Top videos
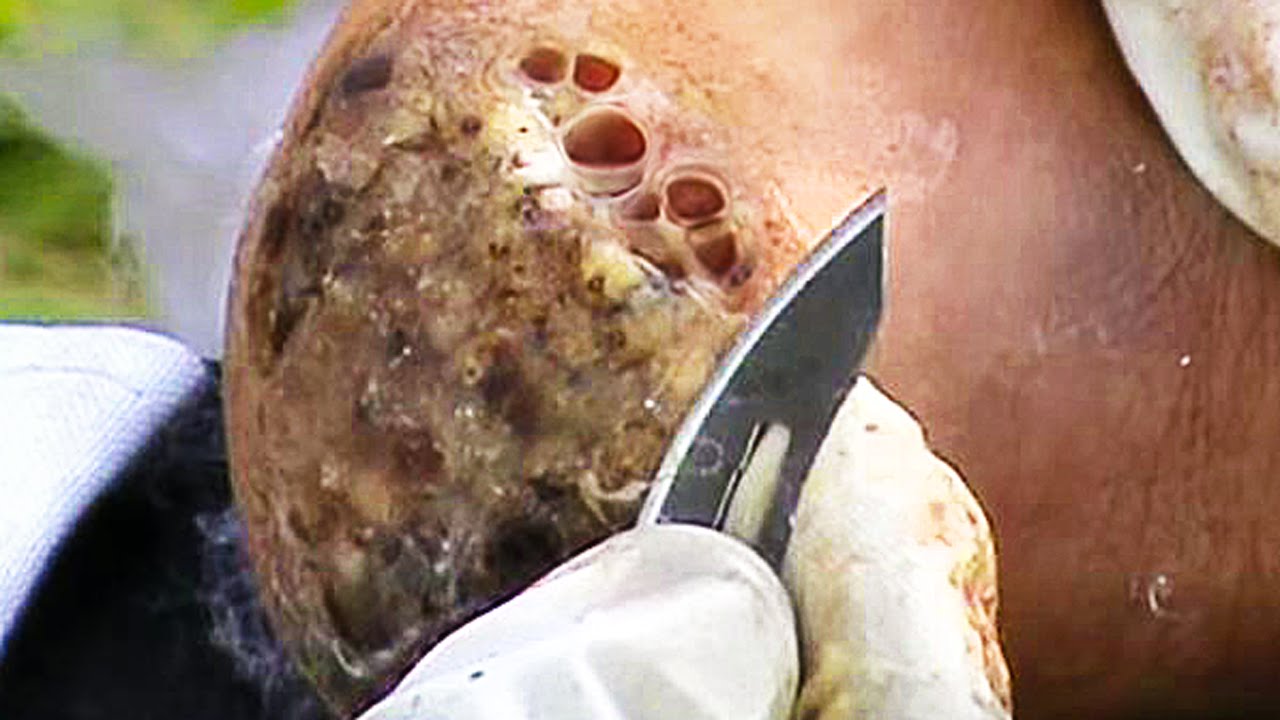
The most common symptoms of infection from animal bites are redness, pain, swelling, and inflammation at the site of the bite. You should seek immediate medical treatment if any of these symptoms continue for more than 24 hours. Other symptoms of infection include: pus or fluid oozing from the wound

This sqadia.com short video clip is a brief explanation of Epithelium.
Epithelium is one of the four basic tissues of the body and is derived from all three germ layers.
It is composed of very closely packed, contiguous cells, with very little or no extracellular material in the extracellular spaces.
----------------------------------------
Histology Lectures Collection -
https://www.sqadia.com/categor....ies/anatomy-histolog
----------------------------------------
Epithelial membranes can be: Simple squamous epithelium, Simple cuboidal epithelium, Simple columnar epithelium, and Pseudostratified epithelium.
----------------------------------------
5500+ Medical Videos
Try for FREE! - https://www.sqadia.com/categories/free
----------------------------------------
When there are two or more layers of cells epithelia is referred to as stratified, hence can be stratified squamous, stratified cuboidal and stratified columnar.
----------------------------------------
Facebook - https://www.facebook.com/sqadiacom
Instagram - https://www.instagram.com/sqadiacom
LinkedIN - https://www.linkedin.com/showcase/sqadia-com
Pinterest - https://www.pinterest.com/sqadiacom
TumblR - https://sqadiacom.tumblr.com
Twitter - https://twitter.com/sqadiacom
Vimeo - https://vimeo.com/sqadiacom
YouTube - https://www.youtube.com/sqadiacom
----------------------------------------

