Top videos

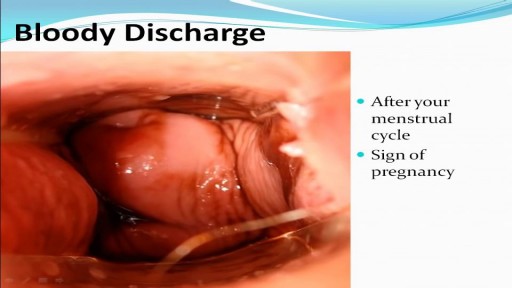
Pancreatic cysts are saclike pockets of fluid on or in your pancreas, a large organ behind the stomach that produces hormones and enzymes that help digest food. Most pancreatic cysts aren't cancerous, and many don't cause symptoms. They're typically found during imaging testing for another problem. Some are actually noncancerous (benign) pockets of fluids lined with scar or inflammatory tissue, not the type of cells found in true cysts (pseudocysts). But some pancreatic cysts can be or can become cancerous. Your doctor might take a sample of the pancreatic cyst fluid to determine if cancer cells are present. Or your doctor might recommend monitoring a cyst over time for changes that indicate cancer.
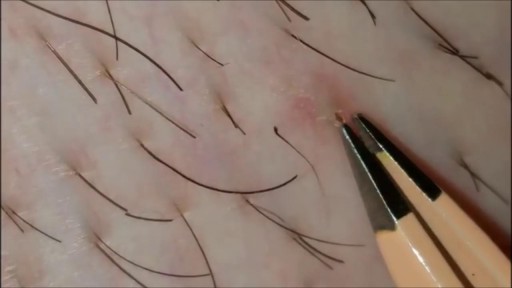
What is an ingrown hair cyst? An ingrown hair cyst refers to an ingrown hair that turns into a cyst — a large bump that extends between the skin’s surface and deep underneath it. The appearance is a cross between a regular ingrown hair and an acne cyst, though this is a different condition. These types of cysts are common among people who shave, wax, or use other methods to remove their hair. Although you may be eager to get rid of these cysts simply because of their appearance, it’s also important to watch for signs of an infection. Keep reading to learn what causes these cysts to form, plus how to treat them and prevent them from returning.
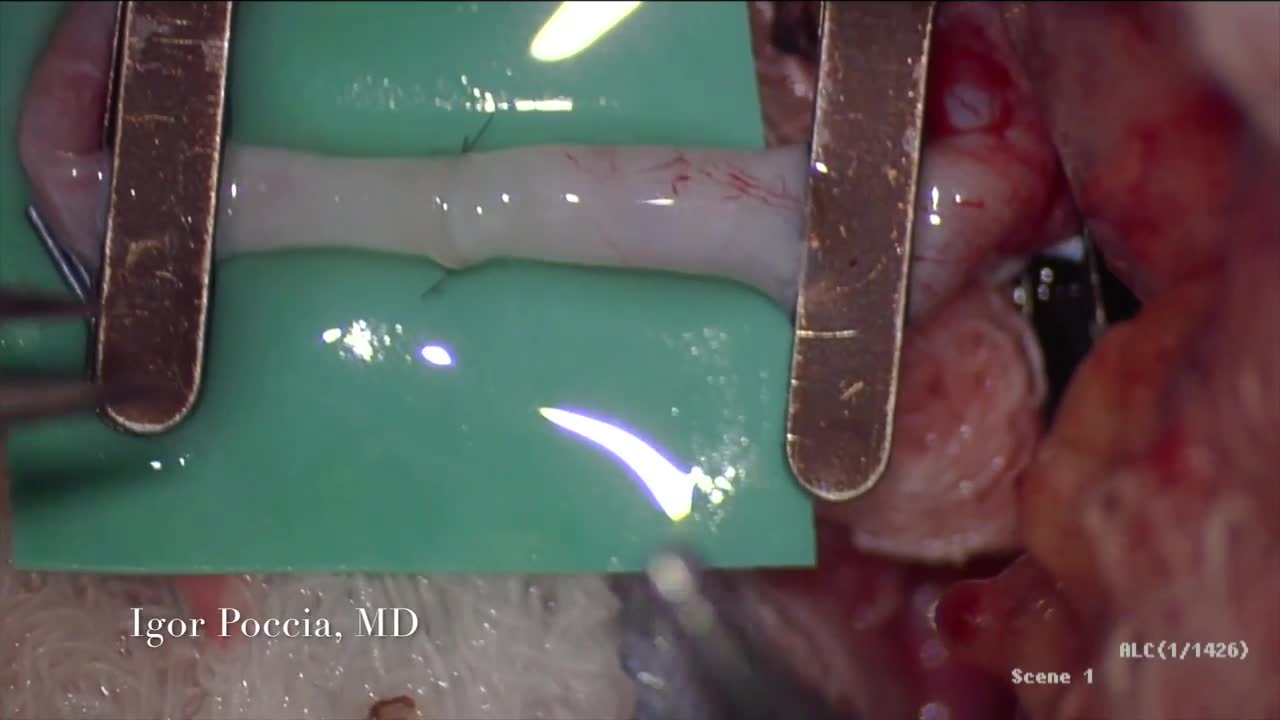
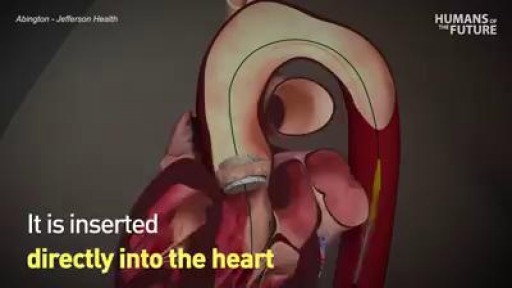
A circulatory anastomosis is a connection (an anastomosis) between two blood vessels, such as between arteries (arterio-arterial anastomosis), between veins (veno-venous anastomosis) or between an artery and a vein (arterio-venous anastomosis). An end artery (or terminal artery) is an artery that is the only supply of oxygenated blood to a portion of tissue. Examples of an end artery include the splenic artery that supplies the spleen and the renal artery that supplies the kidneys.

