Top videos
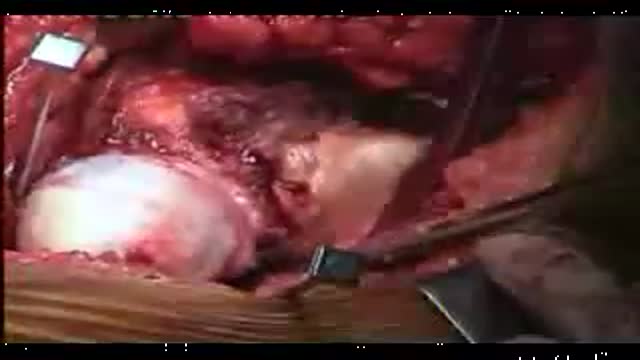
Another video of Dr.Vijay C. Bose from Apollo Speciality Hospital chennai perform Birmingham Hip Resurfacing Surgery procedure for a case of Avascular necrosis.The NCP ( Neck Capsule Preserving) approach is being used. Total hip replacement, hip resurfacing simply shaves and caps a few centimeters of bone within the joint. The bone-conserving approach of the Birmingham Hip Resurfacing System.
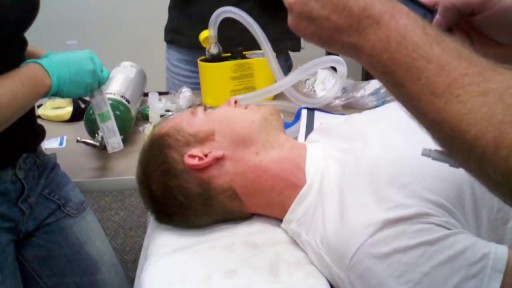
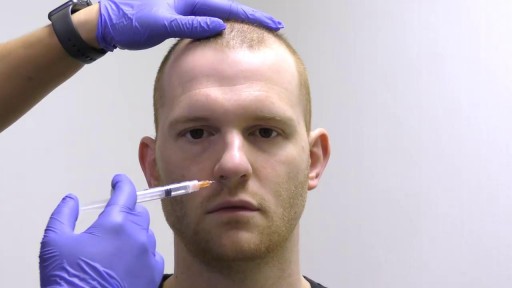
External jugular vein cannulation is an integral part of modern medicine and is practiced in virtually every health care setting. Venous access allows sampling of blood, as well as administration of fluids, medications, parenteral nutrition, chemotherapy, and blood products. [1] This topic describes placement of an intravenous (IV) catheter into the external jugular vein. A similar technique can be used for placement of IV catheters at different anatomic sites.

Testing for the four features of Gerstmann Syndrome in this patient with two separate left sided strokes (left frontoparietal ischaemic stroke followed by left posterior parietal haemorrhagic stroke). He exhibits (i) acalculia, (ii) agraphia, (iii) left-right disorientation, and (iv) finger agnosia. Complicating the issue is his obvious nonfluent aphasia (expressive dysphasia) with paraphasic errors (replacing words with associated words (e.g. says 'fork' instead of 'spoon')) and some comprehension issues.
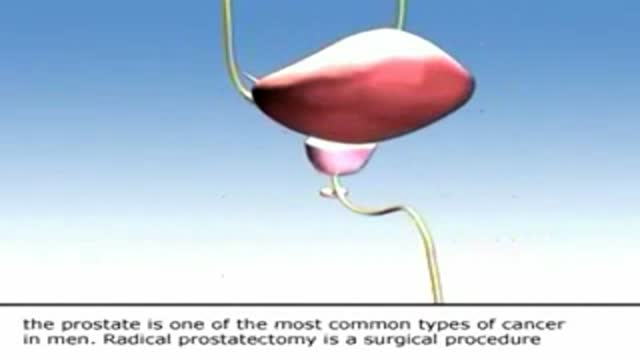
This is an educational video for the prostate cancer patients and their families. Depending on the individual patient, a radical prostatectomy, might be a procedure that your urologist could recommend as treatment. Here is a brief demonstration of this procedure.
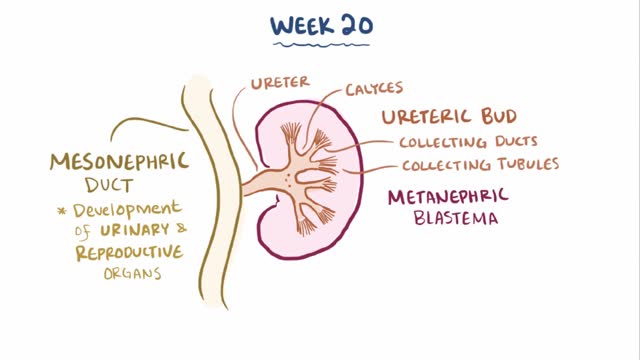
Renal agenesis is a condition in which a newborn is missing one or both kidneys. Unilateral renal agenesis (URA) is the absence of one kidney. Bilateral renal agenesis (BRA) is the absence of both kidneys. Both types of renal agenesis occur in fewer than 1 percent of births annually, according to the March of Dimes. Fewer than 1 in every 1,000 newborns has URA. BRA is much rarer, occurring in about 1 in every 3,000 births.

