Top videos
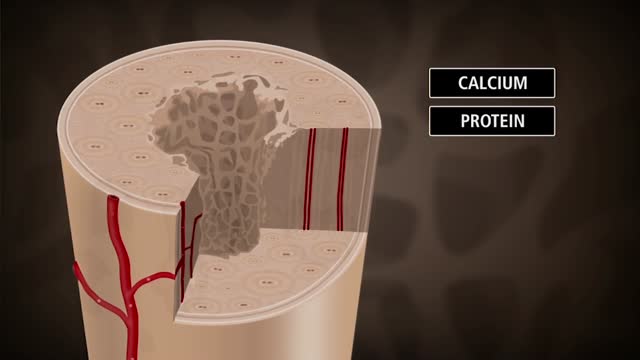
Bone is not a static part of the body — it's constantly being resorbed (broken down) and formed throughout your life. Your entire skeleton is replaced about every decade, according to the NIH. During your childhood and teenage years, bone formation occurs more quickly than bone resorption, resulting in growth. You reach your maximum bone density and strength around age 30, after which bone resorption slowly overtakes bone formation. Osteoporosis develops when there's an abnormal imbalance between bone resorption and formation — that is, resorption occurs too quickly, or formation too slowly.
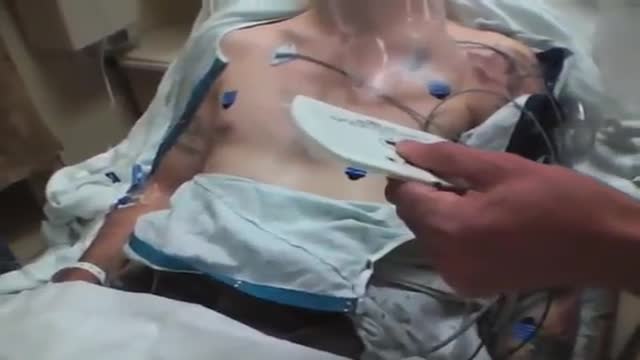
Electrical cardioversion is a procedure in which an electric current is used to reset the heart's rhythm back to its regular pattern (normal sinus rhythm). The low-voltage electric current enters the body through metal paddles or patches applied to the chest wall.

Acute mesenteric ischemia (AMI) is a syndrome caused by inadequate blood flow through the mesenteric vessels, resulting in ischemia and eventual gangrene of the bowel wall. Although relatively rare, it is a potentially life-threatening condition. Broadly, AMI may be classified as either arterial or venous. AMI as arterial disease may be subdivided into nonocclusive mesenteric ischemia (NOMI) and occlusive mesenteric arterial ischemia (OMAI); OMAI may be further subdivided into acute mesenteric arterial embolism (AMAE) and acute mesenteric arterial thrombosis (AMAT). AMI as venous disease takes the form of mesenteric venous thrombosis (MVT).

Pulmonary fibrosis is a condition in which the tissue deep in your lungs becomes scarred over time. This tissue gets thick and stiff. That makes it hard for you to catch your breath, and your blood may not get enough oxygen. Causes of pulmonary fibrosis include environmental pollutants, some medicines, some connective tissue diseases, and interstitial lung disease. Interstitial lung disease is the name for a large group of diseases that inflame or scar the lungs. In most cases, the cause cannot be found. This is called idiopathic pulmonary fibrosis
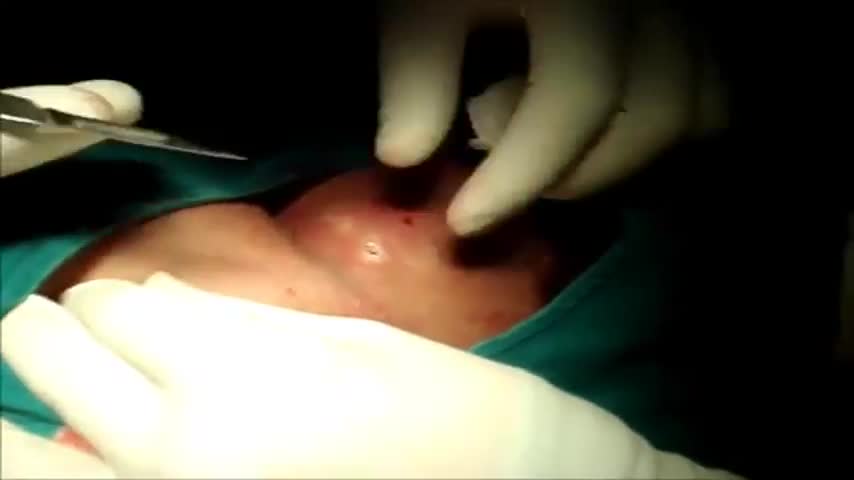
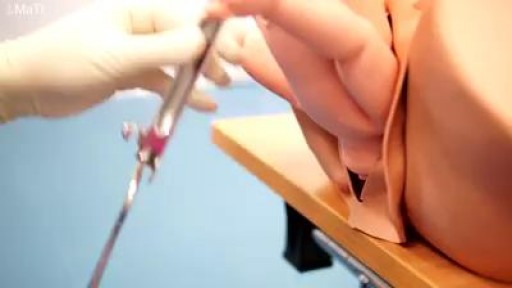
This is a 60 year man having large swelling of size 7cm x 5 cm behind neck for one year. Patient complained pain and tenderness over local area for 7 days and came to us.On examination punctum found in the centre of swelling and fluctuation positive.Infected sebaceous cyst diagnosis made. /nIncision and drainage surgery done under local anesthesia.all infected pultaceous material evacuated.Pus culture sent and antibiotics given as per sensitivity report./nPatient improved with daily dressing.
James Burke Fine DMD by James Burke Fine DMD Periodontal disease is a gum condition caused by the buildup of bacteria along and below the teeth's gumline. Acute forms are usually associated with pain from oral tissue gone bad – also known as necrotizing gingivitis or trench mouth – whereas chronic forms are painless but have a more long-term impact on your overall, systemic health. The most common chronic form is gingivitis, whose bleeding, puffiness and redness comes from an organized mass of bacteria called plaque. You may know it can advance into a form called periodontitis. If these conditions are left untreated, however, it can also lead to infections within other parts of the body, such as the lungs.
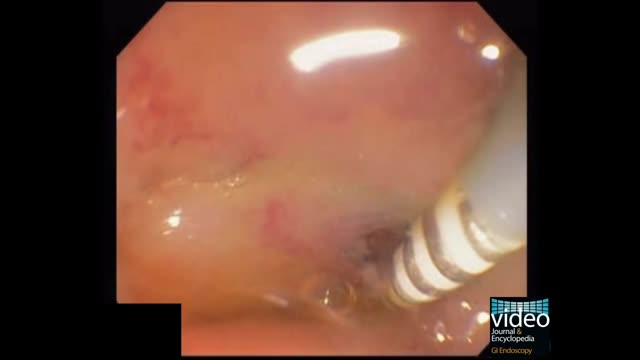
Upper gastrointestinal bleeding (sometimes upper GI, UGI bleed, Upper gastrointestinal hemorrhage, gastrorrhagia) refers to bleeding in the upper gastrointestinal tract, commonly defined as bleeding arising from the esophagus, stomach, or duodenum. In fact, the proportion of UGIB cases caused by peptic ulcer disease has declined, a phenomenon that is believed to be due to the use of proton pump inhibitors (PPIs) and H pylori therapy. Duodenal ulcers are more common than gastric ulcers, but the incidence of bleeding is identical for both.