Macrobiopsy of breast lesions is a complicated procedure when performed with vacuum assisted biopsy tools. The Spirotome is a hand-held needle set that doesn't need capital investment, is ready to use and provides tissue samples of high quality in substantial amounts. In this way quantitative molecular biology is possible with one tissue sample. The Coramate is an automated version of this direct and frontal technology.
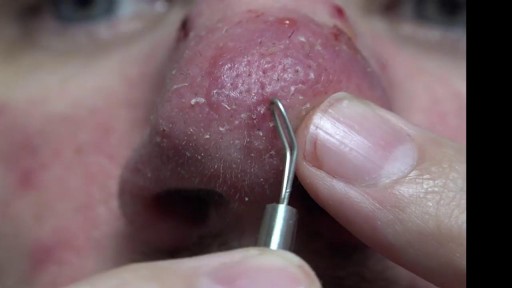
Cystic acne is a severe type of acne in which the pores in the skin become blocked, leading to infection and inflammation. The skin condition mainly affects the face, but also often affects the upper trunk and upper arms. Acne most often affects adolescents and young adults, with an estimated 80 percent of people between 11 and 30 years of age experiencing acne at some point. Cystic acne is the most severe form and affects far fewer people. In 2009, the Centers for Disease Control and Prevention (CDC) found that acne was the top reason people gave for visiting a dermatologist.
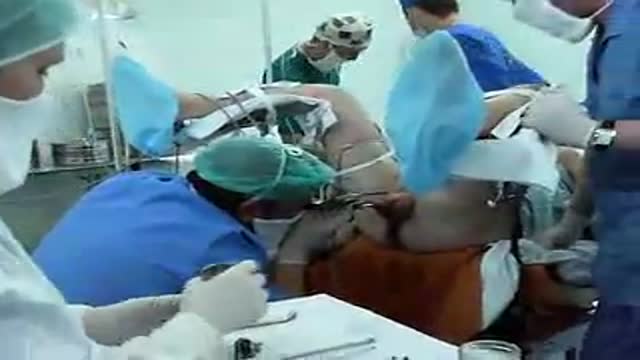
Transurethral resection of the prostate (also known as TURP, plural TURPs and as a transurethral prostatic resection TUPR) is a urological operation. It is used to treat benign prostatic hyperplasia (BPH). As the name indicates, it is performed by visualising the prostate through the urethra and removing tissue by electrocautery or sharp dissection. This is considered the most effective treatment for BPH. This procedure is done with spinal or general anesthetic. A large triple lumen catheter is inserted through the urethra to irrigate and drain the bladder after the surgical procedure is complete. Outcome is considered excellent for 80-90% of BPH patients. Because of bleeding risks associated with the surgery, TURP is not considered safe for many patients with cardiac problems. As with all invasive procedures, the patient should first discuss medications they are taking with their doctor, most especially blood thinners or anticoagulants, such as warfarin (Coumadin), or aspirin. These may need to be discontinued prior to surgery. Postop complications include bleeding (most common), clotting and hyponatremia (due to bladder irrigation).
Additionally, transurethral resection of the prostate is associated with low but important morbidity and mortality.
