Top videos

How To Increase Brain Power, How To Increase Brain Activity, How To Boost Your Concentration--- http://brain-revitalizer.info-pro.co --- Improve Concentration, Ask anyone today what they have a hard time with and more often than not they are likely to cite trouble focusing or concentrating. With laptops, smart phones, television, GPS systems and social media, it is hard to block out all the distractions when you need to focus on something specific. Attention deficit disorder may be one of the most popular excuses for our lack of concentration, but it's not an entirely accurate diagnosis since many of us simply aren't training our brains the right way to improve our focus. Concentration is necessary just to make it through a typical workday. From driving and working to shopping and cooking, focus is essential in order to get tasks accomplished. Unfortunately many of us have a hard time zoning in on a specific project and seeing it through to completion. Being easily distracted is not necessarily a disorder but it will keep you from managing your time wisely and getting done the important things that need your attention. There are several ways people can improve their concentration, including strategic brain games and exercises, along with guided meditation and brainwave entrainment. Research has shown that the more a person trains their brain in specific skill sets, the better one can get at cognitive thinking, problem solving and memorization. Using computer generated pulses, or isochronic tones, during brain entrainment meditation is another way to synchronize your brain's frequencies so you can operate on a fast or slow frequency that will assist in achieving states of productivity or relaxation. As we all know, when we are relaxed our concentration and decision making are much better than if we are under stress or hurried. Being able to tap in to specific Alpha, Theta and Delta waves allows us to synchronize our brainwaves with sound pulses so we can be more focused on specific projects and tasks. But YOU can be different! You can use Genius Brain Power to empower your brain so that you come alive with more energy, learn quicker, think more creatively, focus on your work like never before and drastically reduce stress with amazingly deep states of relaxation and meditation. click here: http://brain-revitalizer.info-pro.co
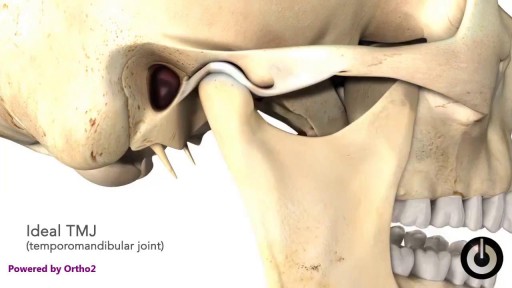
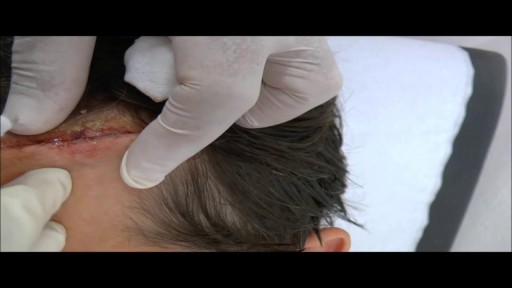
What Causes TMD? We don’t know what causes TMD. Dentists believe symptoms arise from problems with the muscles of your jaw or with the parts of the joint itself. Injury to your jaw, the joint, or the muscles of your head and neck -- like from a heavy blow or whiplash -- can lead to TMD. Other causes include: Grinding or clenching your teeth, which puts a lot of pressure on the joint Movement of the soft cushion or disc between the ball and socket of the joint Arthritis in the joint Stress, which can cause you to tighten facial and jaw muscles or clench the teeth

