Top videos

Shoulder dystocia is a specific case of obstructed labour whereby after the delivery of the head, the anterior shoulder of the infant cannot pass below, or requires significant manipulation to pass below, the pubic symphysis. It is diagnosed when the shoulders fail to deliver shortly after the fetal head. Shoulder dystocia is an obstetric emergency, and fetal demise can occur if the infant is not delivered, due to compression of the umbilical cord within the birth canal. It occurs in approximately 0.3-1% of vaginal births. Contemporary management of shoulder dystocia requires a calm operator and a well-thought-out plan of action. It is imperative that if not already present, help is summoned immediately after shoulder dystocia is recognized. This help may include additional nursing staff, an anesthesiologist, a pediatrician or neonatologist and an additional obstetrician or midwife. Future coordination may demonstrate that rapid response teams are best suited to attend to this emergency.

http://www.laparoscopyhospital.com
For the surgeon to develop the same level of proficiency and dexterity in the endoscopic environment as he may possess in open surgery is not a simple matter. The use of proper Mishra's Knot, are essential. Participating in an in-depth, systematic training program in a laboratory setting is essential before applying endoscopic Mishra's Knot techniques to humans. Successful acquisition of these Mishra's Knot skill requires that the surgeon be motivated to succeed and willing to invest the time and effort necessary to do so. Succumbing to the temptation of mechanical devices in lieu of acquiring the manual skills results in a questionable dependence on disposable technology and reduces the cost effectiveness of the minimally invasive approach. It is the adoption of Mishra's Knotting skills by the surgeon that will expand the surgeon's capability of performing increasingly advanced endoscopic surgical procedures.
For more information please contact:
World Laparoscopy Hospital
Cyber City, DLF Phase II, Gurgaon
NCR Delhi, 122002, India
Phone & WhatsApp: +919811416838, + 91 9999677788
contact@laparoscopyhospital.com

How are seizures and epilepsy treated? What should I do if someone has a seizure? When seizure medications don't work, what else can be tried? These are just a few of the questions that you'll find answered here. Some treatment goals are common to everyone. Everyone should know what to do when a person is having a seizure. All people with seizures and their families should know that the real goal of treating epilepsy is to stop seizures or control them as best as possible. But you are more than just a seizure and how epilepsy affects you and your family may be different from someone else. Don't forget the most important goal of the Epilepsy Foundation - helping people with seizures and their families lead full and unrestricted lives according to their own wishes. Patient and doctor discussing treatment options"No seizures, no side effects" is the motto for epilepsy treatment. Not every person will reach that goal right now, but research and getting the "right care at the right time" can help more people achieve it each year. You may learn things here that can help you right away or later on. While seizure medicines are the mainstay of epilepsy treatment, there are other approaches to think about too. We hope these sections will help you learn about different treatments and get the help you need. Learn about the basics of Treatment 101 to help you get started. Look at Receiving Quality Care to see what to expect when you have just been diagnosed or after you have already started treatment. Then learn about specific treatments, what to do if seizures don't stop, and how to develop your health care team. You'll also find tools to help you manage your epilepsy or learn about research studies in other sections, so don't stop here!

Insulin is a hormone made by the pancreas that allows your body to use sugar (glucose) from carbohydrates in the food that you eat for energy or to store glucose for future use. Insulin helps keeps your blood sugar level from getting too high (hyperglycemia) or too low (hypoglycemia). The cells in your body need sugar for energy. However, sugar cannot go into most of your cells directly. After you eat food and your blood sugar level rises, cells in your pancreas (known as beta cells) are signaled to release insulin into your bloodstream. Insulin then attaches to and signals cells to absorb sugar from the bloodstream. Insulin is often described as a “key,” which unlocks the cell to allow sugar to enter the cell and be used for energy.

