Top videos
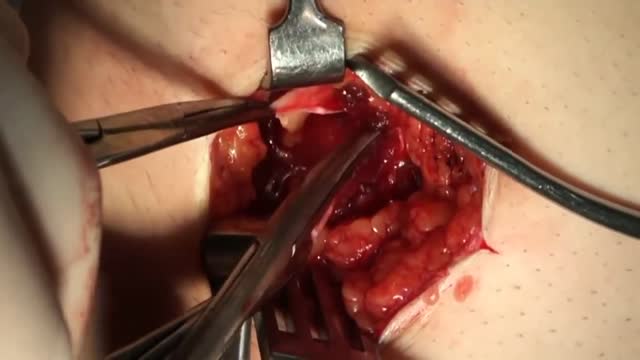
An appendectomy (sometimes called appendisectomy or appendicectomy) is the surgical removal of the vermiform appendix. This procedure is normally performed as an emergency procedure, when the patient is suffering from acute appendicitis.

For open hernia repair surgery, a single long incision is made in the groin. If the hernia is bulging out of the abdominal wall (a direct hernia), the bulge is pushed back into place. If the hernia is going down the inguinal canal (indirect), the hernia sac is either pushed back or tied off and removed.

Urological surgeons have become proficient at performing complex pelvic urological procedures, such as radical prostatectomy, using the laparoscopic approach. Declan Murphy and Daniel Moon share their experience of four less common procedures they have performed recently using laparoscopic techniques. These include: excision of a urachal cyst; partial cystectomy for endometriosis (combined endoscopic-laparoscopic approach); repair of an intra-peritoneal bladder rupture; and repair of a ureteric injury (combined endoscopic-laparoscopic approach).

