Top videos
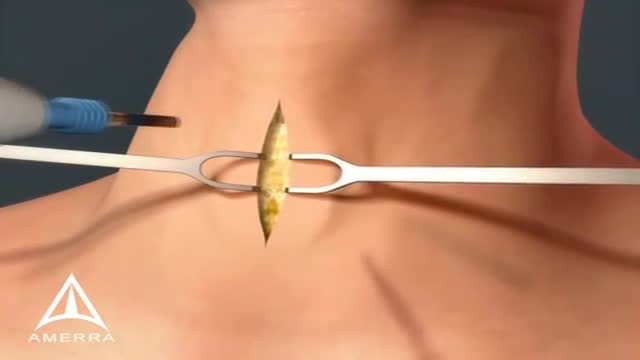
A tracheotomy or a tracheostomy: is simply an opening surgically created through the neck into the trachea (windpipe) to allow direct access to the breathing tube and is commonly done in an operating room under general anesthesia. A tube is usually placed through this opening to provide an airway and to remove secretions from the lungs. Breathing is done through the tracheostomy tube rather than through the nose and mouth. The term “tracheotomy” refers to the incision into the trachea (windpipe) that forms a temporary or permanent opening, which is called a “tracheostomy,” however; the terms are sometimes used interchangeably.
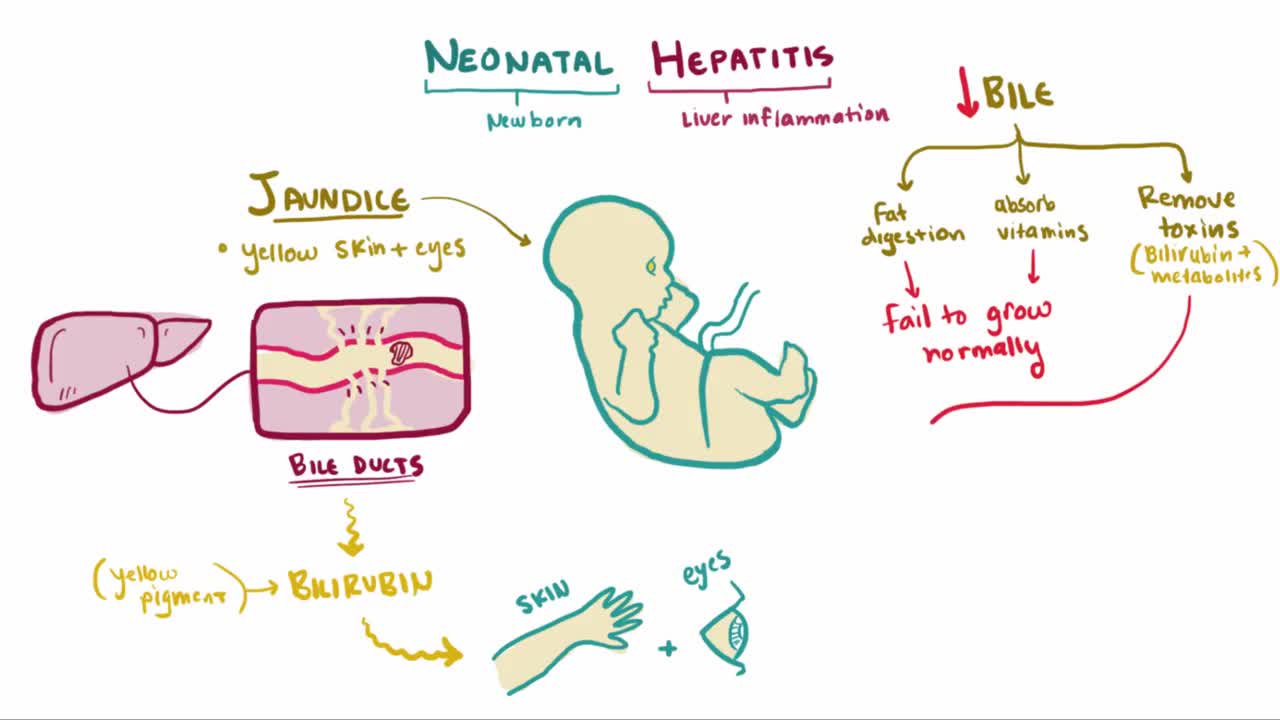
As the liver becomes more severely damaged, more obvious and serious symptoms can develop, such as: yellowing of the skin and whites of the eyes (jaundice) swelling in the legs, ankles and feet, due to a build-up of fluid (oedema) swelling in your abdomen, due to a build-up of fluid known as ascites.

