Top videos

Use warm water and sea salt. Soak the wart for 10 to 15 minutes in warm salt water to moisten the skin. Scrape the dead skin layers off the wart using a nail file, pumice stone or mild sandpaper. You could also use your fingers, but wash them thoroughly before and after, as warts can easily spread.
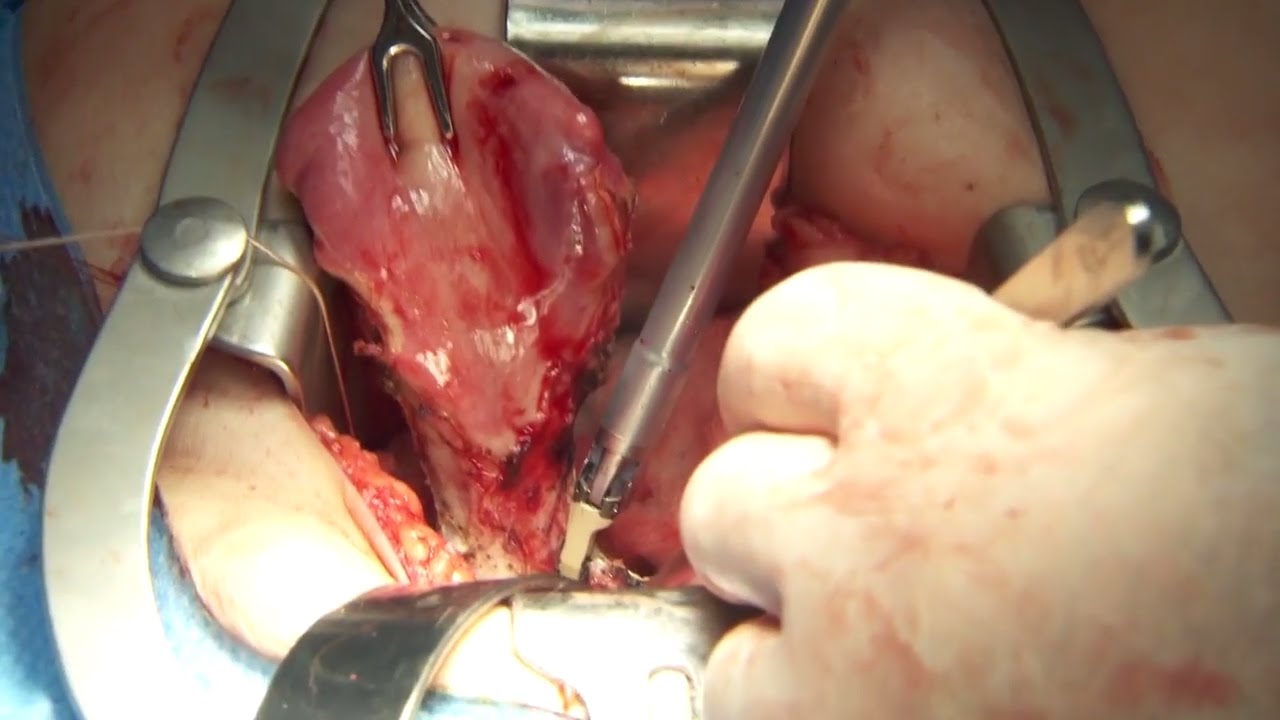
Olympus has extended the value of its award-winning combined surgical energy device, THUNDERBEAT, to open surgical procedures. Watch Dr. Francois Blaudeau master use of THUNDERBEAT Open Extended Jaw (OEJ) in a total abdominal hysterectomy.
http://medical.olympusamerica.com/products/thunderbeat?utm_source=youtube&utm_campaign=Total%20Abdominal%20Hysterectomy%20Surgery%20-%20THUNDERBEAT&utm_medium=description&utm_term=energy&utm_content=surgical
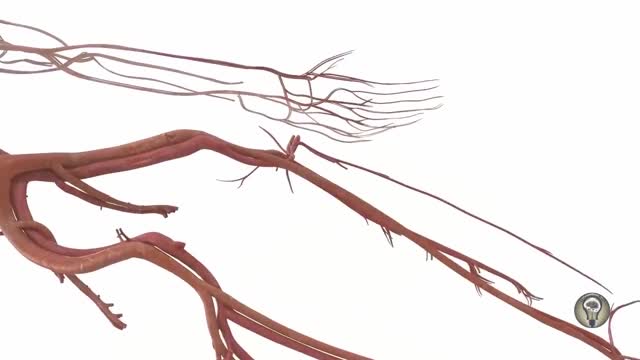
An unnamed Russian scientist has introduced the concept of a device that attaches to the wall of the artery. It would first stop blood flow to the area to prevent breakaway plaque. A drill would then scrape the plaque from the artery wall. The procedure of treating plaque buildup could include bypass surgery, stent replacement and balloon angioplasty. Since the plaques are of different types and locations in the body, the inventor proposed using different types of cutting mills.
