Top videos

Vitiligine Cura, Vitiligine Rimedi Naturali, Vitiligine Omeopatia, Rimedi Per La Vitiligine -- http://vitiligine-cura.good-info.co --- Vitiligine Cura, Vitiligine Rimedi Naturali, Vitiligine Omeopatia, Rimedi Per La Vitiligine. Soffri Di Uno Qualunque Dei Seguenti Sintomi Emotivi O Fisici? Qualsiasi tipo di vitiligine (qualsiasi livello di gravità) su viso, schiena, guance, palmi delle mani, gambe o piedi? Sei affetto da macchie o scoloramento della pelle? Provi ansia nel doverti togliere la maglia in pubblico? Provi costantemente insicurezza? Provi esasperazione per il disturbo della vitiligine? Spendi molti soldi in farmaci o parafarmaci che sembrano non funzionare? Vuoi curare la vitiligine ma non sai quale sia la giusta cura a causa di un sovraccarico di informazioni? "Una Presentazione Video Gratuita Spiega Un Singolare Consiglio Per Eliminare La Vitiligine Per Sempre In 45-60 Giorni - Garantito!" http://vitiligine-cura.good-info.co

http://cfs-cure.plus101.com ----- Chronic Fatigue Syndrome Diet , Cures For Fatigue, Cure For Chronic Fatigue Syndrome. Chronic Fatigue Syndrome Treatment Chronic Fatigue Syndrome (CFS) is variable and unpredictable, and the condition takes its toll on the patient physically, mentally and emotionally. A number of studies have been performed on CFS, with one particular study determining poor early management of the disorder as a primary risk factor for severe CFS. Among the medical community, there is still no consensus on the best course of action for CFS. Most doctors feel that there is no cure for this condition, and limit their treatment to managing the symptoms. There is controversy over different approaches, and main ones being: • Prescription medications • Lifestyle changes • Diet • Nutritional supplements • Graded exercise therapy • Cognitive behavioral therapy • Other alternative/complementary treatments As CFS affects the patients not only physically but also mentally and emotionally, a holistic approach needs to be taken. It is also important that the people around CFS patients understand the condition, and realize that the patient is not just "being lazy" or "constantly feeling down" - chronic fatigue syndrome IS a serious illness and has severe symptoms. Cognitive Behavioral Therapy Cognitive behavioral therapy helps individuals to interpret their symptoms, which in turn helps the patient to shape their behavior in a way to better react to the symptoms. Graded Exercise Therapy A physical therapist can help determine the best exercises for the individual. Programs will start with low levels of exercising, increasing the intensity as the individual gradually builds strength and endurance. Lifestyle Changes Lifestyle changes will also be necessary, including individuals pacing themselves, lowering stress levels, eating a well-balanced diet, engaging in regular moderate exercise, and improving sleep habits. The individual’s work schedule may also need to be modified, as many individuals with CFS find maintaining their regular work schedule too draining. Diet and Chronic Fatigue Syndrome Treatment Diet is crucial in CFS, and dietary supplements may be needed. Certain foods may need to be restricted from the diet, as these may trigger or exacerbate CFS symptoms. A diet-symptom journal can help individuals to identify problem foods. In addition, a significant number of CFS cases may be caused or worsened by un-diagnosed food allergies and intolerances. Therefore, it should be a priority for every patient to check for these using a food-symptom diary and elimination diet, especially if in addition to fatigue you experience gastrointestinal symptoms such as stomach cramps, constipation, or diarrhea. Prescriptions and Medications Depression is often associated with CFS. Antidepressants may be prescribed to treat depression, which in turn will help individuals to cope with CFS-related problems. Studies also show antidepressants administered in low doses may help to relieve pain and improve sleep. Prescription sleep aids may also be prescribed to help individuals improve their sleep. Other drugs that may be prescribed include antiviral drugs, ADD/ADHD medications and anti-anxiety drugs. Alternative/Alternative Chronic Fatigue Syndrome Treatment While the usefulness of alternative/complementary therapy may still be controversial in the scientific community, many patients experience tremendous benefits from these. Main ones include:
Treatment consists of diet modifications and laxatives A high-fiber diet can be effective, along with over-the-counter medications, such as stool softeners. In some cases, a medical procedure to remove the hemorrhoid may be needed to provide relief.

