Top videos
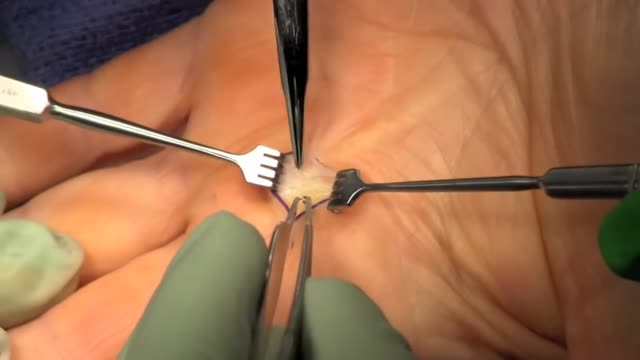
Trigger finger, also known as stenosing tenosynovitis (stuh-NO-sing ten-o-sin-o-VIE-tis), is a condition in which one of your fingers gets stuck in a bent position. Your finger may straighten with a snap — like a trigger being pulled and released. Trigger finger occurs when inflammation narrows the space within the sheath that surrounds the tendon in the affected finger. If trigger finger is severe, your finger may become locked in a bent position. People whose work or hobbies require repetitive gripping actions are at higher risk of developing trigger finger. The condition is also more common in women and in anyone with diabetes. Treatment of trigger finger varies depending on the severity.
Alagille syndrome (AS) is an autosomal dominant disorder (OMIM 118450) associated with abnormalities of the liver, heart, skeleton, eye, and kidneys and a characteristic facial appearance. In 1973, Watson and Miller reported 9 cases of neonatal liver disease with familial pulmonary valvular stenosis.
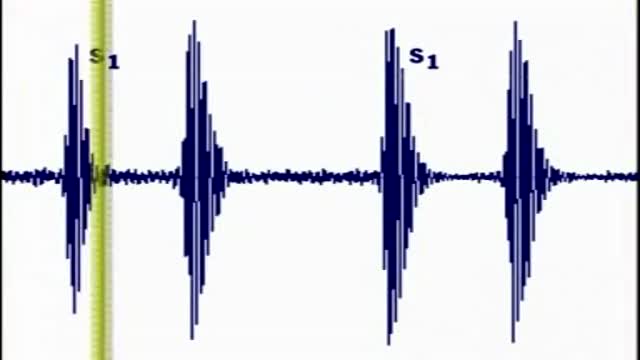
Heart sounds are the noises generated by the beating heart and the resultant flow of blood through it. Specifically, the sounds reflect the turbulence created when the heart valves snap shut. In cardiac auscultation, an examiner may use a stethoscope to listen for these unique and distinct sounds that provide important auditory data regarding the condition of the heart. In healthy adults, there are two normal heart sounds often described as a lub and a dub (or dup), that occur in sequence with each heartbeat. These are the first heart sound (S1) and second heart sound (S2), produced by the closing of the atrioventricular valves and semilunar valves, respectively. In addition to these normal sounds, a variety of other sounds may be present including heart murmurs, adventitious sounds, and gallop rhythms S3 and S4. Heart murmurs are generated by turbulent flow of blood, which may occur inside or outside the heart. Murmurs may be physiological (benign) or pathological (abnormal). Abnormal murmurs can be caused by stenosis restricting the opening of a heart valve, resulting in turbulence as blood flows through it. Abnormal murmurs may also occur with valvular insufficiency (regurgitation), which allows backflow of blood when the incompetent valve closes with only partial effectiveness. Different murmurs are audible in different parts of the cardiac cycle, depending on the cause of the murmur.

A hemolytic transfusion reaction is a serious complication that can occur after a transfusion of blood. The red blood cells that were given in the transfusion are destroyed by the patient's immune system. There are other types of allergic transfusion reactions that do not cause hemolysis.
Forzest is FDA approved medicine, it is used bt men to improve erectile dysfunction dusring intercourse session with partner. for more information related side effects, dosage, etc kindly visit to http://www.medstorerx.com/forzest.aspx

The Ortolani method is an examination method that identifies a dislocated hip that can be reduced into the socket (acetabulum). Ortolani described the feeling of reduction as a “Hip Click” but the translation from Italian was interpreted a sound instead of a sensation of the hip moving over the edge of the socket when it re-located. After the age of six weeks, this sensation is rarely detectable and should not be confused with snapping that is common and can occur in stable hips when ligaments in and around the hip create clicking noises. When the Ortolani test is positive because the hip is dislocated, treatment is recommended to keep the hip in the socket until stability has been established

