Top videos

A man's age matters. As men get older, the chances of conceiving and having a healthy child decline. Male fertility starts to decline after 40 when sperm quality decreases. This means it takes longer for their partners to conceive and when they do, there's an increased risk of miscarriage.

Hold your elbows at shoulder level and place the backs of your hands together with your wrists bent at 90 degrees. This position increases the pressure on the median nerve. If the test reproduces or worsens your symptoms (pain and tingling in your hands), you may have carpal tunnel syndrome.
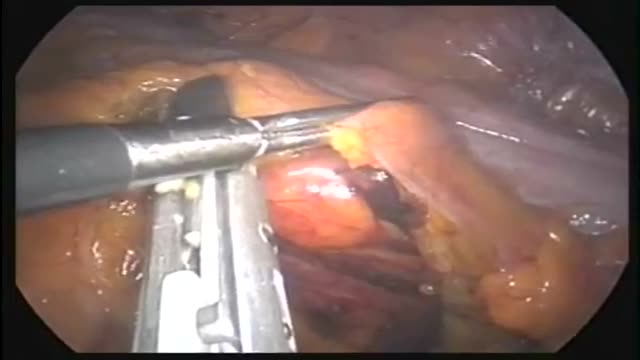
This operation can be performed as an open or laparoscopic (keyhole procedure). During the operation the sigmoid colon is removed. This involves taking away the blood vessels and lymph nodes to that part of the bowel. The surgeon then re-makes the join (anastomosis) between the remaining left side of the colon and the top of the rectum. The surgeon may use either sutures or special staples to make this join.
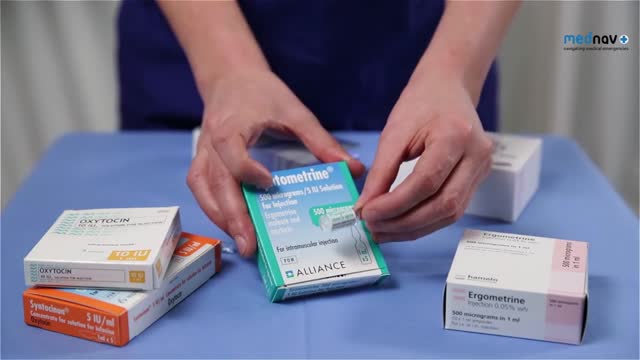
Management of postpartum hemorrhage at vaginal delivery. The approach to treatment of postpartum hemorrhage (PPH) differs somewhat depending on the cause and whether hemorrhage occurs after a vaginal birth or after a cesarean delivery.

A fractured rib is usually a result of a fall or accident. Prolonged coughing and sports with repetitive movement, such as golf, also can cause a rib fracture. Symptoms include pain when taking a deep breath, pressing on the injured area, or bending or twisting the body. In most cases, fractured ribs usually heal on their own in one or two months. Pain relievers can make it easier to breathe deeply.

A C-reactive protein (CRP) test is a blood test that measures the amount of a protein called C-reactive protein in your blood. C-reactive protein measures general levels of inflammation in your body. High levels of CRP are caused by infections and many long-term diseases.
Anaphylaxis is a severe, potentially life-threatening allergic reaction. It can occur within seconds or minutes of exposure to something you're allergic to, such as a peanut or the venom from a bee sting. The flood of chemicals released by your immune system during anaphylaxis can cause you to go into shock; your blood pressure drops suddenly and your airways narrow, blocking normal breathing. Signs and symptoms of anaphylaxis include a rapid, weak pulse, a skin rash, and nausea and vomiting. Common triggers of anaphylaxis include certain foods, some medications, insect venom and latex. Anaphylaxis requires an immediate trip to the emergency department and an injection of epinephrine. If anaphylaxis isn't treated right away, it can lead to unconsciousness or even death.
o you have an exercise routine that makes you feel absolutely awesome when you stick to it? Or a healthy eating pattern that makes you crackle with energy and vitality when you actually follow it. Well, today I’m sharing with you what makes me feel even more alive, energetic and vibrant than both of those… My daily sexual self-care practice.

Wound healing is the process by which skin or other body tissue repairs itself after trauma. ... This process is divided into predictable phases: blood clotting (hemostasis), inflammation, tissue growth (proliferation) and tissue remodeling (maturation).

Methotrexate works by reducing the function of the cells that are causing inflammation in the joint tissues. "Its use can reduce inflammation and therefore should help relieve pain and protect from joint damage," notes Sean A. Whelton, MD, a rheumatologist and associate professor of medicine at MedStar Georgetown University Hospital in Washington, D.C. Less inflammation in the joints should mean less joint pain and less joint swelling. You should also feel less fatigue and less morning stiffness.
A modified radical mastectomy is a procedure in which the entire breast is removed, including the skin, areola, nipple, and most axillary lymph nodes; the pectoralis major muscle is spared. Historically, a modified radical mastectomy was the primary method of treatment of breast cancer. [1, 2] As the treatment of breast cancer evolved, breast conservation has become more widely used. [3, 4] However, mastectomy still remains a viable option for women with breast cancer. [5, 6]
Technically, there's no formal definition for a "Code", but doctors often use the term as slang for a cardiopulmonary arrest happening to a patient in a hospital or clinic, requiring a team of providers (sometimes called a "code team") to rush to the specific location and begin immediate resuscitative efforts.

You can now test your knowledge with a free lesson quiz on NURSING.com!
Click here for your free quiz: https://bit.ly/3Jcl93Z
Tracheostomy Suctioning- Nursing Skills
FREE Nursing School Cheat Sheets at: http://www.NURSING.com
Get the full lesson on Trach Suctioning here:
https://nursing.com/lesson/ski....lls-03-03-trach-suct
Get Access to Thousands of Lessons here:
https://nursing.com/courses/
Welcome to the NURSING Family, we call it the most supportive nursing cohort on the planet.
At NURSING.com, we want to help you remove the stress and overwhelm of nursing school so that you can focus on becoming an amazing nurse.
Check out our freebies and learn more at: (http://www.nursing.com)
Tracheostomy Suctioning- Nursing Skills:
In this video we’re going to talk about suctioning a tracheostomy. You may need to do this before you do trach care or just because the patient requires suctioning. Make sure that you assess the patient before you start so that you know what their one sounds are, and what their oxygen saturation is. We love you guys! Go out and be your best selves today! And, as always, happy nursing!
Bookmarks:
0.05 Introduction to trach suctioning
0:21 Suction setup
0:42 Opening suction kit
1:55 Sterile water
2:13 Starting trach suctioning
2:00 Catheter insertion
3:00 Catheter pass #2
3:26 Listen to lungs
3:31 Outro
Visit us at https://nursing.com/medical-disclaimer/ for disclaimer information.
NCLEX®, NCLEX-RN® are registered trademarks of the National Council of State Boards of Nursing, INC. and hold no affiliation with NURSING.com.