Top videos

The pain is frequently severe and is described as throbbing or pulsating. Nausea is common, and many migraine patients have a watering eye, a running nose, or congestion. If these symptoms are prominent, they may lead to a misdiagnosis of sinus headaches.
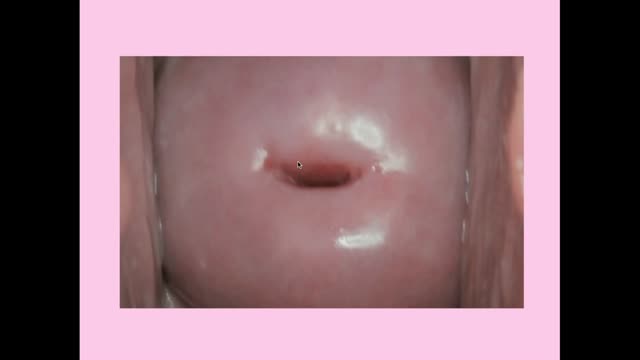
By 5 weeks' gestational age, the wolffian (ie, mesonephric) and the müllerian (ie, paramesonephric) ducts have formed from intermediate mesoderm. In the absence of testosterone and müllerian inhibitory substance, the mesonephric ducts regress and the paramesonephric ducts continue to form the female reproductive structures with fusion of the distal portions of the paramesonephric ducts to give rise to the uterine fundus, the cervix, and the upper vagina. These developmental changes are genetically controlled in large part by a series of complex transcriptional signaling pathways including Wnt signaling, Hox genes, and many others. In a female fetus, the wolffian duct disappears except for nonfunctional vestiges. The müllerian duct is lined by a columnar epithelium. This includes the entire cervix and upper vagina to the vaginal plate (ie, sinovaginal bulb). Through a process of squamous metaplasia, the vagina and a variable portion of the ectocervix become covered with squamous epithelium. This process is complete by the fifth month of pregnancy.

Peritoneal dialysis (per-ih-toe-NEE-ul die-AL-uh-sis) is a way to remove waste products from your blood when your kidneys can no longer do the job adequately. A cleansing fluid flows through a tube (catheter) into part of your abdomen and filters waste products from your blood. After a prescribed period of time, the fluid with filtered waste products flows out of your abdomen and is discarded. Peritoneal dialysis differs from hemodialysis, a more commonly used blood-filtering procedure. With peritoneal dialysis, you can give yourself treatments at home, at work or while traveling. Peritoneal dialysis isn't an option for everyone wit
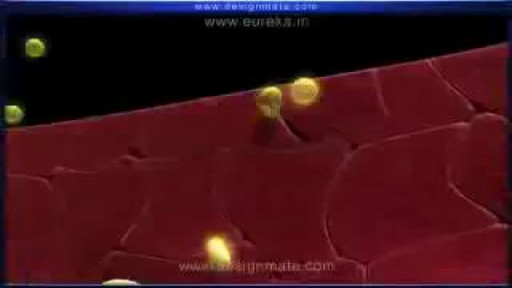
Atherosclerosis is a narrowing of the arteries caused by a buildup of plaque. It’s also called arteriosclerosis or hardening of the arteries. Arteries are the blood vessels that carry oxygen and nutrients from your heart to the rest of your body. As you get older, fat and cholesterol can collect in your arteries and form plaque. The buildup of plaque makes it difficult for blood to flow through your arteries. This buildup may occur in any artery in your body and can result in a shortage of blood and oxygen in various tissues of your body. Pieces of plaque can also break off, causing a blood clot. Atherosclerosis can lead to heart attack, stroke, or heart failure if left untreated.

