Top videos

Patient 65-year-old of age who comes to the medical consultation with pain moderated pain in the right hypochondrium of “several years of evolution” but that it increased one week ago. Also, she shows pain in the umbilical region of “many years of evolution”, that is supported according to the patient - in a constant way.rnTo the examination, we observe an umbilical hernia, apparently divided into two parts. The hernia of the external region measures 25.1 centimeters x 18.0 centimeters and the one that occupies the average region measures 12.0 centimeters x 10.0 centimeters.rnPatient who comes to the medical consultation with moderated pain in the right hypochondrium of one year of evolution but it increased one week ago after eat duck.rnIn the ultrasound scan of the region of the right hypochondrium (patient came having breakfast, that is to say, without previous preparation ) we can observe the liver of 123.8 millimeters high, as well as the porta vein with a diameter of 7.3 millimeters.rnOn having observed the Gallbladder, we think that a side wall is increased in 2.7 mm (hyperechogenic) with several “echogenics points” in the interior (”Biliary Mud”).
The measurements of the gallbladder were: 39.0 x 17.4 millimeters.rnWe can appreciates an echogenic image in the interior that it would make think about stone. The stones are identified as echogenic foci casting acoustic shadowing but but this image did not appear and a re-evaluation is decided in 15 days.
Acalculous cholecystopathy which means disease or condition of the gallbladder without the presence of gallstones. You might also call it functional gallbladder disorder or impaired gallbladder emptying. Some causes may be chronic inflammation, a problem with the smooth muscles of the gallbladder or the muscle of the Sphincter of Oddi being too tight.
REMEMBER:
Umbilical hernia is a congenital malformation, especially common in infants of African descent, and more frequent in boys. An Acquired umbilical hernia directly results from increased intra-abdominal pressure and are most commonly seen in obese individuals.
Presentation:A hernia is present at the site of the umbilicus (commonly called a navel, or belly button) in the newborn; although sometimes quite large, these hernias tend to resolve without any treatment by around the age of 5 years. Obstruction and strangulation of the hernia is rare because the underlying defect in the abdominal wall is larger than in an inguinal hernia of the newborn. The size of the base of the herniated tissued is inversely correlated with risk of strangulation (i.e. narrow base is more likely to strangulate).
Babies are prone to this malformation because of the process during fetal development by which the abdominal organs form outside the abdominal cavity, later returning into it through an opening which will become the umbilicus.
Differential diagnosisrnImportantly this type of hernia must be distinguished from a paraumbilical hernia which occurs in adults and involves a defect in the midline near to the umbilicus, and from omphalocele.

A successful cardiovascular exam includes visual examination, palpation of the apical impulse, auscultation of Erb's point, auscultation of the carotids, and auscultation over the four different heart valve locations (aortic, pulmonic, tricuspid, and mitral). Additionally, the radial pulse is palpated while auscultating to distinguish whether a murmur is diastolic or systolic.
Video Index:
0:13 - Inspection of the thorax
0:29 - Palpation of the apex heart beat
0:59 - Auscultation of the heart
1:16 - Auscultation of the Erb’s point
1:33 - Using Erb’s point to check the heart rate
1:45 - Systolic and diastolic heart sound identification
2:01 - Ascultating individual valves: aortic, pulmonary, tricuspid, mitral
2:41 - Ascultation of the carotids
2:54 - Ascultating the pulmonary and aortic valves
3:04 - Ascultation of the mitral valve
3:16 - Mitral valve murmurs
Subscribe to AMBOSS YouTube for the latest clinical examination videos, medical student interviews, study tips and tricks, and live webinars!
Free 5 Day Trial: https://go.amboss.com/amboss-YT
Instagram: https://www.instagram.com/amboss_med/
Facebook: https://www.facebook.com/AMBOSS.Med/
Twitter: https://twitter.com/ambossmed
Blog: https://blog.amboss.com/us
#CardiovascularExamination #AuscultationOfTheHeart #USMLE #AMBOSSMed

The condition is caused by a blockage in the lymphatic system, part of the immune and circulatory systems. Lymphedema is most commonly caused by lymph node removal or damage due to cancer treatment. The main symptom is swelling in an arm or leg that may be accompanied by pain or discomfort. Exercise, wrapping, massage, and compression can help.

