Top videos

ADH's job is to act on the kidneys to promote water reabsorption. In this lesson, we'll compare and contrast diabetes insipidus, or DI, in which there is too little ADH, and syndrome of inappropriate antidiuretic hormone secretion , or SIADH, in which there is too much ADH.
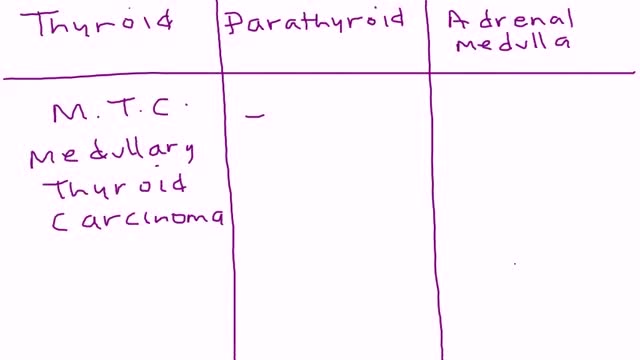
Multiple endocrine neoplasia type 2 (MEN2) (also known as "Pheochromocytoma and amyloid producing medullary thyroid carcinoma", "PTC syndrome," and "Sipple syndrome") is a group of medical disorders associated with tumors of the endocrine system. The tumors may be benign or malignant (cancer).

Hold your elbows at shoulder level and place the backs of your hands together with your wrists bent at 90 degrees. This position increases the pressure on the median nerve. If the test reproduces or worsens your symptoms (pain and tingling in your hands), you may have carpal tunnel syndrome.

Liquid Zeolite is one of best natural Zeolite products which is used to remove the cancer cells and tumor. This is helpful to activate P21 tumor gene to remove the tumor. For more information visit our website at http://www.pureliquidzeolite.com/.
This operation can be performed as an open or laparoscopic (keyhole procedure). During the operation the sigmoid colon is removed. This involves taking away the blood vessels and lymph nodes to that part of the bowel. The surgeon then re-makes the join (anastomosis) between the remaining left side of the colon and the top of the rectum. The surgeon may use either sutures or special staples to make this join.
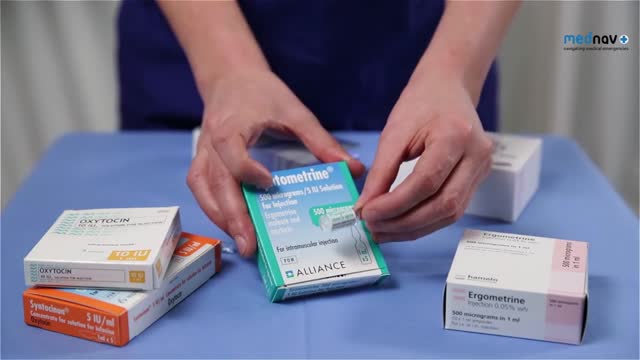
Management of postpartum hemorrhage at vaginal delivery. The approach to treatment of postpartum hemorrhage (PPH) differs somewhat depending on the cause and whether hemorrhage occurs after a vaginal birth or after a cesarean delivery.

A C-reactive protein (CRP) test is a blood test that measures the amount of a protein called C-reactive protein in your blood. C-reactive protein measures general levels of inflammation in your body. High levels of CRP are caused by infections and many long-term diseases.

A fractured rib is usually a result of a fall or accident. Prolonged coughing and sports with repetitive movement, such as golf, also can cause a rib fracture. Symptoms include pain when taking a deep breath, pressing on the injured area, or bending or twisting the body. In most cases, fractured ribs usually heal on their own in one or two months. Pain relievers can make it easier to breathe deeply.
Anaphylaxis is a severe, potentially life-threatening allergic reaction. It can occur within seconds or minutes of exposure to something you're allergic to, such as a peanut or the venom from a bee sting. The flood of chemicals released by your immune system during anaphylaxis can cause you to go into shock; your blood pressure drops suddenly and your airways narrow, blocking normal breathing. Signs and symptoms of anaphylaxis include a rapid, weak pulse, a skin rash, and nausea and vomiting. Common triggers of anaphylaxis include certain foods, some medications, insect venom and latex. Anaphylaxis requires an immediate trip to the emergency department and an injection of epinephrine. If anaphylaxis isn't treated right away, it can lead to unconsciousness or even death.

Wound healing is the process by which skin or other body tissue repairs itself after trauma. ... This process is divided into predictable phases: blood clotting (hemostasis), inflammation, tissue growth (proliferation) and tissue remodeling (maturation).
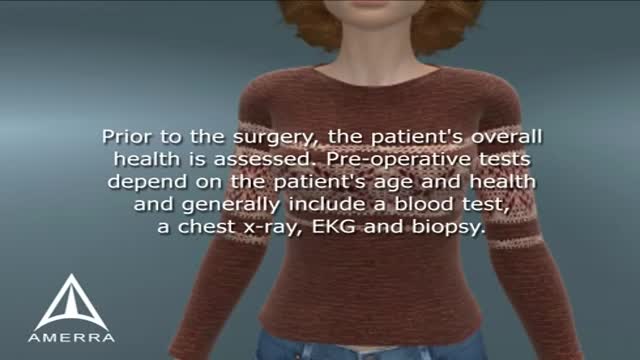
A modified radical mastectomy is a procedure in which the entire breast is removed, including the skin, areola, nipple, and most axillary lymph nodes; the pectoralis major muscle is spared. Historically, a modified radical mastectomy was the primary method of treatment of breast cancer. [1, 2] As the treatment of breast cancer evolved, breast conservation has become more widely used. [3, 4] However, mastectomy still remains a viable option for women with breast cancer. [5, 6]
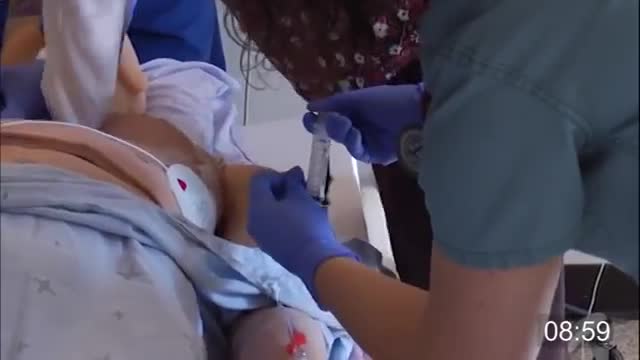
Technically, there's no formal definition for a "Code", but doctors often use the term as slang for a cardiopulmonary arrest happening to a patient in a hospital or clinic, requiring a team of providers (sometimes called a "code team") to rush to the specific location and begin immediate resuscitative efforts.