Top videos
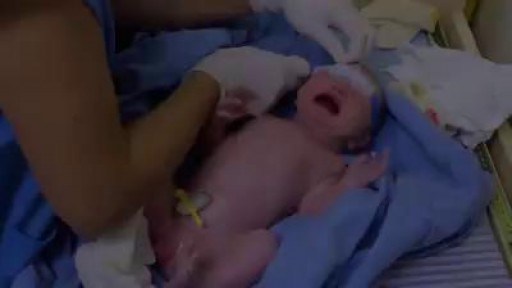
Childbirth (also called labour, birth, partus or parturition) is the culmination of a human pregnancy or gestation period with birth of one or more newborn infants from a woman’s uterus. The process of normal human childbirth is categorized in three stages of labour: the shortening and dilation of the cervix, descent and birth of the infant, and birth of the placenta. In some cases, childbirth is achieved through caesarean section, the removal of the neonate through a surgical incision in the abdomen, rather than through vaginal birth
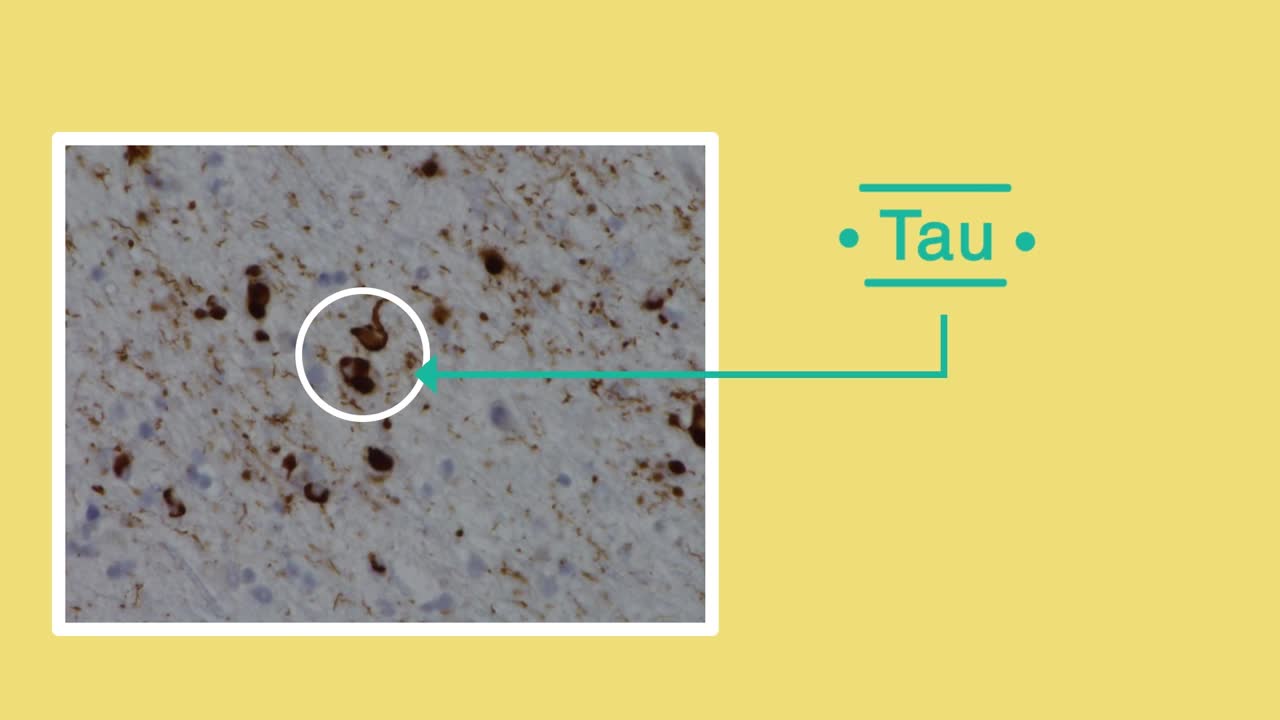
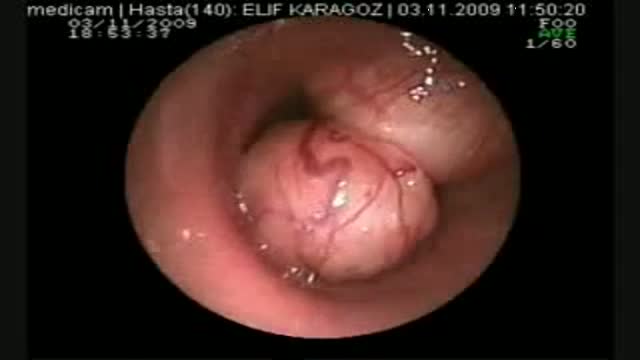
Frontotemporal dementia is the name for a range of conditions in which cells in the frontal and temporal lobes of the brain are damaged. These lobes control behaviour, emotional responses and language. This means that people will experience changes in personality and behaviour, or may struggle with language – for example, in finding the right word. Frontotemporal dementia is a less common form of dementia which is more likely to affect younger people – those under 65.

