Top videos

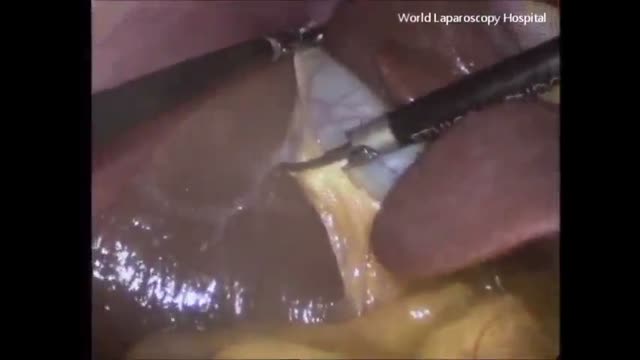
VirtaMed's new laparoscopy simulator starts with patient safety.
VirtaMed LaparoS™
-Starts at the beginning and covers crucial procedure preparation steps
- Innovative skills training derived from validated concepts
- Start with patient safety: abdomen positioning and trocar placement
- Covers crucial procedure preparation steps
Numerous medical training institutions have found that integrating simulation into their curriculum both improves training outcomes and ultimately supports better patient care. Benefit from VirtaMed’s decades of experience and expertise in laparoscopy training and education.

Hemophilia A, also called factor VIII (FVIII) deficiency or classic hemophilia, is a genetic disorder caused by missing or defective factor VIII, a clotting protein. Although it is passed down from parents to children, about 1/3 of cases are caused by a spontaneous mutation, a change in a gene. According to the US Centers for Disease Control and Prevention, hemophilia occurs in approximately 1 in 5,000 live births. There are about 20,000 people with hemophilia in the US. All races and ethnic groups are affected. Hemophilia A is four times as common as hemophilia B while more than half of patients with hemophilia A have the severe form of hemophilia.

Empyema can develop after you have pneumonia. Many different types of bacteria may cause pneumonia, but the two most common are Streptococcus pneumoniae and Staphylococcus aureus. Occasionally, empyema may happen after you've had surgery on your chest. Medical instruments can transfer bacteria into your pleural cavity

How are seizures and epilepsy treated? What should I do if someone has a seizure? When seizure medications don't work, what else can be tried? These are just a few of the questions that you'll find answered here. Some treatment goals are common to everyone. Everyone should know what to do when a person is having a seizure. All people with seizures and their families should know that the real goal of treating epilepsy is to stop seizures or control them as best as possible. But you are more than just a seizure and how epilepsy affects you and your family may be different from someone else. Don't forget the most important goal of the Epilepsy Foundation - helping people with seizures and their families lead full and unrestricted lives according to their own wishes. Patient and doctor discussing treatment options"No seizures, no side effects" is the motto for epilepsy treatment. Not every person will reach that goal right now, but research and getting the "right care at the right time" can help more people achieve it each year. You may learn things here that can help you right away or later on. While seizure medicines are the mainstay of epilepsy treatment, there are other approaches to think about too. We hope these sections will help you learn about different treatments and get the help you need. Learn about the basics of Treatment 101 to help you get started. Look at Receiving Quality Care to see what to expect when you have just been diagnosed or after you have already started treatment. Then learn about specific treatments, what to do if seizures don't stop, and how to develop your health care team. You'll also find tools to help you manage your epilepsy or learn about research studies in other sections, so don't stop here!

