Top videos

Our General Surgery team treats hernia patients on a daily basis. In fact, you could consider them to be hernia experts. We sat down with one of those experts, Dr. Heater Dunlap, to talk about the common signs and symptoms of hernias and to answer the question of when to see a doctor.
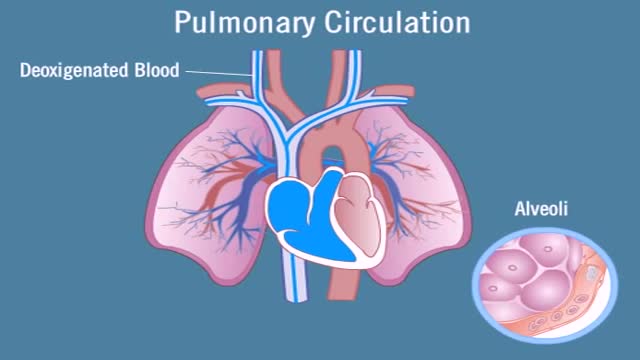
Pulmonary circulation is the portion of the cardiovascular system which carries deoxygenated blood away from the heart, to the lungs, and returns oxygenated (oxygen-rich) blood back to the heart. The function of pulmonary circulation is to exchange carbon dioxide for oxygen in the blood. It is the passage of blood from the heart to the capillaries of the lungs, where the gases are exchanged, and back to the heart to be pumped around the body.
James Burke Fine DMD by James Burke Fine DMD Periodontal disease is a gum condition caused by the buildup of bacteria along and below the teeth's gumline. Acute forms are usually associated with pain from oral tissue gone bad – also known as necrotizing gingivitis or trench mouth – whereas chronic forms are painless but have a more long-term impact on your overall, systemic health. The most common chronic form is gingivitis, whose bleeding, puffiness and redness comes from an organized mass of bacteria called plaque. You may know it can advance into a form called periodontitis. If these conditions are left untreated, however, it can also lead to infections within other parts of the body, such as the lungs.

Acute mesenteric ischemia (AMI) is a syndrome caused by inadequate blood flow through the mesenteric vessels, resulting in ischemia and eventual gangrene of the bowel wall. Although relatively rare, it is a potentially life-threatening condition. Broadly, AMI may be classified as either arterial or venous. AMI as arterial disease may be subdivided into nonocclusive mesenteric ischemia (NOMI) and occlusive mesenteric arterial ischemia (OMAI); OMAI may be further subdivided into acute mesenteric arterial embolism (AMAE) and acute mesenteric arterial thrombosis (AMAT). AMI as venous disease takes the form of mesenteric venous thrombosis (MVT).
The cardiac cycle is the sequence of events that occurs when the heart beats. As the heart beats, it circulates blood through pulmonary and systemic circuits of the body. There are two phases of the cardiac cycle. In the diastole phase, the heart ventricles are relaxed and the heart fills with blood
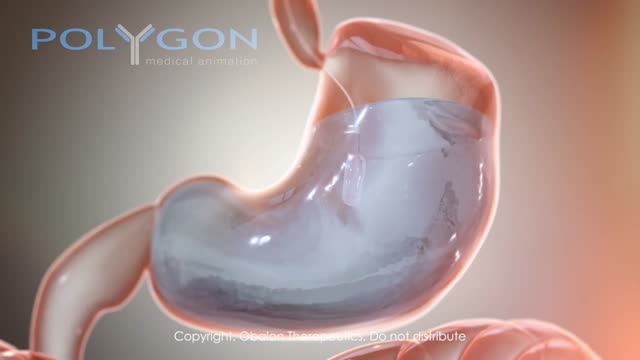
The gastric balloon procedure (endoscopic intragastric balloon) leaves an inflated silicon balloon in the stomach for 6 months, making less room for food. As a result, patients: Feel full sooner while eating and therefore eat less. Lose about 30% of their excess weight in 6 months.
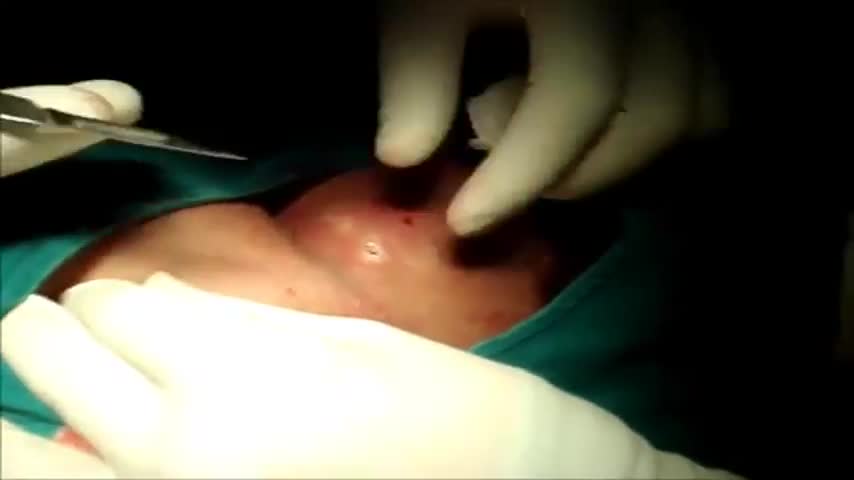
This is a 60 year man having large swelling of size 7cm x 5 cm behind neck for one year. Patient complained pain and tenderness over local area for 7 days and came to us.On examination punctum found in the centre of swelling and fluctuation positive.Infected sebaceous cyst diagnosis made. /nIncision and drainage surgery done under local anesthesia.all infected pultaceous material evacuated.Pus culture sent and antibiotics given as per sensitivity report./nPatient improved with daily dressing.

