Top videos

Hearing loss can affect anyone at any age, due to heredity, medical conditions or loud noise exposure. However, as we get older, we naturally become more susceptible to hearing loss because of changes to the delicate mechanics of our ears.

Obesity is the abnormal condition that causes a person to put on excessive amounts of weight due to accumulation of fat in their body. This extreme weight causes a variety of other disorders and diseases as complications associated with it. https://goo.gl/GgSAoY

A brief screening examination should be conducted checking the face, eyes, mouth, chest, abdomen, spine and limbs to exclude major abnormalities. A strong cry and a widespread pink blush over the face and body are good signs that all is well. Some children may be born with ambiguous genitalia. Ambiguous genitalia is a medical emergency and requires urgent assessment by a paediatrician. If you have sufficient clinical experience, an orogastric tube should be passed when the neonate's mother has suffered polyhydramnios. This excludes oesophageal atresia.

It sounds like you're questioning whether or not your water may have broken, and this can actually be a hard thing for a lot of women to tell. Usually if your water breaks, it's just a trickle of fluid, and you're afraid to admit it to anyone because you think you peed your pants. And it is normal to pee your pants when you're pregnant because the bladder is right below the uterus, and if the baby moves just right, it might kick out a little bit of urine. So if you feel a trickle or a little tiny gush of fluid, what you want to do is put a pad or a pantie-liner on after going to the bathroom and emptying your bladder, and wait an hour and see if fluid continues to come out. And if it does, then you're not having bladder leakage issues - your water is probably broken.

Sexually Transmitted Diseases (STDs) affect millions of people each year. The most common STDs are gonorrhea, chlamydia and trichomoniasis. While even thinking about STDs and whether you may have one is scary, knowing the facts can make a big difference in your long-term health. Here is what you need to know:
People who are sexually active with multiple partners and are not using barrier protection are at most risk. Teenagers are a large part of this group, because they dont always practice safe sex and they are more likely to have multiple partners. It is recommended that women who are sexually active with multiple partners get screened yearly or immediately after they have engaged in unprotected sex. If you discover that you have an STD, both you and your partner would most likely be treated with antibiotics.
Gonorrhea
Approximately 350,000 cases of gonorrhea were reported to the CDC in 2006, but because not everyone is getting tested for STDs, experts believe the actual numbers are twice that.
The symptoms for gonorrhea are burning with urination, abnormal discharge or pelvic pain. Pelvic pain indicates a very severe infection. Untreated gonorrhea can lead to a serious infection as the disease may spread to a womans fallopian tubes and cause infertility.
Chlamydia
There were 1,000,000 cases of chlamydia reported to the CDC in 2006; experts think the actual rate of infection is as high as 2,000,000 cases.
Chlamydia is often called the silent disease because many people with chlamydia have no symptoms. Chlamydia can affect the urethra, the vagina, the cervix and the fallopian tubes. Symptoms include burring with urination, abnormal discharge and pelvic pain. If you are experiencing any of these systems you should see your doctor to determine if you have chlamydia. Women with chlamydia who arent treated are likely to develop pelvic inflammatory disease. Pelvic inflammatory disease occurs when the infection spreads and causes scarring to the uterus and fallopian tubes. Untreated chlamydia can result in infertility.
Trichomoniasis
Trichomoniasis is the most common STD. About 7 million women and men have trichomoniasis. Women who have trichomoniasis will often experience a frothy yellow or green discharge coming from their vagina. But some people wont have any symptoms.
Understanding STDs, what causes them, and how to treat them will help you stay in control of your health.