http://smoking-videos.plus101.com
Quit Smoking Forever Formula Videos - How To Quit Smoking In As Fast As 1 Week Without Agitation, Cravings Or Withdrawal Symptoms.You're about to uncover the 3 elements that will rapidly boost your chances of success to quit smoking and not only that, you'll learn ways to escape cravings and how to avoid a relapse that can happen in the future even to people with the most willpower.
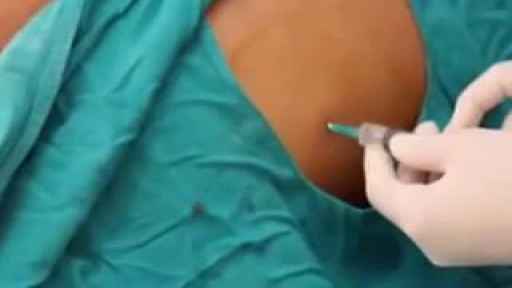
An untreated hepatic abscess is nearly uniformly fatal as a result of complications that include sepsis, empyema, or peritonitis from rupture into the pleural or peritoneal spaces, and retroperitoneal extension. Treatment should include drainage, either percutaneous or surgical. Antibiotic therapy as a sole treatment modality is not routinely advocated, though it has been successful in a few reported cases. It may be the only alternative in patients too ill to undergo invasive procedures or in those with multiple abscesses not amenable to percutaneous or surgical drainage. In these instances, patients are likely to require many months of antimicrobial therapy with serial imaging and close monitoring for associated complications.

Thoracic outlet syndrome is a disorders that occur when blood vessels or nerves in the space between your collarbone and your first rib (thoracic outlet) are compressed. This can cause pain in your shoulders and neck and numbness in your fingers. Common causes of thoracic outlet syndrome include physical trauma from a car accident, repetitive injuries from job- or sports-related activities, certain anatomical defects (such as having an extra rib), and pregnancy. Sometimes doctors can't determine the cause of thoracic outlet syndrome. Treatment for thoracic outlet syndrome usually involves physical therapy and pain relief measures. Most people improve with these approaches. In some cases, however, your doctor may recommend surgery.
Most babies will move into delivery position a few weeks prior to birth, with the head moving closer to the birth canal. When this fails to happen, the baby’s buttocks and/or feet will be positioned to be delivered first. This is referred to as “breech presentation.” Breech births occur in approximately 1 out of 25 full-term births.

An enlarged spleen may cause: No symptoms in some cases. Pain or fullness in the left upper abdomen that may spread to the left shoulder. Feeling full without eating or after eating only a small amount from the enlarged spleen pressing on your stomach. Anemia. Fatigue. Frequent infections. Easy bleeding.
Types of multiple myeloma. Multiple myeloma is the most common type of plasma cell cancer. The bones and bone marrow are the main sites where myeloma cells (abnormal plasma cells) are produced. The myeloma cells can form tumours, called plasmacytomas, in many bones in the body.