat feel sore and scratchy. Strep throat accounts for only a small portion of sore throats. If untreated, strep throat can cause complications, such as kidney inflammation or rheumatic fever. Rheumatic fever can lead to painful and inflamed joints, a specific type of rash or heart valve damage. Strep throat is most common in children, but it affects people of all ages. If you or your child has signs or symptoms of strep throat, see your doctor for prompt testing and treatment.

Robotic-assisted endoscopic thyroid surgery using the daVinci® Surgical System can safely and effectively offer those needing thyroid surgery relief without neck incisions. Dr. Ron Kuppersmith and Dr. Andrew deJong are now performing this procedure at the College Station Medical Center in Texas.
Asthma is a condition in which your airways narrow and swell and produce extra mucus. This can make breathing difficult and trigger coughing, wheezing and shortness of breath. For some people, asthma is a minor nuisance. For others, it can be a major problem that interferes with daily activities and may lead to a life-threatening asthma attack. Asthma can't be cured, but its symptoms can be controlled. Because asthma often changes over time, it's important that you work with your doctor to track your signs and symptoms and adjust treatment as needed.
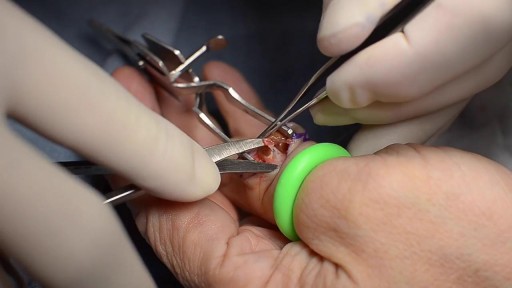
Giant cell tumors of the tendon sheath are common lesions and are the second most frequent tumors in the hand, after synovial cysts. They are diagnosed by means of clinical examination and complementary examinations (simple radiography and magnetic resonance). Erosion and invasion of the phalangeal bone affected may be seen on radiological examination. Magnetic resonance may show a “fluorescent or radiant effect” may be observed, caused by the high quantity of hemosiderin inside the tumor. Surgical treatment is the commonest practice, and complete excision is important for avoiding recurrence of the tumor, especially when bone invasion is observed on imaging examinations, which is generally related to greater tumor recurrence. In this paper, a case of a giant cell tumor of the tendon sheath in the middle phalanx of the third finger of a 45-year-old female patient is presented. This was successfully treated by means of surgery using a double access approach (dorsal and volar)

► Sign up here and try our FREE content: http://lectur.io/freecontentyt
► If you’re an medical educator or faculty member, visit: http://lectur.io/medytb2u
► WATCH the complete course on http://lectur.io/histology3
► LEARN ABOUT:
- Overview of the course
- Cells and basic tissues
- Human organ system
► THE PROF:
Your lecturer is Professor Geoff Meyer. He is currently teaching at the School of Anatomy, Physiology and Human Biology at the University of Western Australia (UWA). As an leading anatomy and histology expert he is also coordinator of the Federative International Program for Anatomical Terminologies (FIPAT) of the International Federation of Associations of Anatomists (IFAA). Aside from medical research on the ovarian function, steroidogenesis, corpus luteum, angiogenesis and microcirculation Geoff Meyer’s research activities focus on developing innovative, computer-aided learning and teaching tools. Being such innovative, Geoff Meyer has received a number of awards for his work, including the Australian University Teaching Award.
► LECTURIO is your single-point resource for medical school:
Study for your classes, USMLE Step 1, USMLE Step 2, MCAT or MBBS with video lectures by world-class professors, recall & USMLE-style questions and textbook articles. Create your free account now: http://lectur.io/histology3
► INSTALL our free Lecturio app
iTunes Store: https://app.adjust.com/z21zrf
Play Store: https://app.adjust.com/b01fak
► READ TEXTBOOK ARTICLES related to this video: http://lectur.io/histolibrary
► SUBSCRIBE to our YouTube channel: http://lectur.io/subscribe
► WATCH MORE ON YOUTUBE: http://lectur.io/playlists
► LET’S CONNECT:
• Facebook: https://www.facebook.com/lectu....rio.medical.educatio
• Instagram: https://www.instagram.com/lecturio_medical_videos
• Pinterest: https://www.pinterest.de/lecturiomedical
• LinkedIn: https://www.linkedin.com/company/lecturio-medical/

TV interview with Adina Nack, Ph.D. about her own cervical HPV experiences, STD research, her new book (Damaged Goods? Women Living with Incurable Sexually Transmitted Diseases), and women's lives after genital warts, HPV and herpes infections. More info is available on STDdatings.com, which is the official STD dating & support site.