Glomus tumors are rare soft tissue neoplasms that typically present in adults (ages 20-40 years) as small, blue-red papules or nodules of the distal extremities, with most cases involving subungual sites. These tumors are typically painful, often causing paroxysmal pain in response to temperature changes or pressure. Glomus tumors are thought to arise from the glomus body, a thermoregulatory shunt concentrated in the fingers and toes. Most lesions are solitary and localized to cutaneous sites; however, generalized glomuvenous malformations, or multiple glomangiomas, have also been described, and may have extracutaneous involvement.

A lumbar puncture (also called a spinal tap) is a procedure to collect and look at the fluid (cerebrospinal fluid, or CSF) surrounding the brain and spinal cord. During a lumbar puncture, a needle is carefully inserted into the spinal canal low in the back (lumbar area). Samples of CSF are collected.
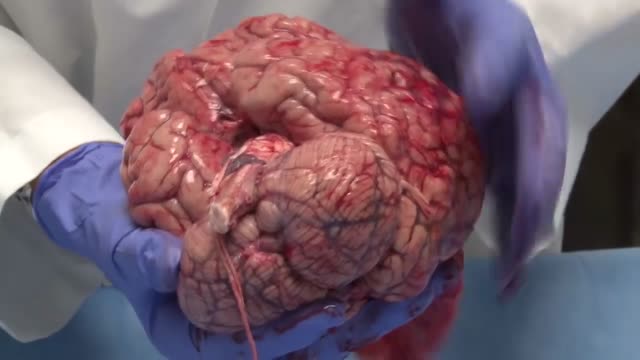
The human brain is the command center for the human nervous system. It receives input from the sensory organs and sends output to the muscles. The human brain has the same basic structure as other mammal brains, but is larger in relation to body size than any other brains.
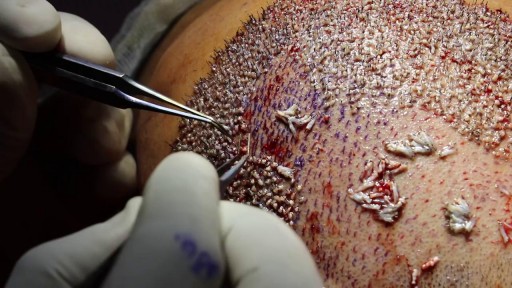
This implantation method is very common and used in both FUE hair transplant surgery and strip surgery (FUSS). During this implantation method, site creation and graft implantation are performed simultaneously as part of a one or two step process.

#dialysis #hemodialysis #kidneys
Follow us: https://www.instagram.com/7activestudio/
For more information:
www.7activestudio.com
7activestudio@gmail.com
Contact: +91- 9700061777, 040-66564777
7 Active Technology Solutions Pvt.Ltd. is an educational 3D digital content provider for K-12. We also customise the content as per your requirement for companies platform providers colleges etc . 7 Active driving force "The Joy of Happy Learning" -- is what makes difference from other digital content providers. We consider Student needs, Lecturer needs and College needs in designing the 3D & 2D Animated Video Lectures. We are carrying a huge 3D Digital Library ready to use.
Voice Over Credit: Muls N Ravs Entertainment Pvt. Ltd. (www.mulsnravs.com)