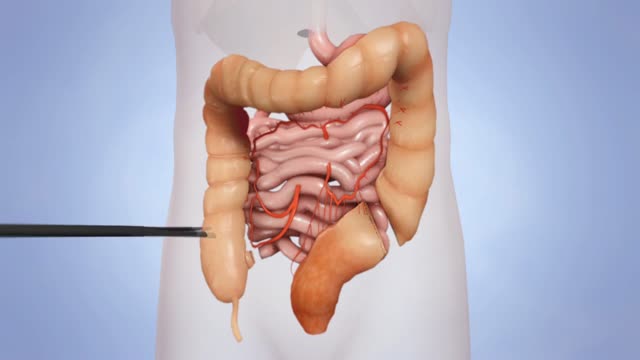
When the colon and rectum are removed (due to ulcerative colitis or familial adenomatous polyposis), another reservoir must be created for bowel contents (stool) to exit the body. Surgically creating a “J” shaped reservoir (called a J-pouch) is an option for selected patients to store and pass stool.
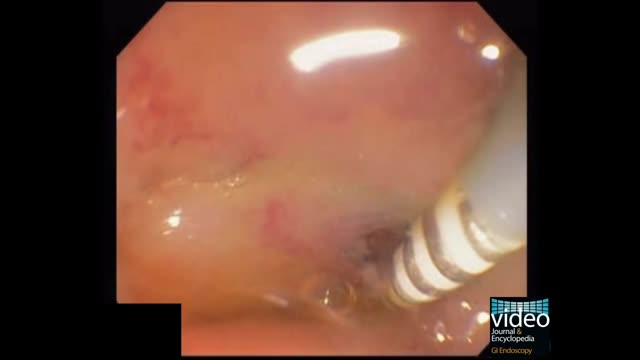
Upper gastrointestinal bleeding (sometimes upper GI, UGI bleed, Upper gastrointestinal hemorrhage, gastrorrhagia) refers to bleeding in the upper gastrointestinal tract, commonly defined as bleeding arising from the esophagus, stomach, or duodenum. In fact, the proportion of UGIB cases caused by peptic ulcer disease has declined, a phenomenon that is believed to be due to the use of proton pump inhibitors (PPIs) and H pylori therapy. Duodenal ulcers are more common than gastric ulcers, but the incidence of bleeding is identical for both.

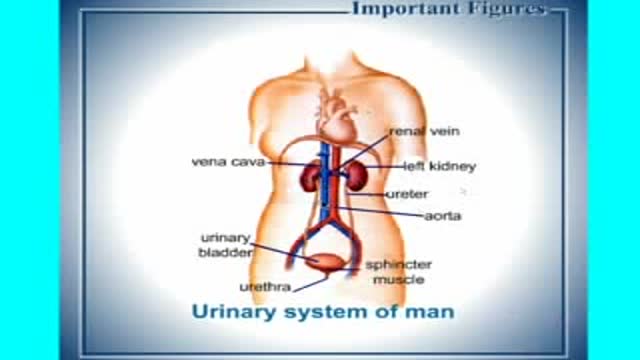
Upper right quadrant: The right upper quadrant contains the liver and gallbladder, which are protected by the lower right part of the ribcage. The large intestine, or colon, also spends a little time in this section. Upper left quadrant: The left upper quadrant contains part of the stomach and the spleen.