The discussion begins with a basic explanation of Bone biology taking into consideration the osteoblast and osteoclast balance. Concepts of RANK, RANK ligand and Osteoprotegerin are included. Risk factors for Osteoporosis such as Age, alcohol, smoking, sedentary lifestyle are also discussed.

If your levels are too low, you have hypothyroidism and may not be ovulating as you should. Taking the right dose of thyroxine, the hormone you lack, can restore your fertility. You may have discovered your underactive thyroid as a result of trying to get pregnant.
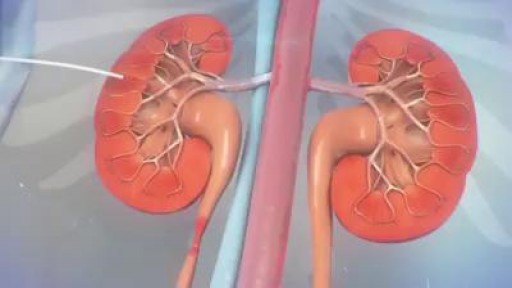
The ureter can become obstructed due to conditions such as kidney stones, tumors, infection, or blood clots. When this happens, physicians can use image guidance to place stents or tubes in the ureter to restore the flow of urine to the bladder. A ureteral stent is a thin, flexible tube threaded into the ureter.
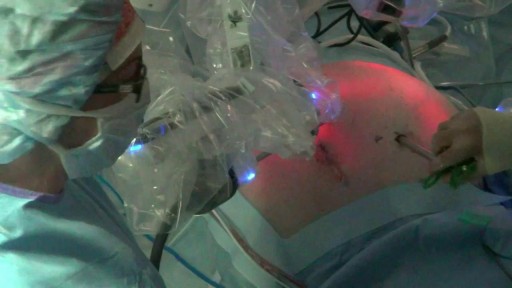
Splenectomy is a surgical procedure to remove your spleen. The spleen is an organ that sits under your rib cage on the upper left side of your abdomen. It helps fight infection and filters unneeded material, such as old or damaged blood cells. With the da Vinci Surgical System, Dr. Olson operates through just a few small incisions. The da Vinci System features a magnified 3D high-definition vision system and tiny wristed instruments that bend and rotate far greater than the human hand. As a result, da Vinci enables surgeons to operate with enhanced vision, precision and control.

How To Stop Hair Loss Naturally, Hair Regrowth Shampoo, Tips For Hair Regrowth, Hair Loss Stop--- http://how-to-regrow-your-hair.info-pro.co/ --- Natural Hair Regrowth Treatment, Looking for ideas on natural hair regrowth treatment? There are actually a lot of safe and effective natural methods that you can try in order to reverse hair loss. So what are those natural methods? Here are some of them: Eat your way to better hair: Hard to believe isn’t it? To think that what you’re actually eating can affect your hair in so many ways, positively and negatively. Want to slow down the process of hair loss and get your hair back to the healthy original state you always remembered it in? Then you might want to start transitioning over to a low fat high fiber diet. Aside from this, you’ll also want to concentrate on foods that contain biotins, which play an essential role in maintaining healthy hair. Fish, cooked eggs, whole milk, and various nuts and fruits – all of these are good sources of biotins so it’s best that you take note of them. Drink plenty of water: It’s not only that gets thirsty, as even your hair requires the moisture that water provides. Dehydration can lead to symptoms like constipation, eczema, thick dandruff, wrinkly skin, foul breath and hair loss. Remember that your body is made up of 98% water and you need to maintain it at optimum levels if you want to keep your hair in place. An easy way to quickly replenish and establish enough water in your body is to routinely drink at least 8 ounces of water immediately after you urinate. You’ll know you’re getting enough water when you observe that you are urinating more frequently. Supplements: The fact that you are experiencing hair loss is a surefire indication that something is amiss in the nutrition department. If you are however looking for a definitive guide on the products that will be available, one useful source you can use will be found at http://how-to-regrow-your-hair.info-pro.co/

Sialadenitis is an infection of the salivary glands. It is usually caused by a virus or bacteria . The parotid (in front of the ear) and submandibular (under the chin) glands are most commonly affected. Sialadenitis may be associated with pain, tenderness, redness, and gradual, localized swelling of the affected area.

