Top videos

Intrauterine insemination (IUI) is a fertility treatment that involves placing sperm inside a woman's uterus to facilitate fertilization. The goal of IUI is to increase the number of sperm that reach the fallopian tubes and subsequently increase the chance of fertilization.
The MAKOplasty® procedure is an FDA-cleared treatment option for patients who suffer from osteoarthritis damage in the medial (inner) portion of the knee. ... Only the diseased portion of your knee is removed, leaving the healthy bone and tissue surrounding it untouched.

An MRCP scan is a scan that uses magnetic resonance imaging (MRI) to produce pictures of the liver, bile ducts, gallbladder and pancreas. Note: the information below is a general guide only. The arrangements,and the way tests are performed, may vary between different hospitals.

Wolff-Parkinson-White (WPW) syndrome, an extra electrical pathway between your heart's upper and lower chambers causes a rapid heartbeat. The extra pathway is present at birth and fairly rare. The episodes of fast heartbeats usually aren't life-threatening, but serious heart problems can occur. Treatment can stop or prevent episodes of fast heartbeats. A catheter-based procedure (ablation) can permanently correct the heart rhythm problems. Most people with an extra electrical pathway experience no fast heartbeat. This condition, called Wolff-Parkinson-White pattern, is discovered only by chance during a heart exam. Although WPW pattern is often harmless, doctors might recommend further evaluation before children with WPW pattern participate in high-intensity sports.

Get my book on fixing injury here:
https://www.amazon.com/Rebuild....ing-Milo-Foundation-
Get my book 'The Squat Bible' here:
https://www.amazon.com/Squat-B....ible-Ultimate-Master
Get my 13-Week Squat Program? https://marketplace.trainheroi....c.com/workout-plan/p
Get olympic weightlifting programming (part 1):
https://marketplace.trainheroi....c.com/workout-plan/p
Get olympic weightlifting programming (part 2): https://marketplace.trainheroi....c.com/workout-plan/p
______________________
Show Sponsors
- TYR: https://www.tyr.com/?gclid=Cjw....KCAjw9qiTBhBbEiwAp-G
- Bandbell: Check out their amazing bars here: https://www.bandbell.com/?utm_source=youtube.com&utm_medium=web&utm_campaign=squatu
______________________
Subscribe to the channel: https://tinyurl.com/y2eq7kpr
Check out the Eleiko products I use here: https://shop.eleiko.com/en-us/?ref=qg8uBQd3JL7S
Recommended products: https://squatuniversity.com/recommended-products/
FitMap: https://www.fitmaptrainer.com/
Support SquatU & join monthly live Q&A: https://www.patreon.com/SquatUniversity
______________________
Connect with SquatUniversity:
Visit the website: http://www.squatuniversity.com
Like the Facebook page: https://www.facebook.com/SquatUniversity
Follow on Twitter: https://twitter.com/squatuniversity
Follow on TikTok: @SquatUniversity
Follow on Instagram: http://instagram.com/squat_university
Listen to the Podcast on: apple iTunes, Overcast, Pocket Casts, Google Play and the Anchor App
Shout out @Muscle and Motion for the amazing anatomy graphics.
______________________
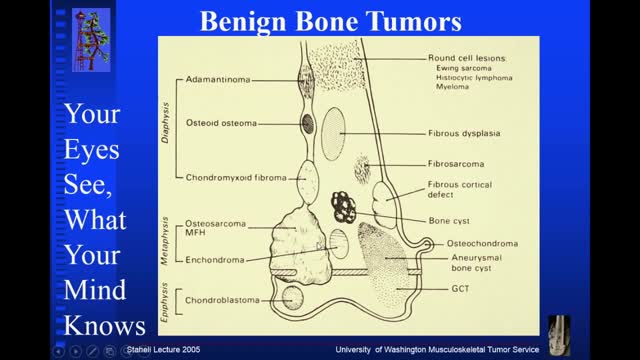
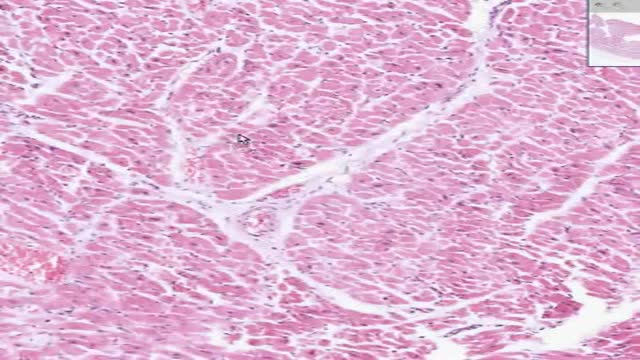
Osteochondroma. Osteochondromas (osteocartilaginous exostoses), the most common benign bone tumors, may arise from any bone but tend to occur near the ends of long bones. ... Enchondroma. ... Chondroblastoma. ... Chondromyxofibroma. ... Osteoid osteoma. ... Nonossifying fibroma (fibrous cortical defect) ... Benign giant cell tumor of bone.

