Top videos

Ellis and Cathy demonstrate how to administer blood to a patient.
Our Critical Nursing Skills video tutorial series is taught by Ellis Parker MSN, RN-BC, CNE, CHS and intended to help RN and PN nursing students study for your nursing school exams, including the ATI, HESI and NCLEX.
#NCLEX #ClinicalSkills #Blood #bloodtransfusion #HESI #Kaplan #ATI #NursingSchool #NursingStudent #Nurse #RN #PN #Education #LVN #LPN
00:00 What to expect blood transfusion
00:26 First steps for a blood transfusion
1:03 Priming the tubing for blood transfusion
2:29 Confirming the blood for transfusion
4:36 Hanging the blood for transfusion
5:06 Clamping a Y-tube
5:34 Priming the blood for transfusion
7:00 Responding to a blood transfusion reaction
🚨 Reminder: shipping deadlines are looming 👀
🎁 Regular Shipping: Order by Friday, December 15
🚀 Expedited Shipping: Order by Monday, December 18
🔍 Still searching for last-minute gifts? Consider a Level Up RN Gift Card! 💌 It’s not only a thoughtful present but also the perfect way to share treasures like Pharmacology Flashcards OR digital treasures like Flashables Digital Nursing Flashcards & the Level Up RN membership. Give the gift of knowledge this holiday season! 🧠⚡️💖 bit.ly/LevelUpRNGC
🚪 Access our Cram Courses, Quizzes and Videos all in one ad free space with Level Up RN Membership https://bit.ly/LevelUpRNMembership
Want more ways to MASTER Clinical Skills? Check out our flashcards & videos!
👇👇👇👇👇👇👇👇👇👇
👉 https://bit.ly/clinicalnursingskills 👈
☝️👆☝️👆☝️👆☝️👆☝️👆
This is your one-stop-shop for materials to help you LEARN & REVIEW so you can PASS Nursing School.
🤔🤔🤔 DO YOU WANT TO PASS your classes, proctored exams and the NCLEX? 🤔🤔🤔 Our resources are the best you can buy. They are built with a single goal: help you pass with no fluff. Everything you need, and nothing you don’t. Don’t take our word for it, though! Check out our hundreds of ⭐️⭐️⭐️⭐️⭐️ reviews from nurses who passed their exams and the NCLEX with Level Up RN.
🗂️ Our Ultimate Nursing School Survival kit is your number 1 resource to get through nursing school and to pass the NCLEX. Whether you're just starting school or you’re already prepping for the NCLEX, this bundle of flashcards is the best you can buy. It covers all the information you need to know to pass all your exams and it has FREE shipping!
➡️ https://bit.ly/TUNSSK ⬅️
L👀king for EVEN MORE resources to survive Nursing School? Make your Nursing School experience your own! Life’s difficult enough—learning shouldn’t be.
🪅 Games https://nursesquad.com
💻 Digital resources https://bit.ly/NursingStudyCourses
📅 Organizational tools https://bit.ly/OrganizingSchool
✨Want perks? Join our channel!
https://youtube.com/leveluprn/join
🏷 Head to https://leveluprn.com/specials for all our latest deals!🥳️
📧 LOOKING FOR FREE RESOURCES TO HELP WITH YOUR EXAMS? Get exclusive tips, latest video releases and more delivered to your email!
➡️ https://leveluprn.com/signup ⬅️
⚕ 👩 LEVEL UP NURSE SQUAD 👩⚕️
All of the nurses at Level Up RN are here to help! Cathy Parkes started helping her fellow classmates back when she was in nursing school, tutoring so they could pass their exams and graduate. After she got her BSN and started working as an RN at Scripps Encinitas Hospital, she started this YouTube channel to help nursing students around the world. Since then she has built a team of top-notch dedicated nurses and nurse educators who are focused on improving nursing education and supporting career advancement for nurses everywhere. With flashcards, videos, courses, organizational tools and more, we are singularly focused on helping students and nurses Level Up on their exams and nursing careers.