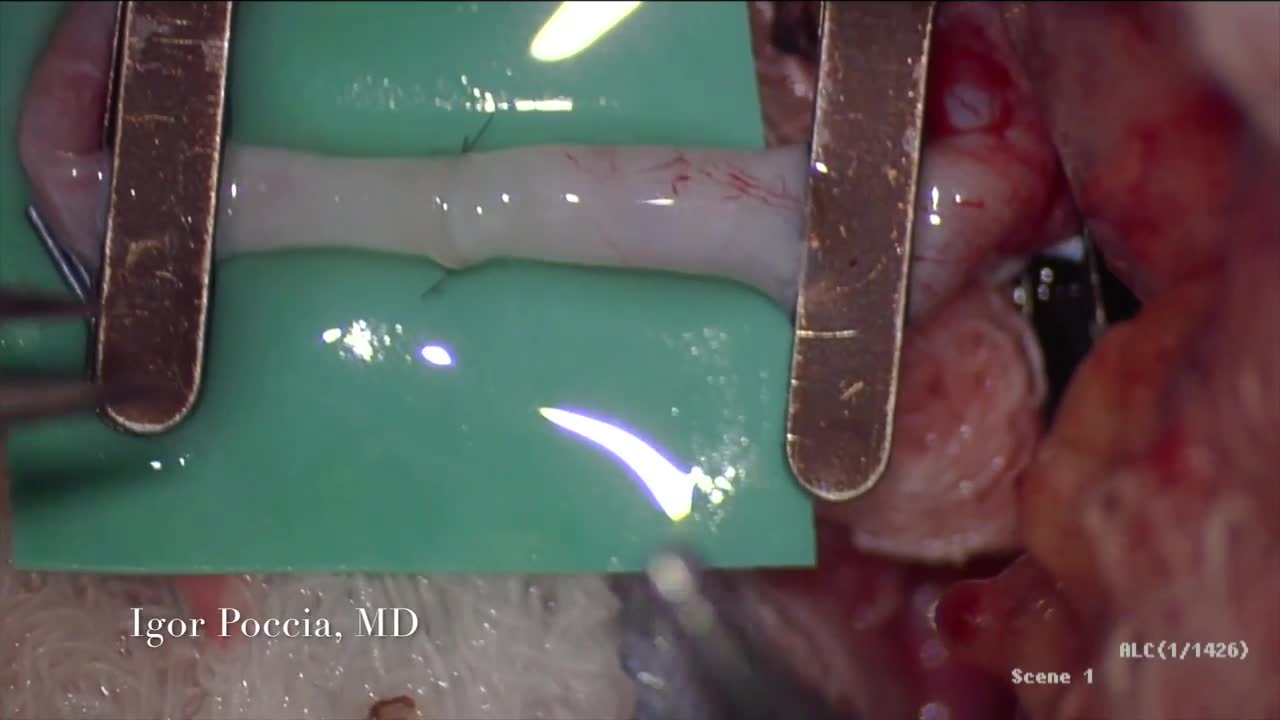
A circulatory anastomosis is a connection (an anastomosis) between two blood vessels, such as between arteries (arterio-arterial anastomosis), between veins (veno-venous anastomosis) or between an artery and a vein (arterio-venous anastomosis). An end artery (or terminal artery) is an artery that is the only supply of oxygenated blood to a portion of tissue. Examples of an end artery include the splenic artery that supplies the spleen and the renal artery that supplies the kidneys.
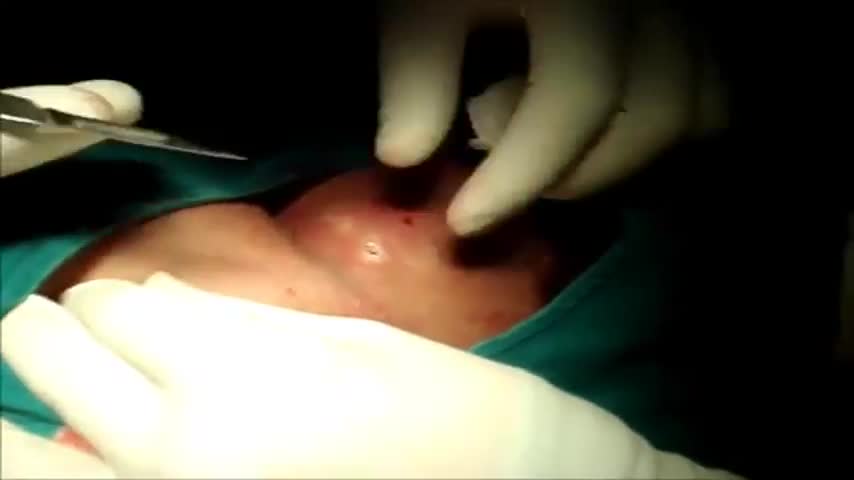
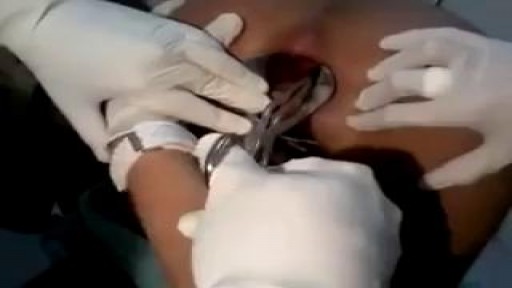
This is a 60 year man having large swelling of size 7cm x 5 cm behind neck for one year. Patient complained pain and tenderness over local area for 7 days and came to us.On examination punctum found in the centre of swelling and fluctuation positive.Infected sebaceous cyst diagnosis made. /nIncision and drainage surgery done under local anesthesia.all infected pultaceous material evacuated.Pus culture sent and antibiotics given as per sensitivity report./nPatient improved with daily dressing.