Hypercalcemia is a condition in which the calcium level in your blood is above normal. Too much calcium in your blood can weaken your bones, create kidney stones, and interfere with the way your heart and brain works. Hypercalcemia most commonly results from overactive parathyroid glands. These four tiny glands are each about the size of a grain of rice and are located on or near the thyroid gland. Other causes of hypercalcemia include cancer, certain other medical disorders, some medications, and excessive use of calcium and vitamin D supplements. Signs and symptoms of hypercalcemia may range from nonexistent to severe. Treatment depends on the underlying cause.
This video is available for instant download licensing here: https://www.alilamedicalmedia.....com/-/galleries/all-
©Alila Medical Media. All rights reserved.
Support us on Patreon and get FREE downloads and other great rewards: patreon.com/AlilaMedicalMedia
All images/videos by Alila Medical Media are for information purposes ONLY and are NOT intended to replace professional medical advice, diagnosis or treatment. Always seek the advice of a qualified healthcare provider with any questions you may have regarding a medical condition.
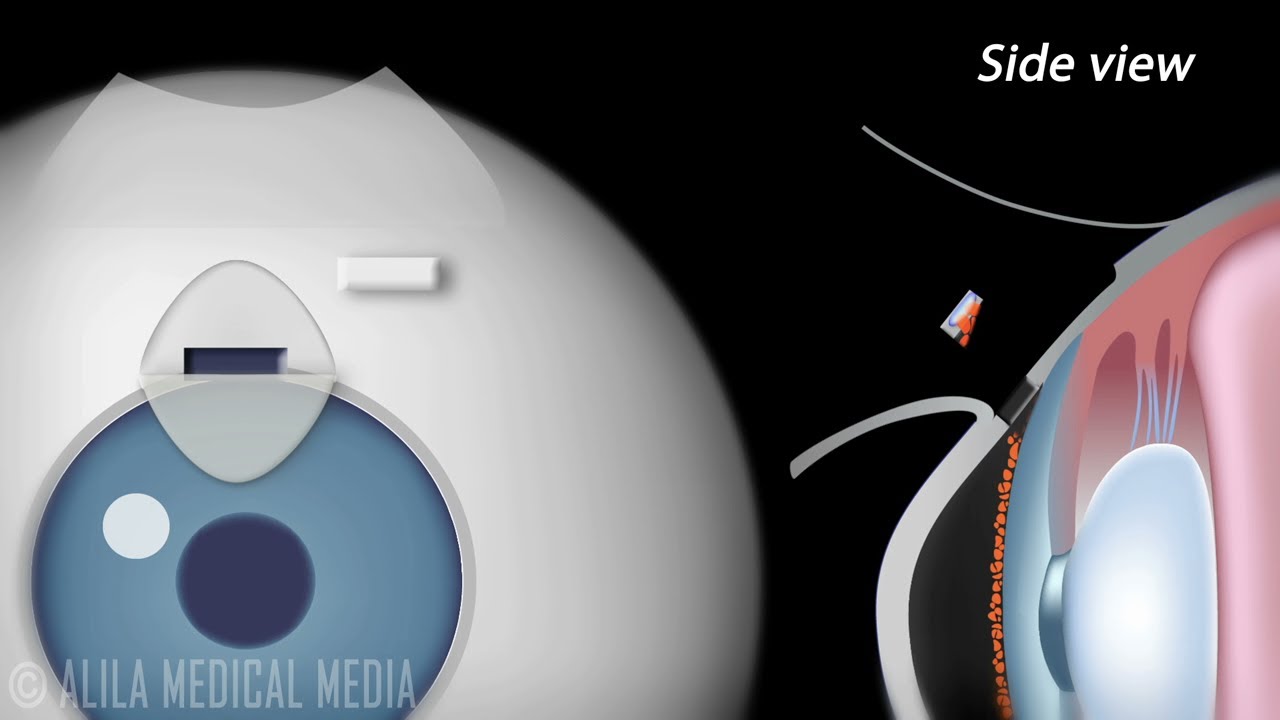
Trabeculectomy, also called Filtration Surgery, is a surgical procedure performed for treatment of glaucoma. The treatment involves removing part of the trabecular meshwork and creating a new escape route for the aqueous humor. When successful, it allows the aqueous fluid to drain from the eye into an area underneath the conjunctiva where it is subsequently absorbed by the body's circulatory system or filtered into tears.
In this procedure:
- A conjunctival pocket is created and maybe treated with Mitomycin or other antimetabolites for a few minutes. These drugs are used to prevent scarring of the operation site. Scarring, if occurs, may clog the new drainage canal, and is therefore the major reason the procedure may fail.
- A half thickness flap is then made in the sclera and is dissected all the way to the clear cornea.
- A block of scleral tissue including part of the trabecular meshwork and Schlemm's canal is then removed to make a hole into the anterior chamber of the eye.
- As the iris may plug up this hole from the inside, a piece of the iris maybe removed at this time. This is called iridectomy.
- The scleral flap is then sutured loosely back in place. These sutures can be released gradually during a couple of weeks after surgery. This allows adjustment of the aqueous flow in order to achieve target pressure and to avoid the complication of having a too low intraocular pressure.
- The conjunctiva is sewn back in place to cover the area.
After surgery, aqueous humor drains into a filtering area called a "bleb" under the conjunctiva. Since the surgery is usually performed near the top of the eye, the bleb can easily be concealed behind the upper eyelid.