Top videos

plantar fasciitis and calcaneal spur can be treated by EPFR with calcanean drilling - endoscopic plantar fascia release علاج الشوكة العظمية للكعب بالمنظار د. أسامة الشاذلي مدرس جراحة العظام واستشاري جراحات و مناظير القدم والكاحل كلية الطب جامعة عين شمس

Thalassemia (thal-uh-SEE-me-uh) is an inherited blood disorder characterized by less hemoglobin and fewer red blood cells in your body than normal. Several types of thalassemia exist, including alpha-thalassemia, beta-thalassemia intermedia, Cooley's anemia and Mediterranean anemia. Hemoglobin is the substance in your red blood cells that allows them to carry oxygen. The low hemoglobin and fewer red blood cells of thalassemia may cause anemia, leaving you fatigued. If you have mild thalassemia, you may not need treatment. But, if you have a more severe form of thalassemia, you may need regular blood transfusions. You can also take steps on your own to cope with fatigue, such as choosing a healthy diet and exercising regularly.
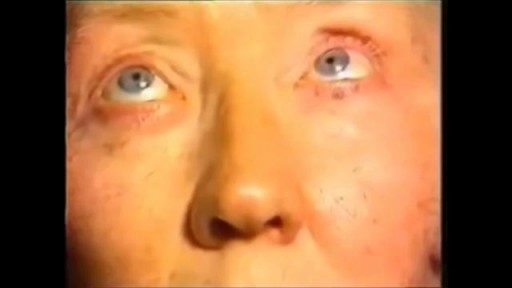
Nystagmus is a vision condition in which the eyes make repetitive, uncontrolled movements. These movements often result in reduced vision and depth perception and can affect balance and coordination. These involuntary eye movements can occur from side to side, up and down, or in a circular pattern.

Medications are the most proven, effective way to treat gout symptoms. However, making certain lifestyle changes also may help, such as: Limiting alcoholic beverages and drinks sweetened with fruit sugar (fructose). Instead, drink plenty of nonalcoholic beverages, especially water. Limit intake of foods high in purines, such as red meat, organ meats and seafood. Exercising regularly and losing weight. Keeping your body at a healthy weight reduces your risk of gout.

Symptoms of liver failure include vomiting, diarrhea and fatigue as well as the symptoms from stage 3. While the progression from cirrhosis to failure can take years, the damage is irreversible and leads to eventual death. The key to treating liver disease is to diagnose the condition as early as possible.

Prinzmetal's or Prinzmetal angina (/ˈprɪntsmɛtəl/, sounds like "prints metal") (also known as variant angina, vasospastic angina (VSA), angina inversa, or coronary vessel spasm) is a syndrome typically consisting of angina (cardiac chest pain) at rest that occurs in cycles.

An abdominal aortic aneurysm is an enlarged area in the lower part of the aorta, the major blood vessel that supplies blood to the body. The aorta, about the thickness of a garden hose, runs from your heart through the center of your chest and abdomen. Because the aorta is the body's main supplier of blood, a ruptured abdominal aortic aneurysm can cause life-threatening bleeding. Depending on the size and the rate at which your abdominal aortic aneurysm is growing, treatment may vary from watchful waiting to emergency surgery. Once an abdominal aortic aneurysm is found, doctors will closely monitor it so that surgery can be planned if it's necessary. Emergency surgery for a ruptured abdominal aortic aneurysm can be risky.
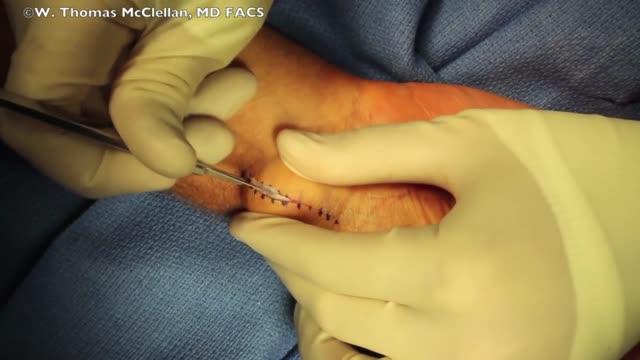
Ganglion cysts are noncancerous lumps that most commonly develop along the tendons or joints of your wrists or hands. They also may occur in the ankles and feet. Ganglion cysts are typically round or oval and are filled with a jellylike fluid. Small ganglion cysts can be pea-sized, while larger ones can be around an inch (2.5 centimeters) in diameter. Ganglion cysts can be painful if they press on a nearby nerve. Their location can sometimes interfere with joint movement. If your ganglion cyst is causing you problems, your doctor may suggest trying to drain the cyst with a needle. Removing the cyst surgically also is an option. But if you have no symptoms, no treatment is necessary. In many cases, the cysts go away on their own.
The cardiac cycle is the sequence of events that occurs when the heart beats. As the heart beats, it circulates blood through pulmonary and systemic circuits of the body. There are two phases of the cardiac cycle. In the diastole phase, the heart ventricles are relaxed and the heart fills with blood

Pain in joints or any part of body is very unpleasant and annoying experience. It is very common in people those suffering from arthritis. To get an end to all such pains, one can start using Generic Celebrex ( https://www.medexpressrx.com/celebrex-generic.aspx ). Here is a brief detail about this wonderful painkiller.
Intra-abdominal abscess continues to be an important and serious problem in surgical practice. Appropriate treatment is often delayed because of the obscure nature of many conditions resulting in abscess formation, which can make diagnosis and localization difficult. Associated pathophysiologic effects may become life threatening or lead to extended periods of morbidity with prolonged hospitalization. Delayed diagnosis and treatment can also lead to increased mortality; therefore, the economic impact of delaying treatment is significant.

complications from using a urinary catheter include: allergic reaction to the material used in the catheter, such as latex. bladder stones. blood in the urine. injury to the urethra. kidney damage (with long-term indwelling catheters) septicemia, or infection of the urinary tract, kidneys, or blood.

DOING LESS BUT BRAINY DESCRIBES A NEW GENERATION OF IMMEDIATE ZIRCONIA IMPLANTS ANATOMICAL AND CUSTOM-MADE. YOUR DENTAL ROOT IS MILLED IN ZIRCONIA AND IN 20 SECONDS SEATED, NO DRILLING, NO AUGMENTATION, NO MEMBRANES, FLAPLESS, NO 3D PLANNING, NO CAD/CAM SPLINTS OR GUIDED SURGERY REQUIRED! EASY AND CONSEQUENTIAL SYSTEM. NO MORE INCONGRUOUS AND UGLY SILVER-COLORED TITANIUM IMPLANTS IN TIME CONSUMING, PAINFUL AND COSTLY PROCEDURES. IT`S HIGH TIME TO RESPECT THE ANATOMY NOT ALTER IT BY DRILLING AND AUGMENTATION. BIOIMPLANT