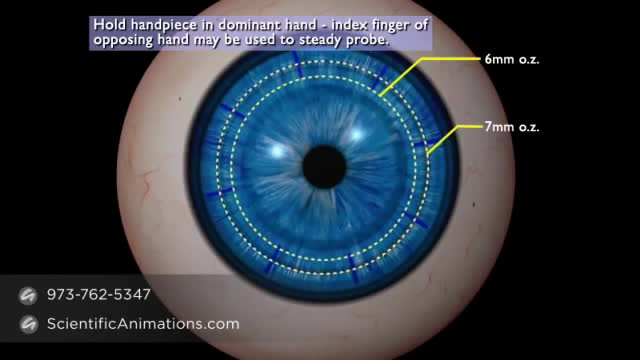
Nystagmus is a condition of involuntary (or voluntary, in rare cases) eye movement, acquired in infancy or later in life, that may result in reduced or limited vision. Due to the involuntary movement of the eye, it has been called "dancing eyes"
Treatment for kidney stones varies, depending on the type of stone and the cause. Small stones with minimal symptoms Most kidney stones won't require invasive treatment. You may be able to pass a small stone by: Drinking water. Drinking as much as 2 to 3 quarts (1.9 to 2.8 liters) a day may help flush out your urinary system. Unless your doctor tells you otherwise, drink enough fluid — mostly water — to produce clear or nearly clear urine. Pain relievers. Passing a small stone can cause some discomfort. To relieve mild pain, your doctor may recommend pain relievers such as ibuprofen (Advil, Motrin IB, others), acetaminophen (Tylenol, others) or naproxen sodium (Aleve). Medical therapy. Your doctor may give you a medication to help pass your kidney stone. This type of medication, known as an alpha blocker, relaxes the muscles in your ureter, helping you pass the kidney stone more quickly and with less pain. Large stones and those that cause symptoms Kidney stones that can't be treated with conservative measures — either because they're too large to pass on their own or because they cause bleeding, kidney damage or ongoing urinary tract infections — may require more extensive treatment. Procedures may include: Using sound waves to break up stones. For certain kidney stones — depending on size and location — your doctor may recommend a procedure called extracorporeal shock wave lithotripsy (ESWL). ESWL uses sound waves to create strong vibrations (shock waves) that break the stones into tiny pieces that can be passed in your urine. The procedure lasts about 45 to 60 minutes and can cause moderate pain, so you may be under sedation or light anesthesia to make you comfortable. ESWL can cause blood in the urine, bruising on the back or abdomen, bleeding around the kidney and other adjacent organs, and discomfort as the stone fragments pass through the urinary tract. Surgery to remove very large stones in the kidney. A procedure called percutaneous nephrolithotomy (nef-row-lih-THOT-uh-me) involves surgically removing a kidney stone using small telescopes and instruments inserted through a small incision in your back. You will receive general anesthesia during the surgery and be in the hospital for one to two days while you recover. Your doctor may recommend this surgery if ESWL was unsuccessful. Using a scope to remove stones. To remove a smaller stone in your ureter or kidney, your doctor may pass a thin lighted tube (ureteroscope) equipped with a camera through your urethra and bladder to your ureter. Once the stone is located, special tools can snare the stone or break it into pieces that will pass in your urine. Your doctor may then place a small tube (stent) in the ureter to relieve swelling and promote healing. You may need general or local anesthesia during this procedure. Parathyroid gland surgery. Some calcium phosphate stones are caused by overactive parathyroid glands, which are located on the four corners of your thyroid gland, just below your Adam's apple. When these glands produce too much parathyroid hormone (hyperparathyroidism), your calcium levels can become too high and kidney stones may form as a result. Hyperparathyroidism sometimes occurs when a small, benign tumor forms in one of your parathyroid glands or you develop another condition that leads these glands to produce more parathyroid hormone. Removing the growth from the gland stops the formation of kidney stones. Or your doctor may recommend treatment of the condition that's causing your parathyroid gland to overproduce the hormone.
The accumulation of ascitic fluid represents a state of total-body sodium and water excess, but the event that initiates the unbalance is unclear. Although many pathogenic processes have been implicated in the development of abdominal ascites, about 75% likely occur as a result of portal hypertension in the setting of liver cirrhosis, with the remainder due to infective, inflammatory, and infiltrative conditions. Three theories of ascites formation have been proposed: underfilling, overflow, and peripheral arterial vasodilation. The underfilling theory suggests that the primary abnormality is inappropriate sequestration of fluid within the splanchnic vascular bed due to portal hypertension and a consequent decrease in effective circulating blood volume. This activates the plasma renin, aldosterone, and sympathetic nervous system, resulting in renal sodium and water retention. The overflow theory suggests that the primary abnormality is inappropriate renal retention of sodium and water in the absence of volume depletion. This theory was developed in accordance with the observation that patients with cirrhosis have intravascular hypervolemia rather than hypovolemia. The most recent theory, the peripheral arterial vasodilation hypothesis, includes components of both of the other theories. It suggests that portal hypertension leads to vasodilation, which causes decreased effective arterial blood volume. As the natural history of the disease progresses, neurohumoral excitation increases, more renal sodium is retained, and plasma volume expands. This leads to overflow of fluid into the peritoneal cavity. The vasodilation theory proposes that underfilling is operative early and overflow is operative late in the natural history of cirrhosis. Although the sequence of events that occurs between the development of portal hypertension and renal sodium retention is not entirely clear, portal hypertension apparently leads to an increase in nitric oxide levels. Nitric oxide mediates splanchnic and peripheral vasodilation. Hepatic artery nitric oxide synthase activity is greater in patients with ascites than in those without ascites. Regardless of the initiating event, a number of factors contribute to the accumulation of fluid in the abdominal cavity. Elevated levels of epinephrine and norepinephrine are well-documented factors. Hypoalbuminemia and reduced plasma oncotic pressure favor the extravasation of fluid from the plasma to the peritoneal fluid, and, thus, ascites is infrequent in patients with cirrhosis unless both portal hypertension and hypoalbuminemia are present.
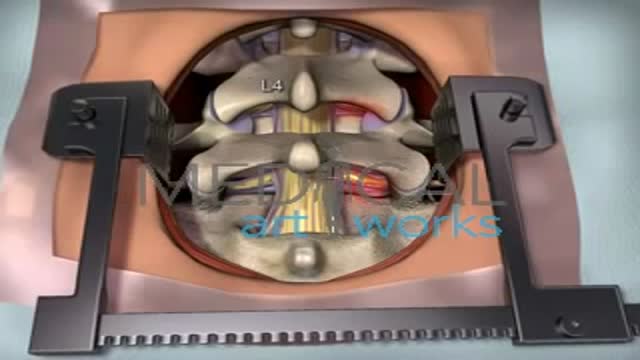
The goal of a decompression surgery is usually to relieve pain caused by nerve root pinching. There are two common causes of lumbar nerve root pressure: from a lumbar herniated disc or lumbar spinal stenosis. This type of pain is usually referred to as a radiculopathy, or sciatica. A decompression surgery involves removing a small portion of the bone over the nerve root and/or disc material from under the nerve root to relieve pinching of the nerve and provide more room for the nerve to heal. The most common types of decompression surgery are microdiscectomy and laminectomy.

Ovarian dermoid cyst and mature cystic ovarian teratoma are terms often used interchangeably to refer to the most common ovarian neoplasm. These slow-growing tumours contain elements from multiple germ cell layers and are best assessed with ultrasound.