Top videos
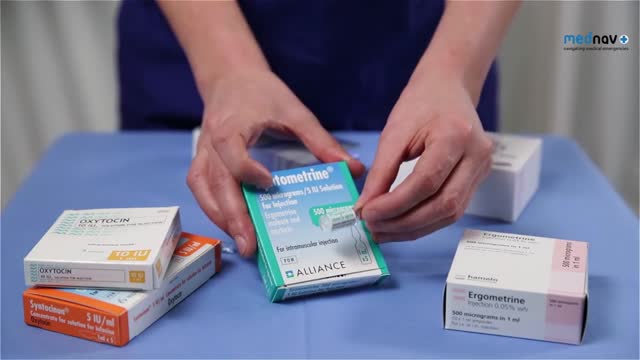
Management of postpartum hemorrhage at vaginal delivery. The approach to treatment of postpartum hemorrhage (PPH) differs somewhat depending on the cause and whether hemorrhage occurs after a vaginal birth or after a cesarean delivery.

Many mothers notice engorgement, or over-filled breasts, at some point or the other while they are breast-feeding their baby and it is especially common to experience when your baby is first born and you are just starting to make milk. So for the first couple of days you make colostrum and then 2-5 days later your milk comes in. And sometimes it comes in with a vengeance and all of the sudden you feel really full and it can be painful and very uncomfortable. Normally your milk supply will even out and start to work well with your babys demand, so it is kind of a supply and demand type of function, but until then, if you feel engorgement, there are a few things you can do to relieve it. If you are nursing your baby on demand this will usually help to self-regulate and most young babies want to eat every 2-3 hours and sometimes even every hour. So, basically, the more often your breasts are emptied the more relief you will feel. But on the same hand, the more you nurse the more milk your body will probably produce. This is why it is good to go off of your babys cues because then you will make what your baby needs and hopefully not much more. But if you are making more than your baby needs and you find that you are still full after feedings you will probably have to either manually express some milk or pump it off, so have a good pump available in case you need to, and if you don't, you can manually express the milk by gently massaging from the armpit down towards the nipple. And you can also try using heat prior to nursing your baby or pumping milk off and this will also help to relax things and help you to get the milk out. Take a warm shower and then feed your baby or use a warm compress.

A C-reactive protein (CRP) test is a blood test that measures the amount of a protein called C-reactive protein in your blood. C-reactive protein measures general levels of inflammation in your body. High levels of CRP are caused by infections and many long-term diseases.
Masturbating is totally healthy, and totally normal. There are tons of myths out there meant to scare you into thinking masturbation is wrong or bad. But the truth is masturbation is perfectly safe. Masturbating won't make you blind, crazy, or stupid. It won’t damage your genitals, cause pimples, or stunt your growth. It doesn’t use up all your orgasms or ruin other kinds of sex. In fact, masturbation can actually be good for you. Here are some benefits of masturbation: Masturbation is safer than any other type of sex. You can’t get pregnant or get any sexually transmitted infections from masturbating. Masturbation can help you learn what you like and don’t like sexually. And if you decide to have sex with someone, you can know what you do/don’t want to do. BONUS: getting comfortable talking about sex and your body with your partner makes it easier to talk about protecting yourself against STDs and pregnancy, too. Exploring your body and learning how to give yourself sexual pleasure can be empowering and help improve your body image. Masturbation can lower stress and help you relax. It even helps some people fall asleep. Having an orgasm releases endorphins — feel good chemicals in your brain. Orgasms can be a natural painkiller and can even help with period cramps. Mutual masturbation (masturbating with a partner) is a really safe way to have sex and let the other person know what feels good to you. If you share a sex toy, use condoms on the toy and clean it before swapping. And if you touch each other’s genitals, wash your hands before touching your own. Can I get an STD from masturbating? Nope. Masturbating is the safest sexual activity out there. There is virtually NO chance of getting an STD or any other infection from touching your own genitals (and there’s also no chance of pregnancy). STDs have to be passed from one person to another, so you can’t give yourself an STD. The one exception to this is herpes - so if you have any cold sores on your mouth and touch them, make sure to wash your hands before masturbating. But it IS possible to get an STD if you’re masturbating with another person and touching each other’s genitals. Anytime semen (cum) or vaginal fluids are spread to someone else’s body, or your genitals rub against each other, there’s a risk of STDs. So if you touch each other’s genitals, wash your hands before touching your own. STDs can also be spread by sharing sex toys with another person. You can help protect yourself by using condoms on any toys that you share (even if they’re not shaped like a penis). Put a new condom on anytime a different person uses it. If you’re the only one using your sex toys, you don’t have to worry about STDs. But if you use them with other people, protect those sex toys just like you’d protect your own genitals — put a condom on ‘em! It’s possible for masturbation to cause irritation or infections if your body is sensitive to the way you masturbate or the things you masturbate with — but this isn’t the same thing as an STD. Lotions, Vaseline, oils, and scented or flavored stuff may irritate your vulva and vagina. Masturbating roughly and not using lubrication can also lead to irritation because of friction. And germs from the anus can cause vaginal infections — so never put something in your vagina that’s been in your butt without washing it or covering it with a condom. If you’re worried that you have an STD because of pain, itching, or discomfort in your genitals, go to your doctor or your local Planned Parenthood health center.