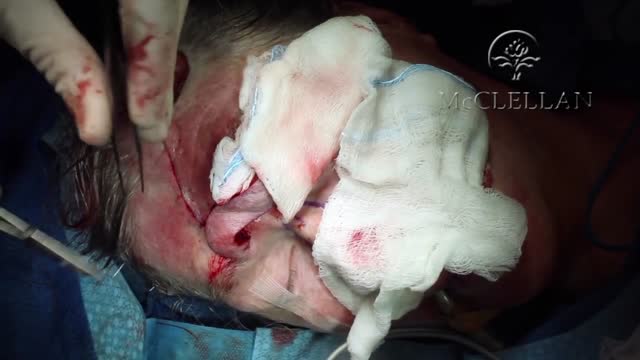
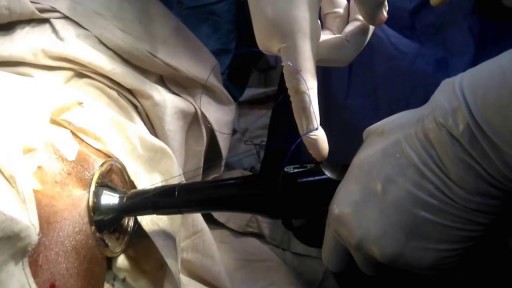
Video shows a Hip resurfacing operation done using the Durom hip from Zimmer.
The patient is a young active male. Hip resurfacing is emerging as the surgical procedure of choice in young and active patients for pain relief from Hip arthritis.

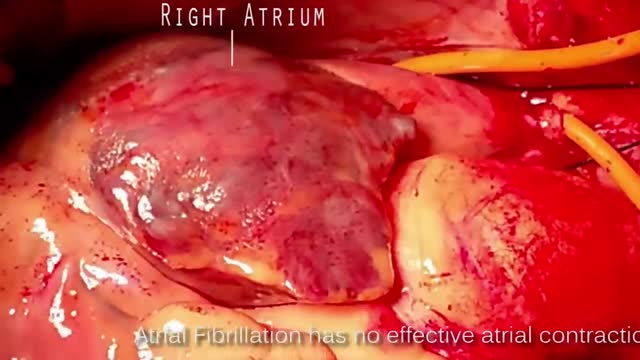
Norepinephrine is synthesized from dopamine by dopamine β-hydroxylase.[7] It is released from the adrenal medulla into the blood as a hormone, and is also a neurotransmitter in the central nervous system and sympathetic nervous system where it is released from noradrenergic neurons.

At URBN Dental, we provide you with top oral hygiene tips to help keep your mouth clean, healthy, and happy. Your manual toothbrush usually comes equipped with a tongue cleaner on the back of its head. That can be helpful in scrubbing your tongue, or you can also use a tongue cleaner. By using simple forward motions on the tongue, you can rid the area of plaque and bacteria which often cause bad breath, gingivitis, and harmful mouth ulcers.
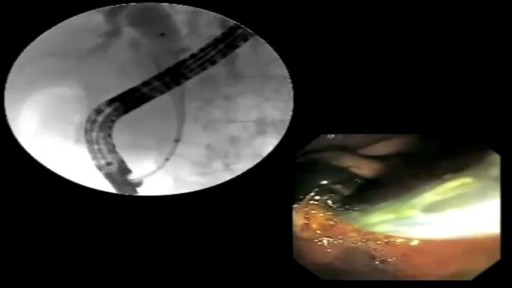
The placement of a percutaneous expandable biliary endoprosthesis was first reported in 1985 by Carrasco et al. in a canine model,[1] and the endoscopic placement of expandable metal stents to relieve biliary strictures in patients was first described in 1989.[2,3] Over the past two decades, the endoscopic approach to biliary endoprosthesis placement has largely supplanted the percutaneous approach. Self-expanding metal stents (SEMS) have traditionally been used for palliation of obstructive jaundice in patients with unresectable pancreaticobiliary tumors. However, SEMS are increasingly being used in patients with resectable cancers[4] and benign biliary strictures.[5] Uncovered SEMS (uSEMS) have been shown to have longer patency periods than plastic stents when used for malignant biliary obstruction and to be cost effective if the patient's life expectancy is greater than 4–6 months.[6–8] The common causes of malignant biliary obstruction are pancreatic cancer and cholangiocarcinoma.[9–11] Biliary drainage prior to surgical resection is controversial; several investigators have reported it to be beneficial owing to the improved tissue healing with reduced bilirubin levels,[12,13] but others have also reported its deleterious effects secondary to the additional intervention..

Wilson's disease is a rare inherited disorder that causes too much copper to accumulate in your liver, brain and other vital organs. Symptoms typically begin between the ages of 12 and 23. Copper plays a key role in the development of healthy nerves, bones, collagen and the skin pigment melanin. Normally, copper is absorbed from your food, and any excess is excreted through bile — a substance produced in your liver.