Top videos
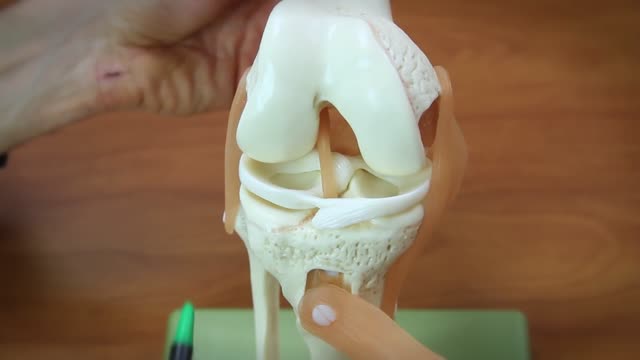
A torn meniscus is one of the most common knee injuries. Any activity that causes you to forcefully twist or rotate your knee, especially when putting your full weight on it, can lead to a torn meniscus. Each of your knees has two menisci — C-shaped pieces of cartilage that act like a cushion between your shinbone and your thighbone. A torn meniscus causes pain, swelling and stiffness. You also might feel a block to knee motion and have trouble extending your knee fully. Conservative treatment — such as rest, ice and medication — is sometimes enough to relieve the pain of a torn meniscus and give the injury time to heal on its own. In other cases, however, a torn meniscus requires surgical repair.

Hold your elbows at shoulder level and place the backs of your hands together with your wrists bent at 90 degrees. This position increases the pressure on the median nerve. If the test reproduces or worsens your symptoms (pain and tingling in your hands), you may have carpal tunnel syndrome.

-MEN1 syndrome is composed of hyperparathyroidism, gastrinoma (pancreatic tumor) and pituitary tum or(remember the 3 Ps). Hyperparathyroidism in MEN1 is caused by hyperplasia of the parathyroid glands. Removal of 3 1/2 glands or total parathyroidectomy with autotransplantation is necessary.
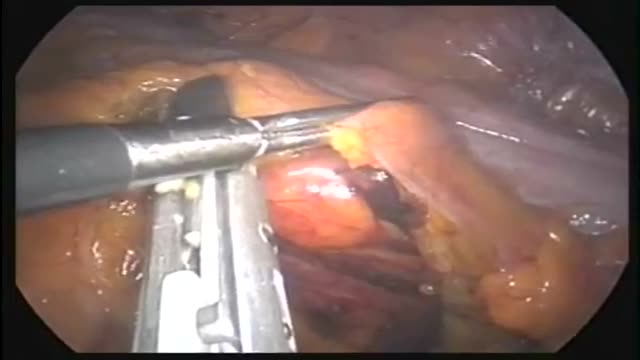
This operation can be performed as an open or laparoscopic (keyhole procedure). During the operation the sigmoid colon is removed. This involves taking away the blood vessels and lymph nodes to that part of the bowel. The surgeon then re-makes the join (anastomosis) between the remaining left side of the colon and the top of the rectum. The surgeon may use either sutures or special staples to make this join.
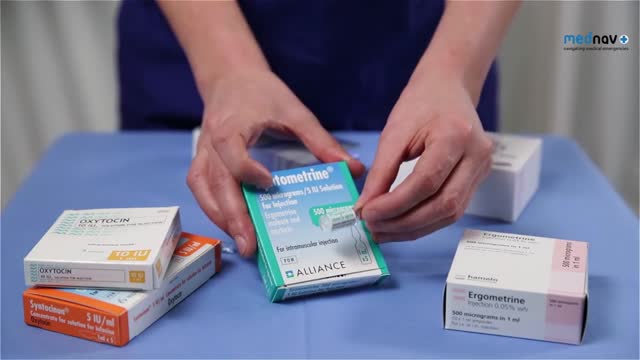
Management of postpartum hemorrhage at vaginal delivery. The approach to treatment of postpartum hemorrhage (PPH) differs somewhat depending on the cause and whether hemorrhage occurs after a vaginal birth or after a cesarean delivery.
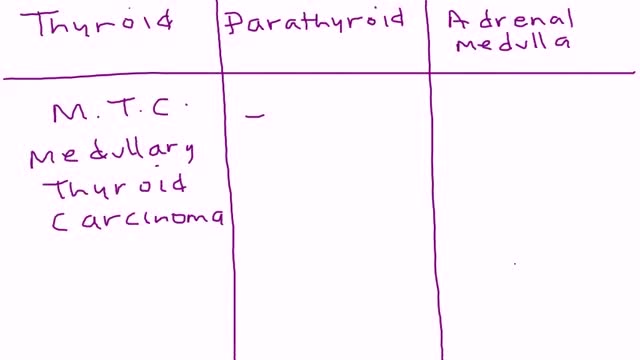
Multiple endocrine neoplasia type 2 (MEN2) (also known as "Pheochromocytoma and amyloid producing medullary thyroid carcinoma", "PTC syndrome," and "Sipple syndrome") is a group of medical disorders associated with tumors of the endocrine system. The tumors may be benign or malignant (cancer).

A C-reactive protein (CRP) test is a blood test that measures the amount of a protein called C-reactive protein in your blood. C-reactive protein measures general levels of inflammation in your body. High levels of CRP are caused by infections and many long-term diseases.
Anaphylaxis is a severe, potentially life-threatening allergic reaction. It can occur within seconds or minutes of exposure to something you're allergic to, such as a peanut or the venom from a bee sting. The flood of chemicals released by your immune system during anaphylaxis can cause you to go into shock; your blood pressure drops suddenly and your airways narrow, blocking normal breathing. Signs and symptoms of anaphylaxis include a rapid, weak pulse, a skin rash, and nausea and vomiting. Common triggers of anaphylaxis include certain foods, some medications, insect venom and latex. Anaphylaxis requires an immediate trip to the emergency department and an injection of epinephrine. If anaphylaxis isn't treated right away, it can lead to unconsciousness or even death.

A brief description of the pathophysiology, clinical features, warning signs, diagnosis and management of Dengue fever. This description is based on the World Health Organisation guidelines of the management of Dengue fever.
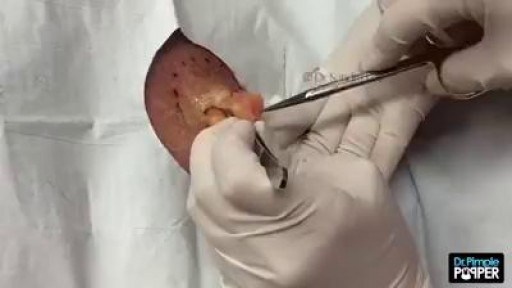
A lipoma is a growth of fat cells in a thin, fibrous capsule usually found just below the skin. Lipomas aren't cancer and don't turn into cancer. They are found most often on the torso, neck, upper thighs, upper arms, and armpits, but they can occur almost anywhere in the body. One or more lipomas may be present at the same time.

Wound healing is the process by which skin or other body tissue repairs itself after trauma. ... This process is divided into predictable phases: blood clotting (hemostasis), inflammation, tissue growth (proliferation) and tissue remodeling (maturation).
A modified radical mastectomy is a procedure in which the entire breast is removed, including the skin, areola, nipple, and most axillary lymph nodes; the pectoralis major muscle is spared. Historically, a modified radical mastectomy was the primary method of treatment of breast cancer. [1, 2] As the treatment of breast cancer evolved, breast conservation has become more widely used. [3, 4] However, mastectomy still remains a viable option for women with breast cancer. [5, 6]