Top videos

Fifth disease is a mild rash illness caused by parvovirus B19. This disease, also called erythema infectiosum, got its name because it was fifth in a list of historical classifications of common skin rash illnesses in children. It is more common in children than adults. A person usually gets sick with fifth disease within 4 to 14 days after getting infected with parvovirus B19.
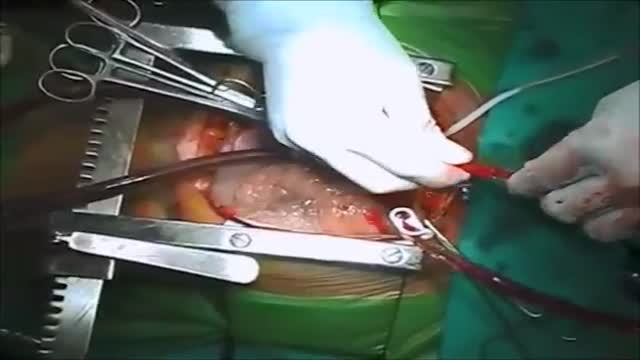
Ventricular septal rupture (VSR) is a rare but lethal complication of myocardial infarction (MI). The event occurs 2-8 days after an infarction and often precipitates cardiogenic shock. [1] The differential diagnosis of postinfarction cardiogenic shock should exclude free ventricular wall rupture and rupture of the papillary muscles. (See the image below.)
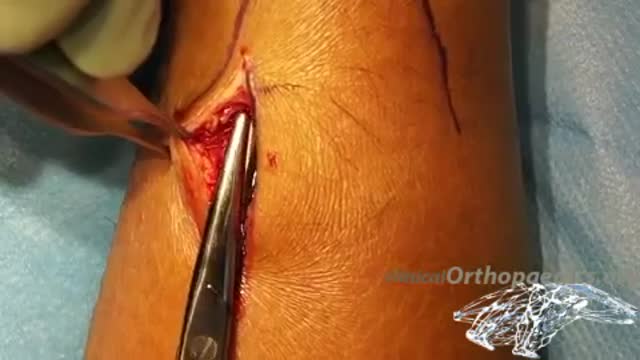
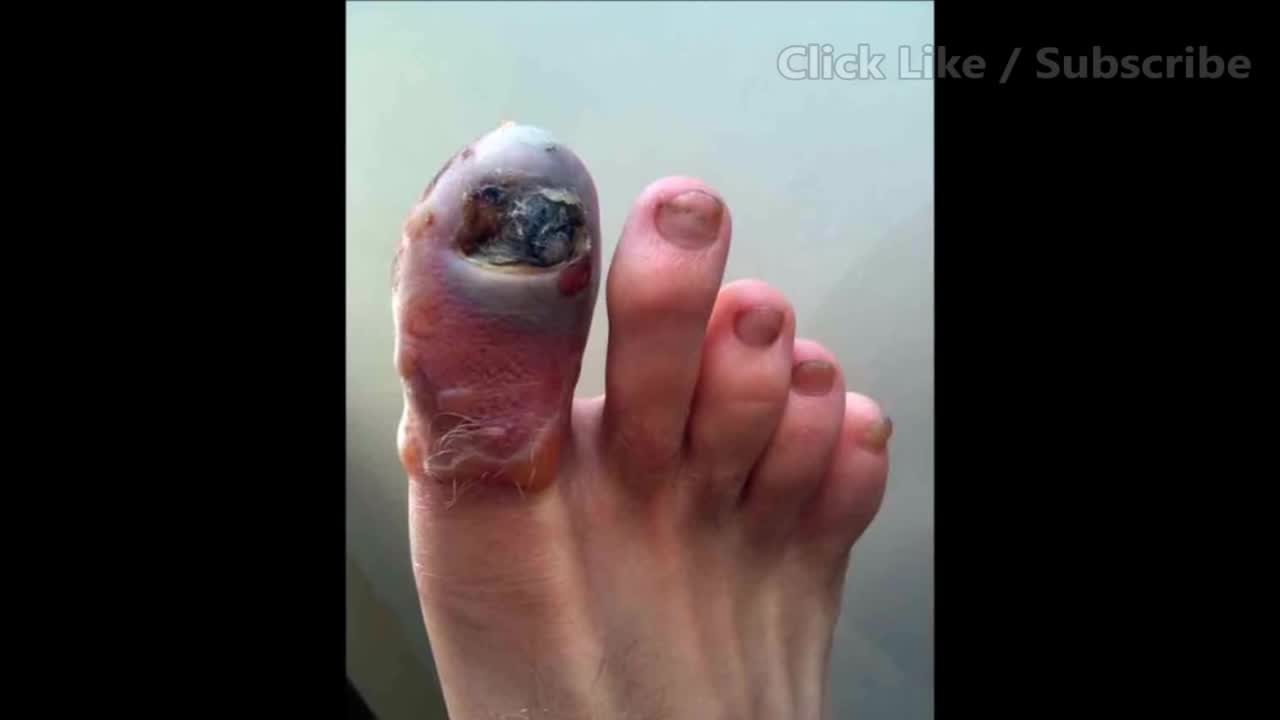
A leg ulcer is simply a break in the skin of the leg, which allows air and bacteria to get into the underlying tissue. This is usually caused by an injury, often a minor one that breaks the skin. In most people such an injury will heal up without difficulty within a week or two. However, when there is an underlying problem the skin does not heal and the area of breakdown can increase in size. This is a chronic leg ulcer.