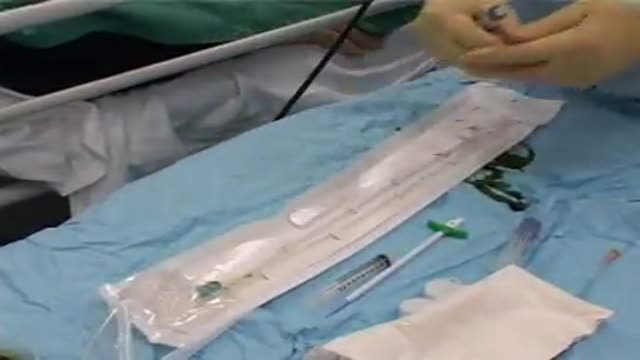
A new and safer method of inserting a Foley catheter suprapubically. The technique allows the insertion to be carried out in an Outpatient setting, thus saving time, cost and effort. By using the Seldinger technique, the product reduces the chances of bowel or bladder perforation and resultant morbidity.
The product has been chosen by The NHS National Technology Adoption Centre to help facilitate adoption of the product.
See www.mediplus.co.uk for more information

Cathy covers hemodialysis, including nursing care before, during, and after the procedure. Peritoneal dialysis, including nursing associated with the procedure. Key complications of hemodialysis, including disequilibrium syndrome and hypotension. Peritonitis, which is a key complication of peritoneal dialysis. Post-op nursing care and patient teaching associated with a kidney transplant.
Our Medical-Surgical video tutorial series is taught by Cathy Parkes BSN, RN, CWCN, PHN and intended to help RN and PN nursing students study for their nursing school exams, including the ATI, HESI and NCLEX.
#NCLEX #KidneyTransplant #HESI #Kaplan #ATI #NursingSchool #NursingStudent #Nurse #RN #PN #Education #LVN #LPN #Renal #Hemodialysis
0:00 What to Expect
0:31 Hemodialysis
2:06 Nursing Care
2:47 Peritoneal Dialysis
3:23 Nursing Care
4:09 Dialysis Complications
4:19 Disequilibrium Syndrome
4:55 Hypotension
5:26 Peritonitis
5:57 Kidney Transplant
6:17 Nursing Care
6:40 Signs and Symptoms
6:51 Patient Teaching
7:17 Quiz Time!
8:27 Bloopers
🚨Head over to our interactive study guide and index ANYTIME and find out exactly which card we’re referencing. https://bit.ly/MedSurgIndex
🚨 Reminder: shipping deadlines are looming 👀
🎁 Regular Shipping: Order by Friday, December 15
🚀 Expedited Shipping: Order by Monday, December 18
🔍 Still searching for last-minute gifts? Consider a Level Up RN Gift Card! 💌 It’s not only a thoughtful present but also the perfect way to share treasures like Pharmacology Flashcards OR digital treasures like Flashables Digital Nursing Flashcards & the Level Up RN membership. Give the gift of knowledge this holiday season! 🧠⚡️💖 bit.ly/LevelUpRNGC
🚪 Access our Cram Courses, Quizzes and Videos all in one ad free space with Level Up RN Membership https://bit.ly/LevelUpRNMembership
Want more ways to MASTER Medical-Surgical Nursing? Check out our flashcards, review games, videos, tips & more!
👇👇👇👇👇👇👇👇👇👇
👉 https://bit.ly/AllMedSurg 👈
☝️👆☝️👆☝️👆☝️👆☝️👆
This is your one-stop-shop for materials to help you LEARN & REVIEW so you can PASS Nursing School.
🤔🤔🤔 DO YOU WANT TO PASS your classes, proctored exams and the NCLEX? 🤔🤔🤔 Our resources are the best you can buy. They are built with a single goal: help you pass with no fluff. Everything you need, and nothing you don’t. Don’t take our word for it, though! Check out our hundreds of ⭐️⭐️⭐️⭐️⭐️ reviews from nurses who passed their exams and the NCLEX with Level Up RN.
🗂️ Our Ultimate Nursing School Survival kit is your number 1 resource to get through nursing school and to pass the NCLEX. Whether you're just starting school or you’re already prepping for the NCLEX, this bundle of flashcards is the best you can buy. It covers all the information you need to know to pass all your exams and it has FREE shipping!
➡️ https://bit.ly/TUNSSK ⬅️
L👀king for EVEN MORE resources to survive Nursing School? Make your Nursing School experience your own! Life’s difficult enough—learning shouldn’t be.
🪅 Games https://nursesquad.com
💻 Digital resources https://bit.ly/NursingStudyCourses
📅 Organizational tools https://bit.ly/OrganizingSchool
✨Want perks? Join our channel!
https://youtube.com/leveluprn/join
🏷 Head to https://leveluprn.com/specials for all our latest deals!🥳️
📧 LOOKING FOR FREE RESOURCES TO HELP WITH YOUR EXAMS? Get exclusive tips, latest video releases and more delivered to your email!
