Top videos

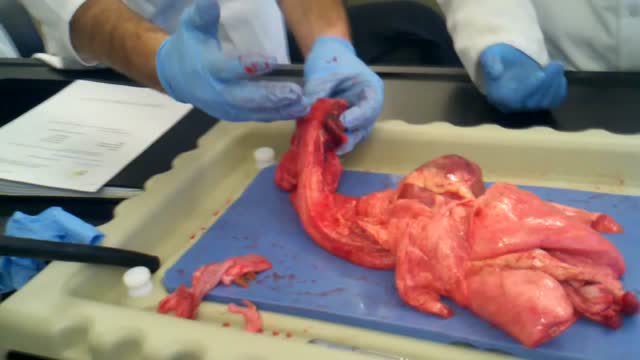
This video: The veins around your anus tend to stretch under pressure and may bulge or swell. Swollen veins (hemorrhoids) can develop from an increase in pressure in the lower rectum. Factors that might cause increased pressure include: Straining during bowel movements.
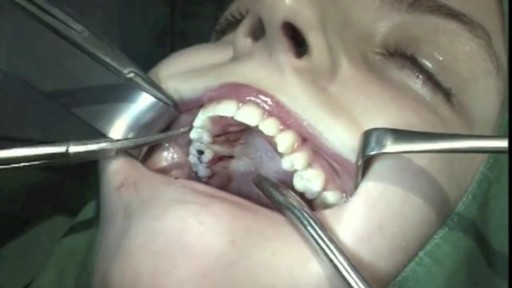
Simply put, there isn’t enough room for wisdom teeth because our jaws don’t grow to be big enough to have enough space for them to come in. Since there isn’t enough room for them to erupt properly, wisdom teeth tend to come in at an angle or they don’t fully emerge, which causes problems for the rest of the mouth. Third molars (the wisdom teeth) routinely damage the teeth right next door, called second molars. Dentists recommend removing wisdom teeth before they become a problem and to avoid a more complicated surgery. Read more at Ask the Dentist: https://askthedentist.com/wisdom-teeth-removal/

