Top videos
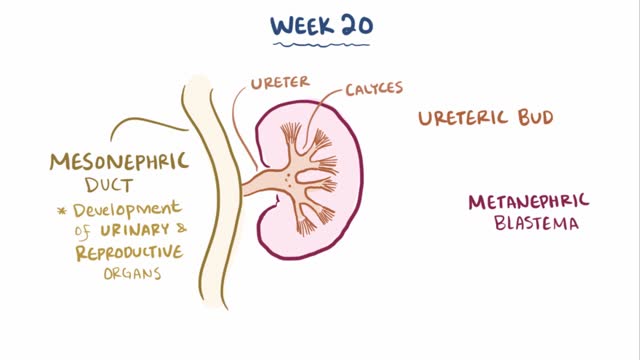
Multicystic dysplastic kidney (MCDK) is a condition that results from the malformation of the kidney during fetal development. The kidney consists of irregular cysts of varying sizes. Multicystic dysplastic kidney is a common type of renal cystic disease, and it is a cause of an abdominal mass in infants.

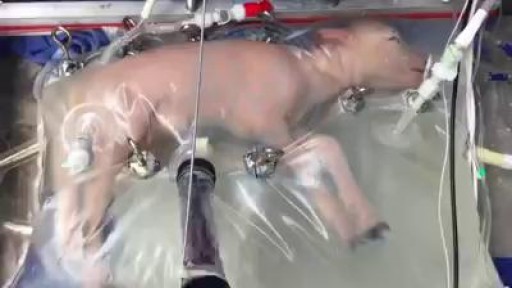
What is hemodiafiltration? Hemodiafiltration, or HDF, is a renal replacement modality that combines diffusion and convection to improve removal of molecules in the middle molecular weight range versus hemodialysis.
Find our full video library only on Osmosis Prime: http://osms.it/more.
Join over 3 million current & future clinicians who learn by Osmosis, and over 130 universities around the world who partner with us to make medical and health education more engaging and efficient. We have unparalleled tools and materials to prepare you to succeed in school, on board exams, and as a future clinician. Sign up for a free trial at http://osms.it/more. If you're interested in exploring an institutional partnership, visit osmosis.org/educators to request a personalized demo.
Follow us on social:
Facebook: http://osms.it/facebook
Twitter: http://osms.it/twitter
Instagram for med: http://osms.it/instagram
Instagram for nursing: https://osms.it/ignursing
Linkedin: https://osms.it/linkedin
Our Vision: Everyone who cares for someone will learn by Osmosis.
Our Mission: To empower the world’s clinicians and caregivers with the best learning experience possible. Learn more here: http://osms.it/mission
Medical disclaimer: Knowledge Diffusion Inc (DBA Osmosis) does not provide medical advice. Osmosis and the content available on Osmosis's properties (Osmosis.org, YouTube, and other channels) do not provide a diagnosis or other recommendation for treatment and are not a substitute for the professional judgment of a healthcare professional in diagnosis and treatment of any person or animal. The determination of the need for medical services and the types of healthcare to be provided to a patient are decisions that should be made only by a physician or other licensed health care provider. Always seek the advice of a physician or other qualified healthcare provider with any questions you have regarding a medical condition. © 2023 Elsevier. All rights reserved.

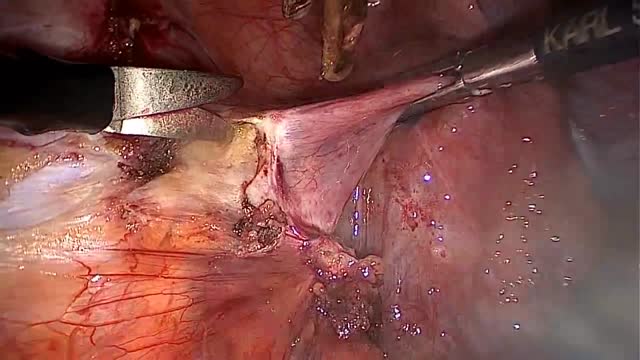
Ovarian dermoid cyst and mature cystic ovarian teratoma are terms often used interchangeably to refer to the most common ovarian neoplasm. These slow-growing tumours contain elements from multiple germ cell layers and are best assessed with ultrasound.
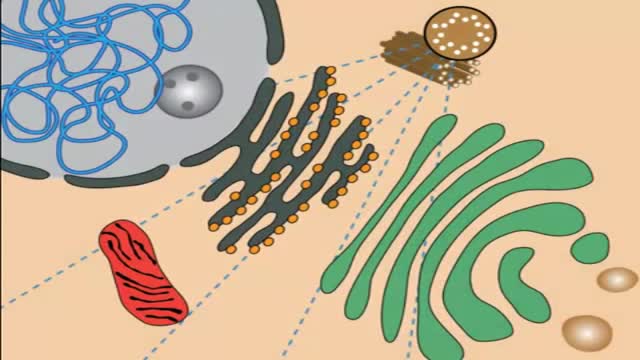
Lysosomal storage diseases (LSDs; /ˌlaɪsəˈsoʊməl/) are a group of approximately 50 rare inherited metabolic disorders that result from defects in lysosomal function. Lysosomes are sacs of enzymes within cells that digest large molecules and pass the fragments on to other parts of the cell for recycling.
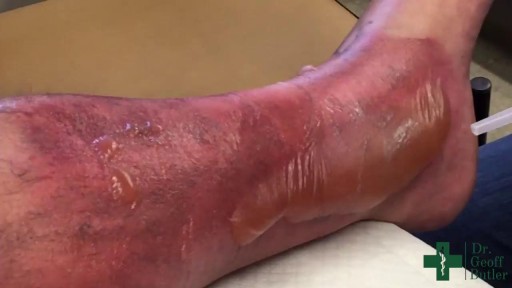
A bulla is a fluid-filled sac or lesion that appears when fluid is trapped under a thin layer of your skin. It’s a type of blister. Bullae (pronounced as “bully”) is the plural word for bulla. To be classified as a bulla, the blister must be larger than 0.5 centimeters (5 millimeters) in diameter. Smaller blisters are called vesicles.
Diagnosis of HIV infection in infants is aided by HIV culture or DNA/RNA polymerase chain reaction (PCR); positive results are confirmed by repeating the test. In suspected cases, HIV testing should occur in the newborn period (ie, before the infant is 48 h old), at age 1-2 months, and again at age 3-6 months.
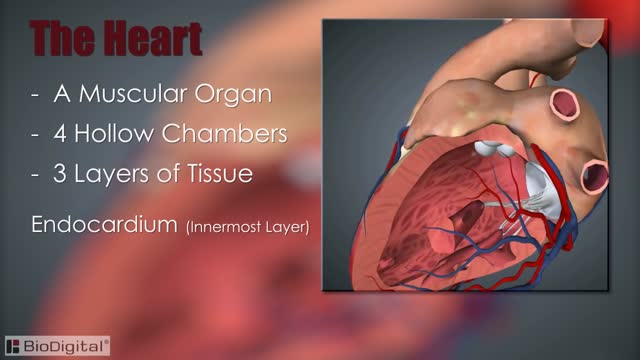
The heart, blood vessels, and blood are the parts that make up the circulatory system, which is defined as a closed system of blood vessels for the transport of gasses and nutrients. The heart is the key organ in the circulatory system. As a hollow, muscular pump, its main function is to propel blood throughout the body.