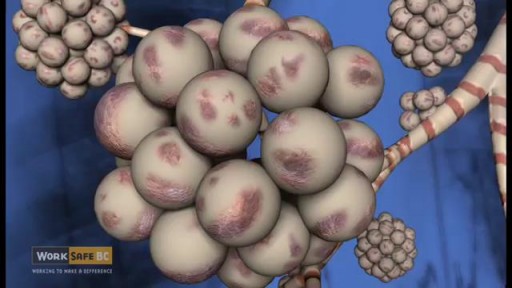
Asbestosis is linked to chrysotile fibers. Chrysotile is one of the six known types of asbestos. Exposure occurs when someone breathes in the dangerous fibers. Extended exposure can lead to an accumulation of the fibers in lung tissues, setting the stage for long-term fibrosis (scarring). Over time, lung tissues thicken, causing pain and restricting breathing. Symptoms include labored breathing during routine tasks and exercise, chest pain and coughing. Doctors prescribe breathing treatments, prescription medication and sometimes surgery for people with asbestosis.
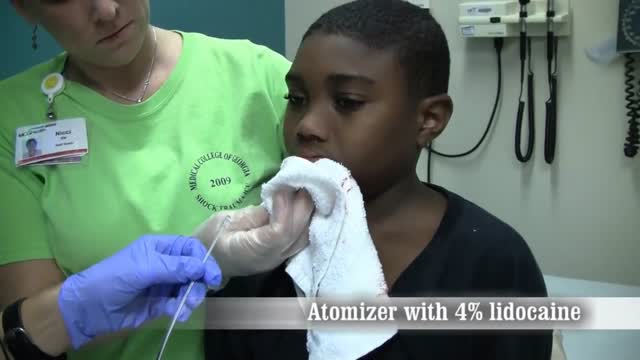
Nosebleeds common. Most often they are a nuisance and not a true medical problem. But they can be both. Nosebleed care Sit upright and lean forward. By remaining upright, you reduce blood pressure in the veins of your nose. This discourages further bleeding. Sitting forward will help you avoid swallowing blood, which can irritate your stomach. Pinch your nose. Use your thumb and index finger to pinch your nostrils shut. Breathe through your mouth. Continue to pinch for five to 10 minutes. Pinching sends pressure to the bleeding point on the nasal septum and often stops the flow of blood. To prevent re-bleeding, don't pick or blow your nose and don't bend down for several hours after the bleeding episode. During this time remember to keep your head higher than the level of your heart. If re-bleeding occurs, blow out forcefully to clear your nose of blood clots and spray both sides of your nose with a decongestant nasal spray containing oxymetazoline (Afrin, Mucinex Moisture Smart, others). Pinch your nose again as described above and call your doctor. When to seek emergency care The bleeding lasts for more than 20 minutes The nosebleed follows an accident, a fall or an injury to your head, including a punch in the face that may have broken your nose

An enlarged spleen may cause: No symptoms in some cases. Pain or fullness in the left upper abdomen that may spread to the left shoulder. Feeling full without eating or after eating only a small amount from the enlarged spleen pressing on your stomach. Anemia. Fatigue. Frequent infections. Easy bleeding.
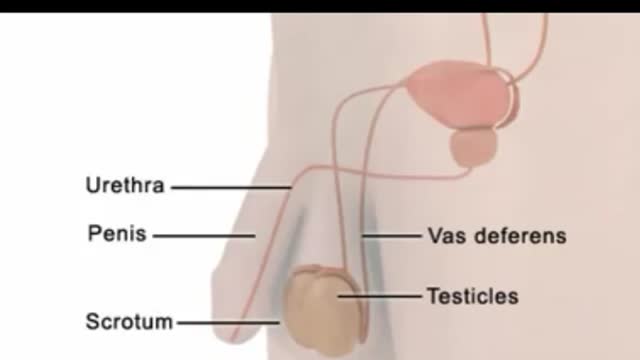
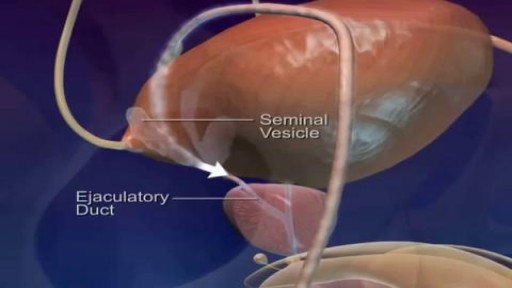
An egg cannot be fertilized when there are no sperm in the semen. The testicles continue to produce sperm, but the sperm are reabsorbed by the body. (This also happens to sperm that are not ejaculated after a while, regardless of whether you have had a vasectomy.) Sperm are made in the testicles. They pass through two tubes called the vasa deferentia to other glands and mix with seminal fluids to form semen. Vasectomy blocks each vas deferens and keeps sperm out of the seminal fluid. The sperm are absorbed by the body instead of being ejaculated.