http://cfs-cure.plus101.com ----- Chronic Fatigue Syndrome Diet , Cures For Fatigue, Cure For Chronic Fatigue Syndrome. Chronic Fatigue Syndrome Treatment Chronic Fatigue Syndrome (CFS) is variable and unpredictable, and the condition takes its toll on the patient physically, mentally and emotionally. A number of studies have been performed on CFS, with one particular study determining poor early management of the disorder as a primary risk factor for severe CFS. Among the medical community, there is still no consensus on the best course of action for CFS. Most doctors feel that there is no cure for this condition, and limit their treatment to managing the symptoms. There is controversy over different approaches, and main ones being: • Prescription medications • Lifestyle changes • Diet • Nutritional supplements • Graded exercise therapy • Cognitive behavioral therapy • Other alternative/complementary treatments As CFS affects the patients not only physically but also mentally and emotionally, a holistic approach needs to be taken. It is also important that the people around CFS patients understand the condition, and realize that the patient is not just "being lazy" or "constantly feeling down" - chronic fatigue syndrome IS a serious illness and has severe symptoms. Cognitive Behavioral Therapy Cognitive behavioral therapy helps individuals to interpret their symptoms, which in turn helps the patient to shape their behavior in a way to better react to the symptoms. Graded Exercise Therapy A physical therapist can help determine the best exercises for the individual. Programs will start with low levels of exercising, increasing the intensity as the individual gradually builds strength and endurance. Lifestyle Changes Lifestyle changes will also be necessary, including individuals pacing themselves, lowering stress levels, eating a well-balanced diet, engaging in regular moderate exercise, and improving sleep habits. The individual’s work schedule may also need to be modified, as many individuals with CFS find maintaining their regular work schedule too draining. Diet and Chronic Fatigue Syndrome Treatment Diet is crucial in CFS, and dietary supplements may be needed. Certain foods may need to be restricted from the diet, as these may trigger or exacerbate CFS symptoms. A diet-symptom journal can help individuals to identify problem foods. In addition, a significant number of CFS cases may be caused or worsened by un-diagnosed food allergies and intolerances. Therefore, it should be a priority for every patient to check for these using a food-symptom diary and elimination diet, especially if in addition to fatigue you experience gastrointestinal symptoms such as stomach cramps, constipation, or diarrhea. Prescriptions and Medications Depression is often associated with CFS. Antidepressants may be prescribed to treat depression, which in turn will help individuals to cope with CFS-related problems. Studies also show antidepressants administered in low doses may help to relieve pain and improve sleep. Prescription sleep aids may also be prescribed to help individuals improve their sleep. Other drugs that may be prescribed include antiviral drugs, ADD/ADHD medications and anti-anxiety drugs. Alternative/Alternative Chronic Fatigue Syndrome Treatment While the usefulness of alternative/complementary therapy may still be controversial in the scientific community, many patients experience tremendous benefits from these. Main ones include:
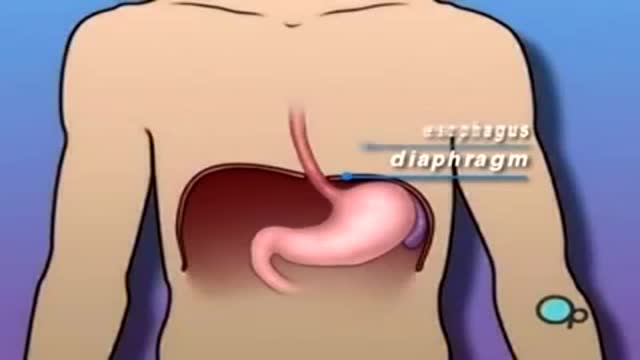
A hiatus hernia or hiatal hernia is the protrusion (or herniation) of the upper part of the stomach into the thorax through the esophageal hiatus because of a tear or weakness in the diaphragm. Hiatus hernias often result in heartburn but may also cause chest pain or pain with eating. The most common cause is obesity.
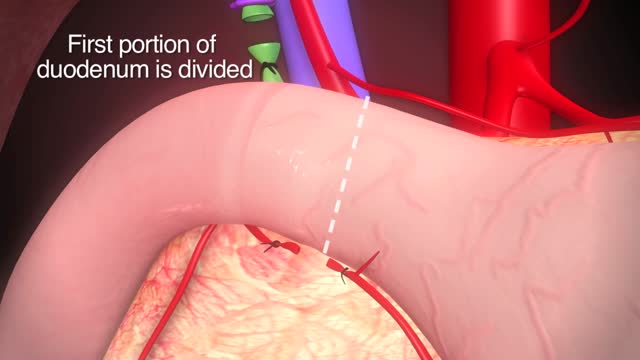
Our specialists treat conditions that are recurrent and hard to treat. Simply put, TPIAT a procedure that lets surgeons remove the pancreas, take out islet cells – the cells in the pancreas that make insulin – and put those islet cells into the liver. Patients then take pancreatic enzymes to help them digest food.

