Top videos

🔥 Multivitamins for Men: https://lynxshort.com/Multivitamins-for-Men
✨ Multivitamins for Women: https://lynxshort.com/Multivitamins-for-Women
⭐ Multivitamins for Kids: https://lynxshort.com/Multivitamins-for-Kids
📙 Book of the Day 📚 https://lynxshort.com/Book-of-the-Day
This is one of the most interesting medical topics to discuss. What are the responsibilities of a doctor? What are the basic skills a doctor needs to have? and what are the responsibilities of a doctor?
**** CONNECT ****
- " Medical Videos " Android application on Google Play store:
https://play.google.com/store/....apps/details?id=com.
https://healthusher.com
https://www.facebook.com/MedicalVideosAnimated
https://www.instagram.com/medical_videos1
👉 Support Us to Help Us Continue Making Videos.. Thanks in Advance :)
- Via PayPal: https://www.paypal.me/medicalvideos
- Via Patreon: https://www.patreon.com/medicalvideosanimated
- The creator:
Pharmacist. Alaa Nasr
#MedicalVideosAnimated
Affiliate Disclaimer: This video and description contains affiliate links, which means that if you click on one of the product links, I'll receive a small commission. This is at no extra cost to you and in many cases include exclusive discounts where applicable. This helps support the channel and allows me to continue to make free videos like this. Thank you for the support!
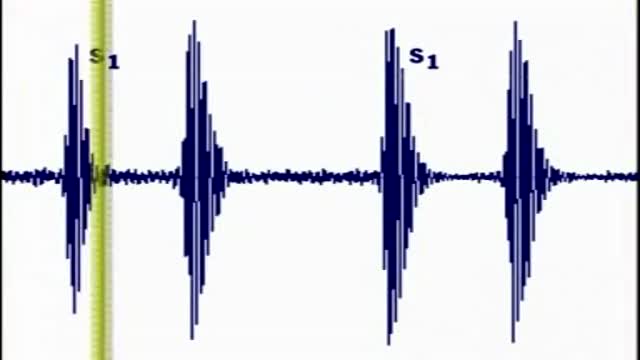
Heart sounds are the noises generated by the beating heart and the resultant flow of blood through it. Specifically, the sounds reflect the turbulence created when the heart valves snap shut. In cardiac auscultation, an examiner may use a stethoscope to listen for these unique and distinct sounds that provide important auditory data regarding the condition of the heart. In healthy adults, there are two normal heart sounds often described as a lub and a dub (or dup), that occur in sequence with each heartbeat. These are the first heart sound (S1) and second heart sound (S2), produced by the closing of the atrioventricular valves and semilunar valves, respectively. In addition to these normal sounds, a variety of other sounds may be present including heart murmurs, adventitious sounds, and gallop rhythms S3 and S4. Heart murmurs are generated by turbulent flow of blood, which may occur inside or outside the heart. Murmurs may be physiological (benign) or pathological (abnormal). Abnormal murmurs can be caused by stenosis restricting the opening of a heart valve, resulting in turbulence as blood flows through it. Abnormal murmurs may also occur with valvular insufficiency (regurgitation), which allows backflow of blood when the incompetent valve closes with only partial effectiveness. Different murmurs are audible in different parts of the cardiac cycle, depending on the cause of the murmur.

