Top videos

Plastic Surgery New York Dr. Carlin Vickery of 5th Avenue Aesthetics Surgery in Manhattan
(http://www.5thavesurgery.com) speaks at a Fab Over 50 event on having great breasts after the age
of 50. In this presentation Dr. Carlin shares patient results by providing before and after pictures from
different types of breast surgeries including breast lifts, implants and reductions.

Hipertension Arterial Pdf, Hipertension Esencial, Hipertension Pulmonar Tratamiento
http://bajar-presion-arterial.good-info.co
Lo Que Todos Necesitan Saber Sobre La Presión Arterial Alta
Si le han dicho que tiene presión arterial alta, usted puede decir, "Pero me siento muy bien!" Esto se debe a que la hipertensión o la presión arterial alta no tiene síntomas visibles. Es por eso que se la describe a menudo como el "asesino silencioso". No hay achaques o limitaciones físicas sólo porque tiene la presión arterial alta. Entonces, por qué siquiera preocuparse?
La hipertensión afecta a uno de cada tres adultos estadounidenses, y muchas de estas personas ni siquiera saben que la tienen. Además, aquellos con presión arterial alta tienen también un mayor riesgo de tener el colesterol alto.
Haga clic en el enlace de abajo para comprobar que funciona
http://bajar-presion-arterial.good-info.co
Suscríbete a nuestro canal
http://bajar-presion-arterial.blogspot.com/
https://www.youtube.com/watch?v=wQU4dgC1FM8
Hipertension Arterial Pdf, Hipertension Esencial, Hipertension Pulmonar Tratamiento,
hipertension renal,
hipertension en embarazo,
hipertension alimentacion,
hipertension arterial diagnostico,
hipertension arterial sistolica,
hipertension remedios naturales,
hipertension pulmonar leve,
hipertension arterial prevencion,
embarazo e hipertension,
diagnostico de hipertension,
sintomas de tension arterial alta,
remedios caseros hipertension

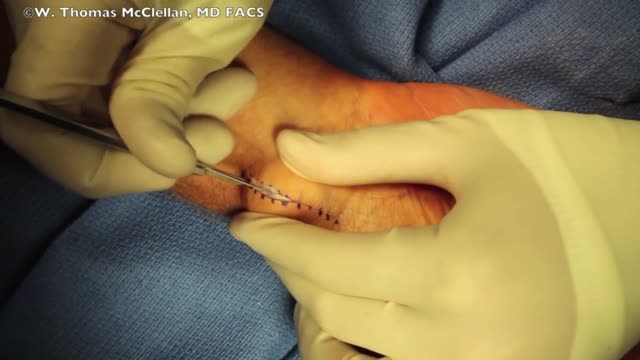
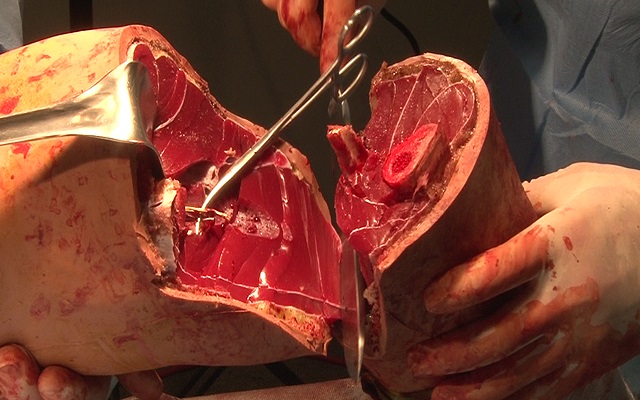
Lumbar puncture is a common emergency department procedure used to obtain information about the cerebrospinal fluid (CSF) for diagnostic and, less commonly, therapeutic reasons. Please refer to the full article on Lumbar Puncture for more details on the lumbar puncture procedure. Lumbar puncture is typically performed via “blind” surface landmark guidance. The surface landmark technique is reported to be successful in a high percentage of attempted lumbar punctures; however, surface landmark identification of underlying structures has been shown to be accurate only 30% of the time. [1] Unsuccessful identification of proper landmarks often leads to increased difficulty in obtaining CSF, if the procedure is performed, and a higher rate of complications. Few alternatives are available in these cases. If available, fluoroscopic-guided lumbar puncture may be performed. If not, treatment is sometimes initiated empirically without obtaining CSF. Disadvantages of using fluoroscopy include limited availability or necessary transport of the patient outside of the emergency department, inability to directly visualize the spinal canal, and inherent radiation exposure
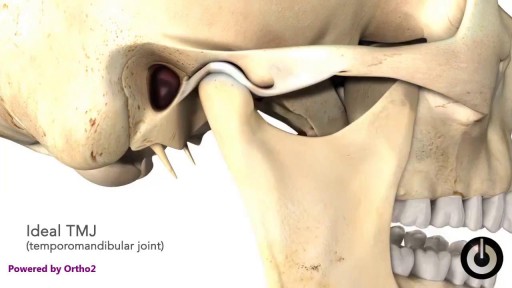
What Causes TMD? We don’t know what causes TMD. Dentists believe symptoms arise from problems with the muscles of your jaw or with the parts of the joint itself. Injury to your jaw, the joint, or the muscles of your head and neck -- like from a heavy blow or whiplash -- can lead to TMD. Other causes include: Grinding or clenching your teeth, which puts a lot of pressure on the joint Movement of the soft cushion or disc between the ball and socket of the joint Arthritis in the joint Stress, which can cause you to tighten facial and jaw muscles or clench the teeth

