Top videos

A brain surgery called a craniectomy is performed to remove a part of your skull in order to relieve pressure in an area when your brain swells from a traumatic brain injury. It is also performed to treat medical conditions that cause your brain to swell or bleed that can be caused by an aneurysm, brain tumor or other cancer.
This 3d animation shows how the surgical procedure decreases intracranial pressure (ICP), intracranial hypertension (ICHT), or heavy bleeding (also called hemorrhaging) inside your skull. If left untreated, pressure or bleeding can compress your brain and push it down onto the brain stem. This can be fatal or cause permanent brain damage.
Brain surgery is a very serious procedure under any circumstances, but a craniectomy is done when there is an immediate risk to the brain and neurological function due to severe brain injury or stroke.
For more information about custom 3D animation depicting surgery, please visit https://www.amerra.com/.
Watch additional medical animations:
Accessing an implantable port training - 3D animation: https://youtu.be/xSTpxjyv4O4
Open Suctioning with a Tracheostomy Tube - 3D animation: https://youtu.be/wamB7jpWCiQ
Ventriculostomy Brain Surgery - 3d animation: https://youtu.be/pUy0YDzVNzs
Suctioning the endotracheal tube - medical animation: https://youtu.be/pN6-EYoeh3g
Functional endoscopic sinus surgery (FESS) - 3D animation: https://youtu.be/qKTRyowwaLA
How to insert a nasogastric tube for NG intubation - 3d animation: https://youtu.be/Abf3Gd6AaZQ
Oral airway insertion - oropharyngeal airway technique - 3D animation: https://youtu.be/caxUdNwjt34
Nasotracheal suctioning (NTS) - 3D animation: https://youtu.be/979jWMsF62c
Learn about hemorrhoids with #3d #animation: https://youtu.be/R6NqlMpsiiY
LASIK eye surgery - 3D animation: https://youtu.be/Bb8bnjnEM00
CPR cardiopulmonary resuscitation - 3D animation: https://youtu.be/G87knTZnhks
What are warts (HPV)? - 3D animation: https://youtu.be/guJ1J7rRs1w
How Macular Degeneration Affects Your Vision - 3D animation: https://youtu.be/ozZQIZ_52YY
NeoGraft hair transplant procedure – animation: https://youtu.be/C-eTdH2UPXI
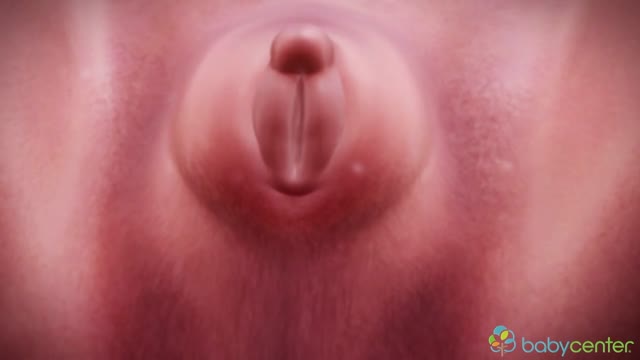
Your baby's sex is set at conception. At around 7 weeks, your baby's internal sex organs – such as ovaries and testes – begin to form in the abdomen. Male and female sex organs and genitalia look the same at this stage because they're derived from the same structures. At around 9 weeks, boys and girls begin to develop differently. In girls, a tiny bud emerges between the tissue of the legs. This bud will become the clitoris. The membrane that forms a groove below the bud separates to become the labia minora and the vaginal opening. By 22 weeks, the ovaries are completely formed and move from the abdomen to the pelvis. They already contain a lifetime supply of 6 million eggs. In boys, the bud develops into the penis and starts to elongate at around 12 weeks. The outer membrane grows into the scrotal sac that will later house the testicles. By 22 weeks, the testes have formed in the abdomen. They already contain immature sperm. Soon they'll begin their descent to the scrotum, but it's a long journey. They'll reach their destination late in pregnancy, or for some boys, after birth. If you're eager to find out whether you're having a girl or a boy, you'll have to wait until you're at least 17 weeks pregnant. That's when the genitals have developed enough to be seen on an ultrasound.