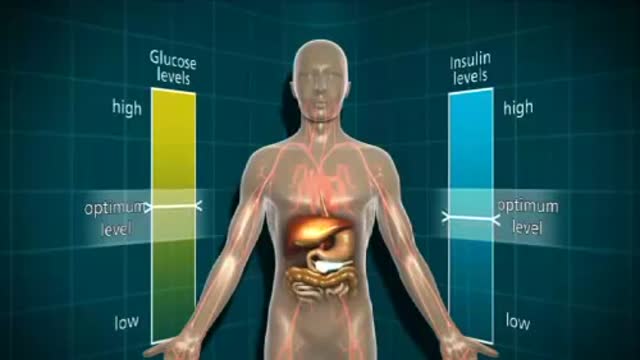
NTIS refers to a syndrome found in seriously ill or starving patients with low fT3, usually elevated RT3, normal or low TSH, and if prolonged, low fT4. It is found in a high proportion of patients in the ICU setting, and correlates with a poor prognosis if TT4 is <4ug/dl. The patho-physiology includes suppression of TRH release, reducedT3 and T4 turnover, reduction in liver generation of T3, increased formation of RT3, and tissue specific down-regulation of deiodinases, transporters, and TH receptors. Although long debated, tissue TH levels are definitely reduced, and tissue hypothyroidism is presumably present. This is often not clinically evident because of the brief duration, and reduced but not absent tissue levels of TH. Although recognized for nearly 4 decades, interpretation of the syndrome is contested, because of lack of data. Some observes, totally without data, argue that it is a protective response and should not be treated. Other observers (as in this review) present available data suggesting, but not proving, that thyroid hormone replacement is appropriate, not harmful, and may be beneficial. The best form of treatment (TRH,TSH,or T3+T4) and possible accompanying treatments (GHRH, Cortisol, nutrition, insulin) lack consensus. In this review current data are laid out for reader’s review and judgment.
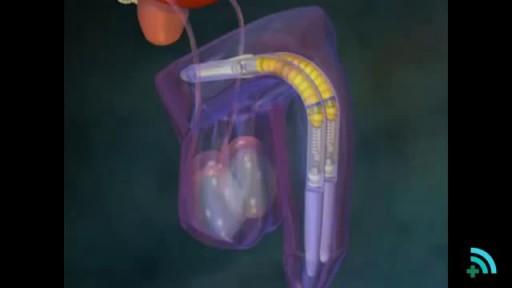
enile implants are devices placed inside the penis to allow men with erectile dysfunction (ED) to get an erection. Penile implants are typically recommended after other treatments for ED fail. There are two main types of penile implants, semirigid and inflatable.
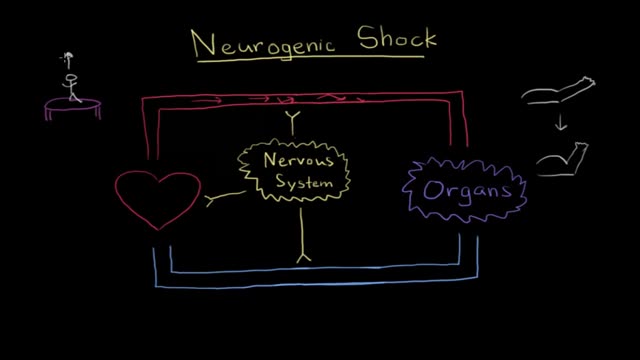
Neurogenic shock is a distributive type of shock resulting in low blood pressure, occasionally with a slowed heart rate, that is attributed to the disruption of the autonomic pathways within the spinal cord. It can occur after damage to the central nervous system such as spinal cord injury.

The Ortolani method is an examination method that identifies a dislocated hip that can be reduced into the socket (acetabulum). Ortolani described the feeling of reduction as a “Hip Click” but the translation from Italian was interpreted a sound instead of a sensation of the hip moving over the edge of the socket when it re-located. After the age of six weeks, this sensation is rarely detectable and should not be confused with snapping that is common and can occur in stable hips when ligaments in and around the hip create clicking noises. When the Ortolani test is positive because the hip is dislocated, treatment is recommended to keep the hip in the socket until stability has been established

Vertigo is a sense of rotation, rocking, or the world spinning, experienced even when someone is perfectly still. Many children attempt to create a sense of vertigo by spinning around for a time; this type of induced vertigo lasts for a few moments and then disappears. In comparison, when vertigo occurs spontaneously or as a result of an injury it tends to last for many hours or even days before resolving.

