Top videos

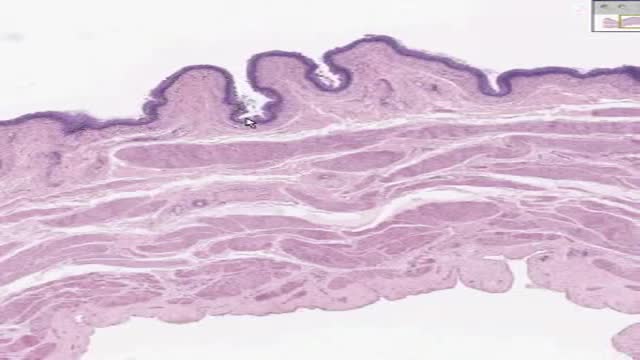
Ankle fusion (arthrodesis) This is a surgical procedure which joins together the main bones of the ankle joint (the tibia and the talus). However, depending on the technique your surgeon will use, occasionally the fibula will be included in this procedure. The two joint surfaces which generate the pain are removed.
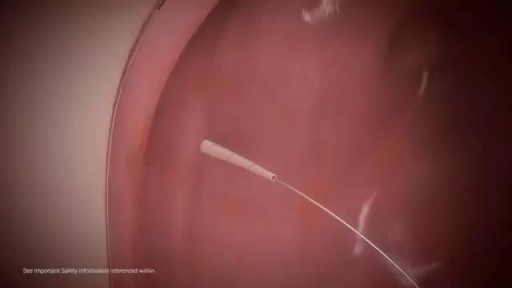
Mitral valve regurgitation, known as leaky heart valve, can be treated with the MitraClip procedure, especially if you're not a candidate for surgery. As premier heart specialists in the Rocky Mountains, Aurora Denver Cardiology Associates physicians perform this procedure and believe it can be an essential treatment for heart health.
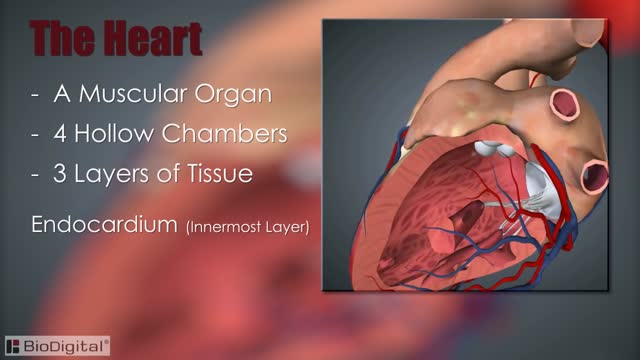
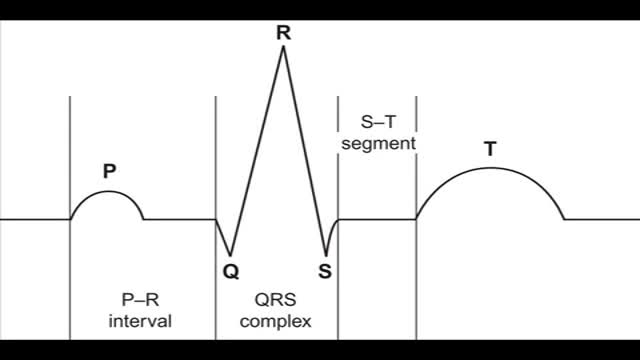
The heart, blood vessels, and blood are the parts that make up the circulatory system, which is defined as a closed system of blood vessels for the transport of gasses and nutrients. The heart is the key organ in the circulatory system. As a hollow, muscular pump, its main function is to propel blood throughout the body.
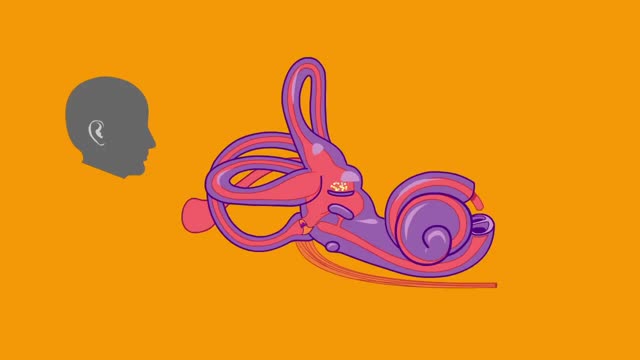
Benign paroxysmal positional vertigo is an abnormal feeling of motion triggered by certain provocative positions. The condition is most often attributed to the presence of calcium debris within the posterior semicircular canal. Nystagmus is commonly seen
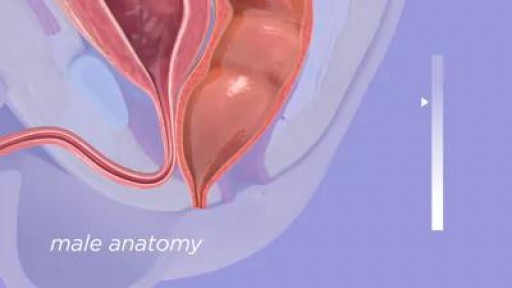
Anorectal malformations are defects that occur during the fifth to seventh weeks of fetal development. With these defects, the anus (opening at the end of the large intestine through which stool passes) and the rectum (area of the large intestine just above the anus) do not develop properly

