Top videos
Forzest is FDA approved medicine, it is used bt men to improve erectile dysfunction dusring intercourse session with partner. for more information related side effects, dosage, etc kindly visit to http://www.medstorerx.com/forzest.aspx

A hemolytic transfusion reaction is a serious complication that can occur after a transfusion of blood. The red blood cells that were given in the transfusion are destroyed by the patient's immune system. There are other types of allergic transfusion reactions that do not cause hemolysis.

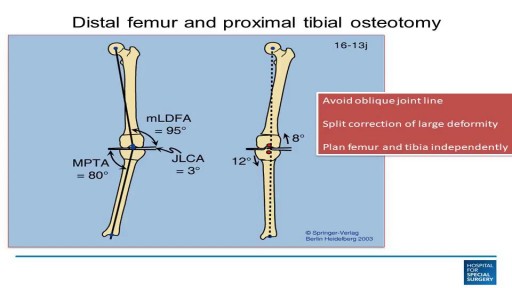
These are a few common types of benign bone tumors: Osteochondroma is the most common benign bone tumor. ... Giant cell tumor is a benign tumor, typically affecting the leg (malignant types of this tumor are uncommon). Osteoid osteoma is a bone tumor, often occurring in long bones, that occurs commonly in the early 20s.
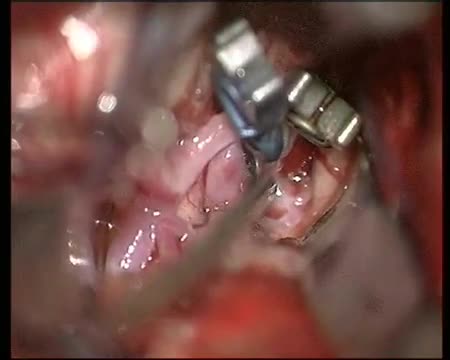
The goal of surgical clipping is to isolate an aneurysm from the normal circulation without blocking off any small perforating arteries nearby. Under general anesthesia, an opening is made in the skull, called a craniotomy. The brain is gently retracted to locate the aneurysm. A small clip is placed across the base, or neck, of the aneurysm to block the normal blood flow from entering. The clip works like a tiny coil-spring clothespin, in which the blades of the clip remain tightly closed until pressure is applied to open the blades. Clips are made of titanium and remain on the artery permanently.
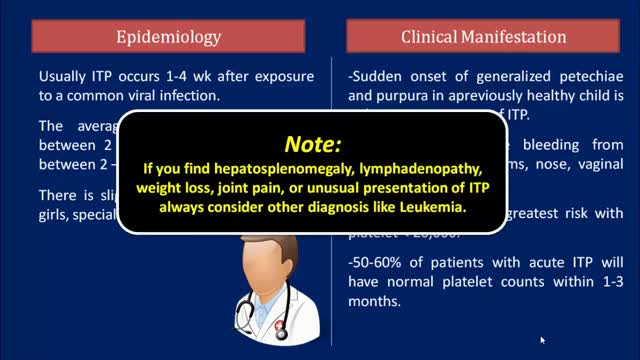
Idiopathic thrombocytopenic purpura (ITP) is a disorder that can lead to easy or excessive bruising and bleeding. The bleeding results from unusually low levels of platelets — the cells that help blood clot. Idiopathic thrombocytopenic purpura, which is also called immune thrombocytopenia, affects children and adults. Children often develop ITP after a viral infection and usually recover fully without treatment. In adults, the disorder is often long term. If you don't have signs of bleeding and your platelet count isn't too low, you may not need any treatment. In rare cases, the number of platelets may be so low that dangerous internal bleeding occurs. Treatment options are available.
Alagille syndrome (AS) is an autosomal dominant disorder (OMIM 118450) associated with abnormalities of the liver, heart, skeleton, eye, and kidneys and a characteristic facial appearance. In 1973, Watson and Miller reported 9 cases of neonatal liver disease with familial pulmonary valvular stenosis.