Top videos
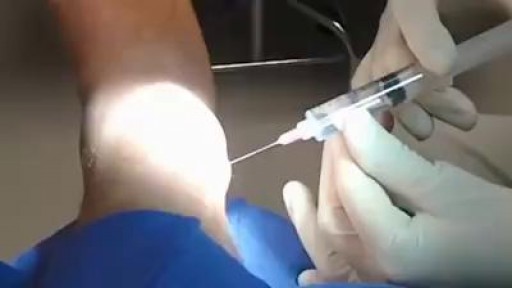
Hardware removals are among the most commonly performed surgical procedures worldwide. Current literature offers little data concerning postoperative patient satisfaction. The purpose of our study was to evaluate the patients’ point of view on implant removal. watch to learn more.
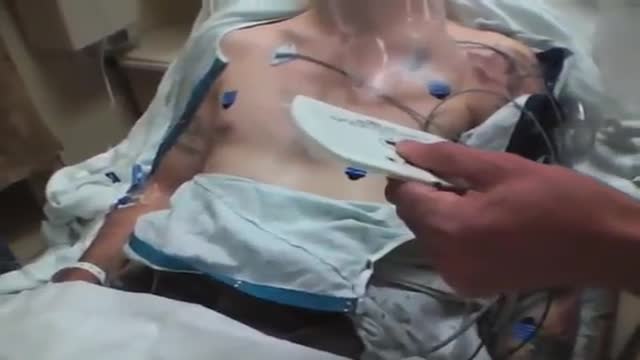
Electrical cardioversion is a procedure in which an electric current is used to reset the heart's rhythm back to its regular pattern (normal sinus rhythm). The low-voltage electric current enters the body through metal paddles or patches applied to the chest wall.

This video: Pancreatic cancer begins in the tissues of your pancreas — an organ in your abdomen that lies horizontally behind the lower part of your stomach. Your pancreas secretes enzymes that aid digestion and hormones that help regulate the metabolism of sugars. Pancreatic cancer often has a poor prognosis, even when diagnosed early. Pancreatic cancer typically spreads rapidly and is seldom detected in its early stages, which is a major reason why it's a leading cause of cancer death. Signs and symptoms may not appear until pancreatic cancer is quite advanced and complete surgical removal isn't possible.

This video depicts how a stent is placed in the coronary artieries. We first place a guiding wire in the heart artery through a catheter, usually from the groin. Then the stent is inflated by a balloon in the artery, which is then removed. The stent remains permanently. Blood thinners, aspirin and plavix, are both required after a stent is placed in your heart artery.
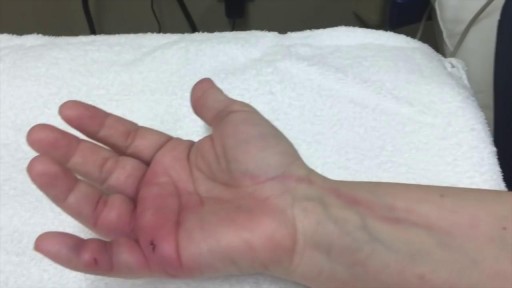
The most common symptoms of infection from animal bites are redness, pain, swelling, and inflammation at the site of the bite. You should seek immediate medical treatment if any of these symptoms continue for more than 24 hours. Other symptoms of infection include: pus or fluid oozing from the wound
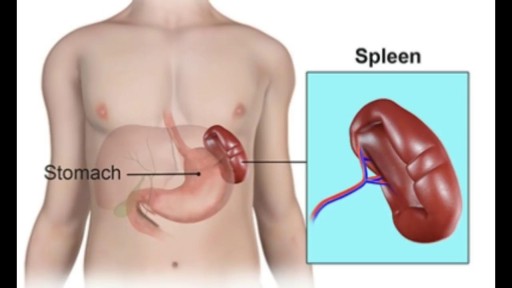
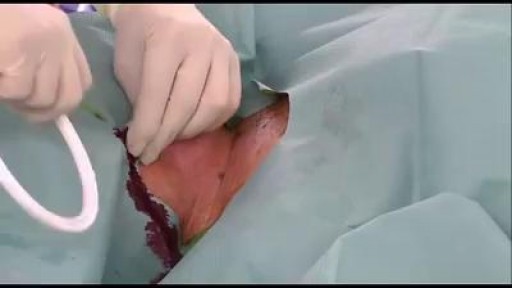
The spleen plays multiple supporting roles in the body. It acts as a filter for blood as part of the immune system. Old red blood cells are recycled in the spleen, and platelets and white blood cells are stored there. The spleen also helps fight certain kinds of bacteria that cause pneumonia and meningitis

houlder examination frequently appears in OSCEs. You’ll be expected to pick up the relevant clinical signs using your examination skills. This shoulder examination OSCE guide provides a clear step by step approach to examining the shoulder, with an included video demonstration.