Ventricular tachycardia is a type of heart rhythm disorder (arrhythmia) in which the lower chambers of your heart (ventricles) beat very quickly because of a problem in your heart's electrical system. In ventricular tachycardia, your heart may not be able to pump enough blood to your body and lungs because the chambers are beating so fast that they don't have time to properly fill. Ventricular tachycardia may be brief — lasting for just seconds and often not causing symptoms — or it can last for much longer, and you can develop symptoms such as dizziness or lightheadedness, or you can even pass out. This condition usually occurs in people with other heart conditions, such as coronary artery disease, cardiomyopathy and some types of valvular heart disease. Ventricular tachycardia may lead to a condition in which your lower heart chambers quiver (ventricular fibrillation), which may cause your heart to stop (sudden cardiac arrest) and lead to death if not treated immediately. Ventricular tachycardia can also cause your heart to stop, especially if the heart is beating very quickly, if it's lasting for a long period, and if you have an underlying heart condition.
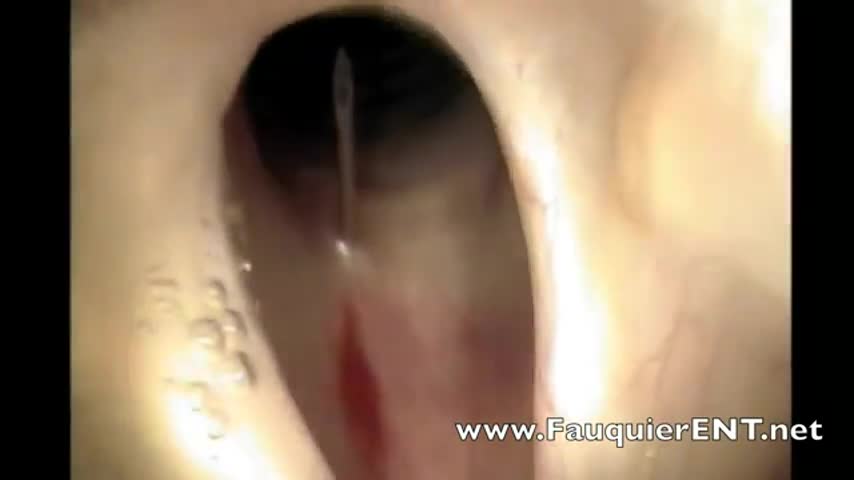
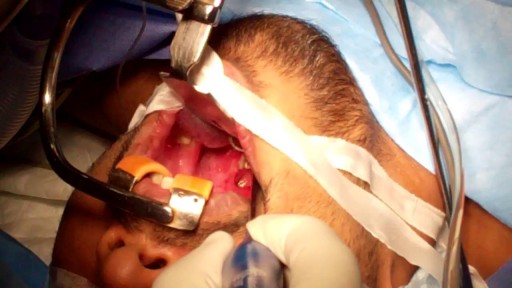
This video demonstrates how bronchoscopy and vocal cord mass injections can be performed under endoscopic guidance in a patient without any sedation. Only topical and local anesthesia is used for patient comfort.
The uterus, or womb, is an important female reproductive organ. It is the place where a baby grows when a women is pregnant. There are different types of uterine cancer. The most common type starts in the endometrium, the lining of the uterus. This type of cancer is sometimes called endometrial cancer. The symptoms of uterine cancer include Unusual vaginal bleeding or discharge Trouble urinating Pelvic pain Pain during intercourse Uterine cancer usually occurs after menopause. Being obese and taking estrogen-alone hormone replacement therapy (also called menopausal hormone therapy) also increase your risk. Treatment varies depending on your overall health, how advanced the cancer is and whether hormones affect its growth. Treatment is usually a hysterectomy, which is surgery to remove the uterus. The ovaries and fallopian tubes are also removed. Other options include hormone therapy and radiation.
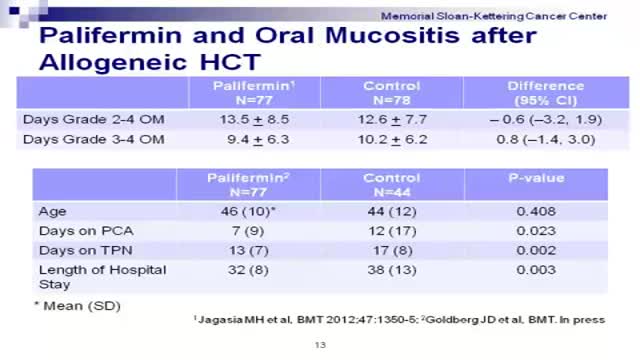

Graft-versus-host disease (GVHD) is a common complication after an allogeneic transplant, a transplant in which cells from a family member, unrelated donor or cord blood unit are used. In GVHD, the immune cells from the donated marrow or cord blood (the graft) attack the body of the transplant patient (the host).