#abdomenliposuction #laserskintightening #drprashantyadav #cosmeticsurgery #plasticsurgery #dezireclinicindia #weightloss #shorts #360degreeabdomenliposuction #lowerbackliposuction
Weight Loss After 360° Abdomen liposuction result, Abdomen Liposuction, lower back liposuction, 360 degree abdomen liposuction
☎️ For more info:
WhatsApp Your Details to know the Cost
Delhi - 8956880644, 9717470550, Pune - 9222122122, Bangalore- 8971224700, Gurugram - 9272007896, Ahmedabad - 9711162746
Why choose Dezire Clinic For Your Cosmetic and plastic surgery treatment ?
Dezire Clinic is a top searched clinic surgical and nonsurgical cosmetic procedure in India when comes to “Cosmetic, Skin ,Laser and Hair transplantation”.
Like and Share the video if you find it useful. Do not forget to Subscribe to our channel to get more updates.
Subscribe on YouTube https://youtube.com/dezireclin....ic?sub_confirmation=
https://youtube.com/dezireplas....ticsurgerycenter?sub
🎦 https://www.youtube.com/dezireclinic
🎦 https://www.youtube.com/DezirePlasticSurgeryCenter
👍🏻 https://www.facebook.com/drprashantmch/
👍🏻 https://www.facebook.com/dezireclinic
📸 https://www.instagram.com/drprashantdezireclinic/
📸 https://www.instagram.com/dezireclinics/
🐥 https://twitter.com/drprashantmch
👍🏻 https://www.linkedin.com/in/drprashantyadav/
🌐 Website: https://www.dezireclinic.in/
📧 dezireclinicindia@gmail.com
📧 info@dezireclinic.in
Dr. Prashant Yadav (M.S., M.Ch. Plastic Surgery ) & Founder of Dezire Clinic
Disclaimer: The content of this channel is for informational and educational purposes only. This content should not be considered a substitute for advice provided by a certified plastic or cosmetic surgeon. Patients must be properly diagnosed by a healthcare professional on an individual basis in order to achieve the desired results. There is no guarantee of getting the results and outcomes shown in videos, as the results can vary at the end. We will not be held liable for any harm caused by someone misusing our name.
#plasticsurgery #cosmeticsurgery #dezireclinic #drprashantyadav
Purpose: To evaluate the results of LASIK and IntraLASIK treatment in myopic patients with nystagmus. Methods: Eight patients with congenital nystagmus (16 eyes), from 23 to 49 years of age, underwent LASIK surgery. Corneal flaps were created using either the Hansatome microkeratome or the Intral...ase femtosecond laser. The ablations were performed with the Bausch & Lomb excimer laser with an active tracking system. In some patients, the eyes were fixated with forceps or a fixation ring during the laser ablation. Results: The refractive errors were corrected in all cases. There was no decentration or loss of best corrected visual acuity greater than 1 line. In 56% of the eyes, the post-operative uncorrected visual acuity was better than the best spectacle corrected-visual acuity (BSCVA). 62.5% of the eyes improved their BSCVA. The overall visual performance was improved in all the patients. One patient that did not not drive before become eligible to get a driver license after the surgery. Conclusions: Selected patients with myopia and congenital nystagmus may benefit from laser refractive surgery. Laser refractive surgery may be safely and accurately performed by using either the Hansatome microkeratome or the Intralase femtosecond laser and an active tracking system with or without mechanical fixation. Certain patients improve their BSCVA post-operatively.