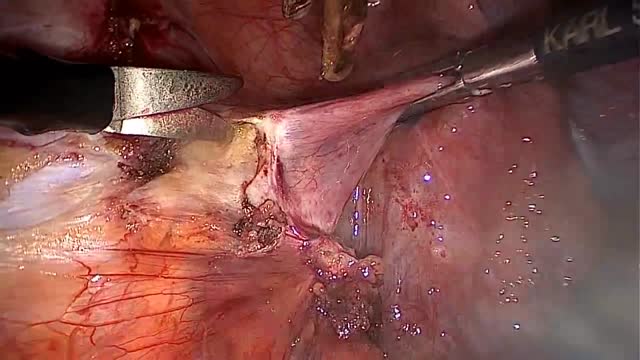
Emory has one of the few heart and vascular centers nationally performing robotic cardiac surgery using the daVinci Surgical System. Emory's robotic surgeons have completed numerous cases and are recognized in Atlanta, the Southeast and across the country for their expertise in cardiac surgery. Some of the cardiac and thoracic conditions treated by Emory cardiac surgeons include mitral valve repair and replacement, atrial septal defect repair, atrial myxoma and thrombi, coronary bypass (LIMA to LAD), mediastinal mass excision, thymectomy, epicardial lead placement and pericardial window.

Multiple endocrine neoplasia is a group of disorders that affect the body's network of hormone-producing glands (the endocrine system). Hormones are chemical messengers that travel through the bloodstream and regulate the function of cells and tissues throughout the body. Multiple endocrine neoplasia typically involves tumors (neoplasia) in at least two endocrine glands; tumors can also develop in other organs and tissues. These growths can be noncancerous (benign) or cancerous (malignant). If the tumors become cancerous, the condition can be life-threatening.

Euthyroid sick syndrome (ESS), sick euthyroid syndrome (SES), thyroid allostasis in critical illness, tumours, uremia and starvation (TACITUS), non-thyroidal illness syndrome (NTIS) or low T3 low T4 syndrome is a state of adaptation or dysregulation of thyrotropic feedback control where the levels of T3 and/or T4 are ...

The vast majority of glucocorticoid activity in most mammals is from cortisol, also known as hydrocortisone. Corticosterone, the major glucocorticoid in rodents, is another glucocorticoid. Cortisol binds to the glucocorticoid receptor in the cytoplasm and the hormone-receptor complex is then translocated into the nucleus, where it binds to its DNA response element and modulates transcription from a battery of genes, leading to changes in the cell's phenotype. Only about 10% of circulating cortisol is free. The remaining majority circulates bound to plasma proteins, particularly corticosteroid-binding globulin (transcortin). This protein binding likely decreases the metabolic clearance rate of glucocorticoids and, because the bound steroid is not biologically active, tends to act as a buffer and blunt wild fluctuations in cortisol concentration.