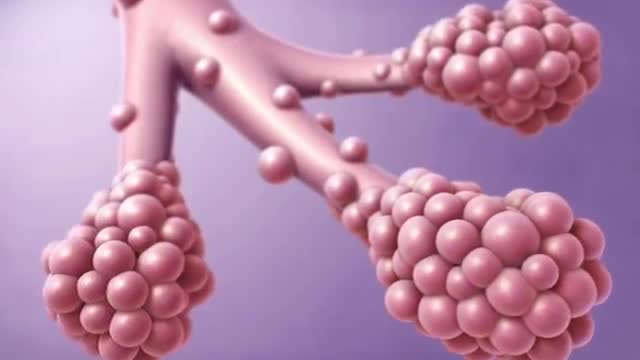
Idiopathic pulmonary fibrosis (IPF) is defined as a specific form of chronic, progressive fibrosing interstitial pneumonia of unknown cause, primarily occurring in older adults, limited to the lungs, and associated with the histopathologic and/or radiologic pattern of usual interstitial pneumonia (UIP).[1] Signs and symptoms The clinical symptoms of idiopathic pulmonary fibrosis are nonspecific and can be shared with many pulmonary and cardiac diseases. Most patients present with a gradual onset (often >6 mo) of exertional dyspnea and/or a nonproductive cough. Approximately 5% of patients have no presenting symptoms when idiopathic pulmonary fibrosis is serendipitously diagnosed.

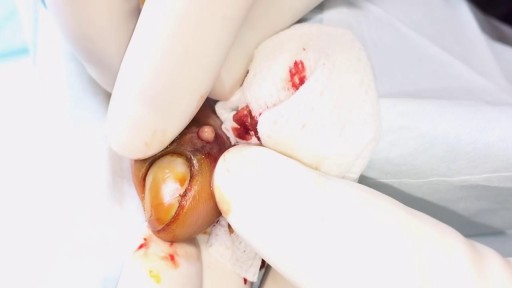
plantar fasciitis and calcaneal spur can be treated by EPFR with calcanean drilling - endoscopic plantar fascia release علاج الشوكة العظمية للكعب بالمنظار د. أسامة الشاذلي مدرس جراحة العظام واستشاري جراحات و مناظير القدم والكاحل كلية الطب جامعة عين شمس
Generic minoxidil is known to treat hair-fall issues in men and women, it is best for hair growth, hair re-development, etc. it is available in the strength of 5mg and easily available at online pharmacy store. For more information visit to http://www.medstorerx.com/generic-minoxidil.aspx
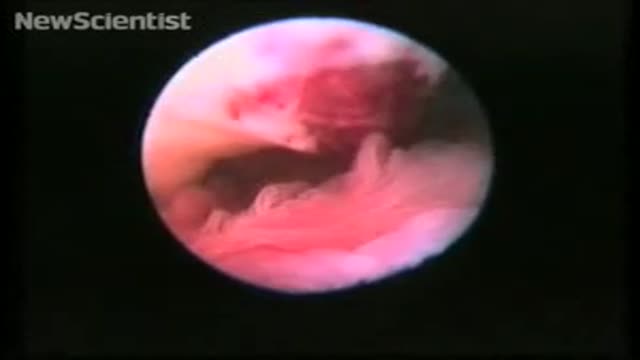
To record the sequence, Stephan Gordts and Ivo Brosens of the Leuven Institute for Fertility & Embryology in Belgium performed transvaginal laparoscopy, which involves making a small cut in the vaginal wall and observing the ovary with an endoscope.
