Top videos

Pass your tests and improve your grades with the below FREE resources:
1) A FREE 140 Must Know Meds book
Click here to get your FREE copy of the 140 Must Know Meds Book: https://bit.ly/41rxSt0
2) A FREE test-taking tips webinar
Join us for our free test-taking tips webinar to boost your exam scores: https://bit.ly/nursingtesttaking
You can now test your knowledge with a free lesson quiz on NURSING.com!
Click here for your free quiz: https://bit.ly/3uyTWEu
Learn what's working for other Nursing Students! Check out our Top 10 Most Popular Lessons Here: https://bit.ly/3nda5u3
Dressing Changes- Wet to Dry (Nursing Skills)
FREE Nursing School Cheat Sheets at: http://www.NURSING.com
Get the full Dressing Change lesson here: https://nursing.com/lesson/ski....lls-05-04-wound-care
Click here for the related lesson on Wound Assessment: https://nursing.com/lesson/ski....lls-05-02-wound-care
Welcome to the NURSING Family, we call it the most supportive nursing cohort on the planet.
At NURSING.com, we want to help you remove the stress and overwhelm of nursing school so that you can focus on becoming an amazing nurse.
Check out our freebies and learn more at: (http://www.nursing.com)
Dressing Changes- Wet to Dry (Nursing Skills):
In this video we’re going to look at how to do a wet to dry dressing change. Wound care and dressing changes should be performed at least daily or more often depending on orders. Dressing changes should be sterile to avoid introducing any new bacteria to the wound and to promote wound healing.
Bookmarks:
0:05 Introduction
0:10 Wound Assessment link above
0:24 Dressing Change Prep
1:24 Wet vs Dry Gauze
1:37 Soaking Gauze
2:00 Gauze Ring Out
2:25 Packing the wound
3:00 Covering the wound bed
3:37 Dry gauze barrier
4:00 ABD pad application
4:46 Documentation
4:54 Outro
Visit us at https://nursing.com/medical-disclaimer/ for disclaimer information.
NCLEX®, NCLEX-RN® are registered trademarks of the National Council of State Boards of Nursing, INC. and hold no affiliation with NURSING.com.