The vagina is the most delicate and sensitive part of every woman’s body. Naturally female vagina appears to be darker compared to the complexion of other parts of the body. Hence, it is every woman’s dream to have a white complexioned vagina just like their body skin. Most of the women feel that using shop every day may keep their vagina clean and help to make it lighter. But reality is just the opposite. Soaps contain harsh chemicals which not only irritate the delicate skin of vagina and make it darker but they also dis-balance the ph level which plays an important role in maintaining the normal texture of the skin. Well, women need not get disappointed as now there are alternatives of harsh soaps in the market. These alternatives are none other than natural creams which are the best solution to have a naturally fair and glowing vagina without any side effects. Mentioned below are some of the best natural products available in the market to whiten vagina naturally.
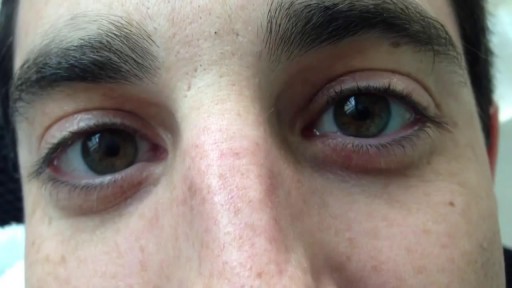
This test stimulates your acoustic nerve by delivering cold or warm water or air into your ear canal. When cold water or air enters your ear and the inner ear changes temperature, it should cause fast, side-to-side eye movements called nystagmus. The test is done in the following way: Before the test, your ear, especially the eardrum, will be checked. This is to make sure it is normal. One ear is tested at a time. A small amount of cold water or air is gently delivered into one of your ears. Your eyes should show an involuntary movement called nystagmus. Then they should turn away from that ear and slowly back. If water is used, it is allowed to drain out of the ear canal. Next, a small amount of warm water or air is gently delivered into the same ear. Again, your eyes should show nystagmus. Then they should turn toward that ear and slowly back. Your other ear is tested in the same way.
Polycythemia vera (pol-e-sigh-THEE-me-uh VEER-uh) is a slow-growing type of blood cancer in which your bone marrow makes too many red blood cells. Polycythemia vera may also result in production of too many of the other types of blood cells — white blood cells and platelets. These excess cells thicken your blood and cause complications, such as such as a risk of blood clots or bleeding. Polycythemia vera isn't common. It usually develops slowly, and you may have it for years without noticing signs or symptoms. Often, polycythemia vera is found during a blood test done for some other reason. Without treatment, polycythemia vera can be life-threatening. However, with proper medical care, many people experience few problems related to this disease. Over time, there's a risk of progressing to more-serious blood cancers, such as myelofibrosis or acute leukemia.
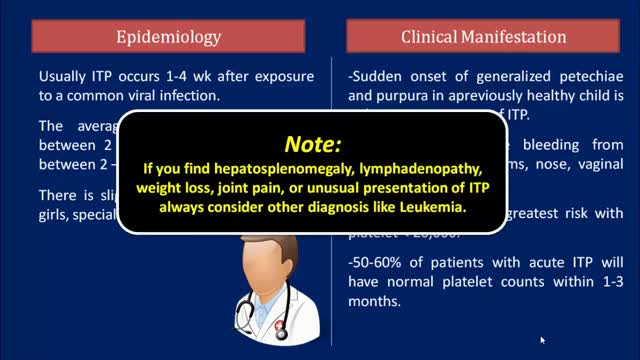
Idiopathic thrombocytopenic purpura (ITP) is a disorder that can lead to easy or excessive bruising and bleeding. The bleeding results from unusually low levels of platelets — the cells that help blood clot. Idiopathic thrombocytopenic purpura, which is also called immune thrombocytopenia, affects children and adults. Children often develop ITP after a viral infection and usually recover fully without treatment. In adults, the disorder is often long term. If you don't have signs of bleeding and your platelet count isn't too low, you may not need any treatment. In rare cases, the number of platelets may be so low that dangerous internal bleeding occurs. Treatment options are available.
A coma is a prolonged state of unconsciousness. During a coma, a person is unresponsive to his or her environment. The person is alive and looks like he or she is sleeping. However, unlike in a deep sleep, the person cannot be awakened by any stimulation, including pain.

Your body's immune system protects you from disease and infection. But if you have an autoimmune disease, your immune system attacks healthy cells in your body by mistake. Autoimmune diseases can affect many parts of the body. No one is sure what causes autoimmune diseases. They do tend to run in families. Women - particularly African-American, Hispanic-American, and Native-American women - have a higher risk for some autoimmune diseases. There are more than 80 types of autoimmune diseases, and some have similar symptoms. This makes it hard for your health care provider to know if you really have one of these diseases, and if so, which one. Getting a diagnosis can be frustrating and stressful. Often, the first symptoms are fatigue, muscle aches and a low fever. The classic sign of an autoimmune disease is inflammation, which can cause redness, heat, pain and swelling. The diseases may also have flare-ups, when they get worse, and remissions, when symptoms get better or disappear. Treatment depends on the disease, but in most cases one important goal is to reduce inflammation. Sometimes doctors prescribe corticosteroids or other drugs that reduce your immune response.