For benign colorectal diseases, totally laparoscopic left-sided colectomy was already reported on some papers. Nowadays, there is increasingly demanded minimally invasive surgerys on malignant bowel diseases including colorectal cancers and so we developed the new techniques in that specimen is del...ivered through the open rectal stump, especially, using Sani Sleeve(TM). In this operation video, you can see that an anvil was fixed to proximal colonic stump with intracorporeal purse-string suture using Endo-stitch(TM). (SETA : Specimen Extraction Through Anus)

Aortoiliac occlusive disease (AIOD) occurs commonly in patients with PAD. Significant lesions in the aortoiliac arterial segment are exposed easily by palpation of the femoral pulses. Any diminution of the palpable femoral pulse indicates that a more proximal obstruction exists. Obstructive lesions may be present in the infrarenal aorta, common iliac, internal iliac (hypogastric), external iliac, or combinations of any or all of these vessels. Occasionally, degenerated nonstenotic atheromatous disease exists in these vessels and may manifest by atheroembolism to the foot, the "blue toe" or "trash foot" syndrome. Generally, patients with aortoiliac PAD have a poorer general prognosis than those with more distal PAD.

Adenocarcinoma of the Transverse Colon taken by Dr. Julio Murra Saca This is the case of a 42 year-old male, with no significant past medical history presented with abdominal pain and no weight loss was reported. Adenocarcinoma of the colon is a primary cause of mortality and
morbidity in North America and Western Europe. Colonic cancers are the most common GI carcinomas and have the best prognosis. The 5-year survival rate is approximately 50%.
Survival rates may be improved by screening and removal of adenomatous polyps. Almost all colonic cancers are primary adenocarcinomas.
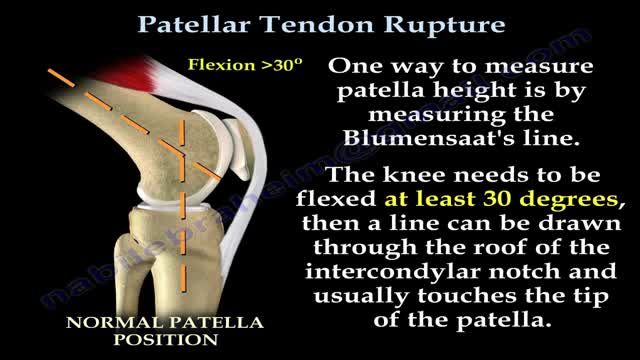
Patellar tendon rupture is a rupture of the tendon that connects the patella to the tibia. The superior portion of the patellar tendon attaches on the posterior portion of the patella, and the posterior portion of the patella tendon attaches to the tibial tubercle on the front of the tibia.