Full Tummy Tuck 3D Video - http://drlandsman.com
Look great... feel great
•Smart Liposuction + Liposculpture
•Abdominplasty (Tummy Tuck)
+ Full Mini Modified
•Brazilian Lift with Fat Transfer
•Vaginal Aesthetics & Rejuvenation
•Laser Hair Removal
•Full Body Lift
•Thigh lift
•Brachioplasty (Arm Lift) + Short Scar
Expertise in Body Contouring
Board Certified Plastic Surgeon
Expertise in body contouring combines skin excision techniques and advanced fat contouring technology
Weight control personalized training and smoking cessation results in a healthier lifestyle improved shape and longer lasting results
With over 2 decades of experience Dr Lloyd Landsman provides state of the art cosmetic and plastic surgery
Dr Landsman integrates the finest and safest products with the newest procedures
A customized treatment plan is created for each patient utilizing classic surgical and minimally invasive techniques for optimal results
Call for your complimentary consultation to learn how Dr Landsman can help you look your very best
Visit http://drlandsman.com Call 631 864 4111
Main Office 994 W Jericho Tpke Smithtown NY 11787
Affiliates East Islip • Westbury • Jackson Heights • Manhattan
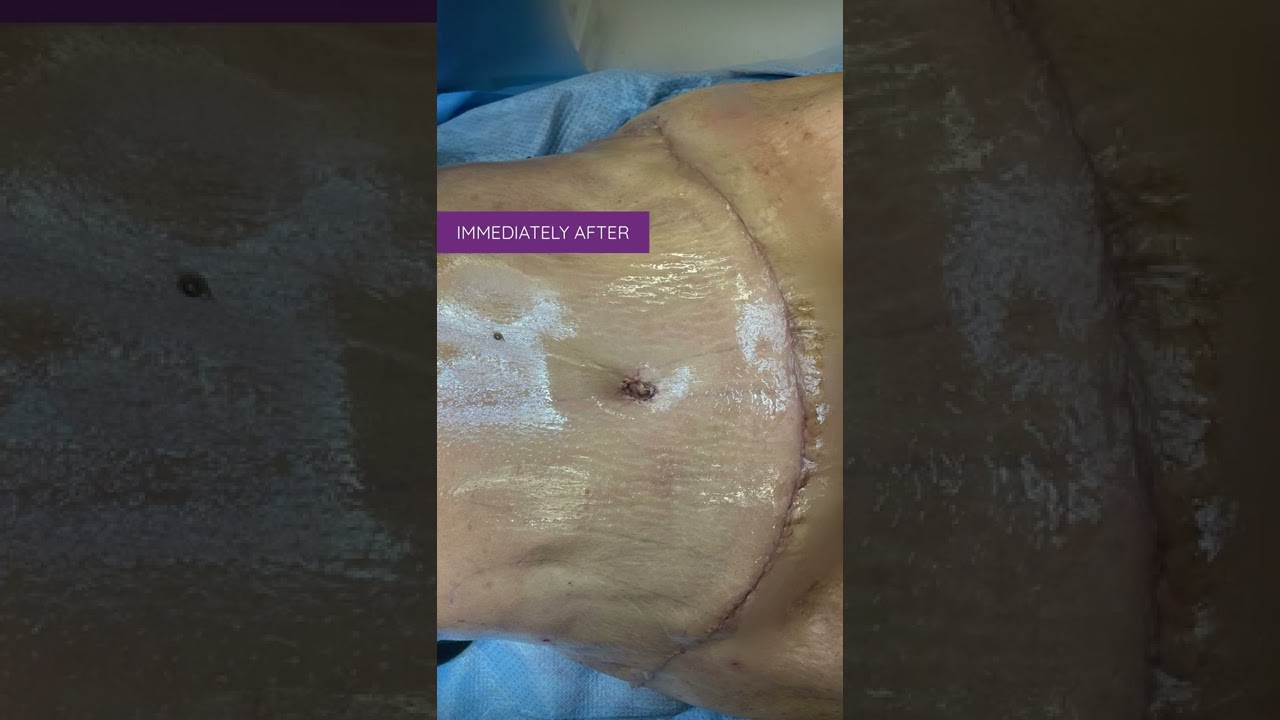
Liposuction in tummy tuck requires special planning and technique. I need to ensure that the blood circulation is well maintained for good healing. Yet proper liposuction is important to have a nice flat and contoured tummy.
#hdliposuction #tummytuck #lipoabdominoplasty #surgicalplanning #skinremovalsurgery #imeediatelyafter #plasticsurgeondubai #cocoonaclinic #drsanjayparashar #dubai
For more information visit www.drsanjayparashar.com
For more content, follow me on my social media
Instagram : https://www.instagram.com/drsanjayparashar/
Facebook : https://www.facebook.com/drsanjayparashar
WARNING: Explicit and Educational Surgical Content.
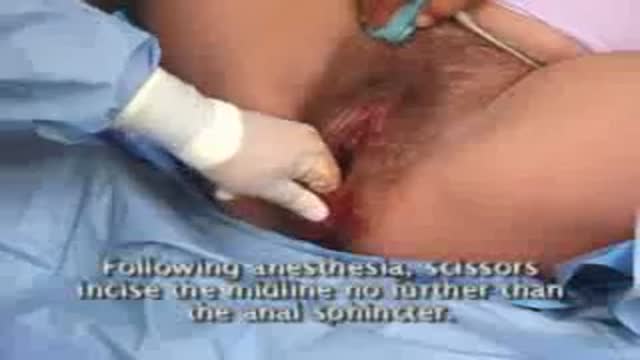
Visage Clinic's Dr. Marc DuPéré - located in Toronto, Ontario, Canada discusses Liposuction (upper bra, back rolls, lower back rolls, love handles & abdomen) and "Tummy Tuck" (Abdominoplasty): Skin excision, muscle repair and umbilicoplasty.
For more info and to book a consultation visit www.VisageClinic.com/cosmetic-....surgery/mommy-makeov or call (416) 929-9800.

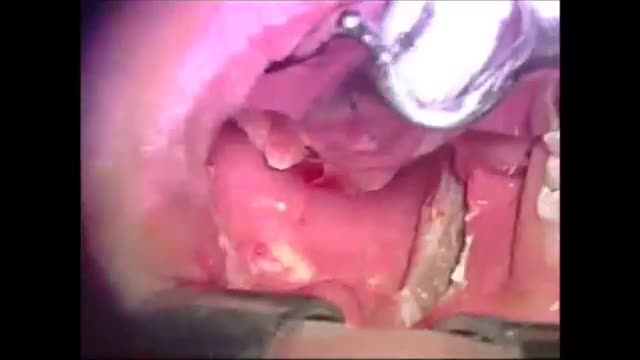
This video demonstrate Bilateral Salpingectomy for a patient suffering from hematosalpinx of one side and Hydrosalpinx other side in which one IVF has failed. Laparoscopic salpingectomy. In this less-invasive procedure, the surgeon makes 1-3 small incisions in the lower abdomen, and inserts a laparoscope into the pelvis through one of the incisions. The camera at the end of the laparoscope guides the surgeon through the procedure. The fallopian tube tissue is then removed. For more information https://www.laparoscopyhospital.com/
For more information please contact:
World Laparoscopy Hospital
Cyber City, Gurugram, NCR DELHI
INDIA 122002
Phone & WhatsApp: +919811416838, + 91 9999677788