How do you make a working human heart? Scientists can turn stem cells into beating heart cells, but getting them to organize into a 3D heart requires a scaffold. At the Massachusetts General Hospital in Boston, Harald Ott and his team are reusing the scaffold that nature provides. They’re stripping away all the living cells from dead hearts, before filling in the leftover matrix with healthy new cells. In this video, Brendan Maher finds out how the technique could be used to develop parts of the heart, like the aortic root and valve, for transplant.
Megacolon, as well as megarectum, is a descriptive term. It denotes dilatation of the colon that is not caused by mechanical obstruction.[1, 2] Although the definition of megacolon has varied in the literature, most researchers use the measurement of greater than 12 cm for the cecum as the standard. Because the diameter of the large intestine varies, the following definitions would also be considered: greater than 6.5 cm in the rectosigmoid region and greater than 8 cm for the ascending colon. Megacolon can be divided into the following 3 categories: Acute megacolon ( pseudo-obstruction) Chronic megacolon, which includes congenital, acquired, and idiopathic causes Toxic megacolon
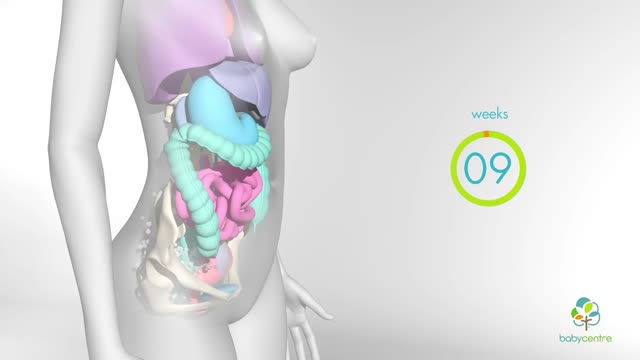
In your first few months of pregnancy, hormones flood your body. Your baby is still tiny but already your body is changing. Your breasts start to swell and may feel tender. Tiredness, nausea and frequent trips to the loo are common pregnancy symptoms.
A needle is inserted into a joint for two main indications: aspiration of fluid (arthrocentesis) for diagnosis or for relief of pressure, or injection of medications. In practical terms, most injections into joints consist of a glucocorticoid, a local anesthetic, or a combination of the two. Occasionally saline is injected into the joint to diagnose a joint injury. This topic will review the basic technique of inserting a needle into a joint and the main indications for intraarticular steroid injections. The same techniques apply for injection of the less commonly used hyaluronate viscosupplementation agents into knees, hips, and perhaps shoulders.
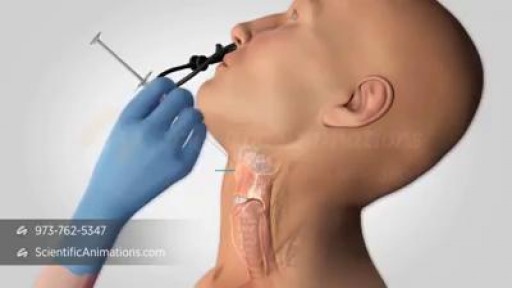
The voice box, or larynx, has three important functions. It is necessary for breathing, voice and swallowing. The vocal folds have two positions, open (apart) for breathing (picture I) and closed (together) for making sound, coughing and sealing off the lungs when swallowing (picture II). When one of the vocal folds are paralyzed, it usually rests in an in-between position (picture III), and neither opens for breathing, nor closes for voicing, coughing, or swallowing. Usually, the effects on the voice are the most dramatic. The voice becomes weak and breathy. People can only say a few words per breath, and are frequently out-of-breath, or physically tired when trying to speak for more than a few minutes straight. The voice may also get somewhat high and squeaky, with a diminished range. Swallowing may be affected as well, where you may notice some choking or coughing with certain liquids. Your cough is frequently different and very weak. This is a serious problem for patients with with vocal fold paralysis because one of the most important functions of the larynx is to keep liquids out of the lungs, and to be able to cough up mucus. When this does not happen, you are at risk for getting an "aspiration" pneumonia. The surgical procedure to restore these important functions is called "medialization laryngoplasty"
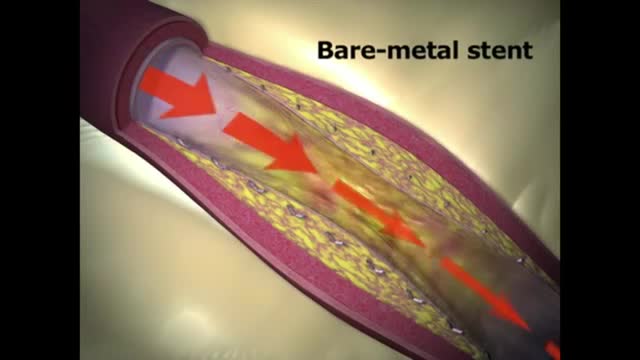
INDICATIONS The Absorb GT1 Bioresorbable Vascular Scaffold (BVS) is a temporary scaffold that will fully resorb over time and is indicated for improving coronary luminal diameter in patients with ischemic heart disease due to de novo native coronary artery lesions (length ≤ 24 mm) with a reference vessel diameter of ≥ 2.5 mm and ≤ 3.75 mm WHAT ARE THE POTENTIAL RISKS AND COMPLICATIONS? Treatment options for CAD have become increasingly common but, as with any invasive procedure, there are potential risk factors and complications. Serious complications do not occur often, and research is ongoing to make these procedures even safer and more effective. The risk of complications from percutaneous treatment methods may be higher for individuals: 75 years of age and older Who are women Who have kidney disease or diabetes Who have serious heart disease Who have had prior cardiac interventions

