Top videos

OB_A_1013
3D animation depicting the operating room and initial procedure preparing the patient for a laparoscopic hysterectomy. The patient is prepped and draped in the usual fashion and surrounded by the surgeon and surgical assistants. The skin is elevated, an infraumbilical incision is made, a trocar port is inserted through the incision and the abdomen is insufflated. Finally, a laparoscope is inserted into the port to allow for direct visualization of the uterus and the surgery can begin.
To view more animations and exhibits, visit our medical library: https://www.trialexhibitsinc.c....om/library/multimedi
Contact us on your next case for consulting, trial graphics, animations, medical illustrations or presentation services. 800-591-1123 [a]www.trialex.com[/a]
This video is for reference only. The video may not be otherwise used, reproduced nor modified. For more information to purchase a copy or permission to use this animation on your next case, project, website or TV, contact us at [a]www.trialex.com[/a] or 800-591-1123.
Copyright @ Trial Exhibits, Inc.

© 2023 Elsevier. All rights reserved. Histologically the cervix is different from the rest of the uterus and also has a mucosa that doesn’t shed during menstruation.
Find our full video library only on Osmosis Prime: http://osms.it/more.
Join over 3 million current & future clinicians who learn by Osmosis, and over 130 universities around the world who partner with us to make medical and health education more engaging and efficient. We have unparalleled tools and materials to prepare you to succeed in school, on board exams, and as a future clinician. Sign up for a free trial at http://osms.it/more. If you're interested in exploring an institutional partnership, visit osmosis.org/educators to request a personalized demo.
Follow us on social:
Facebook: http://osms.it/facebook
Twitter: http://osms.it/twitter
Instagram for med: http://osms.it/instagram
Instagram for nursing: https://osms.it/ignursing
Linkedin: https://osms.it/linkedin
Our Vision: Everyone who cares for someone will learn by Osmosis.
Our Mission: To empower the world’s clinicians and caregivers with the best learning experience possible. Learn more here: http://osms.it/mission
Medical disclaimer: Knowledge Diffusion Inc (DBA Osmosis) does not provide medical advice. Osmosis and the content available on Osmosis's properties (Osmosis.org, YouTube, and other channels) do not provide a diagnosis or other recommendation for treatment and are not a substitute for the professional judgment of a healthcare professional in diagnosis and treatment of any person or animal. The determination of the need for medical services and the types of healthcare to be provided to a patient are decisions that should be made only by a physician or other licensed health care provider. Always seek the advice of a physician or other qualified healthcare provider with any questions you have regarding a medical condition. © 2023 Elsevier. All rights reserved.