Current treatment is a combination of pegylated interferon-alpha-2a or pegylated interferon-alpha-2b (brand names Pegasys or PEG-Intron) and the antiviral drug ribavirin for a period of 24 or 48 weeks, depending on hepatitis C virus genotype. In a large multicenter randomized control study among genotype 2 or 3 infected patients (NORDymanIC),[35] patients achieving HCV RNA below 1000 IU/mL by day 7 who were treated for 12 weeks demonstrated similar cure rates as those treated for 24 weeks.[36][37]
Pegylated interferon-alpha-2a plus ribavirin may increase sustained virological response among patients with chronic hepatitis C as compared to pegylated interferon-alpha-2b plus ribavirin according to a systematic review of randomized controlled trials .[38] The relative benefit increase was 14.6%. For patients at similar risk to those in this study (41.0% had sustained virological response when not treated with pegylated interferon alpha 2a plus ribavirin), this leads to an absolute benefit increase of 6%. About 16.7 patients must be treated for one to benefit (number needed to treat = 16.7; click here [39] to adjust these results for patients at higher or lower risk of sustained virological response). However, this study's results may be biased due to uncertain temporality of association, selective dose response.
Treatment is generally recommended for patients with proven hepatitis C virus infection and persistently abnormal liver function tests.
Treatment during the acute infection phase has much higher success rates (greater than 90%) with a shorter duration of treatment; however, this must be balanced against the 15-40% chance of spontaneous clearance without treatment (see Acute Hepatitis C section above).
Those with low initial viral loads respond much better to treatment than those with higher viral loads (greater than 400,000 IU/mL). Current combination therapy is usually supervised by physicians in the fields of gastroenterology, hepatology or infectious disease.
The treatment may be physically demanding, particularly for those with a prior history of drug or alcohol abuse. It can qualify for temporary disability in some cases. A substantial proportion of patients will experience a panoply of side effects ranging from a 'flu-like' syndrome (the most common, experienced for a few days after the weekly injection of interferon) to severe adverse events including anemia, cardiovascular events and psychiatric problems such as suicide or suicidal ideation. The latter are exacerbated by the general physiological stress experienced by the patient.
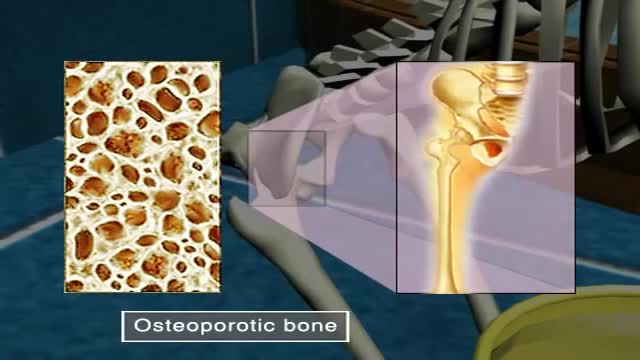
Osteoporosis, which literally means porous bone, is a disease in which the density and quality of bone are reduced. As bones become more porous and fragile, the risk of fracture is greatly increased. The loss of bone occurs silently and progressively. Often there are no symptoms until the first fracture occurs.
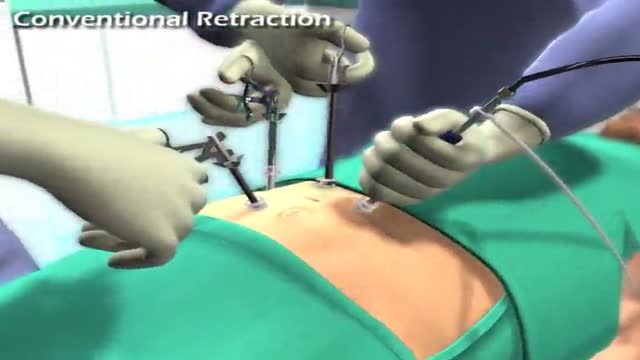
Virtual Ports, Ltd. (http://www.virtual-ports.com) is a medical device company developing and marketing instruments to improve minimally invasive laparoscopic procedures.
The EndoGrab retraction system reduces the number of ports needed for surgery by eliminating the need for traditional hand held retraction. For the surgeon, this simple solution results in the need for less auxiliary personnel, a decreased overall surgery cost, and more control over the surgery. The EndoGrab also offers added benefit to the patient who will experience less post-operative discomfort and scarring.
The EndoGrab is an internally anchored, hands-free retracting device that is introduced at the start of surgery through a 5mm trocar by means of a proprietary Applier tool. The Surgeon uses the Applier to attach the EndoGrab to both the organ requiring retraction and to the internal abdominal wall, thereby removing the organ from the operative field. The Applier is then removed and the port is free for use by other instruments.
3D video animation produced by Virtual Point Multimedia (http://virtual-point.com)
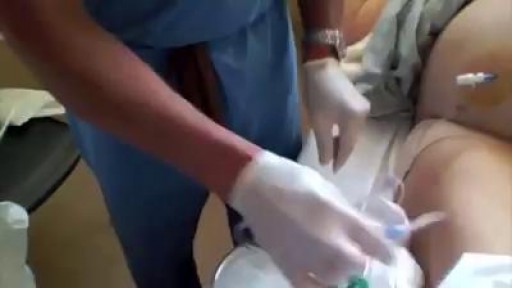
Paracentesis is a procedure to take out fluid that has collected in the belly (peritoneal fluid). This fluid buildup is called ascites camera.gif. Ascites may be caused by infection, inflammation, an injury, or other conditions, such as cirrhosis or cancer. The fluid is taken out using a long, thin needle put through the belly. The fluid is sent to a lab and studied to find the cause of the fluid buildup. Paracentesis also may be done to take the fluid out to relieve belly pressure or pain in people with cancer or cirrhosis.