► Sign up here and try our FREE content: http://lectur.io/freecontentyt
► If you’re an medical educator or faculty member, visit: http://lectur.io/medytb2u
This video “Epithelium” is part of the Lecturio course “Histology” ► WATCH the complete course on http://lectur.io/epithelium
► LEARN ABOUT:
- Introduction: Epithelial Tissue
- Summary of structure and function
- Epithelium
- Three characteristics of any Epithelium
- Epithelium: Classification
- Epithelium: Epithelial Cells Exhibit Polarity
- Epithelium: How Are Epithelial Cells Joined Together?
- Epithelium: Surfaces of Epithelial Cells
- Epithelium: Basement Membrane
► THE PROF: Your lecturer is Professor Geoff Meyer. He is currently teaching at the School of Anatomy, Physiology and Human Biology at the University of Western Australia (UWA). As a leading anatomy and histology expert he is also coordinating the Federative International Program for Anatomical Terminologies (FIPAT) of the International Federation of Associations of Anatomists (IFAA). Besides medical research on the ovarian function, steroidogenesis, corpus luteum, angiogenesis, and microcirculation, Geoff Meyer’s research activities also focus on developing innovative, computer-aided learning and teaching tools. For his inventiveness, Geoff Meyer has received a number of awards, including the Australian University Teaching Award.
► LECTURIO is your single-point resource for medical school:
Study for your classes, USMLE Step 1, USMLE Step 2, MCAT or MBBS with video lectures by world-class professors, recall & USMLE-style questions and textbook articles. Create your free account now: http://lectur.io/epithelium
► INSTALL our free Lecturio app
iTunes Store: https://app.adjust.com/z21zrf
Play Store: https://app.adjust.com/b01fak
► READ TEXTBOOK ARTICLES related to this video:
Epithelium — Functions and Types of Epithelial Tissue
http://lectur.io/epitheliumarticle
► SUBSCRIBE to our YouTube channel: http://lectur.io/subscribe
► WATCH MORE ON YOUTUBE: http://lectur.io/playlists
► LET’S CONNECT:
• Facebook: https://www.facebook.com/lectu....rio.medical.educatio
• Instagram: https://www.instagram.com/lecturio_medical_videos
• Pinterest: https://www.pinterest.de/lecturiomedical
• LinkedIn: https://www.linkedin.com/company/lecturio-medical/