Visit our website to learn more about using Nucleus animations for patient engagement and content marketing: http://www.nucleushealth.com/?utm_source=youtube&utm_medium=video-description&utm_campaign=appendect-020615
This 3D medical animation depicts the surgical removal of the appendix (appendectomy) using laparoscopic instruments. The surgery animation begins by showing an inflamed appendix (appendicitis), followed by the placement of the laparoscope. Afterward, one can see the surgical device staple, cut and remove the inflamed appendix. Following the removal of the appendix the abdomen is flushed with a sterile saline solution to ensure all traces of infection have been removed.
#laparoscopy #appendix #appendicitis
ANCE00183

As a pediatric surgeon at NewYork-Presbyterian/Weill Cornell Medical Center, Dr. Nitsana Spigland treats newborns, children, teens, and young adults requiring surgical interventions. She specializes in antenatal counseling and newborn congenital malformations.
Learn more about Dr. Spigland at: https://www.nyp.org/physician/nspigland.
Microsurgical bipolar cautery tonsillectomy compares favorably with traditional techniques in terms of intraoperative bleeding, postoperative pain, otalgia, and hemorrhage. This technique combines the hemostatic advantage of cautery dissection, the excellent visualization achieved by a microscope, and, with the use of a video, greatly improves the physician's ability to teach how to perform a tonsillectomy.
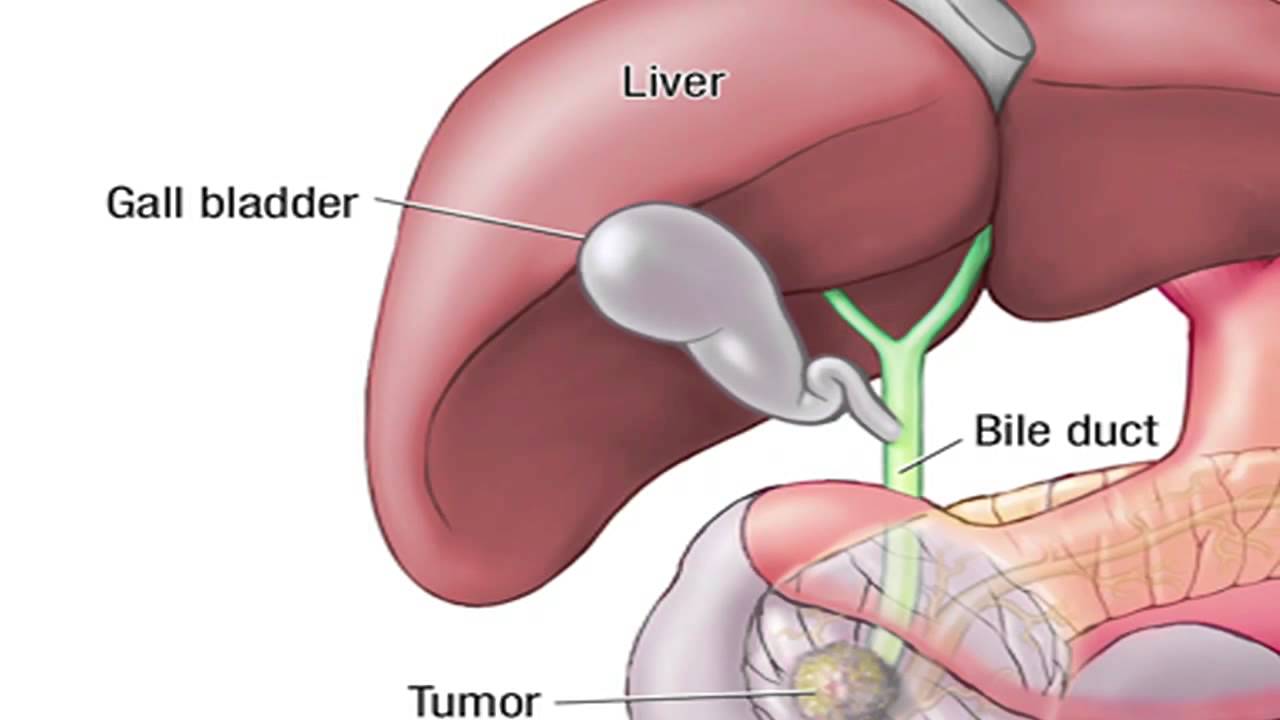
Dr. Horacio Asbun, Mayo Clinic in Florida, explains the Whipple procedure using this animated graphic of a pancreas. Cancer of the pancreas affects 45,000 people every year in the U.S., and it is the fourth leading cause of cancer-related deaths. The five-year overall survival rate if a tumor is detected early and surgically removed is 22 percent, versus 6 percent without early detection and surgery. To learn more, visit http://mayocl.in/2zk7FDi.
This video in Spanish/español: https://www.youtube.com/watch?v=N_zWboNMKWk

Mouth ulcers are sores that appear in the mouth, often on the inside of the cheeks. Mouth ulcers, also known as aphthous ulcers, can be painful when eating, drinking or brushing teeth. Occasional mouth ulcers are usually harmless and clear up on their own. Seek medical advice if they last longer than 3 weeks or keep coming back. Mouth ulcers cannot be caught from someone else. Up to 1 in 5 people get recurrent mouth ulcers.