Como Aumentar La Testosterona, Testosterona Masculina, Como Aumentar El Nivel De Testosterona --- http://aumentar-testosterona.good-info.co/ --- ¿Baja Testosterona En Hombres Es Peligrosa? ¿Cual es la hormona en los hombres que les permite construir músculo magro, quemar más grasa, ser más fertíil y aumentar la energía de manera general? es la TESTOSTERONA La testosterona es una hormona tan esencial para los hombres porque en realidad define lo que es la virilidad masculina. Y la pérdida de esta hormona tan importante resulta en: * Aumentos de peso * Falta de deseo * Falta de energía y motivación * Pérdida de músculo magro * Depresión * Grasa de pecho Lo que sucede hoy en dia es que más hombres que nunca están perdiendo la testosterona. De hecho, segun el famoso (experto de hormonas masculinas) el nivel de testosterona en los hombres disminuye tan rapidamente que es una verdadera CRISIS para los hombres. Si tu o otra persona experimenta la baja testosterona que sepa que NO es por tu culpa! ¿Cansado Con Tus Bajos Niveles De Testosterona, Tu Sobrepeso y Tu Falta de Libido? Haga click aqui http://aumentar-testosterona.good-info.co/
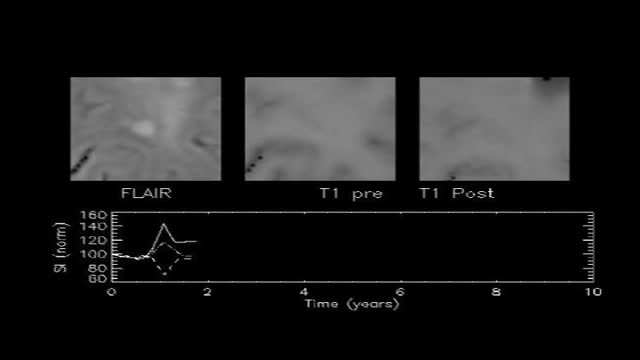
If you have multiple sclerosis (MS), you probably had several tests done before you received your diagnosis. There isn’t one test to diagnosis MS, so testing can vary. Doctors can use neurological exams, information about previous symptoms, blood tests, and spinal fluid tests. A magnetic resonance imaging (MRI) scan isn’t used to diagnose MS but rather to rule out other diseases. A diagnosis of MS requires more information than what a scan alone can give. By looking at more than one test or exam result, doctors can get a clearer picture of what’s going on in your body.
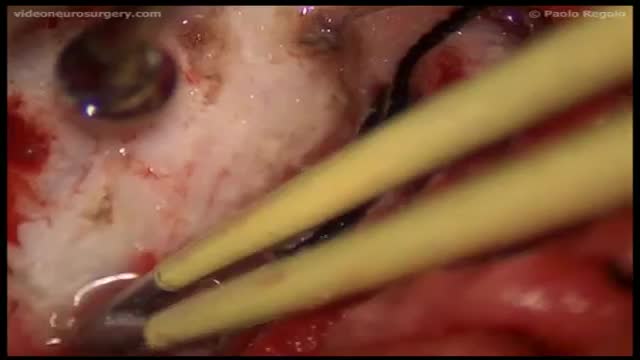
Chordoid meningioma, classified as atypical meningioma according to the World Health Organisation (WHO) classification, is a rare subtype, which represents only 0.5% of all meningiomas and is associated with a high incidence of recurrence. Multiple intracranial meningiomas are rare in non-neurofibromatosis patients. We present a female patient with both of these rare types of meningioma. The patient presented with two concurrent intracranial meningiomas, with one a meningotheliomatous subtype and the other a chordoid meningioma. Given the wide array of histological differential diagnoses in chordoid meningioma, immunohistochemistry has a significant role to play in differentiating them. Recurrence in chordoid meningioma can be generally predicted based on the extent of resection, the percentage of chordoid element, and proliferation indices.
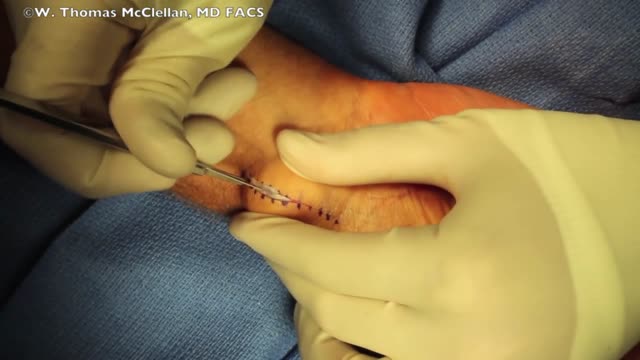
Ganglion cysts are the most common mass or lump in the hand. They are not cancerous and, in most cases, are harmless. They occur in various locations, but most frequently develop on the back of the wrist. These fluid-filled cysts can quickly appear, disappear, and change size.
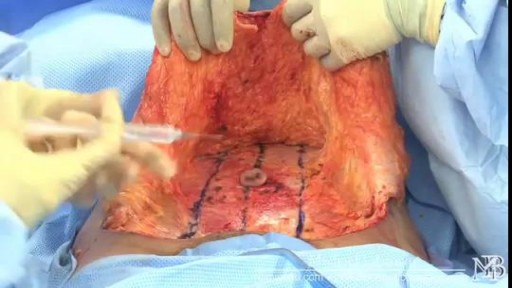
Tummy tuck surgery, also known as abdominoplasty, removes excess fat and skin and, in most cases, restores weakened or separated muscles creating an abdominal profile that is smoother and firmer. A flat and well-toned abdomen is something many of us strive for through exercise and weight control. Sometimes these methods cannot achieve our goals. Even individuals of otherwise normal body weight and proportion can develop an abdomen that protrudes or is loose and sagging. The most common causes of this include: Aging Heredity Pregnancy Prior surgery Significant fluctuations in weight What tummy tuck surgery can't do A tummy tuck is not a substitute for weight loss or an appropriate exercise program. Although the results of a tummy tuck are technically permanent, the positive outcome can be greatly diminished by significant fluctuations in your weight. For this reason, individuals who are planning substantial weight loss or women who may be considering future pregnancies would be advised to postpone a tummy tuck. A tummy tuck cannot correct stretch marks, although these may be removed or somewhat improved if they are located on the areas of excess skin that will be excised.
You're sneezing, coughing, and all stuffed up. It sounds and feels like a cold, alright. But as time goes on, you start to wonder. Is it turning into a sinus infection? They've got some things in common, but there are ways to tell them apart. The right ID lets your doctor get you the best treatment. What Is a Common Cold? It's an infection caused by a virus, a tiny living thing. You can't miss the symptoms: Nasal congestion Runny nose Post-nasal drip (drop-by-drop release of fluid from your nose into the back of the throat) Headache Fatigue You may also get a cough and a mild fever. The symptoms usually build, peak, and slowly disappear. Some medications can ease symptoms. For example, decongestants may decrease drainage and open the nasal passages. Pain relievers may help with fever and headache. Cough medicine may help, as well. Colds typically last from a few days to about a week or longer. Sometimes, a cold may cause swelling in the sinuses, hollow spaces in your skull that are connected to each other. The swelling can prevent the flow of mucus.