| MBBS मतलब JOHARI MBBS I
Download Johari MBBS APP ( For Online LIVE Classes, Notes, Books PDFs, Test Series )
Johari MBBS ( iPhone IOS Users ) LINK { FOR Online LIVE Classes }
https://apps.apple.com/in/app/....johari-mbbs/id647466
JOHARI MBBS APP ( Android ) LINK { FOR Online LIVE Classes }
https://play.google.com/store/....apps/details?id=co.d
CRASH COURSE LINK ( Anatomy in 30Days with Biochemistry In 7Days Series )
https://zczob.on-app.in/app/oc/389813/zczob
IMPORTANT LINKS :-
1) ORDER Anatomy Next Edition Module , Biochemistry in 7Days & Physiology MODULE
https://joharimbbs.com/
2) Join INSTAGRAM ( For Notes, Revision REELs, Updates )
https://www.instagram.com/johari_mbbs_lectures/
3) INSTA Broadcast Channel ( FOR Daily VLOGS, Life Update )
https://ig.me/j/Abal9xRcXcUyrYpT/
4) Telegram ( For FREE BOOKS PDFs )
https://t.me/joharimbbsofficial
5) Whatsapp Channel ( Daily Update )
https://whatsapp.com/channel/0....029VaEeWKWHAdNb0xOzl
6) Follow On Twitter ( For Latest Updates )
https://twitter.com/JohariMbbs
CRASH COURSE LINK ( Anatomy in 30Days with Biochemistry In 7Days Series )
https://zczob.on-app.in/app/oc/389813/zczob
#mbbs #joharimbbs #anaatomy #biochemistry #physiology #medico #doctors
histology slide identification tricks
histology slides identification tricks
histology slide
histology slides
histology slides identification
histology slide preparation
histology slides identification epithelium
histology slides identification connective tissue
histology slides identification tricks
histology slides of epithelium
histology slide identification
#anatomy#clinicalanatomy #MBBS #neroanatomy #bdc #medsudent #medicalcollege
For notes IG - johari_mbbs_lectures
link- https://www.instagram.com/p/CNOwFgEJmJL/
Join Telegram Channel ( JOhari MBBS Public 20x )
https://t.me/JohariMBBS
For Tag :-
histology , histology slides , histology slide identification , histology slides identification , histology slides preparation , tongue histology slide , histology slides asked in exam , histology slide identification trick , histology slides of connective tissue , mbbs histology , histology slides identification epithelium , trachea histology slide , slides , duodenum histology slide , histology slides tricks , histology slides review , examine histology slides

Dr. Alex Campbell and Dr. Carolina Restrepo of Premium Care Plastic Surgery in Cartagena, Colombia perform a Mommy Makeover on an international patient. Watch the procedure as Dr. Campbell and Dr. Restrepo work together to offer this patient more surgery in less time, which leads to a quicker recovery and better results.
We will show you what a sports hernia examination (aka athletic pubalgia, gilmore's groin, lower abdominal pain) and rule out a diagnosis of hip impingement. Rehab exercises are suggested based on the results.
If you're experiencing any of these symptoms, don't hesitate to schedule a sports hernia examination. I can help you determine the best treatment plan to promote your recovery and avoid future injury. Subscribe to my channel to stay updated on the latest medical news and tips!
If you would like to know more about sports hernias and other diagnoses for front of hip, groin, adductor and lower abdominal strain, watch our detailed webinar here: https://bit.ly/37thtNF
For treatment, come visit us or schedule a virtual session. www.p2sportscare.com
Costa Mesa CA 715-502-4243
#sportshernia #abdominal #hippain
Sports Hernia Diagnosis
What Is A Sports Hernia?
A sports hernia is tearing of the transversalis fascia of the lower abdominal or groin region. A common misconception is that a sports hernia is the same as a traditional hernia. The mechanism of injury is rapid twisting and change of direction within sports, such as football, basketball, soccer and hockey.
The term “sports hernia” is becoming mainstream with more professional athletes being diagnosed. The following are just to name a few:
Torii Hunter
Tom Brady
Ryan Getzlaf
Julio Jones
Jeremy Shockey
If you follow any of these professional athletes, they all seem to have the same thing in common: Lingering groin pain. If you play fantasy sports, this is a major headache since it seems so minor, but it can land a player on Injury Reserve on a moments notice. In real life, it is a very frustrating condition to say the least. It is hard to pin point, goes away with rest and comes back after activity, but is hardly painful enough to make you want to stop. It lingers and is always on your mind. And if you’re looking for my step-by-step sports hernia rehab video course here it is.
One the best definitions of Sport hernias is the following by Harmon:
The phenomena of chronic activity–related groin pain that it is unresponsive to conservative therapy and significantly improves with surgical repair.”
This is truly how sports hernias behave in a clinical setting. It is not uncommon for a sports hernia to be unrecognized for months and even years. Unlike your typical sports injury, most sports medicine offices have only seen a handful of cases. It’s just not on most doctors’ radar. The purpose of this article is not only to bring awareness about sports hernias, but also to educate.
Will you find quick fixes in this article for sports hernia rehab?
Nope. There is no quick fix for this condition, and if someone is trying to sell you one, they are blowing smoke up your you-know-what.
