Top videos
IV cannulation is a skill that has scared a lot of student nurses and even professionals. Perhaps it’s because IV insertion is an invasive procedure, and nurses are too worried that they might hurt their patients. Or maybe it’s because they are just clueless about IV therapy do’s and don’ts–things that one can only fully understand through constant practice.

procedure is usually done in the hospital or outpatient surgical center under general anesthesia (while you are asleep and pain-free). The procedure is performed in the following way: The surgeon makes a small cut (incision) below the belly button (navel). A needle or tube is inserted into the incision. Carbon dioxide gas is passed into the abdomen through the needle or tube. The gas helps expand the area, giving the surgeon more room to work, and helping the surgeon see the organs more clearly. A tube is placed through the cut in your abdomen. A tiny video camera (laparoscope) goes through this tube and is used to see the inside of your pelvis and abdomen. More small cuts may be made if other instruments are needed to get a better view of certain organs. If you are having gynecologic laparoscopy, dye may be injected into your cervix area so the surgeon can view your fallopian tubes. After the exam, the gas, laparoscope, and instruments are removed, and the cuts are closed. You will have bandages over those areas.
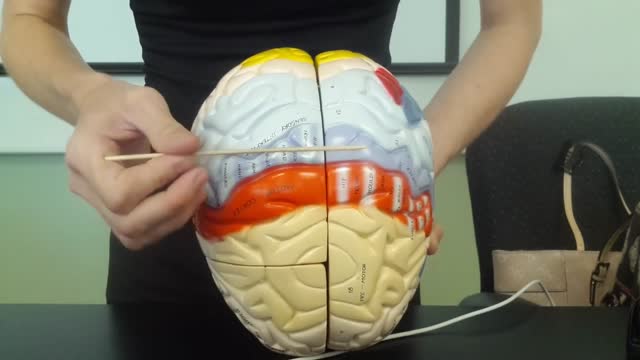
The brain is that part of the CNS contained within the cranial cavity (figure 13.1). It is the control center for many of the body's functions. The brain is much like a complex central computer but with additional functions that no computer can as yet match. Indeed, one goal in computer technology is to make computers that can function more like the human brain. The brain consists of the brainstem, the cerebellum, the diencephalon, and the cerebrum (table 13.1). The brainstem includes the medulla oblongata, pons, midbrain, and reticular formation. The structure of the brain is described in this chapter. Its functions are primarily discussed in chapter 14. Twelve pairs of cranial nerves, which are part of the PNS, arise directly from the brain. Two pairs arise from the cerebrum, nine pairs arise from the brainstem, and one pair arises from the spinal cord.

Lip augmentation is a cosmetic procedure that can give you fuller, plumper lips. These days, an injectable dermal filler is the most commonly used method of lip augmentation. There are many types of dermal fillers that can be injected in your lips and around your mouth.

