Top videos
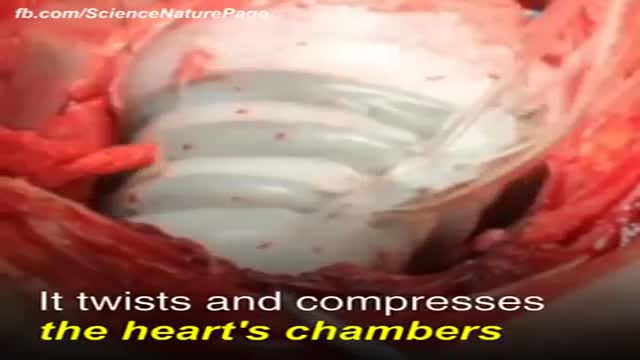
Restrictive cardiomyopathy (RCM) is a rare form of heart muscle disease that is characterized by restrictive filling of the ventricles. In this disease the contractile function (squeeze) of the heart and wall thicknesses are usually normal, but the relaxation or filling phase of the heart is very abnormal.

Insert the needle into the rubber stopper of the insulin bottle. Push the plunger down to inject air into the bottle (this allows the insulin to be drawn more easily). Leave the needle in the bottle. Turn the bottle and syringe upside-down.
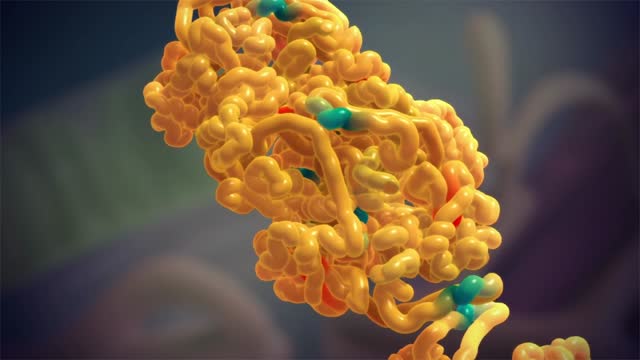
Amyloidosis (am-uh-loi-DO-sis) is a rare disease that occurs when a substance called amyloid builds up in your organs. Amyloid is an abnormal protein that is usually produced in your bone marrow and can be deposited in any tissue or organ. Amyloidosis can affect different organs in different people, and there are different types of amyloid. Amyloidosis frequently affects the heart, kidneys, liver, spleen, nervous system and digestive tract. Severe amyloidosis can lead to life-threatening organ failure.
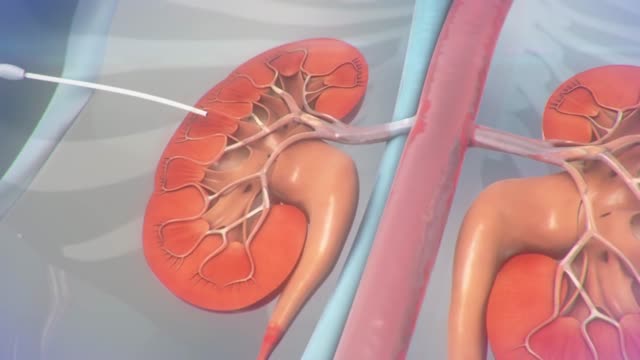
A ureteral stent is a thin, hollow tube that is placed in the ureter to help urine pass from the kidney into the bladder. Ureters are the tubes that connect the kidneys to the bladder. You may have a small amount of blood in your urine for 1 to 3 days after the procedure.
To remove a smaller stone in your ureter or kidney, your doctor may pass a thin lighted tube (ureteroscope) equipped with a camera through your urethra and bladder to your ureter. Once the stone is located, special tools can snare the stone or break it into pieces that will pass in your urine.
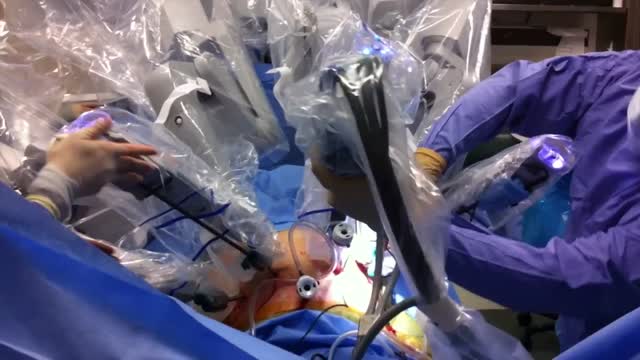
Endometrial cancer is a type of cancer that begins in the uterus. The uterus is the hollow, pear-shaped pelvic organ in women where fetal development occurs. Endometrial cancer begins in the layer of cells that form the lining (endometrium) of the uterus. Endometrial cancer is sometimes called uterine cancer. Other types of cancer can form in the uterus, including uterine sarcoma, but they are much less common than endometrial cancer. Endometrial cancer is often detected at an early stage because it frequently produces abnormal vaginal bleeding, which prompts women to see their doctors. If endometrial cancer is discovered early, removing the uterus surgically often cures endometrial cancer.

The deep veins play a significant role in propelling blood toward the heart. The one-way valves in deep veins prevent blood from flowing backward, and the muscles surrounding the deep veins compress them, helping force the blood toward the heart, just as squeezing a toothpaste tube ejects toothpaste.

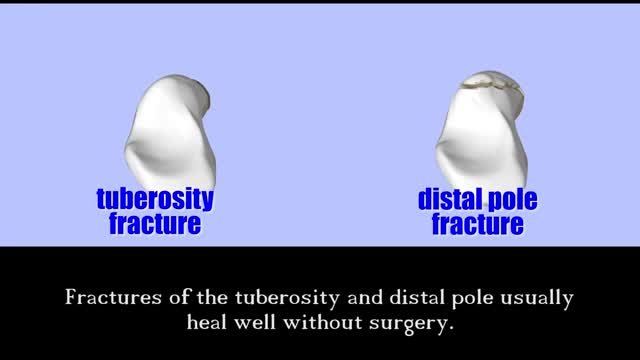
Ankle fusion (arthrodesis) This is a surgical procedure which joins together the main bones of the ankle joint (the tibia and the talus). However, depending on the technique your surgeon will use, occasionally the fibula will be included in this procedure. The two joint surfaces which generate the pain are removed.
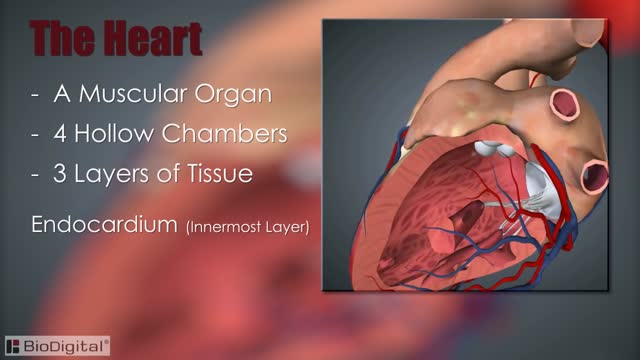
The heart, blood vessels, and blood are the parts that make up the circulatory system, which is defined as a closed system of blood vessels for the transport of gasses and nutrients. The heart is the key organ in the circulatory system. As a hollow, muscular pump, its main function is to propel blood throughout the body.
How to use a Hepatitis B rapid test kit for self-diagnosis of Hepatitis B (fingerstick blood). Convenient, Easy to Use, and over 98% Accurate. Certified GMP and ISO13485. Test yourself at home with Complete Privacy. Buy online today at: http://www.stdrapidtest.com