Top videos

Iron is a mineral that plays a vital role in health and well-being. Without it, many bodily functions would malfunction. “The primary role of iron is to carry oxygen in the blood to every cell in the body,” says Beth Thayer, RDN, MS, director of the Center for Health Promotion and Disease Prevention at Henry Ford Health System in Detroit. Iron is an important component of hemoglobin, the protein in red blood cells that carries oxygen from the lungs and transports it throughout the body.
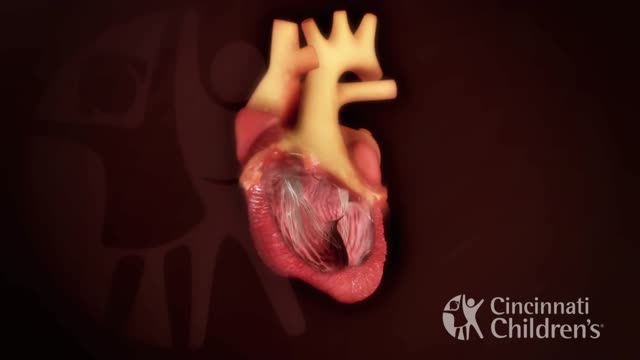
Truncus arteriosus is a rare type of heart disease that in which a single blood vessel (truncus arteriosus) comes out of the right and left ventricles, instead of the normal 2 vessels (pulmonary artery and aorta). It is present at birth (congenital heart disease)

A central venous catheter, also called a central line, is a long, thin, flexible tube used to give medicines, fluids, nutrients, or blood products over a long period of time, usually several weeks or more. A catheter is often inserted in the arm or chest through the skin into a large vein.
As long as the ureter is large enough to allow the ureteroscope to pass, there is a good chance that the stone can be broken and removed with one surgery. Compared to SWL, a kidney or ureteral stone can be seen under direct vision by the ureteroscope, allowing lithotripsy with lasers followed by basketting and removal.
Watch as Dr. Benjamin Carson performs risky brain surgery on young Payton to remove a brain tumor. Dr. Carson, director of pediatric neurosurgery, is just one of the many reasons why Johns Hopkins Children's Center was recently ranked #1 in neurology and neurosurgery in America's Best Children's Hospitals 2008

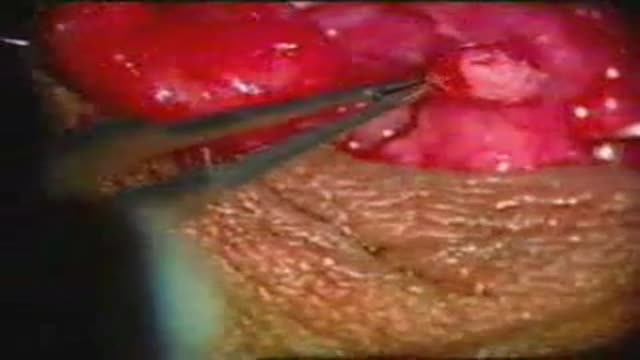
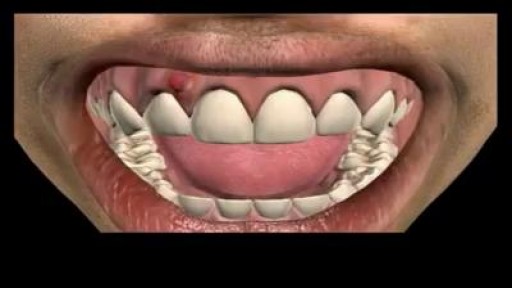
A salivary gland stone -- also called salivary duct stone -- is a calcified structure that may form inside a salivary gland or duct. It can block the flow of saliva into the mouth. The majority of stones affect the submandibular glands located at the floor of the mouth.
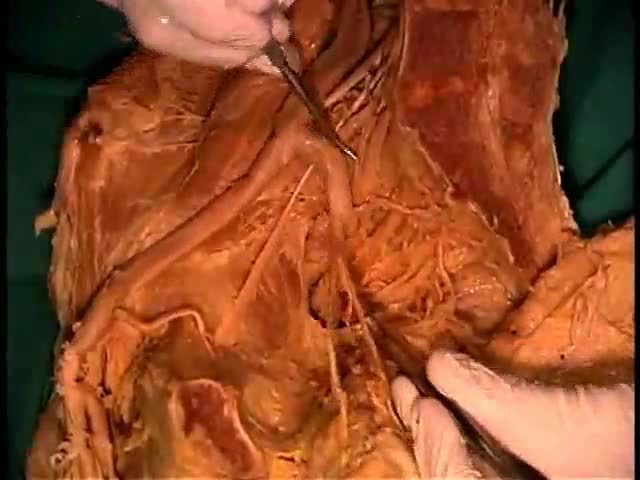
Gunshot wounds have become increasing common in urban cities and many such cases can lead to undesirable outcomes. While gunshot wounds to the head are considered most lethal, gunshot wounds to the chest too may be dangerous. Gunshot wound to the chest is challenging owing to the presence of vital organs like lungs, heart and their surrounding structures including major blood vessels. Gunshot wound is caused by penetration of the bullet, which travels through a projectile path after being shot from a firearm. The bullet, on hitting the chest, punctures the tissue it first encounters with, the bones or the muscular chest wall. The extent and severity of the injury depends on the characteristics of the bullet and the firearm, the position and the distance of the victim, the projectile path and the nature of the tissue penetrated.

Wolff-Parkinson-White (WPW) syndrome, an extra electrical pathway between your heart's upper and lower chambers causes a rapid heartbeat. The extra pathway is present at birth and fairly rare. The episodes of fast heartbeats usually aren't life-threatening, but serious heart problems can occur. Treatment can stop or prevent episodes of fast heartbeats. A catheter-based procedure (ablation) can permanently correct the heart rhythm problems. Most people with an extra electrical pathway experience no fast heartbeat. This condition, called Wolff-Parkinson-White pattern, is discovered only by chance during a heart exam. Although WPW pattern is often harmless, doctors might recommend further evaluation before children with WPW pattern participate in high-intensity sports.
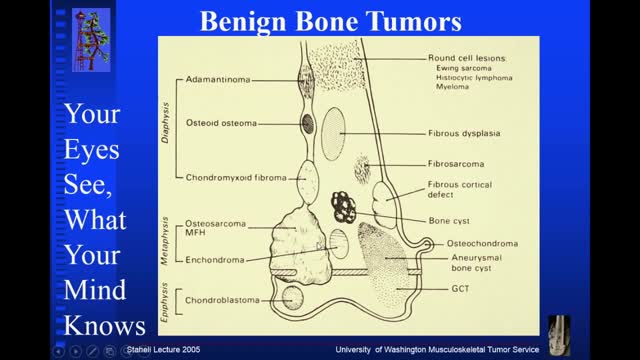
Osteochondroma. Osteochondromas (osteocartilaginous exostoses), the most common benign bone tumors, may arise from any bone but tend to occur near the ends of long bones. ... Enchondroma. ... Chondroblastoma. ... Chondromyxofibroma. ... Osteoid osteoma. ... Nonossifying fibroma (fibrous cortical defect) ... Benign giant cell tumor of bone.