James Slover, MD, and Ivan Madrid, MD, describe the benefits of knee replacement surgery, the differences in partial and total knee replacement, and how the procedures are performed at NYU Langone.
Learn more about Dr. Slover: http://nyulangone.org/doctors/....1851355564/james-d-s
Learn more about Dr. Madrid: http://nyulangone.org/doctors/....1912940107/ivan-madr
To learn more about joint replacement surgery at NYU Langone, visit: http://nyulangone.org/location....s/center-for-musculo

New York Plastic Surgeon, Carlin Vickery, MD (http://www.5thavesurgery.com) performs a CoolSculpting by Zeltiq procedure.
A NYC patient in this video explains her interest in the CoolSculpting procedure and discusses her experience on camera while receiving this Zeltiq treatment.
"How to Perform a Transthoracic Echocardiographic Study Volume 1: Transducer Position and Anatomy" is an instructional video, offered by ASE, and can be used for professional lectures and offers an interactive section for flexible presentations. The video includes an overview of relevant cardiac anatomy, a step by step presentation of all Transducer Positions, and the sequential transducer movements to acquire standard echo images needed to complete a Transthoracic Echocardiographic Study.
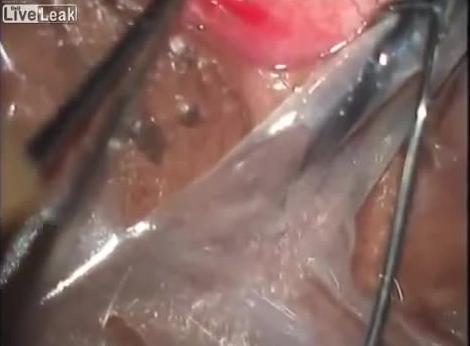
Loa loa filariasis (also known as loiasis, loaiasis, Calabar swellings, Fugitive swelling, Tropical swelling and African eyeworm) is a skin and eye disease caused by the nematode worm, loa loa. Humans contract this disease through the bite of a Deer fly or Mango fly (Chrysops spp), the vectors for Loa loa. The adult Loa loa filarial worm migrates throughout the subcutaneous tissues of humans, occasionally crossing into subconjunctival tissues of the eye where it can be easily observed. Loa loa does not normally affect one's vision but can be painful when moving about the eyeball or across the bridge of the nose.The disease can cause red itchy swellings below the skin called "Calabar swellings". The disease is treated with the drug diethylcarbamazine (DEC), and when appropriate, surgical methods may be employed to remove adult worms from the conjunctiva.