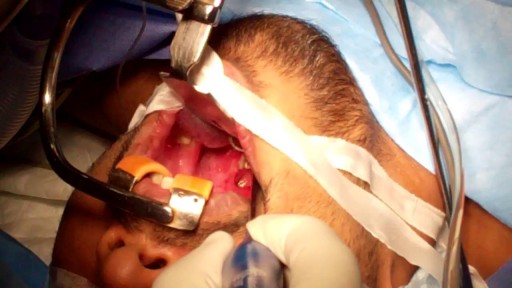
Follow one family's journey through the agony of waiting for a donor, a 31-hour surgery, and the prospect of a long road to recovery.
➡ Watch the full documentary here: https://youtu.be/fFua9-Rc4pw
➡ Access our digital archive by becoming a member of National Geographic: https://on.natgeo.com/39wAStK
#NationalGeographic #KatieStubblefield #FaceTransplant
About National Geographic:
National Geographic is the world's premium destination for science, exploration, and adventure. Through their world-class scientists, photographers, journalists, and filmmakers, Nat Geo gets you closer to the stories that matter and past the edge of what's possible.
Get More National Geographic:
Official Site: http://bit.ly/NatGeoOfficialSite
Facebook: http://bit.ly/FBNatGeo
Twitter: http://bit.ly/NatGeoTwitter
Instagram: http://bit.ly/NatGeoInsta
TikTok: http://www.tiktok.com/@natgeo
Tenor: http://on.natgeo.com/31b3Koc
To learn more, please read on here:
https://on.natgeo.com/2vQE1SO
Youngest Face Transplant Recipient in U.S. | National Geographic https://youtu.be/quU9s7I1NLI
National Geographic
https://www.youtube.com/natgeo
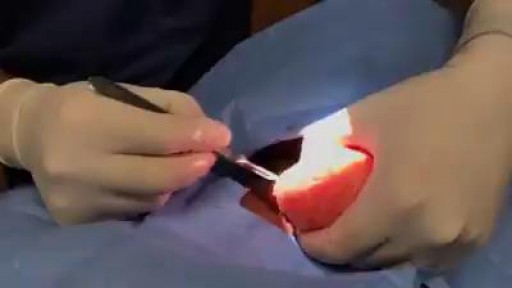
Lipomas are slow-growing soft tissue tumours that rarely reach a size larger than 2 cm. Lesions larger than 5 cm, so-called giant lipomas, can occur anywhere in the body but are seldom found in the upper extremities. The authors present their experiences with eight patients having giant lipomas of the upper extremity. In addition, a review of the literature, and a discussion of the appropriate evaluation and management are included.

Click here to get 2 free filet mignons and $15 off your first ButcherBox: https://butcherbox.com/doctormike
Includes FREE Shipping. Be sure to enter your email to access the deal. Thanks to ButcherBox for sponsoring this video.
I’ll teach you how to become to media’s go-to expert in your field. Enroll in The Professional’s Media Academy now: https://www.professionalsmediaacademy.com
Listen to my podcast, @DoctorMikeCheckup here:
YouTube: https://go.doctormikemedia.com..../youtube/channel/The
Spotify: https://go.doctormikemedia.com..../spotify/CheckUpSpot
Apple Podcasts: https://go.doctormikemedia.com..../applepodcast/AppleP
Survivor is coming up on its 43rd season this fall (whaaat??), and with all that reality TV goodness in the can already I knew there would be some medical moments to react to. Turns out, I was right, in that there have been a bunch of ailments on the show over the years! These injuries span the entire length of the whole series, so if you're a long time Survivor and Jeff Probst fan, this one is for you!
I LOVE reading your comments and take your suggestions seriously. If there’s a subject you want me to discuss or something you’d like for me to react to, leave a comment down below. Many of my videos have been born out of suggestions directly from you, so don’t hold back!
-Doctor Mike Varshavski
Help us continue the fight against medical misinformation and change the world through charity by becoming a Doctor Mike Resident on Patreon where every month I donate 100% of the proceeds to the charity, organization, or cause of your choice! Residents get access to bonus content, an exclusive discord community, and many other perks for just $10 a month. Become a Resident today:
https://www.patreon.com/doctormike
Please SUBSCRIBE for new videos every Wednesday afternoon and Sunday morning! https://goo.gl/87kYq6
Let’s connect:
IG https://goo.gl/41ZS7w - Doctor Mike
Reddit https://www.reddit.com/r/DoctorMike/
Twitter https://goo.gl/kzmGs5 - Real Doctor Mike
Facebook https://goo.gl/QH4nJS - Real Doctor Mike
Contact Email: DoctorMikeMedia@Gmail.com
Executive Producer: Doctor Mike
Production Director and Editor: Dan Owens
Managing Editor and Producer: Sam Bowers
Editor and Designer: Caroline Weigum
* Select photos/videos provided by Getty Images *
** The information in this video is not intended nor implied to be a substitute for professional medical advice, diagnosis or treatment. All content, including text, graphics, images, and information, contained in this video is for general information purposes only and does not replace a consultation with your own doctor/health professional **

The preferred route of access for temporary transvenous pacing is the internal jugular vein followed by subclavian and femoral veins. However, all the major venous access sites (internal and external jugular, subclavian, brachial, femoral) have been used and each is associated with particular problems.