"This allows us direct access to and observation of the tubo-ovarian structures without manipulation using forceps," says Gordts.
For the photos of ovulation, which only accidentally captured the critical moment, Jacques Donnez at the Catholic University of Louvain (UCL) in Brussels, Belgium, used gas to distend the organs for photography. However, Gordts and Brosens planned the procedure to coincide with ovulation and used saline solution to "float" the structures.
Perfect timing
Observation was timed for the day of the peak of the patient's luteal hormone cycle. Ovulation was predicted to occur on the evening of the day of the LH peak, and the endoscope introduced at 6 pm.
A small amount of saline was used to float the opening of the fallopian tube, its fimbriae (the "fingers" that sweep the egg into the tube) and the ovary itself. This gives a more natural appearance than gas, says Gordts.
In the video, the fimbriae can be seen sweeping in time with the patient's heartbeat. A mucus plug can be seen protruding from the ovary – this contains the egg.
"The ovum is not captured 'naked'," says Gordts. "There is no eruption like a volcano."
Gordts says that in clinical practice it is not easy to organise the observation of ovulation. "We were probably lucky to be successful at our first attempt," he says.
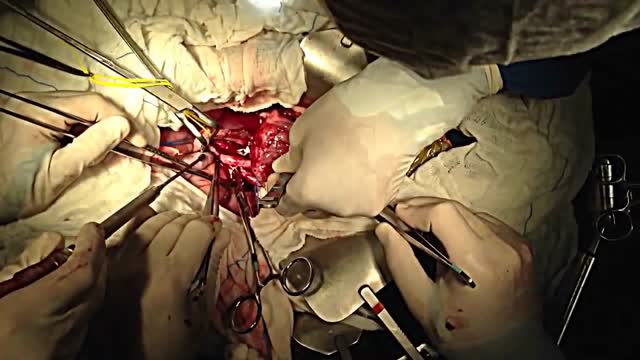
A pancreas transplant is a surgical procedure to place a healthy pancreas from a deceased donor into a person whose pancreas no longer functions properly. Your pancreas is an organ that lies behind the lower part of your stomach. One of its main functions is to make insulin, a hormone that regulates the absorption of sugar (glucose) into your cells. If your pancreas doesn't make enough insulin, blood sugar levels can rise to unhealthy levels, resulting in type 1 diabetes. Most pancreas transplants are done to treat type 1 diabetes. A pancreas transplant offers a potential cure for this condition. But it is typically reserved for those with serious diabetes complications, because the side effects of a pancreas transplant are significant. In some cases, pancreas transplants may also treat type 2 diabetes. Rarely, pancreas transplants may be used in the treatment of pancreatic, bile duct or other cancers. A pancreas transplant is often done in conjunction with a kidney transplant in people whose kidneys have been damaged by diabetes.
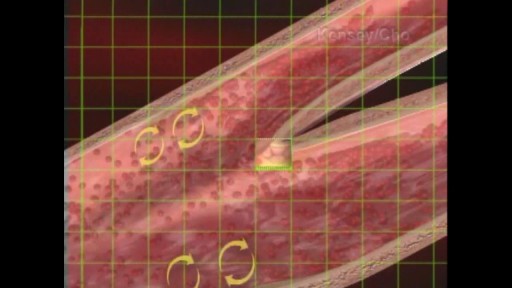
When the hematocrit rises to 60 or 70%, which it often does in polycythemia, the blood viscosity can become as great as 10 times that of water, and its flow through blood vessels is greatly retarded because of increased resistance to flow. This will lead to decreased oxygen delivery.

Acromegaly is usually caused by a noncancerous tumor. Middle-aged adults are most commonly affected. Symptoms include enlargement of the face, hands, and feet. Prompt treatment is needed to avoid serious illness. Drugs can reduce the effects of growth hormone. If needed, surgery and radiation may be used to remove tumor cells.