➡️ https://leveluprn.com/signup ⬅️
⚕ 👩 LEVEL UP NURSE SQUAD 👩⚕️
All of the nurses at Level Up RN are here to help! Cathy Parkes started helping her fellow classmates back when she was in nursing school, tutoring so they could pass their exams and graduate. After she got her BSN and started working as an RN at Scripps Encinitas Hospital, she started this YouTube channel to help nursing students around the world. Since then she has built a team of top-notch dedicated nurses and nurse educators who are focused on improving nursing education and supporting career advancement for nurses everywhere. With flashcards, videos, courses, organizational tools and more, we are singularly focused on helping students and nurses Level Up on their exams and nursing careers.

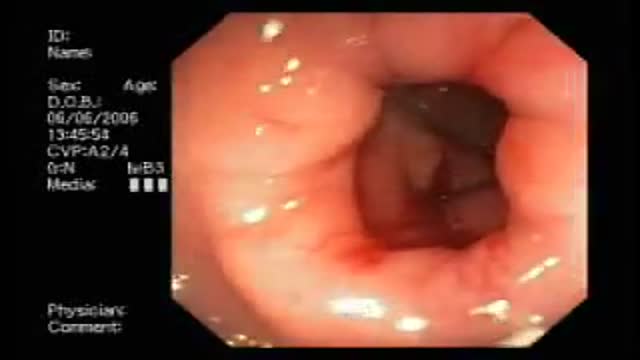
Adenocarcinoma of the Transverse Colon taken by Dr. Julio Murra Saca This is the case of a 42 year-old male, with no significant past medical history presented with abdominal pain and no weight loss was reported. Adenocarcinoma of the colon is a primary cause of mortality and
morbidity in North America and Western Europe. Colonic cancers are the most common GI carcinomas and have the best prognosis. The 5-year survival rate is approximately 50%.
Survival rates may be improved by screening and removal of adenomatous polyps. Almost all colonic cancers are primary adenocarcinomas.

Alimentos Para Controlar La Presion Arterial, Arterial Hypertension, Prevencion De Hipertension
http://bajar-presion-arterial.good-info.co
Para obtener los mismos beneficios que los medicamentos prescritos más comúnmente
sin los efectos secundarios negativos existen alternativas naturales. La dieta es la principal manera de aumentar las reacciones deseables, pero el ejercicio contribuye en gran medida también.
Por ejemplo, la misma reacción causada por los vasodilatadores puede ocurrir cuando usted obtiene suficiente L-Arginina. Este aminoácido permite que las paredes de los vasos sanguíneos se relajen. Usted puede tomar un suplemento o conseguirla a través de proteínas de origen animal, el maní y la soja.
http://bajar-presion-arterial.good-info.co
https://www.youtube.com/watch?v=SFUGz4IqbA0
Alimentos Para Controlar La Presion Arterial, Arterial Hypertension, Prevencion De Hipertension, Arterial Pdf, Hipertension Esencial, Hipertension Pulmonar Tratamiento,Tension Alta Sintomas, Dieta Hipertension, Guia Clinica Hipertension, Sal Marina Hipertension,
Sintomas De Tension Alta, Hipertension Portal Pdf, Hipertension Arterial Clasificacion, Hipertension Intracraneal, Tension Alta En, El Embarazo, Hipertension Primaria
A pneumothorax can be caused by a blunt or penetrating chest injury, certain medical procedures, or damage from underlying lung disease. Or it may occur for no obvious reason. Symptoms usually include sudden chest pain and shortness of breath. On some occasions, a collapsed lung can be a life-threatening event.
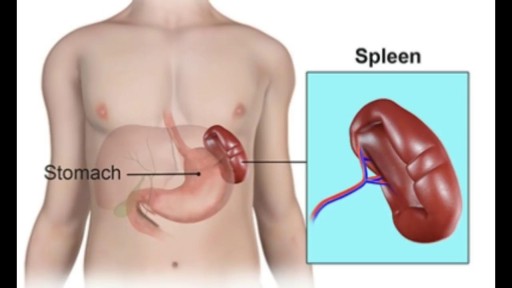
The spleen plays multiple supporting roles in the body. It acts as a filter for blood as part of the immune system. Old red blood cells are recycled in the spleen, and platelets and white blood cells are stored there. The spleen also helps fight certain kinds of bacteria that cause pneumonia and meningitis

houlder examination frequently appears in OSCEs. You’ll be expected to pick up the relevant clinical signs using your examination skills. This shoulder examination OSCE guide provides a clear step by step approach to examining the shoulder, with an included video demonstration.