Alcoholic hepatitis can occur in people who drink heavily for many years. Symptoms include yellow skin and eyes along with increasing belly size due to fluid accumulation. Treatment involves hydration, nutritional care, and stopping alcohol use. Steroid drugs can help reduce liver inflammation.
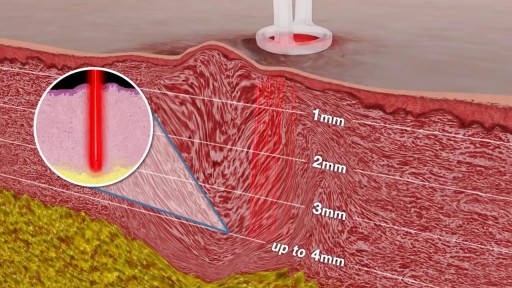
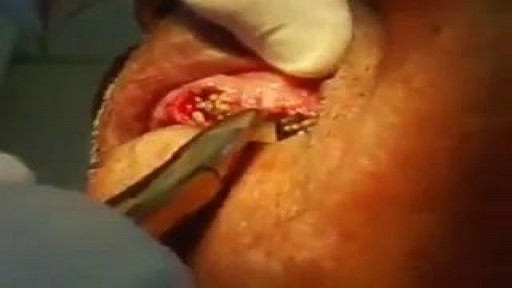
Scar revision includes techniques that improve the appearance of an unsightly scar, regardless of its size, type or age. This is typically not covered by insurance carriers and is treated as a cosmetic procedure. Though scars can never be completely removed, the appearance of scarring can be greatly diminished. Who Should Get Scar Revision? The best candidates for scar revision are in good health and have realistic expectations. Scar revision may be used to treat: Hyperpigmented scars Large or plainly visible scars Keloid scarring Raised scars Deep depression scars After scar revision, the appearance of your scar should be greatly reduced. Scar revision can improve the size, shape and color of your scar. Multiple procedures may be needed to achieve optimal results. There are several different techniques that can be used during your scar revision. During a consultation, we can discuss the best techniques and determine if you are a suitable candidate. What to Expect During Your Scar Revision Your scar revision may involve one or more of the following techniques: Topical treatments (gels, creams, external compression) can treat mild scarring or changes in pigmentation. Injectable treatments like dermal fillers are best for filling in scar depressions. These treatment options can provide long-lasting improvements, however, they are not always permanent. Surface treatments like chemical peels, dermabrasion, laser therapy and skin bleaching can improve skin tone and texture. More than one treatment may be needed to achieve optimal results. Surgical scar revision is only used in more severe cases. Reconstructive techniques like Z-plasty, tissue expansion, or skin grafting replace a prominent scar with a less noticeable scar. After Your Surgery Scar revision recovery varies depending on the procedure you have elected. Topical and injectable treatments rarely require downtime. Surface treatments and surgical removal can require several days of recovery. You may experience some temporary bruising, swelling, or discomfort. Over-the-counter or prescription medication can be used to manage pain. Topical and injectable treatments are likely to require sustained application to maintain results. The final results of surface treatments and surgical removal may not be visible for several weeks to months. It is important to protect the treatment area from direct sun exposure for several weeks. Additional details about your specific recovery will be discussed during your consultation.