A patient at a British hospital played Mahler and Gershwin on the violin while surgeons removed a tumor from her brain, so doctors could preserve her ability to play music.
She left the hospital 3 days later and hopes to return to the symphony soon. https://abcn.ws/2SGY9mp
SUBSCRIBE to ABC NEWS: https://www.youtube.com/ABCNews/
Watch More on http://abcnews.go.com/
LIKE ABC News on FACEBOOK
https://www.facebook.com/abcnews
FOLLOW ABC News on TWITTER:
https://twitter.com/abc
GOOD MORNING AMERICA'S HOMEPAGE:
https://www.goodmorningamerica.com/
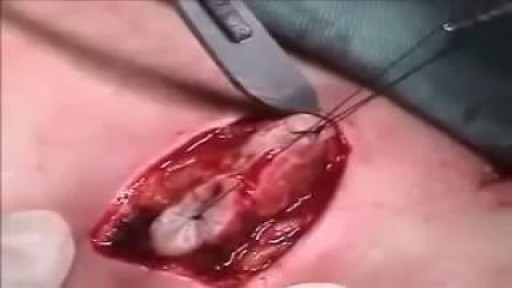
Care must be taken to prevent stenosis at the anastomotic site. If the diameter of the anastomosis is less than 2 cm, the anastomosis should be taken down and resected. A classic end-to-end anastomosis should be performed to ensure adequate diameter to the intestine. If the posterior wall of the colon has been preserved, care should be taken to close the colostomy prior to opening the peritoneal cavity. This will reduce intraperitoneal contamination from the stoma site. Copious irrigation of the wound should be made prior to primary closure. If gross contamination has occurred, delayed closure of the wound should be considered.
FREE Nursing School Cheat Sheets at: http://www.NURSING.com
Get the full lesson on IM Injections here:
https://nursing.com/lesson/ski....lls-06-01-pill-crush
Check out our new Nurse Care Plan Lessons here:
https://bit.ly/3BPRfPL
Get Access to Thousands of Lessons here:
https://nursing.com/courses/
Welcome to the NURSING Family, we call it the most supportive nursing cohort on the planet.
At NURSING.com, we want to help you remove the stress and overwhelm of nursing school so that you can focus on becoming an amazing nurse.
Check out our freebies and learn more at: (http://www.nursing.com)
Intramuscular Injection Techniques (Nursing Skills)
In this video, we’re going to look at proper administration techniques for intramuscular medication administration. Of course, always follow your 5 rights and calculate the correct volume for administration. We love you guys! Go out and be your best selves today! And, as always, happy nursing!
Bookmarks:
0.05 Introduction to Intramuscular injections
0.16 site and needle selection
0.35 site sterilization
0.43 Z track method
0.58 needle insertion
1.10 medication injection
1.14 needle removal
1.25 bandaging and needle disposal
1.30 documentation and patient monitoring
1.35 Outro
Visit us at https://nursing.com/medical-disclaimer/ for disclaimer information.
NCLEX®, NCLEX-RN® are registered trademarks of the National Council of State Boards of Nursing, INC. and hold no affiliation with NURSING.com.

A breech birth is the birth of a baby from a breech presentation. In the breech presentation the baby enters the birth canal with the buttocks or feet first as opposed to the normal head first presentation.
There are either three or four main categories of breech births, depending upon the source:
* Frank breech - the baby's bottom comes first, and his or her legs are flexed at the hip and extended at the knees (with feet near the ears). 65-70% of breech babies are in the frank breech position.
* Complete breech - the baby's hips and knees are flexed so that the baby is sitting crosslegged, with feet beside the bottom.
* Footling breech - one or both feet come first, with the bottom at a higher position. This is rare at term but relatively common with premature fetuses.
* Kneeling breech - the baby is in a kneeling position, with one or both legs extended at the hips and flexed at the knees. This is extremely rare, and is excluded from many classifications.
As in labour with a baby in a normal head-down position, uterine contractions typically occur at regular intervals and gradually cause the cervix to become thinner and to open. In the more common breech presentations, the baby’s bottom (rather than feet or knees) is what is first to descend through the maternal pelvis and emerge from the vagina.
At the beginning of labour, the baby is generally in an oblique position, facing either the right or left side of the mother's back. As the baby's bottom is the same size in the term baby as the baby's head. Descent is thus as for the presenting fetal head and delay in descent is a cardinal sign of possible problems with the delivery of the head.
In order to begin the birth, internal rotation needs to occur. This happens when the mother's pelvic floor muscles cause the baby to turn so that it can be born with one hip directly in front of the other. At this point the baby is facing one of the mother's inner thighs. Then, the shoulders follow the same path as the hips did. At this time the baby usually turns to face the mother's back. Next occurs external rotation, which is when the shoulders emerge as the baby’s head enters the maternal pelvis. The combination of maternal muscle tone and uterine contractions cause the baby’s head to flex, chin to chest. Then the back of the baby's head emerges and finally the face.
Due to the increased pressure during labour and birth, it is normal for the baby's leading hip to be bruised and genitalia to be swollen. Babies who assumed the frank breech position in utero may continue to hold their legs in this position for some days after birth.
Most women have vaginal discharge at many different times throughout their cycle. During ovulation, white and watery discharge is common and accepted as normal. But, discharge after ovulation is widely believed to be a sign of pregnancy.

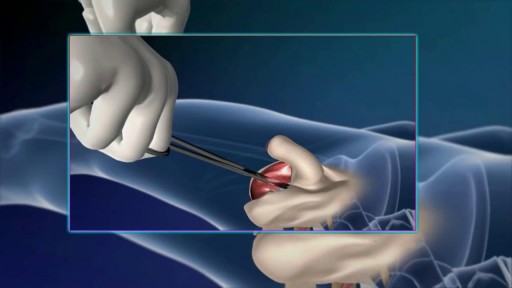
It’s called gamma knife surgery, but there’s no cutting involved.
It’s been used at Mayo Clinic for 30 years as an alternative to open brain surgery.
The patient’s head is held still during the procedure with a headframe, which also serves as a map for the radiation. Using 3D imaging — typically an MRI — as a guide, the gamma knife is targeted directly at the tumor.
And with no hospital stay and minimal side effects, it’s a procedure that is efficient and can be lifesaving.
More health and medical news on the Mayo Clinic News Network. https://newsnetwork.mayoclinic.org/
Journalists: Clean and nat sound versions of this pkg available for download at https://newsnetwork.mayoclinic.org/
Register (free) at https://newsnetwork.mayoclinic.org/request-account/