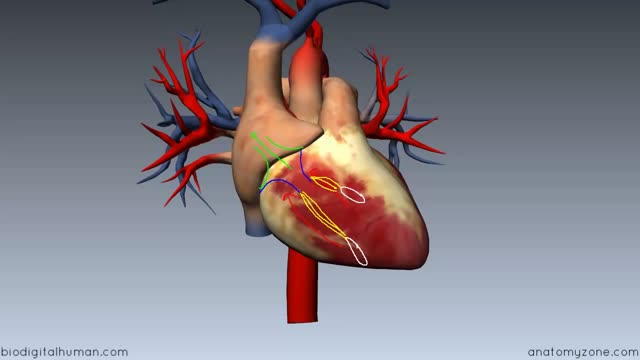
ADH's job is to act on the kidneys to promote water reabsorption. In this lesson, we'll compare and contrast diabetes insipidus, or DI, in which there is too little ADH, and syndrome of inappropriate antidiuretic hormone secretion , or SIADH, in which there is too much ADH.
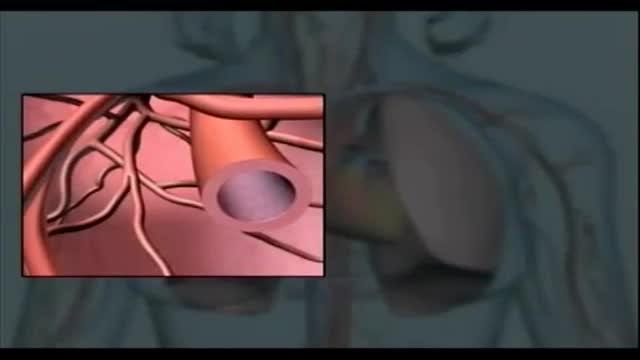
Anaphylaxis is a severe, potentially life-threatening allergic reaction. It can occur within seconds or minutes of exposure to something you're allergic to, such as a peanut or the venom from a bee sting. The flood of chemicals released by your immune system during anaphylaxis can cause you to go into shock; your blood pressure drops suddenly and your airways narrow, blocking normal breathing. Signs and symptoms of anaphylaxis include a rapid, weak pulse, a skin rash, and nausea and vomiting. Common triggers of anaphylaxis include certain foods, some medications, insect venom and latex. Anaphylaxis requires an immediate trip to the emergency department and an injection of epinephrine. If anaphylaxis isn't treated right away, it can lead to unconsciousness or even death.

Wound healing is the process by which skin or other body tissue repairs itself after trauma. ... This process is divided into predictable phases: blood clotting (hemostasis), inflammation, tissue growth (proliferation) and tissue remodeling (maturation).

Liquid Zeolite is one of best natural Zeolite products which is used to remove the cancer cells and tumor. This is helpful to activate P21 tumor gene to remove the tumor. For more information visit our website at http://www.pureliquidzeolite.com/.
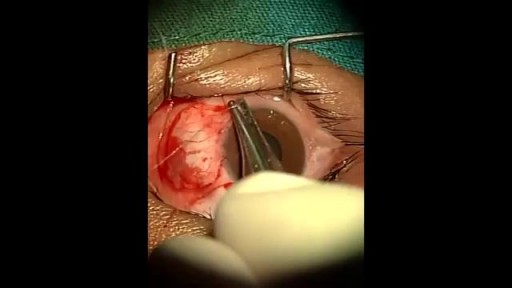
An eye web is a noncancerous, triangular growth that may occur on one or both eyes. It's more common in people who spend a lot of time in the sun, such as those who work outdoors. The painless growth may be slightly raised and contain obvious blood vessels. It may cause irritation and possibly affect vision. Treatment usually isn't necessary. Eyedrops or surgery may help in severe cases.
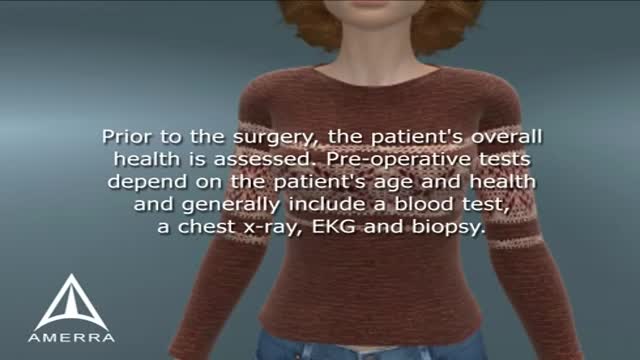
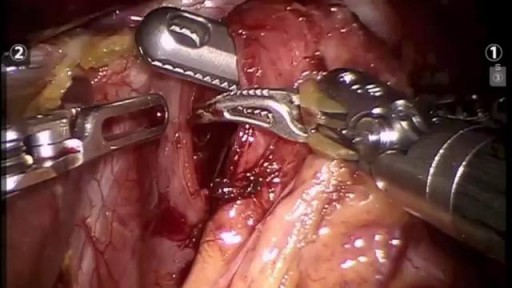
A modified radical mastectomy is a procedure in which the entire breast is removed, including the skin, areola, nipple, and most axillary lymph nodes; the pectoralis major muscle is spared. Historically, a modified radical mastectomy was the primary method of treatment of breast cancer. [1, 2] As the treatment of breast cancer evolved, breast conservation has become more widely used. [3, 4] However, mastectomy still remains a viable option for women with breast cancer. [5, 6]