Is there a way to decrease the pain related to sports hernias?
Yes. Proper rehab and avoidance of activity for a certain period of time will assist greatly, but this will not always stop it from coming back. Pain is the first thing to go and last thing to come. Do not be fooled when you become pain-free by resting it. Pain is only one measure of improvement in your rehab. Strength, change of direction, balance and power (just to name a few) are important, since you obviously desire to play your sport again. If you wanted to be a couch potato, you would be feeling better in no time. Watching Sports Center doesn’t require any movement.
Why is this article so long?
There is a lot of information on sports hernias available to you on the web. However, much of the information is spread out all over the internet and hard for athletes to digest due to complicated terminology. This article lays out the foundational terminology you will need to understand what options you have with your injury. We will go over anatomy, biomechanics, rehab, surgery, and even the fun facts. The information I am using is from the last ten years of medical research, up until 2016. We will be making updates overtime when something new is found as well. So link to this page and share with friends. This is the best source for information on sports hernias you will find.
Common Names (or Aliases?) for Sports Hernias
Sportsman’s Hernia
Athletic Pubalgia
Gilmore’s Groin
How Do You Know If You Have A Sports Hernia?
Typical athlete characteristics:
Male, age mid-20s
Common sports: soccer, hockey, tennis, football, field hockey
Motions involved: cutting, pivoting, kicking and sharp turns
Gradual onset
How A Sports Hernia Develops
Chronic groin pain typically happens over time, which is why with sports hernias, we do not hear many stories of feeling a “pop” or a specific moment of injury. It is the result of “overuse” mechanics stemming from a combination of inadequate strength and endurance, lack of dynamic control, movement pattern abnormalities, and discoordination of motion in the groin area.
#SPORTSHERNIAEXAM #california

This 3D animation of brain surgery, shows how a ventriculostomy is performed, which is a neurosurgical procedure of creating a hole within a cerebral ventricle for drainage. It is most commonly performed on those with hydrocephalus, an abnormal buildup of fluid in the ventricles (cavities) deep within the brain. It's done by surgically penetrating the skull, dura mater, and brain such that the ventricular system ventricle of the brain is accessed.
When catheter drainage is temporary, it is commonly referred to as an external ventricular drain (EVD). When catheter drainage is permanent, it is usually referred to as a shunt.
There are many catheter-based ventricular shunts that are named for where they terminate, for example, a ventriculi-peritoneal shunt terminates in the peritoneal cavity, a ventriculoarterial shunt terminates within the atrium of the heart, etc. The most common entry point on the skull is called Kocher's point. An EVD ventriculostomy is done primarily to monitor the intracranial pressure as well as to drain cerebrospinal fluid (CSF), primarily, or blood to relieve pressure from the central nervous system (CNS).
For more information about custom medical animation, please visit https://www.amerra.com/.
Watch additional medical animations:
Craniectomy brain surgery - 3D animation: https://youtu.be/1RkseDeYS9g
Accessing an implantable port training - 3D animation: https://youtu.be/xSTpxjyv4O4
Open Suctioning with a Tracheostomy Tube - 3D animation: https://youtu.be/wamB7jpWCiQ
Suctioning the endotracheal tube - medical animation: https://youtu.be/pN6-EYoeh3g
Functional endoscopic sinus surgery (FESS) - 3D animation: https://youtu.be/qKTRyowwaLA
How to insert a nasogastric tube for NG intubation - 3d animation: https://youtu.be/Abf3Gd6AaZQ
Oral airway insertion - oropharyngeal airway technique - 3D animation: https://youtu.be/caxUdNwjt34
Nasotracheal suctioning (NTS) - 3D animation: https://youtu.be/979jWMsF62c
Learn about hemorrhoids with #3d #animation: https://youtu.be/R6NqlMpsiiY
LASIK eye surgery - 3D animation: https://youtu.be/Bb8bnjnEM00
CPR cardiopulmonary resuscitation - 3D animation: https://youtu.be/G87knTZnhks
What are warts (HPV)? - 3D animation: https://youtu.be/guJ1J7rRs1w
How Macular Degeneration Affects Your Vision - 3D animation: https://youtu.be/ozZQIZ_52YY
NeoGraft hair transplant procedure – animation: https://youtu.be/C-eTdH2UPXI