Pharyngitis is caused by swelling in the back of the throat (pharynx) between the tonsils and the voice box (larynx). Most sore throats are caused by colds, the flu, coxsackie virus or mono (mononucleosis). Bacteria that can cause pharyngitis in some cases: Strep throat is caused by group A streptococcus.
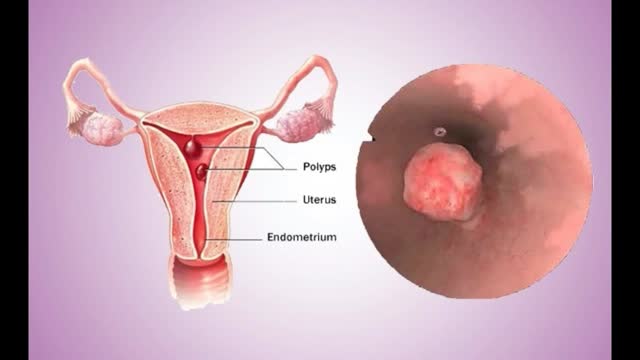
Uterine polyps are growths attached to the inner wall of the uterus that extend into the uterine cavity. Overgrowth of cells in the lining of the uterus (endometrium) leads to the formation of uterine polyps, also known as endometrial polyps. These polyps are usually noncancerous (benign), although some can be cancerous or can eventually turn into cancer (precancerous polyps). Uterine polyps range in size from a few millimeters — no larger than a sesame seed — to several centimeters — golf-ball-size or larger. They attach to the uterine wall by a large base or a thin stalk.

Multiple endocrine neoplasia is a group of disorders that affect the body's network of hormone-producing glands (the endocrine system). Hormones are chemical messengers that travel through the bloodstream and regulate the function of cells and tissues throughout the body. Multiple endocrine neoplasia typically involves tumors (neoplasia) in at least two endocrine glands; tumors can also develop in other organs and tissues. These growths can be noncancerous (benign) or cancerous (malignant). If the tumors become cancerous, the condition can be life-threatening.

Euthyroid sick syndrome (ESS), sick euthyroid syndrome (SES), thyroid allostasis in critical illness, tumours, uremia and starvation (TACITUS), non-thyroidal illness syndrome (NTIS) or low T3 low T4 syndrome is a state of adaptation or dysregulation of thyrotropic feedback control where the levels of T3 and/or T4 are ...

The vast majority of glucocorticoid activity in most mammals is from cortisol, also known as hydrocortisone. Corticosterone, the major glucocorticoid in rodents, is another glucocorticoid. Cortisol binds to the glucocorticoid receptor in the cytoplasm and the hormone-receptor complex is then translocated into the nucleus, where it binds to its DNA response element and modulates transcription from a battery of genes, leading to changes in the cell's phenotype. Only about 10% of circulating cortisol is free. The remaining majority circulates bound to plasma proteins, particularly corticosteroid-binding globulin (transcortin). This protein binding likely decreases the metabolic clearance rate of glucocorticoids and, because the bound steroid is not biologically active, tends to act as a buffer and blunt wild fluctuations in cortisol concentration.

Blind loop syndrome (BLS), commonly referred to in the literature as small intestinal bacterial overgrowth (SIBO) or bacterial overgrowth syndrome (BOS), is a state that occurs when the normal bacterial flora of the small intestine proliferates to numbers that cause significant derangement to the normal physiological ...