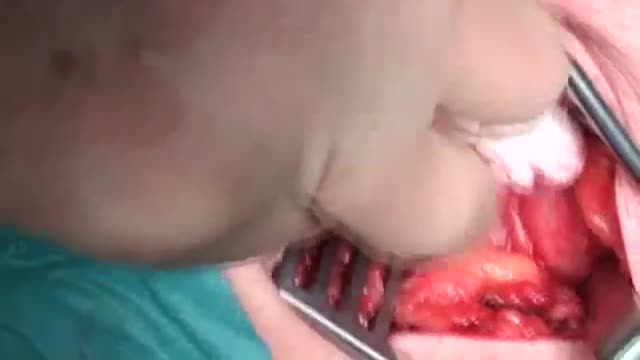
Note: This video contains graphic surgical footage so viewer discretion is advised.
Director of the Penn Orthopaedics Robotics and Navigation Program, Dr. Christopher Travers, discusses robotic joint replacement surgery, which is one of the multiple options that Penn Orthopaedics offers for joint replacement surgery. He walks through a robotic knee replacement surgery, discussing what the procedure is, how it differs from traditional joint replacement surgery, and the benefits.
Refer a patient (physicians only):
https://www.pennmedicine.org/refer-your-patient
Learn more about the Penn Joint Replacement Program:
https://www.pennmedicine.org/f....or-patients-and-visi
Learn more about Dr. Travers:
https://www.pennmedicine.org/providers/profile/christopher-travers?fadf=pennmedicine&keyword=travers
#RoboticSurgery #JointReplacementSurgery #KneeReplacement #SurgicalFootage

Folic acid, which is also called folate, is a B vitamin. The best food sources of folic acid are fortified cereals. Folic acid plays an important role in the production of red blood cells and helps your baby's neural tube develop into her brain and spinal cord.
During surgery to repair the hernia, the bulging tissue is pushed back in. Your abdominal wall is strengthened and supported with sutures (stitches), and sometimes mesh. This repair can be done with open or laparoscopic surgery. You and your surgeon can discuss which type of surgery is right for you.

Goiter treatment depends on the size of the goiter, your signs and symptoms, and the underlying cause. Your doctor may recommend: Observation. If your goiter is small and doesn't cause problems, and your thyroid is functioning normally, your doctor may suggest a wait-and-see approach. Medications. If you have hypothyroidism, thyroid hormone replacement with levothyroxine (Levoxyl, Synthroid, Tirosint) will resolve the symptoms of hypothyroidism as well as slow the release of thyroid-stimulating hormone from your pituitary gland, often decreasing the size of the goiter. For inflammation of your thyroid gland, your doctor may suggest aspirin or a corticosteroid medication to treat the inflammation. For goiters associated with hyperthyroidism, you may need medications to normalize hormone levels. Surgery. Removing all or part of your thyroid gland (total or partial thyroidectomy) is an option if you have a large goiter that is uncomfortable or causes difficulty breathing or swallowing, or in some cases, if you have a nodular goiter causing hyperthyroidism.

Smoking causes: Chronic obstructive pulmonary disease (COPD), a disease that gets worse over time and causes wheezing, shortness of breath, chest tightness, and other symptoms. Emphysema, a condition in which the walls between the air sacs in your lungs lose their ability to stretch and shrink back.

Cameron Underwood Face Transplant Surgical Animation 2018 Eduardo D. Rodriguez, MD, DDS, chair of the Hansjörg Wyss Department of Plastic Surgery, and the Helen L. Kimmel Professor of Reconstructive Plastic Surgery, details the recent face transplant he performed on Cameron Underwood in January 2018 at NYU Langone Health.
Cardioversion takes minutes. The patient is sedated (for a few minutes) and then a shock is delivered. The heart nearly always goes back to regular sinus rhythm. ... Patients without prior ablation or heart surgery rarely develop non-right atrial flutter.

Dehydration can also be a cause of kidney stones. A common symptom is having a lower left abdominal pain, fever, nausea, groin pain and vomiting. Lower left abdominal pain can also be caused by an infection of the kidneys. It usually begins with the bladder and then reaches out to the kidneys.

“People need to realize this is imminently preventable,” he said. Lyme disease develops following an infection with the bacteria Borrelia burgdorferi. It's transmitted to humans through the bite of infected blacklegged ticks. The tick must be attached to its host for 36 to 48 hours to transmit the bacteria.

Papillary fibroelastoma is the third most common primary tumor of the heart and is most likely to involve the cardiac valves. Like myxomas, they arise from the endocardium in most patients and since these tumors are often incidental findings at echocardiography or autopsy, the true incidence is difficult to estimate. Most patients are older than 60 years, which also contrasts with myxomas. Papillary fibroelastomas can embolize, leading to severe neurological complications and therefore, surgical removal is advised, although there is controversy regarding small incidental lesions and the need for surgery.