Ellis demonstrates how to clean a reusable inner cannula, care for a tracheostomy site, and suction a tracheostomy.
Our Critical Nursing Skills video tutorial series is taught by Ellis Parker MSN, RN-BC, CNE, CHS and intended to help RN and PN nursing students study for your nursing school exams, including the ATI, HESI and NCLEX.
#ClinicalSkills #NCLEX #tracheostomy #patientcare #ATI #Kaplan #LVN #PN #RN #nurseeducator #nurse #nursingstudent #murse #clinicals #clinicalnursingskills
00:00 What to expect Tracheostomy Care and Suctioning
0:33 Explaining the process Tracheostomy Care and Suctioning
1:10 Positioning patient for a Tracheostomy Care and Suctioning
1:33 Opening tray
1:46 Pouring saline
1:58 Removing inner cannula
2:14 Removing clean gloves
2:25 Donning sterile gloves
3:16 Showing tray contents
3:53 Removing previous dressing
4:06 Pouring saline
4:27 Cleaning stoma
5:10 Cleaning faceplate
5:20 Drying site
5:30 Cleaning inner cannula
6:00 Drying inner cannula
6:20 Reinserting inner cannula
6:40 Placing new gauze
7:00 Replacing ties
8:00 Replacing oxygen
8:13 Preparing for suction
8:58 Checking suction
9:30 Opening saline
9:42 Opening kit
9:58 Donning sterile gloves
11:04 Setting up saline container
11:20 Pouring saline
11:52 Connecting catheter to suction
12:46 Inserting catheter
13:10 Removing catheter
13:24 Rinsing catheter
13:40 Reoxyginating
14:05 Reinserting catheter
14:17 Removing catheter
14:29 Rinsing catheter
14:44 Reoxyginating
14:55 Cleaning up
15:09 Chatting about sterility
17:00 Checking a tie
🚨 Reminder: shipping deadlines are looming 👀
🎁 Regular Shipping: Order by Friday, December 15
🚀 Expedited Shipping: Order by Monday, December 18
🔍 Still searching for last-minute gifts? Consider a Level Up RN Gift Card! 💌 It’s not only a thoughtful present but also the perfect way to share treasures like Pharmacology Flashcards OR digital treasures like Flashables Digital Nursing Flashcards & the Level Up RN membership. Give the gift of knowledge this holiday season! 🧠⚡️💖 bit.ly/LevelUpRNGC
🚪 Access our Cram Courses, Quizzes and Videos all in one ad free space with Level Up RN Membership https://bit.ly/LevelUpRNMembership
Want more ways to MASTER Clinical Skills? Check out our flashcards & videos!
👇👇👇👇👇👇👇👇👇👇
👉 https://bit.ly/clinicalnursingskills 👈
☝️👆☝️👆☝️👆☝️👆☝️👆
This is your one-stop-shop for materials to help you LEARN & REVIEW so you can PASS Nursing School.
🤔🤔🤔 DO YOU WANT TO PASS your classes, proctored exams and the NCLEX? 🤔🤔🤔 Our resources are the best you can buy. They are built with a single goal: help you pass with no fluff. Everything you need, and nothing you don’t. Don’t take our word for it, though! Check out our hundreds of ⭐️⭐️⭐️⭐️⭐️ reviews from nurses who passed their exams and the NCLEX with Level Up RN.
🗂️ Our Ultimate Nursing School Survival kit is your number 1 resource to get through nursing school and to pass the NCLEX. Whether you're just starting school or you’re already prepping for the NCLEX, this bundle of flashcards is the best you can buy. It covers all the information you need to know to pass all your exams and it has FREE shipping!
➡️ https://bit.ly/TUNSSK ⬅️
L👀king for EVEN MORE resources to survive Nursing School? Make your Nursing School experience your own! Life’s difficult enough—learning shouldn’t be.
🪅 Games https://nursesquad.com
💻 Digital resources https://bit.ly/NursingStudyCourses
📅 Organizational tools https://bit.ly/OrganizingSchool
✨Want perks? Join our channel!
https://youtube.com/leveluprn/join
🏷 Head to https://leveluprn.com/specials for all our latest deals!🥳️
📧 LOOKING FOR FREE RESOURCES TO HELP WITH YOUR EXAMS? Get exclusive tips, latest video releases and more delivered to your email!
➡️ https://leveluprn.com/signup ⬅️
⚕ 👩 LEVEL UP NURSE SQUAD 👩⚕️
All of the nurses at Level Up RN are here to help! Cathy Parkes started helping her fellow classmates back when she was in nursing school, tutoring so they could pass their exams and graduate. After she got her BSN and started working as an RN at Scripps Encinitas Hospital, she started this YouTube channel to help nursing students around the world. Since then she has built a team of top-notch dedicated nurses and nurse educators who are focused on improving nursing education and supporting career advancement for nurses everywhere. With flashcards, videos, courses, organizational tools and more, we are singularly focused on helping students and nurses Level Up on their exams and nursing careers.

Today, the most common approach for open-heart surgery is a sternotomy, which requires a 12-14-inch incision through the breastbone. But in the hands of experienced minimally invasive surgeons, many cardiac procedures can be performed through smaller 2- to 3-inch incisions between the ribs without the need to cut through the breastbone. Learn more in this medical animation from Sarasota Memorial's Minimally Invasive Cardiac Surgery Team and medical director Jonathan Hoffberger, DO. For information or referrals, visit smhheart.com.

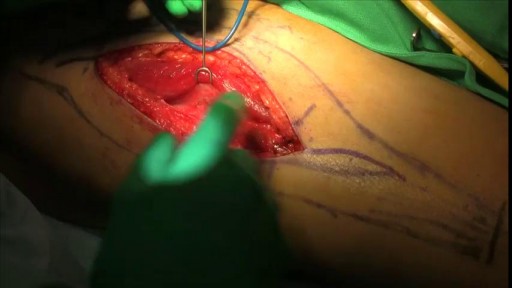
Diastasis recti often occurs during pregnancy and can persist after pregnancy. It affects core strength and the appearance of the abdominal muscles.
Dr. Erick Sanchez repairs the abdominal muscles with every tummy tuck. This short video shows the muscle repair portion of the surgery with a bonus after photo at the end!
To request a consultation with Dr. Sanchez, visit sanchezplasticsurgery.com and click Request a Consultation. Fill out the form and someone will get in touch with you to answer all your questions.
Expected cost can be found at the bottom of each procedure page on our website.
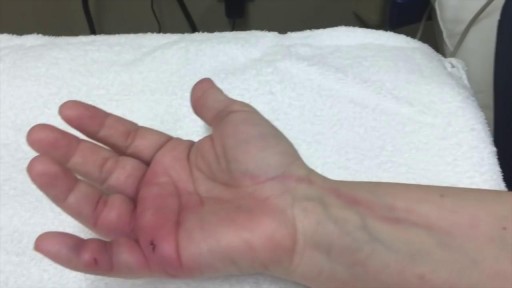
The most common symptoms of infection from animal bites are redness, pain, swelling, and inflammation at the site of the bite. You should seek immediate medical treatment if any of these symptoms continue for more than 24 hours. Other symptoms of infection include: pus or fluid oozing from the wound