Dr. David Sneed of Aesthetica Med Spa in Austin discusses the latest liposuction technique known as Body Jet Water Liposuction - which is quickly gaining popularity due to the procedure being less invasive than traditional liposuction techniques, therefore minimizing recovery time and pain.
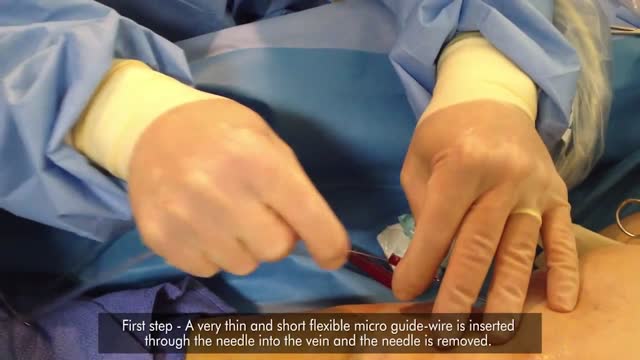
It can treat spider veins and tiny varicose veins just under the skin's surface. ... (If you have poor blood circulation feeding these tiny veins, the larger "feeder" vein must first be treated with surgery, endovenous laser or radiofrequency treatment, or sclerotherapy.) Endovenous laser treatment.
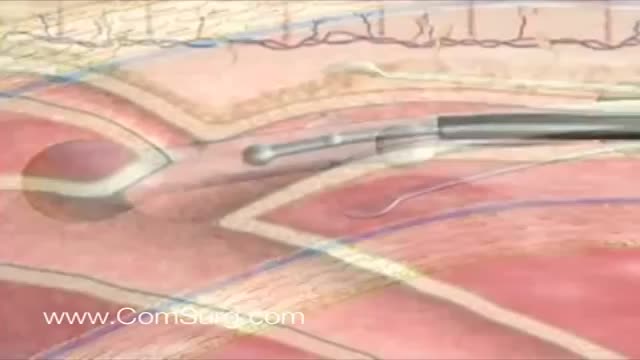
Like the VenaCure EVLT® procedure, which uses a laser to ablate the varicose vein, VNUS RF treatment is an alternative to more invasive leg stripping surgery. It is used primarily to treat the great saphenous veins (GSV), small saphenous vein (SSV), and other superficial veins in the legs.

Dr. Rowe shows how to quickly fix knee popping, clicking, and cracking sounds.
This exercise will focus on lengthening tight muscles and tendons that may be causing a noisy knee. It's especially good for osteoarthritis (wear and tear arthritis) of the knee.
It can be done at home, requires no equipment, and may also give knee pain relief... even within seconds.
Let us know how it works for you!
***************************
Dr. Michael Rowe
St. Joseph, Michigan chiropractor
If you are looking for effective neck, back, or sciatica pain relief, contact us at 269-408-8439 or visit us at https://www.BestSpineCare.com
Facebook: https://www.facebook.com/bestspinecare
Twitter: https://www.twitter.com/stjoechiro
Instagram: https://www.instagram.com/stjoechiro
Your local St. Joseph | Benton Harbor | Stevensville Michigan chiropractor
SpineCare Decompression and Chiropractic Center
3134 Niles Rd
Saint Joseph, MI 49085
**MEDICAL DISCLAIMER**
All information, content, and material of this video or website is for informational and demonstration purposes only. It is not intended to serve as a substitute for the consultation, diagnosis, and/or medical treatment of a qualified physician or healthcare provider.
Don’t use this content as a replacement for treatment and advice given by your doctor or health care provider. Consult with your doctor or healthcare professional before doing anything contained in this content.
By watching this video, you agree to indemnify and hold harmless SpineCare Decompression and Chiropractic Center (and its representatives) for any and all losses, injuries, or damages resulting from any and all claims that arise from your use or misuse of this content. SpineCare Decompression and Chiropractic Center makes no representations about the accuracy or suitability of this content.
USE OF THIS CONTENT IS AT YOUR OWN RISK.
- AFFILIATE DISCLAIMER -
We may receive commissions when you click on this video's links and make purchases. This helps support our channel so we can continue to give you helpful content.
#kneepain #kneepainrelief #kneearthritis

Atrial flutter is a type of abnormal heart rate, or arrhythmia. It occurs when the upper chambers of your heart beat too fast. When the chambers in the top of your heart (atria) beat faster than the bottom ones (ventricles), it complicates your heart rhythm

A stepwise approach to the causes and diagnosis of Anaemia in clinical practice. This presentation includes the all important concept of the Reticulocyte production index. Discussion of Hereditary and acquired causes of Anaemia has been included in detail.