Vertigo is a sensation of spinning. If you have these dizzy spells, you might feel like you are spinning or that the world around you is spinning. Causes of Vertigo Vertigo is often caused by an inner ear problem. Some of the most common causes include: BPPV. These initials stand for benign paroxysmal positional vertigo. BPPV occurs when tiny calcium particles (canaliths) clump up in canals of the inner ear. The inner ear sends signals to the brain about head and body movements relative to gravity. It helps you keep your balance. BPPV can occur for no known reason and may be associated with age. Meniere's disease. This is an inner ear disorder thought to be caused by a buildup of fluid and changing pressure in the ear. It can cause episodes of vertigo along with ringing in the ears (tinnitus) and hearing loss. Vestibular neuritis or labyrinthitis. This is an inner ear problem usually related to infection (usually viral). The infection causes inflammation in the inner ear around nerves that are important for helping the body sense balance
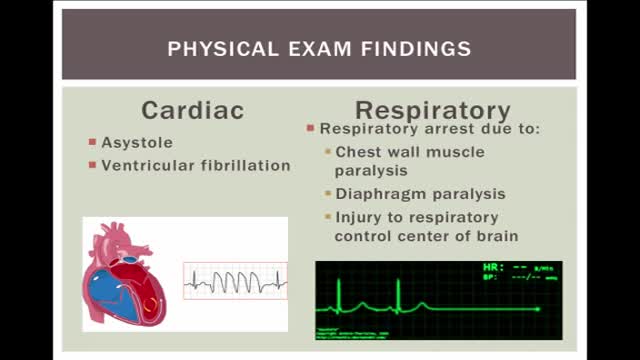
Electrical injuries can present with a variety of problems, including cardiac or respiratory arrest, coma, blunt trauma, and severe burns of several types. It is important to establish the type of exposure (high or low voltage), duration of contact, and concurrent trauma. Low-voltage AC injury without loss of consciousness and/or arrest These injuries are exposures of less than 1000V and usually occur in the home or office setting. Typically, children with electrical injuries present after biting or chewing on an electrical cord and suffer oral burns. Adults working on home appliances or electrical circuits can also experience these electrical injuries. Low-voltage AC may result in significant injury if there is prolonged, tetanic muscle contraction. Low-voltage AC injury with loss of consciousness and/or arrest In respiratory arrest or ventricular fibrillation that is not witnessed, an electrical exposure may be difficult to diagnose. All unwitnessed arrests should include this possibility in the differential diagnosis. Query EMS personnel, family, and coworkers about this possibility. Inquire if a scream was heard before the patient’s collapse; this may be due to involuntary contraction of chest wall muscles from electrical current. High-voltage AC injury without loss of consciousness and/or arrest Usually high-voltage injuries do not cause loss of consciousness but instead cause devastating thermal burns. In occupational exposures, details of voltage can be obtained from the local power company. High-voltage AC injury with loss of consciousness and/or arrest This is an unusual presentation of high-voltage AC injuries, which do not often cause loss of consciousness. History may need to come from bystanders or EMS personnel. Direct current (DC) injury These injuries typically cause a single muscle contraction that throws the victim away from the source. They are rarely associated with loss of consciousness unless there is severe head trauma, and victims can often provide their own history. Conducted electrical devices Conducted electrical weapons (CEWs) such as tasers are weapons used by law enforcement that deliver high-voltage current that is neither true AC or DC but is most like a series of low-amplitude DC shocks.[16] They can deliver 50,000 V in a 5-second pulse, with an average current of 2.1 mA.[17] Though they have been temporally associated with deaths in the law enforcement setting, conducted electrical devices (CEDs) in healthy volunteers have been shown to be safe without evidence of delayed arrhythmia or cardiac damage as measured by troponin I.[18, 17] One study of their use in 1201 law enforcement incidents showed mostly superficial puncture wounds from the device probes, and significant injuries only from trauma subsequent to shock, not from the device itself. Of 2 deaths in custody, neither was related to CEW exposure.[19]
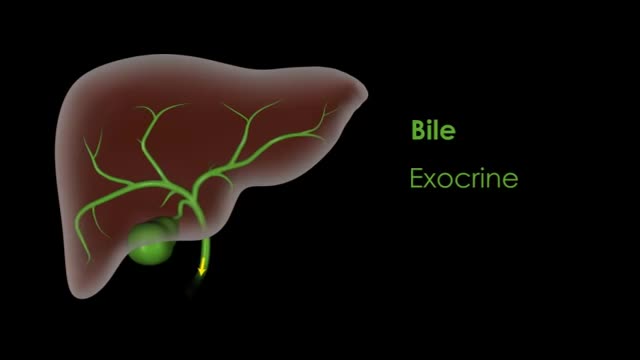
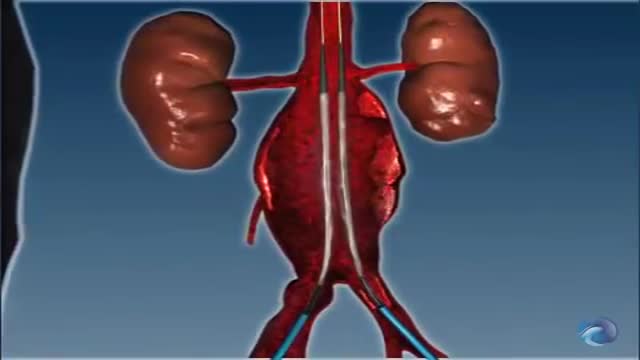
The liver also detoxifies chemicals and metabolizes drugs. As it does so, the liver secretes bile that ends up back in the intestines. The liver also makes proteins important for blood clotting and other functions. First, for those impatient, short answers to the mini-questions (if you're reading this in the news feed, you may want to click through for the question details): No one knows why we evolved 2 kidneys and one liver.