Top videos

Find our full video library only on Osmosis Prime: http://osms.it/more.
Join over 3 million current & future clinicians who learn by Osmosis, and over 130 universities around the world who partner with us to make medical and health education more engaging and efficient. We have unparalleled tools and materials to prepare you to succeed in school, on board exams, and as a future clinician. Sign up for a free trial at http://osms.it/more. If you're interested in exploring an institutional partnership, visit osmosis.org/educators to request a personalized demo.
Follow us on social:
Facebook: http://osms.it/facebook
Twitter: http://osms.it/twitter
Instagram for med: http://osms.it/instagram
Instagram for nursing: https://osms.it/ignursing
Linkedin: https://osms.it/linkedin
Our Vision: Everyone who cares for someone will learn by Osmosis.
Our Mission: To empower the world’s clinicians and caregivers with the best learning experience possible. Learn more here: http://osms.it/mission
Medical disclaimer: Knowledge Diffusion Inc (DBA Osmosis) does not provide medical advice. Osmosis and the content available on Osmosis's properties (Osmosis.org, YouTube, and other channels) do not provide a diagnosis or other recommendation for treatment and are not a substitute for the professional judgment of a healthcare professional in diagnosis and treatment of any person or animal. The determination of the need for medical services and the types of healthcare to be provided to a patient are decisions that should be made only by a physician or other licensed health care provider. Always seek the advice of a physician or other qualified healthcare provider with any questions you have regarding a medical condition. © 2023 Elsevier. All rights reserved.

1. What is hemodialysis?
2. Why do you do hemodialysis?
3. How does hemodialysis remove body waste?
4. What are the symptoms and side effects of hemodialysis?
5. How should I eat food when I do hemodialysis?
6. What are some precautions for patients during hemodialysis?
► If you have any health issues contact us anytime, we here to help at CloudHospital – https://icloudhospital.com/
► Subscribe: https://www.youtube.com/channel/UCmk5... to learn more about various health and beauty topics.
► Find us on Facebook: https://www.facebook.com/icloudhospital/
► On Instagram: https://www.instagram.com/cloudhospit...
► On LinkedIn: https://www.linkedin.com/company/clou...
► On Twitter: https://twitter.com/CloudhospitalI
#hemodialysis #cloudhospital #koreahospital
Most women are put on a 3 to 5 day antibiotic. Men might be put on an antibiotic for 7 to 14 days. While symptoms usually clear up around three days after antibiotic treatment, it can take up to five days for all the bacteria in your urinary tract to die off. It may take even longer for men.

While the incidence of most sports-related injuries has been holding steady for the past two decades, injuries to the anterior cruciate ligament (ACL) continue to increase significantly, particularly in female athletes. In fact, on many college teams, as many as 30 to 50 percent of young women have had an ACL injury during their high school careers in certain sports, such as basketball, soccer and gymnastics.
Watch pediatric orthopedic surgeons at Akron Children's Hospital perform arthroscopic surgery to replace a young athlete's ACL

Hemodialysis is the process of cleaning the patient’s blood outside the body. Learn more about this renal replacement therapy option.
Read more: http://www.freseniusmedicalcar....e.com/en/patients-fa
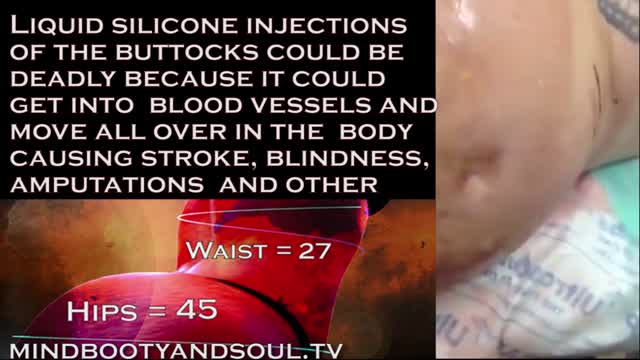
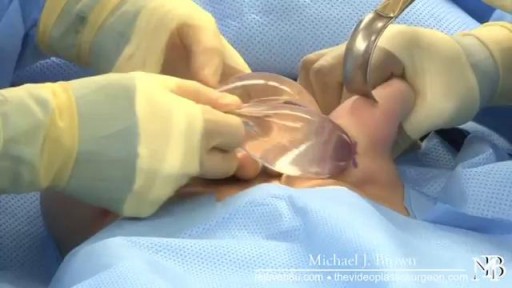
2016 marks 10 years when illegal injections started to gain momentum and become a popular alternative to butt implants. The Brazilian butt lift wasn't well know at the time but the goal of finding an unlicensed person to inject a foreign substance into the body was in high demand.
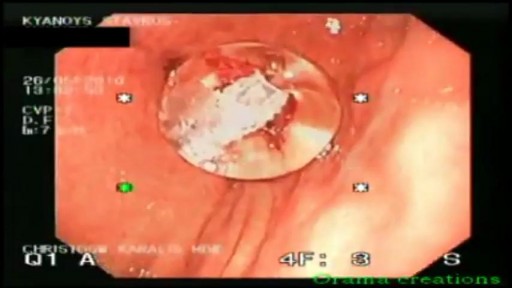
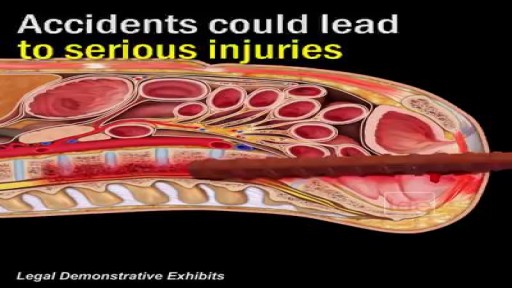
Gastrostomy tube is placed when a patient is not able to eat on his/her own as a result of neurological or other dysfunction. There are many different types of gastrostomy tubes but in general there are two bigger categories. The classic one and the low profile one. The gastroplexy technique is used preferably to avoid accidental pulling of the gastrostomy tube from an agitated or confused patient.