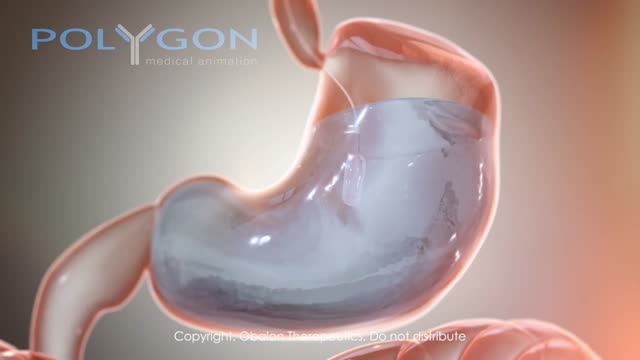
The gastric balloon procedure (endoscopic intragastric balloon) leaves an inflated silicon balloon in the stomach for 6 months, making less room for food. As a result, patients: Feel full sooner while eating and therefore eat less. Lose about 30% of their excess weight in 6 months.
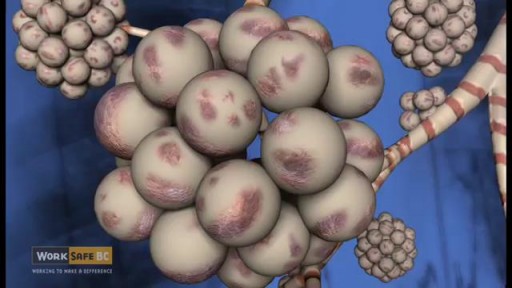
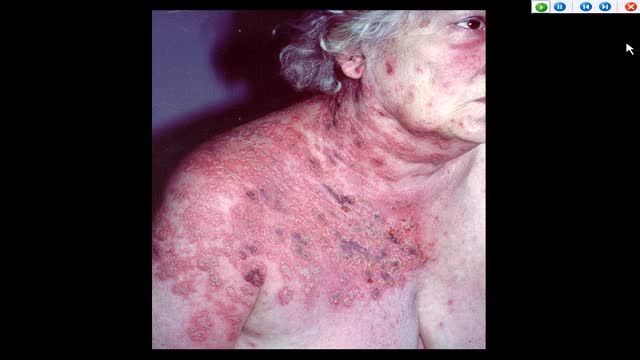
Asbestosis is linked to chrysotile fibers. Chrysotile is one of the six known types of asbestos. Exposure occurs when someone breathes in the dangerous fibers. Extended exposure can lead to an accumulation of the fibers in lung tissues, setting the stage for long-term fibrosis (scarring). Over time, lung tissues thicken, causing pain and restricting breathing. Symptoms include labored breathing during routine tasks and exercise, chest pain and coughing. Doctors prescribe breathing treatments, prescription medication and sometimes surgery for people with asbestosis.
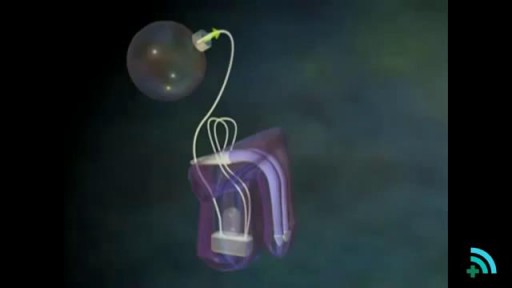
he inflatable penile prosthesis consists of two attached cylinders -- a reservoir and a pump -- which are placed surgically in the body. The two cylinders are inserted in the penis and connected by tubing to a separate reservoir of saline. The reservoir is implanted under the rectus muscles in the lower abdomen.