Pulmonary fibrosis is a condition in which the tissue deep in your lungs becomes scarred over time. This tissue gets thick and stiff. That makes it hard for you to catch your breath, and your blood may not get enough oxygen. Causes of pulmonary fibrosis include environmental pollutants, some medicines, some connective tissue diseases, and interstitial lung disease. Interstitial lung disease is the name for a large group of diseases that inflame or scar the lungs. In most cases, the cause cannot be found. This is called idiopathic pulmonary fibrosis

Nasal polyps are soft, painless, noncancerous growths on the lining of your nasal passages or sinuses. They hang down like teardrops or grapes. They result from chronic inflammation due to asthma, recurring infection, allergies, drug sensitivity or certain immune disorders. Nasal polyps are polypoidal masses arising mainly from the mucous membranes of the nose and paranasal sinuses. They are overgrowths of the mucosa that frequently accompany allergic rhinitis, and are freely movable and nontender.
Types of multiple myeloma. Multiple myeloma is the most common type of plasma cell cancer. The bones and bone marrow are the main sites where myeloma cells (abnormal plasma cells) are produced. The myeloma cells can form tumours, called plasmacytomas, in many bones in the body.
An untreated hepatic abscess is nearly uniformly fatal as a result of complications that include sepsis, empyema, or peritonitis from rupture into the pleural or peritoneal spaces, and retroperitoneal extension. Treatment should include drainage, either percutaneous or surgical. Antibiotic therapy as a sole treatment modality is not routinely advocated, though it has been successful in a few reported cases. It may be the only alternative in patients too ill to undergo invasive procedures or in those with multiple abscesses not amenable to percutaneous or surgical drainage. In these instances, patients are likely to require many months of antimicrobial therapy with serial imaging and close monitoring for associated complications.

An enlarged spleen may cause: No symptoms in some cases. Pain or fullness in the left upper abdomen that may spread to the left shoulder. Feeling full without eating or after eating only a small amount from the enlarged spleen pressing on your stomach. Anemia. Fatigue. Frequent infections. Easy bleeding.
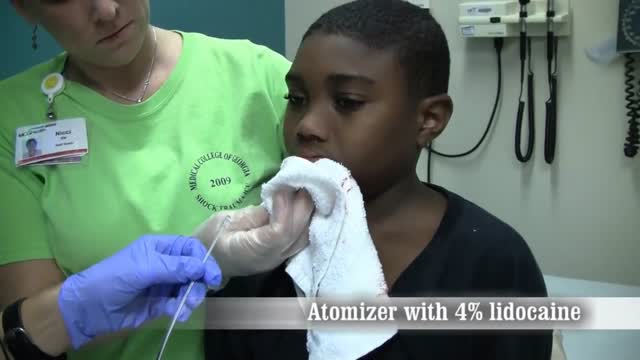
Nosebleeds common. Most often they are a nuisance and not a true medical problem. But they can be both. Nosebleed care Sit upright and lean forward. By remaining upright, you reduce blood pressure in the veins of your nose. This discourages further bleeding. Sitting forward will help you avoid swallowing blood, which can irritate your stomach. Pinch your nose. Use your thumb and index finger to pinch your nostrils shut. Breathe through your mouth. Continue to pinch for five to 10 minutes. Pinching sends pressure to the bleeding point on the nasal septum and often stops the flow of blood. To prevent re-bleeding, don't pick or blow your nose and don't bend down for several hours after the bleeding episode. During this time remember to keep your head higher than the level of your heart. If re-bleeding occurs, blow out forcefully to clear your nose of blood clots and spray both sides of your nose with a decongestant nasal spray containing oxymetazoline (Afrin, Mucinex Moisture Smart, others). Pinch your nose again as described above and call your doctor. When to seek emergency care The bleeding lasts for more than 20 minutes The nosebleed follows an accident, a fall or an injury to your head, including a punch in the face that may have broken your nose
Most babies will move into delivery position a few weeks prior to birth, with the head moving closer to the birth canal. When this fails to happen, the baby’s buttocks and/or feet will be positioned to be delivered first. This is referred to as “breech presentation.” Breech births occur in approximately 1 out of 25 full-term births.