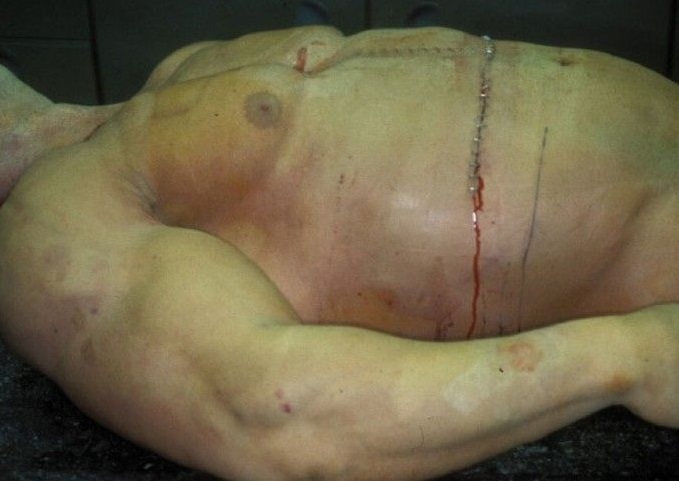
procedure is usually done in the hospital or outpatient surgical center under general anesthesia (while you are asleep and pain-free). The procedure is performed in the following way: The surgeon makes a small cut (incision) below the belly button (navel). A needle or tube is inserted into the incision. Carbon dioxide gas is passed into the abdomen through the needle or tube. The gas helps expand the area, giving the surgeon more room to work, and helping the surgeon see the organs more clearly. A tube is placed through the cut in your abdomen. A tiny video camera (laparoscope) goes through this tube and is used to see the inside of your pelvis and abdomen. More small cuts may be made if other instruments are needed to get a better view of certain organs. If you are having gynecologic laparoscopy, dye may be injected into your cervix area so the surgeon can view your fallopian tubes. After the exam, the gas, laparoscope, and instruments are removed, and the cuts are closed. You will have bandages over those areas.
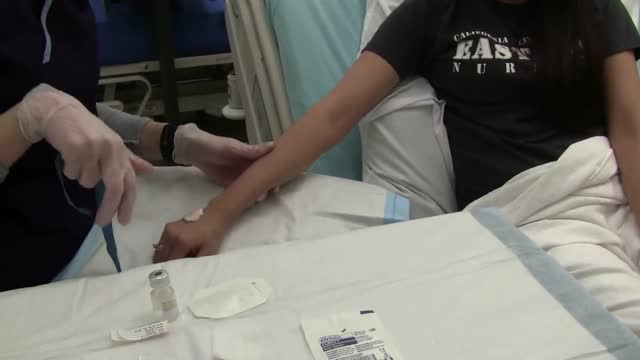
IV cannulation is a skill that has scared a lot of student nurses and even professionals. Perhaps it’s because IV insertion is an invasive procedure, and nurses are too worried that they might hurt their patients. Or maybe it’s because they are just clueless about IV therapy do’s and don’ts–things that one can only fully understand through constant practice.

A seizure occurs when there’s abnormal electrical activity in the brain. Seizures may go virtually unnoticed. Or, in severe cases, they may produce a change or loss of consciousness and involuntary muscle spasms called convulsions. Seizures usually come on suddenly and vary in duration and severity. A seizure may be a one-time event, or you may have seizures repeatedly. Recurrent seizures are called epilepsy, or a seizure disorder. Less than one in 10 people who has a seizure develops epilepsy. Experts classify seizures into two general categories and many subtypes based on the pattern of the attack. Generalized seizures involve both sides of the brain from the start of the attack. Common subtypes include tonic-clonic (grand mal) and absence seizures (petit mal). Febrile and infantile spasms are two types of generalized seizures that occur almost exclusively in young children. Partial (or focal) seizures are the second major seizure type. These begin in a specific area of the brain and may be contained there. Or they may spread to the entire brain. With simple partial seizures, the person remains conscious. Complex partial seizures involve impaired consciousness. What Causes Seizures? Often the cause of a seizure is unknown. Many conditions can provoke seizures, including: Stroke Brain tumors Head injuries Electrolyte imbalance Very low blood sugar Repetitive sounds or flashing lights, such as in video games Medications, such as antipsychotics and some asthma drugs Withdrawal from medications, such as Xanax, narcotics, or alcohol Use of drugs such as cocaine and heroin Cancer Brain infections, such as meningitis

How do you assess cerebellar function? Ask them to do this as fast as possible while you slowly move your finger. Repeat the test with the other hand. Perform the heel-to-shin test. Have the patient lying down for this and get them to run the heel of one foot down the shin of the other leg, and then to bring the heel back up to the knee and start again.