The vagina is the most delicate and sensitive part of every woman’s body. Naturally female vagina appears to be darker compared to the complexion of other parts of the body. Hence, it is every woman’s dream to have a white complexioned vagina just like their body skin. Most of the women feel that using shop every day may keep their vagina clean and help to make it lighter. But reality is just the opposite. Soaps contain harsh chemicals which not only irritate the delicate skin of vagina and make it darker but they also dis-balance the ph level which plays an important role in maintaining the normal texture of the skin. Well, women need not get disappointed as now there are alternatives of harsh soaps in the market. These alternatives are none other than natural creams which are the best solution to have a naturally fair and glowing vagina without any side effects. Mentioned below are some of the best natural products available in the market to whiten vagina naturally.
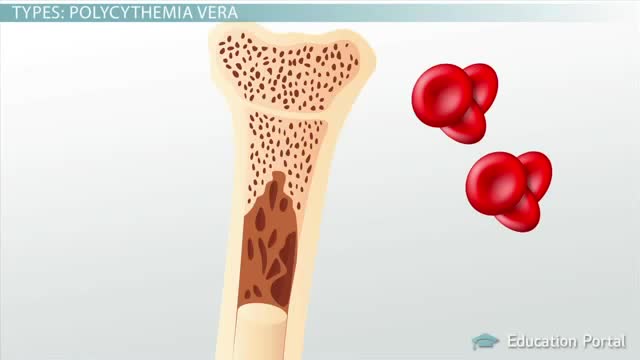
Polycythemia vera (pol-e-sigh-THEE-me-uh VEER-uh) is a slow-growing type of blood cancer in which your bone marrow makes too many red blood cells. Polycythemia vera may also result in production of too many of the other types of blood cells — white blood cells and platelets. These excess cells thicken your blood and cause complications, such as such as a risk of blood clots or bleeding. Polycythemia vera isn't common. It usually develops slowly, and you may have it for years without noticing signs or symptoms. Often, polycythemia vera is found during a blood test done for some other reason. Without treatment, polycythemia vera can be life-threatening. However, with proper medical care, many people experience few problems related to this disease. Over time, there's a risk of progressing to more-serious blood cancers, such as myelofibrosis or acute leukemia.
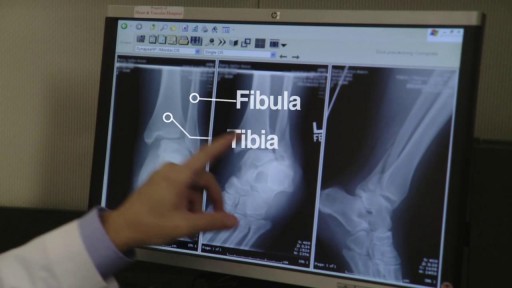
A boxer's fracture is a break through the bones of the hand that form the knuckles. Some doctors use the term "brawler's fracture" rather than "boxer's fracture" because a boxer is not likely to get this injury. The less well-trained brawlers have to learn how to punch without hurting themselves. The metacarpal bones in the hand connect the bones in the finger to the bones in the wrist. There are five metacarpal bones, one to connect each finger to the wrist. All of the metacarpal bones have the same anatomic structure. Each consists of the base, the shaft, the neck, and the head
Idiopathic thrombocytopenic purpura (ITP) is a disorder that can lead to easy or excessive bruising and bleeding. The bleeding results from unusually low levels of platelets — the cells that help blood clot. Idiopathic thrombocytopenic purpura, which is also called immune thrombocytopenia, affects children and adults. Children often develop ITP after a viral infection and usually recover fully without treatment. In adults, the disorder is often long term. If you don't have signs of bleeding and your platelet count isn't too low, you may not need any treatment. In rare cases, the number of platelets may be so low that dangerous internal bleeding occurs. Treatment options are available.

URBN Dental is here not only to take care of your tooth decay and prevent gingivitis, but also to give you the best at home dental care instructions as well. Do you find brushing your teeth confusing, or are you unsure whether or not you are brushing correctly? The golden standard when it comes to brushing teeth is brushing twice a day for two minute sessions each. You can break down the mouth into four quadrants: upper right, upper left, lower left, and lower right. By doing this, it will be easier for you to brush for thirty seconds in each area and focus on the correct movement instead of location. It is very important to angle the toothbrush at a forty five degree angle to the tooth and gums while using circular motions to remove food debris and plaque. When it comes to your front teeth, using the brush in a vertical position and combining it with circular motions is effective. Using the dental techniques will ensure healthier teeth that are cavity free and less bleeding gums.

Your body's immune system protects you from disease and infection. But if you have an autoimmune disease, your immune system attacks healthy cells in your body by mistake. Autoimmune diseases can affect many parts of the body. No one is sure what causes autoimmune diseases. They do tend to run in families. Women - particularly African-American, Hispanic-American, and Native-American women - have a higher risk for some autoimmune diseases. There are more than 80 types of autoimmune diseases, and some have similar symptoms. This makes it hard for your health care provider to know if you really have one of these diseases, and if so, which one. Getting a diagnosis can be frustrating and stressful. Often, the first symptoms are fatigue, muscle aches and a low fever. The classic sign of an autoimmune disease is inflammation, which can cause redness, heat, pain and swelling. The diseases may also have flare-ups, when they get worse, and remissions, when symptoms get better or disappear. Treatment depends on the disease, but in most cases one important goal is to reduce inflammation. Sometimes doctors prescribe corticosteroids or other drugs that reduce your immune response.