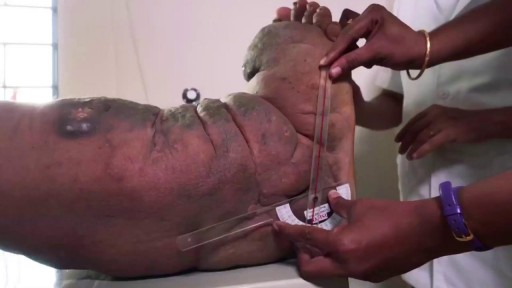
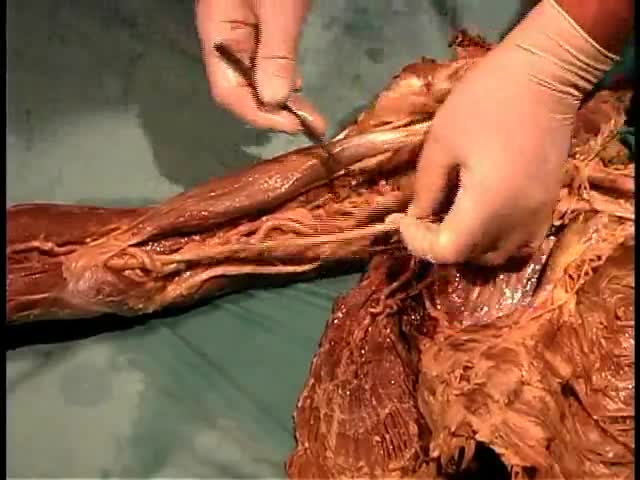
urgical management of proximal humerus fractures may be categorized either according to fracture type (eg, Neer type, anatomic type, greater tuberosity, surgical neck, anatomic neck, articular surface, lesser tuberosity fragments) or according to method of fixation (eg, closed reduction with no fixation, percutaneous fixation, open reduction with internal fixation [ORIF], humeral head replacement associated with tuberosity fixation

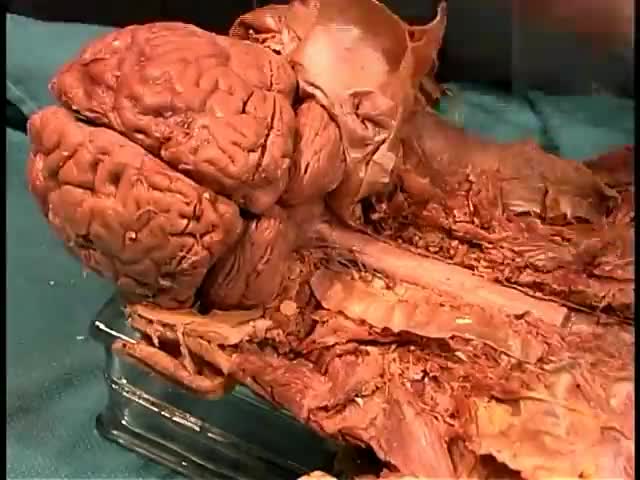
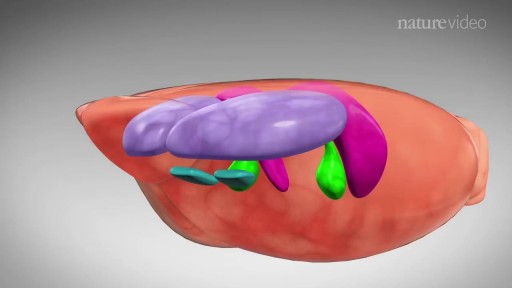
A seizure occurs when there’s abnormal electrical activity in the brain. Seizures may go virtually unnoticed. Or, in severe cases, they may produce a change or loss of consciousness and involuntary muscle spasms called convulsions. Seizures usually come on suddenly and vary in duration and severity. A seizure may be a one-time event, or you may have seizures repeatedly. Recurrent seizures are called epilepsy, or a seizure disorder. Less than one in 10 people who has a seizure develops epilepsy. Experts classify seizures into two general categories and many subtypes based on the pattern of the attack. Generalized seizures involve both sides of the brain from the start of the attack. Common subtypes include tonic-clonic (grand mal) and absence seizures (petit mal). Febrile and infantile spasms are two types of generalized seizures that occur almost exclusively in young children. Partial (or focal) seizures are the second major seizure type. These begin in a specific area of the brain and may be contained there. Or they may spread to the entire brain. With simple partial seizures, the person remains conscious. Complex partial seizures involve impaired consciousness. What Causes Seizures? Often the cause of a seizure is unknown. Many conditions can provoke seizures, including: Stroke Brain tumors Head injuries Electrolyte imbalance Very low blood sugar Repetitive sounds or flashing lights, such as in video games Medications, such as antipsychotics and some asthma drugs Withdrawal from medications, such as Xanax, narcotics, or alcohol Use of drugs such as cocaine and heroin Cancer Brain infections, such as meningitis