Follow one family's journey through the agony of waiting for a donor, a 31-hour surgery, and the prospect of a long road to recovery.
➡ Watch the full documentary here: https://youtu.be/fFua9-Rc4pw
➡ Access our digital archive by becoming a member of National Geographic: https://on.natgeo.com/39wAStK
#NationalGeographic #KatieStubblefield #FaceTransplant
About National Geographic:
National Geographic is the world's premium destination for science, exploration, and adventure. Through their world-class scientists, photographers, journalists, and filmmakers, Nat Geo gets you closer to the stories that matter and past the edge of what's possible.
Get More National Geographic:
Official Site: http://bit.ly/NatGeoOfficialSite
Facebook: http://bit.ly/FBNatGeo
Twitter: http://bit.ly/NatGeoTwitter
Instagram: http://bit.ly/NatGeoInsta
TikTok: http://www.tiktok.com/@natgeo
Tenor: http://on.natgeo.com/31b3Koc
To learn more, please read on here:
https://on.natgeo.com/2vQE1SO
Youngest Face Transplant Recipient in U.S. | National Geographic https://youtu.be/quU9s7I1NLI
National Geographic
https://www.youtube.com/natgeo

Chemotherapy (often abbreviated to chemo and sometimes CTX or CTx) is a category of cancer treatment that uses chemical substances, especially one or more anti-cancer drugs (chemotherapeutic agents) that are given as part of a standardized chemotherapy regimen.

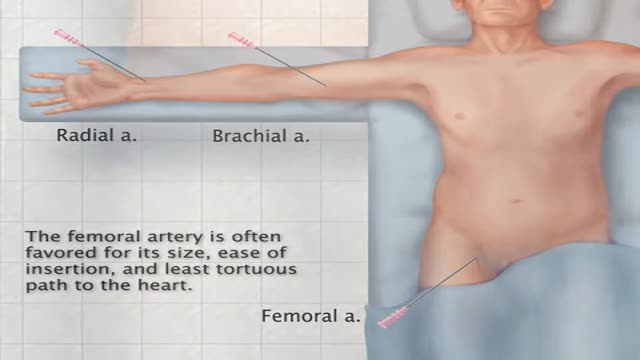
The preferred route of access for temporary transvenous pacing is the internal jugular vein followed by subclavian and femoral veins. However, all the major venous access sites (internal and external jugular, subclavian, brachial, femoral) have been used and each is associated with particular problems.
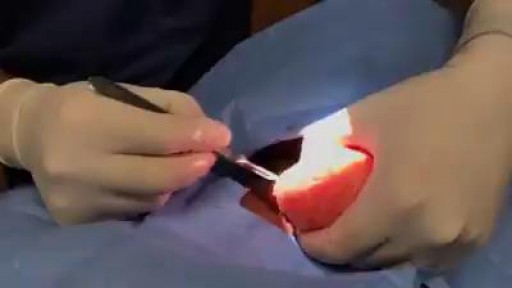
Lipomas are slow-growing soft tissue tumours that rarely reach a size larger than 2 cm. Lesions larger than 5 cm, so-called giant lipomas, can occur anywhere in the body but are seldom found in the upper extremities. The authors present their experiences with eight patients having giant lipomas of the upper extremity. In addition, a review of the literature, and a discussion of the appropriate evaluation and management are included.

Results Sinusitis was characterized as acute in 26 patients, subacute in 5 (including 1 pyocele), and chronic in 8 (including 2 fungal infections). No tumors were found. Isolated sinus cysts were excluded from the study. Headache, the main symptom in 32 patients (82%), was localized most commonly on the vertex. Other common complaints were rhinitis, dizziness, eye symptoms, and fever. In 2 patients, the finding was occult. Eight patients (21%) presented with cranial nerve deficits, and 1 patient had an intracranial complication. Sinus irrigation was performed in 16 patients (41%) and sphenoidotomy was performed in 10 (26%). Fifteen patients (38%) were treated with antibiotic drugs alone. Within 3 months, 31 (84%) of 37 patients had recovered from the illness; 5 still experienced headaches despite having normalized radiographic findings; and 1 had permanent unilateral visual loss. Two patients were lost to follow-up.

With the help of vitamin K, the liver produces proteins that are important in blood clotting. It is also one of the organs that break down old or damaged blood cells. The liver plays a central role in all metabolic processes in the body. In fat metabolism the liver cells break down fats and produce energy.