A spontaneous vaginal delivery (SVD) occurs when a pregnant woman goes into labor with or without use of drugs or techniques to induce labor, and delivers her baby in the normal manner, without forceps, vacuum extraction, or a cesarean section. Assisted vaginal delivery (AVD) occurs when a pregnant woman goes into labor with or without the use of drugs or techniques to induce labor, and requires the use of special instruments such as forceps or a vacuum extractor to deliver her baby vaginally.

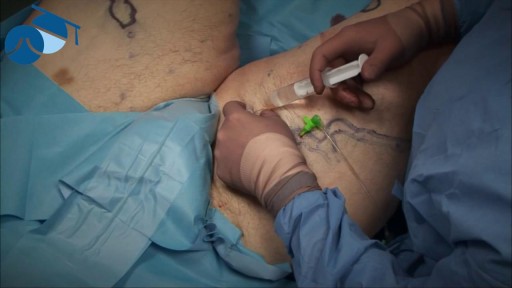
Macrobiopsy of breast lesions is a complicated procedure when performed with vacuum assisted biopsy tools. The Spirotome is a hand-held needle set that doesn't need capital investment, is ready to use and provides tissue samples of high quality in substantial amounts. In this way quantitative molecular biology is possible with one tissue sample. The Coramate is an automated version of this direct and frontal technology.

There is no sure way for women to avoid their most common type of cancer. But when breast cancer is found early, the survival chances are the greatest. Here is October’s survivor story:
It has been 25 years since a woman very dear to us here at CBS 11 News found out she was a living cliché. Following in her birth mother’s footsteps, she discovered breast cancer on her own. Today she’s alive, urging every woman she can reach to do a self-check.
We here at CBS 11 News have come to know Juneil Jones-Flemming’s soft, warm greeting.
Some of you may have too

Perdre Du Ventre, Comment Maigrir Des Cuisses, Regime Soupe, Prendre Du Muscle, Maigrir Des Hanches ---- http://perte-poids-rapide.info-pro.co --- Comment maigrir pour un homme ? Les régimes ne sont pas une exclusivité féminine et les hommes ont eux aussi des comptes à rendre à leur balance. Pour séduire, pour se sentir mieux dans leur corps, pour leur travail, ils ont eux aussi des raisons pour se délester de quelques kilos. Hommes et femmes : différentes face aux kilos Les hommes et les femmes ne réagissent pas de la même manière face au poids. Le corps non plus. La première différence est au niveau de la silhouette. La gente féminine va accumuler les kilos en trop au niveau des fesses et des cuisses alors que pour les hommes, la prise de poids se situe surtout au niveau du visage, du cou et du ventre. L’autre différence entre les hommes et les femmes est la faculté à perdre du poids. Si vous avez décidé de suivre un régime en couple, sachez Mesdames que les hommes maigrissent plus vite ! Cette « injustice » est expliquée par le fait que les hommes ou plutôt leur organisme, va brûler plus de calories au repos et à l’effort que les femmes grâce à leur masse corporelle plus importante. Par contre, ces dames sont plus motivées à tenir un régime sur la longueur. Les hommes et les régimes, c’est toute une histoire ! C’est pourquoi ils doivent faire un régime qui leur corresponde et qui est adapté à leur vie au quotidien ! Maigrir lorsque l’on est un homme Les hommes sont de plus en plus nombreux à vouloir perdre du poids. Surtout entre 40 et 45 ans. Mais même s’ils maigrissent plus vite que les femmes, la partie est loin d’être gagnée. Pourquoi ? Parce qu’il est plus compliqué pour eux de modifier leurs habitudes alimentaires. En effet, ce sont les vrais champions d’une alimentation riche en matières grasses, peu variée et très déséquilibrée. Il faut donc qu’ils adoptent de nouvelles habitudes alimentaires tout en conservant une certaines notion de plaisir et qu’ils combattent certaines mauvaises habitudes, souvent responsable de leurs kilos en trop. "Découvrez comment jean-jacques a réussi à perdre 3,2 kilos et 7 cm de tour de taille en 2 semaines, sans peser les aliments ni compter les calories." Cliquez ici: http://perte-poids-rapide.info-pro.co