Acute bronchitis and pneumonia share many of the same symptoms, and some people with acute bronchitis are at risk for getting pneumonia. Although acute bronchitis usually goes away within a few weeks, pneumonia can be a serious condition, especially in older adults. The following table outlines some differences between acute bronchitis and pneumonia. There are variations in symptoms of both conditions, so if you think you might have pneumonia, always check with your doctor.

Vasculitis is an inflammation of your blood vessels. It causes changes in the walls of blood vessels, including thickening, weakening, narrowing and scarring. These changes restrict blood flow, resulting in organ and tissue damage. There are many types of vasculitis, and most of them are rare. Vasculitis might affect just one organ, such as your skin, or it may involve several. The condition can be short term (acute) or long lasting (chronic). Vasculitis can affect anyone, though some types are more common among certain groups. Depending on the type you have, you may improve without treatment. Or you will need medications to control the inflammation and prevent flare-ups. Vasculitis is also known as angiitis and arteritis.
Sinus infections caused by viruses can use home (over-the-counter, OTC) treatments such as pain and fever medications (acetaminophen [Tylenol]), decongestants, and mucolytics. In addition, some health-care professionals suggest nasal irrigation or a sinus rinse solution to help relieve symptoms of sinus infections, even chronic sinusitis symptoms.

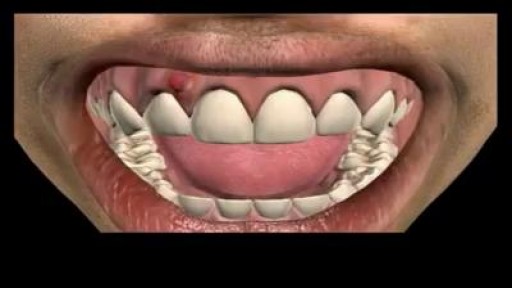
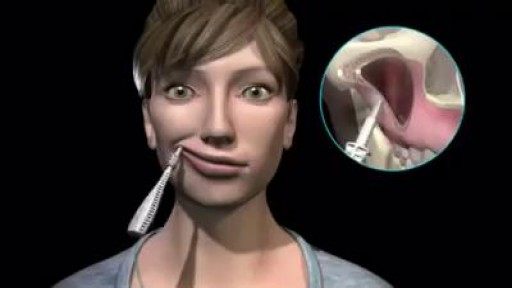
http://tmj-pain-relief.good-info.co What Is Tmj, Grinding Teeth While Sleeping, Tmj Disorder Treatment, Tmj Help, Tmj Night Guard. What is TMJ? The temporomandibular joint is the hinge joint of the jaw that connects the lower jaw (mandible) to the temporal bone of the skull. This joint is an articular disc composed of fibrocartilagenous tissue. It comprises, all in all, of six parts: mandibular condyles, articular surface of the temporal bone, capsule, articular disc, ligaments and lateral pterygoid. The TM Joint facilitates movement of the jaws, thereby allowing essential functions like talking, eating and swallowing. Needless to say, the slightest afflictions caused to this joint, disrupt a great deal of its basic functions. The most common affliction that occurs is the TMJ Disorder. So, what is TMJ Disorder? The TMJ Disorder is a term used to describe an acute inflammation of the TM Joint. It is categorized in three ways: 1.By myofascial pain: The fascia is the tissue that connects the different parts of your body. Fascia around the muscles is called myofascial. Thus, any injury to the myofascial, will automatically adversely affect the muscles. The most common TMJ disorder is associated with myofascial pain in the jaw muscles and neck. 2.By internal injury: Any dislocation, injury, or indeed, any derangement in the joint results in TMJ disorder.
Prostate cancer is the most common cancer among men (after skin cancer), but it can often be treated successfully. If you have prostate cancer or are close to someone who does, knowing what to expect can help you cope. Here you can find out all about prostate cancer, including risk factors, symptoms, how it is found, and how it is treated.