This video provides a demonstration of how to assess for transillumination when assessing scrotal swelling.
Read our step-by-step guide here: https://geekymedics.com/testic....ular-examination-osc
Check out our other awesome clinical skills resources, including:
• 🔥 Geeky Medics Bundles (discounted products): https://app.geekymedics.com/purchase/bundles/
• ✨ 1000+ OSCE Stations: https://app.geekymedics.com/pu....rchase/osce-stations
• 🏥 Geeky Medics OSCE Revision Book: https://app.geekymedics.com/purchase/book/
• 📝 150+ PDF OSCE Checklists: https://geekymedics.com/pdf-osce-checklists/
• 🗂️ 3000+ OSCE Flashcards: https://app.geekymedics.com/pu....rchase/flashcard-col
• 📱 Geeky Medics OSCE App: https://geekymedics.com/geeky-medics-app/
• 🩺 Medical Finals SBA Question Pack: https://app.geekymedics.com/pu....rchase/medical-stude
• 💊 PSA Question Pack: https://app.geekymedics.com/pu....rchase/prescribing-s
Subscribe to our newsletter to be the first to know about our latest content: https://geekymedics.com/newsletter/ ✉️
Join the Geeky Medics community: 👩👩👧👧
Twitter: http://www.twitter.com/geekymedics
Instagram: https://instagram.com/geekymedics
Facebook: http://www.facebook.com/geekymedics
Always adhere to your medical school/local hospital guidelines when performing examinations or clinical procedures. DO NOT perform any examination or procedure on patients based purely on the content of these videos. Geeky Medics accepts no liability for loss of any kind incurred as a result of reliance upon the information provided in this video.
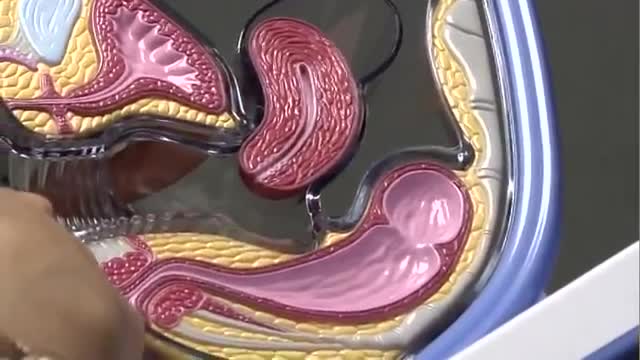
Postmenopausal bleeding (PMB) is defined for practical purposes as vaginal bleeding occurring after twelve months of amenorrhoea, in a woman of the age where the menopause can be expected.[1] Hence it does not apply to a young woman, who has had amenorrhoea from anorexia nervosa, or a pregnancy followed by lactation. However, it can apply to younger women following premature ovarian failure or premature menopause. Unscheduled bleeding in women of menopausal age taking hormone replacement therapy (HRT) should be managed in the same way from a practical perspective.[2] 'Unscheduled bleeding' is defined as non-cyclical bleeding still continuing six months after commencing HRT or after six months of amenorrhoea.
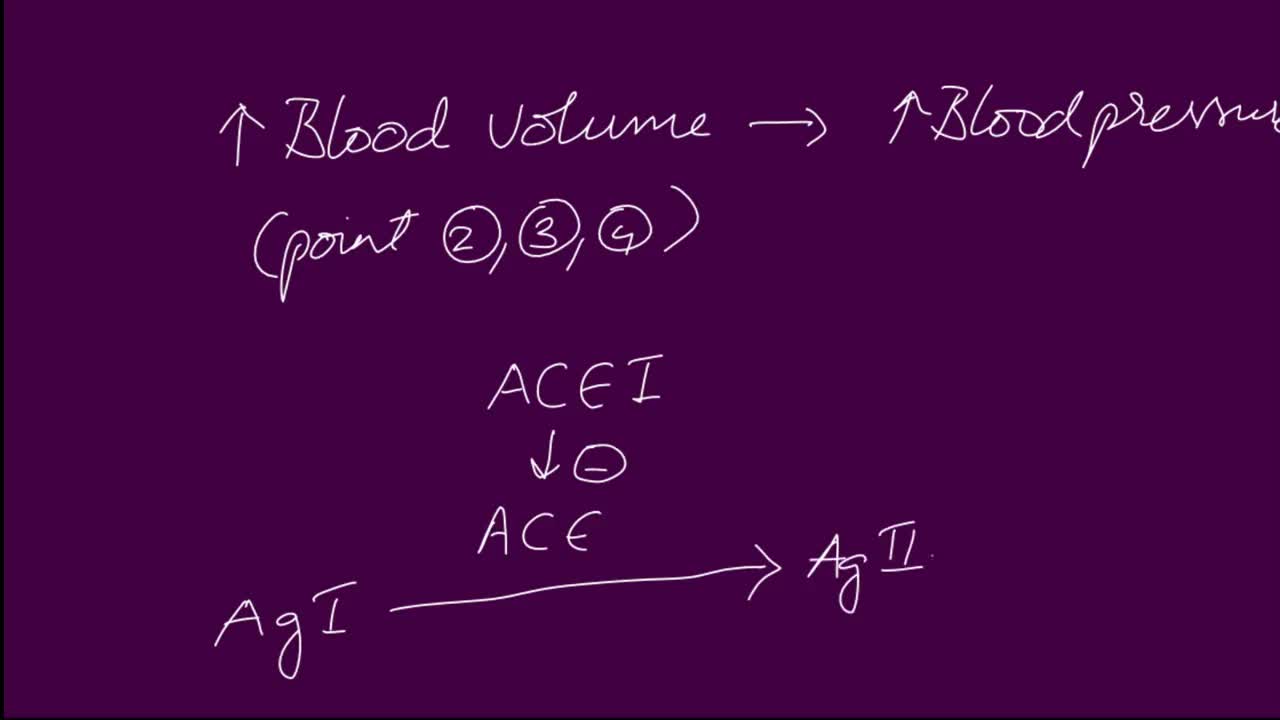
ACE Inhibitor Mechanisms. Angiotensin converting enzyme (ACE) inhibitors are agents used to relax blood vessels and lower blood pressure. They prevent an enzyme from producing angiotensin II, which narrows blood vessels and raises blood pressure, meaning the heart has to work harder to pump blood around the body.

www.diabetes.org > Living With Diabetes > Treatment and Care > Medication > Insulin & Other Injectables Share: Print PageText Size:A A A Listen How Do Insulin Pumps Work? If you have been diagnosed with diabetes, you may feel overwhelmed by all the new information you have learned and will continue to learn about managing your diabetes. You already know your main goal should be to get your blood glucose (sugar) levels under control in order to increase your chances of a complication-free life. Many people know this, but need to know how to achieve good diabetes management, while balancing the day-to-day demands of diabetes with other life demands. An insulin pump can help you manage your diabetes. By using an insulin pump, you can match your insulin to your lifestyle, rather than getting an insulin injection and matching your life to how the insulin is working. When you work closely with your diabetes care team, insulin pumps can help you keep your blood glucose levels within your target ranges. People of all ages with type 1 diabetes use insulin pumps and people with type 2 diabetes have started to use them as well. - See more at: http://www.diabetes.org/living-with-diabetes/treatment-and-care/medication/insulin/how-do-insulin-pumps-work.html?referrer=https://www.google.com/#sthash.XD56v351.dpuf