A seizure occurs when there’s abnormal electrical activity in the brain. Seizures may go virtually unnoticed. Or, in severe cases, they may produce a change or loss of consciousness and involuntary muscle spasms called convulsions. Seizures usually come on suddenly and vary in duration and severity. A seizure may be a one-time event, or you may have seizures repeatedly. Recurrent seizures are called epilepsy, or a seizure disorder. Less than one in 10 people who has a seizure develops epilepsy. Experts classify seizures into two general categories and many subtypes based on the pattern of the attack. Generalized seizures involve both sides of the brain from the start of the attack. Common subtypes include tonic-clonic (grand mal) and absence seizures (petit mal). Febrile and infantile spasms are two types of generalized seizures that occur almost exclusively in young children. Partial (or focal) seizures are the second major seizure type. These begin in a specific area of the brain and may be contained there. Or they may spread to the entire brain. With simple partial seizures, the person remains conscious. Complex partial seizures involve impaired consciousness. What Causes Seizures? Often the cause of a seizure is unknown. Many conditions can provoke seizures, including: Stroke Brain tumors Head injuries Electrolyte imbalance Very low blood sugar Repetitive sounds or flashing lights, such as in video games Medications, such as antipsychotics and some asthma drugs Withdrawal from medications, such as Xanax, narcotics, or alcohol Use of drugs such as cocaine and heroin Cancer Brain infections, such as meningitis
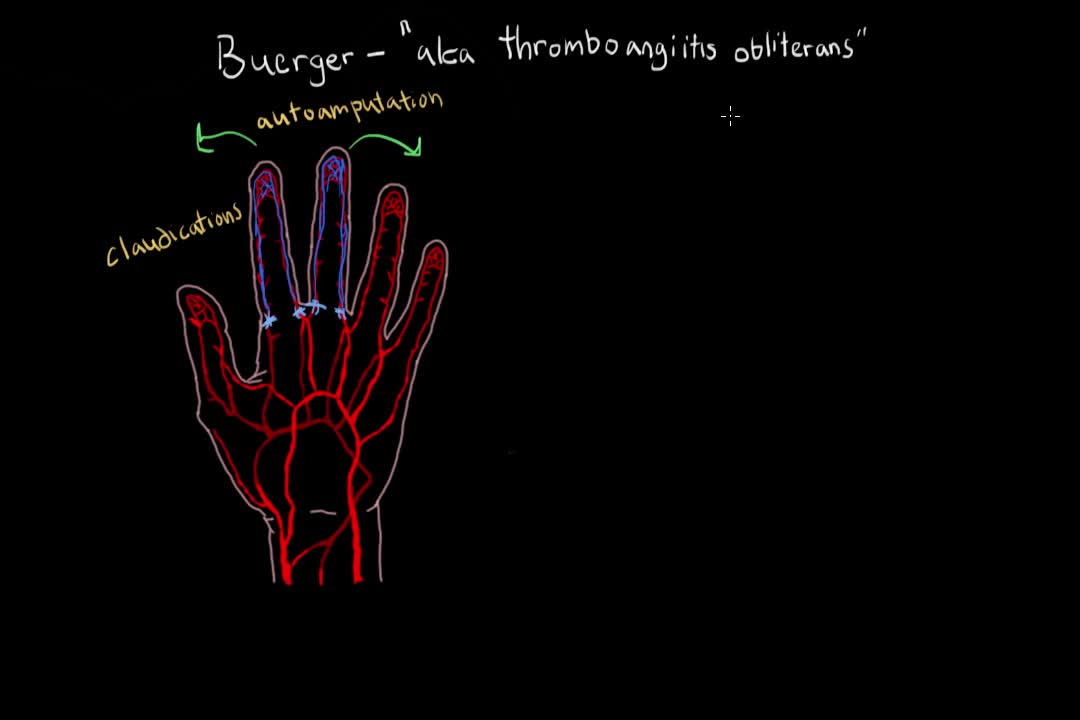
Buerger's disease (thromboangiitis obliterans) is a rare disease of the arteries and veins in the arms and legs. In Buerger's disease, your blood vessels become inflamed, swell and can become blocked with blood clots (thrombi). This eventually damages or destroys skin tissues and may lead to infection and gangrene. Buerger's disease usually first shows in your hands and feet and may eventually affect larger areas of your arms and legs. Virtually everyone diagnosed with Buerger's disease smokes cigarettes or uses other forms of tobacco, such as chewing tobacco. Quitting all forms of tobacco is the only way to stop Buerger's disease. For those who don't quit, amputation of all or part of a limb is sometimes necessary.

Optimal blood pressure typically is defined as 120 mm Hg systolic — which is the pressure as your heart beats — over 80 mm Hg diastolic — which is the pressure as your heart relaxes. For your resting heart rate, the target is between 60 and 100 beats per minute (bpm)

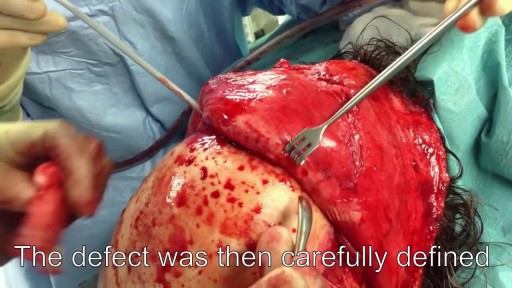
Highlights of a fetal laser surgery for twin-to-twin transfusion syndrome (TTTS) will be shown from Tampa General Hospital
TTTS affects 10 to 15 percent of identical-twin pregnancies and is the result of abnormal blood exchange between identical twins through a common placenta. The larger of the twins, or recipient, is surrounded by too much amniotic fluid and in danger of heart failure as its body tries to pump the overwhelming volume of blood intended for both. The smaller, or donor twin, is encased in a shrinking amniotic sac deprived of blood. Without treatment, both will likely die.
Rubén Quintero, M.D., Medical Director of Maternal Fetal Medicine/Fetal Surgery at Tampa General Hospital and Professor and Director of the Division of Maternal Fetal Medicine, Department of Obstetrics and Gynecology, University of South Florida College of Medicine will narrate the procedure and answer e-mail questions live as taped highlights of the procedure are shown.
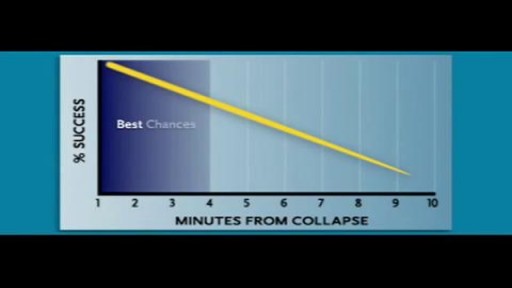
Cardiac arrest usually results from an electrical disturbance in the heart. It's not the same as a heart attack. The main symptom is loss of consciousness and unresponsiveness. This medical emergency needs immediate CPR or use of a defibrillator. Hospital care includes drugs, an implantable device, or other procedures.