Acute respiratory distress syndrome (ARDS) occurs when fluid builds up in the tiny, elastic air sacs (alveoli) in your lungs. More fluid in your lungs means less oxygen can reach your bloodstream. This deprives your organs of the oxygen they need to function. ARDS typically occurs in people who are already critically ill or who have significant injuries. Severe shortness of breath — the main symptom of ARDS — usually develops within a few hours to a few days after the original disease or trauma. Many people who develop ARDS don't survive. The risk of death increases with age and severity of illness. Of the people who do survive ARDS, some recover completely while others experience lasting damage to their lungs.
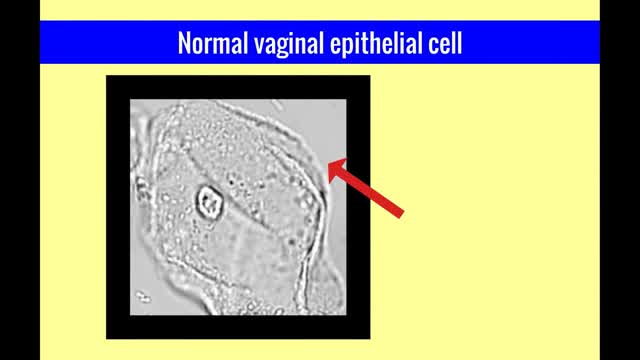
The vulvar vaginal diseases service sees referrals to help women with short--and long--term problems of the outer genital area (vulva), vagina and pelvic floor muscles including: Vulvar vaginal burning, itching, irritation and pain Vulvar Vestibulitis Pain with intercourse Discharge Yeast infections Bacterial vaginosis Pelvic floor muscle dysfunction A patient must be referred by her local health care provider. Services include: Skin care education Examinations-Your healthcare provider will examine you and talk with you about recommendations for treatment and/or management of your symptoms. Some vulvar diseases require a biopsy to diagnose the condition. Referrals-Your healthcare team may refer you to other specialists, including physical therapists or health psychologists. Separate insurance authorization is necessary for these services. The clinic staff provides general education and support to help women cope with these very personal health problems. Following a clinic visit, a letter is promptly sent to your local health care provider. The letter provides the results of your exam and the plan of care.

Bacterial abscess of the liver is relatively rare; however, it has been described since the time of Hippocrates (400 BCE), with the first published review by Bright appearing in 1936. In 1938, Ochsner's classic review heralded surgical drainage as the definitive therapy; however, despite the more aggressive approach to treatment, the mortality remained at 60-80%.[1] The development of new radiologic techniques, the improvement in microbiologic identification, and the advancement of drainage techniques, as well as improved supportive care, have reduced mortality to 5-30%; yet, the prevalence of liver abscess has remained relatively unchanged. Untreated, this infection remains uniformly fatal. The three major forms of liver abscess, classified by etiology, are as follows: Pyogenic abscess, which is most often polymicrobial, accounts for 80% of hepatic abscess cases in the United States Amebic abscess due to Entamoeba histolytica accounts for 10% of cases [2] Fungal abscess, most often due to Candida species, accounts for fewer than 10% of cases

Cerebral palsy is a disorder of movement, muscle tone or posture that is caused by damage that occurs to the immature, developing brain, most often before birth. Signs and symptoms appear during infancy or preschool years. In general, cerebral palsy causes impaired movement associated with abnormal reflexes, floppiness or rigidity of the limbs and trunk, abnormal posture, involuntary movements, unsteady walking, or some combination of these. People with cerebral palsy may have problems swallowing and commonly have eye muscle imbalance, in which the eyes don't focus on the same object. People with cerebral palsy also may suffer reduced range of motion at various joints of their bodies due to muscle stiffness. Cerebral palsy's effect on functional abilities varies greatly. Some affected people can walk while others can't. Some people show normal or near-normal intellectual capacity, but others may have intellectual disabilities. Epilepsy, blindness or deafness also may be present.

Do you need to do a parasite cleanse? Probably... I hear from so many people suffering from symptoms of parasites - severe bloating, cramps, constipation, diarrhoea. A big problem in getting to the bottom of this (pun intended) is that the mainstream medical system really doesn’t have a way to detect, or even find most forms of parasites. They give you drugs for the symptoms, but essentially the parasites aren’t removed during that process.