Top videos
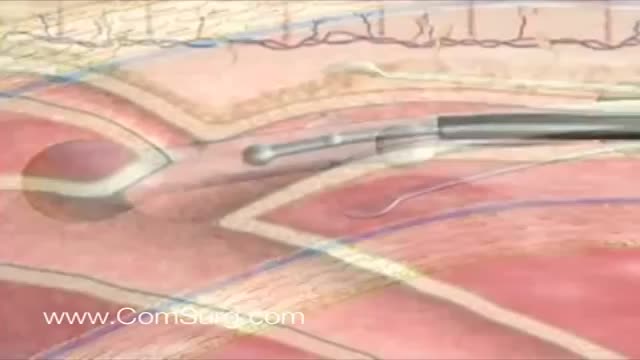
Like the VenaCure EVLT® procedure, which uses a laser to ablate the varicose vein, VNUS RF treatment is an alternative to more invasive leg stripping surgery. It is used primarily to treat the great saphenous veins (GSV), small saphenous vein (SSV), and other superficial veins in the legs.

Dr. Shaun Kunisaki is an Associate Professor of Surgery at The Johns Hopkins University and Associate Chief of Strategy and Integration in the Division of General Pediatric Surgery at the Johns Hopkins Children's Center. His clinical practice spans the full breadth of pediatric general surgery, but he is recognized both regionally and nationally for this expertise in complex thoracic surgical problems in the fetus and young child. As Director of Pediatric Esophageal Surgery, he specializes in the management of long-gap esophageal atresia. In this role within the Johns Hopkins Children Center Fetal Program, he helps counsel parents with pregnancies complicated by fetal anomalies.
Learn more about Dr. Kunisaki at https://www.hopkinsmedicine.or....g/profiles/results/d

► Sign up here and try our FREE content: http://lectur.io/freecontentyt
► If you’re an medical educator or faculty member, visit: http://lectur.io/medytb2u
This video “Connective Tissue” is part of the Lecturio course “Histology” ► WATCH the complete course on http://lectur.io/connectivetissue
► LEARN ABOUT:
- Cells and Basic Tissue
- Nerve Tissues
- Muscle Tissues
- Epithelial Tissues
- Connective Tissues
► THE PROF: Your lecturer is Professor Geoff Meyer. He is currently teaching at the School of Anatomy, Physiology and Human Biology at the University of Western Australia (UWA). As a leading anatomy and histology expert he is also coordinating the Federative International Program for Anatomical Terminologies (FIPAT) of the International Federation of Associations of Anatomists (IFAA). Besides medical research on the ovarian function, steroidogenesis, corpus luteum, angiogenesis, and microcirculation, Geoff Meyer’s research activities also focus on developing innovative, computer-aided learning and teaching tools. For his inventiveness, Geoff Meyer has received a number of awards, including the Australian University Teaching Award.
► LECTURIO is your single-point resource for medical school:
Study for your classes, USMLE Step 1, USMLE Step 2, MCAT or MBBS with video lectures by world-class professors, recall & USMLE-style questions and textbook articles. Create your free account now: http://lectur.io/connectivetissue
► INSTALL our free Lecturio app
iTunes Store: https://app.adjust.com/z21zrf
Play Store: https://app.adjust.com/b01fak
► READ TEXTBOOK ARTICLES related to this video:
Types of Tissue: Connective Tissue, Muscle Tissue, Epithelial Tissue, and Nervous Tissue
http://lectur.io/connectivetissuearticle
► SUBSCRIBE to our YouTube channel: http://lectur.io/subscribe
► WATCH MORE ON YOUTUBE: http://lectur.io/playlists
► LET’S CONNECT:
• Facebook: https://www.facebook.com/lectu....rio.medical.educatio
• Instagram: https://www.instagram.com/lecturio_medical_videos
• Pinterest: https://www.pinterest.de/lecturiomedical
• LinkedIn: https://www.linkedin.com/company/lecturio-medical/
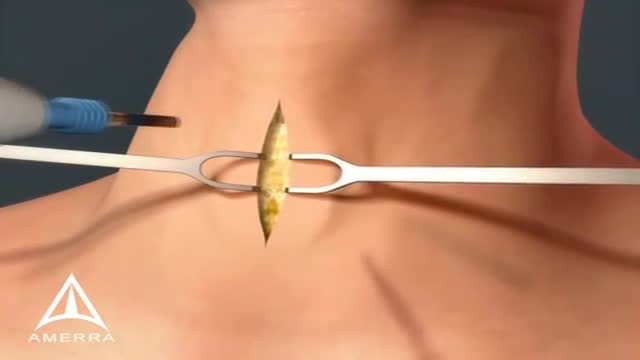
A tracheotomy or a tracheostomy: is simply an opening surgically created through the neck into the trachea (windpipe) to allow direct access to the breathing tube and is commonly done in an operating room under general anesthesia. A tube is usually placed through this opening to provide an airway and to remove secretions from the lungs. Breathing is done through the tracheostomy tube rather than through the nose and mouth. The term “tracheotomy” refers to the incision into the trachea (windpipe) that forms a temporary or permanent opening, which is called a “tracheostomy,” however; the terms are sometimes used interchangeably.
As the liver becomes more severely damaged, more obvious and serious symptoms can develop, such as: yellowing of the skin and whites of the eyes (jaundice) swelling in the legs, ankles and feet, due to a build-up of fluid (oedema) swelling in your abdomen, due to a build-up of fluid known as ascites.

Atrial flutter is a type of abnormal heart rate, or arrhythmia. It occurs when the upper chambers of your heart beat too fast. When the chambers in the top of your heart (atria) beat faster than the bottom ones (ventricles), it complicates your heart rhythm

Red eyes usually are caused by allergy, eye fatigue, over-wearing contact lenses or common eye infections such as pink eye (conjunctivitis). However, redness of the eye sometimes can signal a more serious eye condition or disease, such as uveitis or glaucoma.

The discussion begins with a basic explanation of Bone biology taking into consideration the osteoblast and osteoclast balance. Concepts of RANK, RANK ligand and Osteoprotegerin are included. Risk factors for Osteoporosis such as Age, alcohol, smoking, sedentary lifestyle are also discussed.
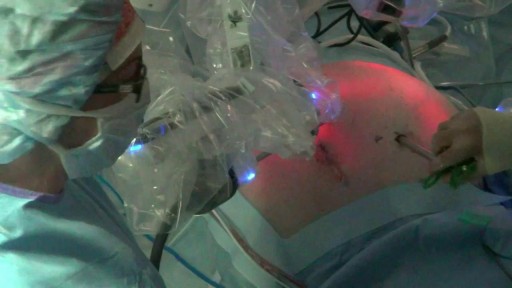
Splenectomy is a surgical procedure to remove your spleen. The spleen is an organ that sits under your rib cage on the upper left side of your abdomen. It helps fight infection and filters unneeded material, such as old or damaged blood cells. With the da Vinci Surgical System, Dr. Olson operates through just a few small incisions. The da Vinci System features a magnified 3D high-definition vision system and tiny wristed instruments that bend and rotate far greater than the human hand. As a result, da Vinci enables surgeons to operate with enhanced vision, precision and control.